 |
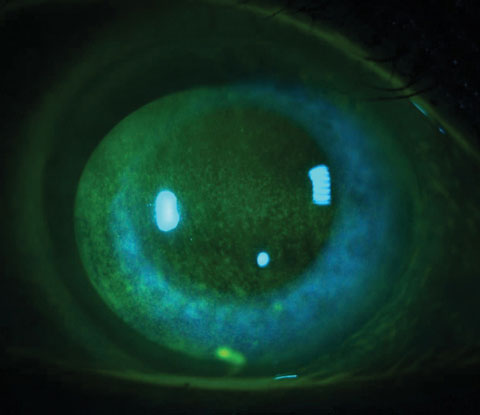
| Although it may be limited, glaucoma can have an effect on ocular dryness. Photo: Jacob R. Lang, OD. Click image to enlarge. |
One of the well-known downsides of glaucoma medications is their propensity to trigger dry eye symptoms. Unfortunately, due to higher costs of some preservative-free versions, it’s not always possible for a patient to make the switch. As such, studies have reported that glaucoma patients with dry eye tend to have reduced medication compliance. To investigate how ocular surface disease affects patients using glaucoma drugs, researchers in Korea examined dry eye-associated measures and quality of life. They found that while glaucoma medications worsened dry eye, the change was limited and quality of life didn’t decrease.
The study included 31 controls (62 eyes) and 30 patients (60 eyes) using glaucoma medications. The researchers measured tear breakup time (TBUT), lipid layer thickness (LLT), corneal and conjunctival staining scores, ocular surface disease index (OSDI) scores and visual function questionnaire 25 (VFQ-25) scores over the course of one year.
They found that glaucomatous eyes exhibited a lower change in mean LLT than control eyes after one year. While OSDI scores deteriorated, the researchers noted improved conjunctival staining and Schirmer test results in glaucomatous eyes compared with control eyes. They observed that the average LLT decreased at six and 12 months and didn’t change at 24 months. According to pairwise analysis, the six-month period of decrease in LLT was statistically significant. Additionally, VFQ-25 scores for near activity and social function demonstrated deterioration over one year in the glaucoma group, but there was no difference in the total VFQ-25 score.
One interesting finding was that Schirmer test results and conjunctival stain grade “reportedly showed improvement in a group of patients using glaucoma medications,” the researchers said. They interpret this to be a “result of increased tear secretion due to compensation mechanisms caused by deterioration of ocular surface conditions and instability of LLT.” Another study, they say, reported that loss of meibomian glands increased tear secretion as a compensatory mechanism.
They also noted no statistically significant difference in the ocular pain category of VFQ-25. “This may be due to the fact that questions in VFQ-25 focus on the overall quality of life of the patient,” the researchers said. “Of the 25 questions in the VFQ-25, there’s only one question related to ocular surface discomfort.”
The researchers say that their study results indicate that “there was no significant deterioration in quality of life of patients using glaucoma medication, as represented by the total VFQ-25 score. However, when determining a treatment plan, clinicians should consider treatment compliance, as patients with glaucoma may complain of difficulty in near activity or social functioning.”
Maeng K, Lee K, Kim S, et al. Effects of glaucoma medication on dry eye syndrome and quality of life in patients with glaucoma. Korean J Ophthalmol. October 21, 2021. [Epub ahead of print]. |


