 |
|
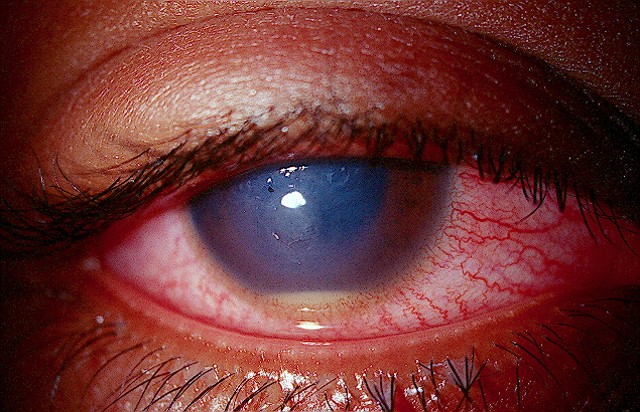
Increasing surgical volume and years of experience are both associated with significantly lower infection incidences. Photo: Joseph Sowka, OD. Click image to enlarge. |
Infamous for being “the most feared complication” of ocular surgery, endophthalmitis is fortunately rare but occurs more often after glaucoma surgeries than other types of intraocular surgeries. In order to better understand the risk factors and the incidence of endophthalmitis, which can vary significantly across different types of glaucoma surgeries, researchers analyzed glaucoma surgery outcomes using a large Medicare claims database. They found that incidences were nearly double those of cataract surgery.
In the retrospective, longitudinal study, 466,928 glaucoma surgeries were identified based on 2016-2019 Medicare Fee-For-Service and Medicare Advantage claims of patients 65 and older. Endophthalmitis cases within 42 days of surgery were identified based on ICD-10 codes. About two-thirds of the glaucoma surgeries were combined with cataract surgery. (The researchers used cataract surgeries alone (n=8,460,360) as a reference group.) Most of the glaucoma surgeries were MIGS (67.8%), followed by trabeculectomies (14%) and tube shunt procedures (10.9%). Other procedures made up 7.3% of surgeries.
A total of 572 cases of endophthalmitis occurred following all glaucoma surgeries (an incidence of 1.2 per thousand). The breakdown for incidences per thousand procedures were as follows: glaucoma surgeries alone 1.5, combined cataract/glaucoma 1.1 and cataract alone 0.8.
The researchers found that the median day of endophthalmitis diagnosis was later for glaucoma surgeries (16.5 days) than combined cataract/glaucoma (eight days) or cataract alone (six days).
They identified two significant risk factors for endophthalmitis with both standalone and combined surgery—tube shunts and Charlson comorbidity index. They also found that age and male gender were significant risk factors for only combined cataract/glaucoma surgeries.
“The median onset of endophthalmitis following traditional glaucoma surgeries was one to two weeks later than that following cataract or MIGS, suggesting that the wait time between sequential surgery on contralateral eyes should perhaps be slightly longer for traditional glaucoma surgeries unless immediate pressure lowering is needed,” the researchers explained in their Ophthalmology paper.
They added that the identified risk factors will be “relevant in assessing surgical risk for the individual patient” and may serve as a national benchmark for endophthalmitis incidence after glaucoma surgery.
Sabharwal J, Dai X, Dun C, et al. Early endophthalmitis incidence and risk factors following glaucoma surgery in the Medicare population from 2016 to 2019. Ophthalmology 2023. [Epub ahead of print]. |


