 A 57-year-old white male transferred care to our office after moving to the area in summer 2012. He had a history of open-angle glaucoma, for which he was medicated with Travatan Z (travoprost, Alcon) HS OU for the past three years. He described his glaucoma as “mild” and that his previous provider initiated therapy more as a “preventative” treatment option. His only systemic medication was lisinopril QD for hypertension.
A 57-year-old white male transferred care to our office after moving to the area in summer 2012. He had a history of open-angle glaucoma, for which he was medicated with Travatan Z (travoprost, Alcon) HS OU for the past three years. He described his glaucoma as “mild” and that his previous provider initiated therapy more as a “preventative” treatment option. His only systemic medication was lisinopril QD for hypertension.
Diagnostic Data
At his initial visit, best-corrected visual acuity was 20/20 OD, OS, OU through myopic (-3.00D) astigmatic and presbyopic correction. Pupils were round and reactive to light and accommodation with no afferent defect; physiologic anisocoria of 6mm was present in the right pupil and 5mm in the left in ambient light. Extraocular motilities were full in all positions of gaze.
Slit lamp examination of his anterior segments was unremarkable. Anterior chambers demonstrated wide-open angles OU, as estimated by the Van Herick method. Intraocular pressure by applanation tonometry measured 18mm Hg OD and 16mm Hg OS at 11:15 a.m. Central corneal thickness measured 529µm OD and 541µm OS.
Upon dilation, his crystalline lenses appeared clear in both eyes, with partial anterior vitreous separations OU. Stereoscopic evaluation of the optic nerves demonstrated cup-to-disc ratios of 0.55 x 0.85 OD with significant erosion of the inferior temporal neuroretinal rim and 0.50 x 0.55 OS. The inferior temporal rim margin OD sloped from the perioptic retinal nerve fiber layer (RNFL) horizontally to the cup, with lamina visible only in the center of the optic disc. There was a small amount of peripapillary atrophy (beta PPA) located in the inferotemporal aspect of this rim, adjacent to the neuroretinal rim notch.
His retinal vascular evaluations were normal OU, with no evidence of hypertensive retinopathy or retinal arteriolar narrowing in any quadrant of either eye. Macular evaluations also were normal, with loss of only the central foveal reflex. Peripheral retinas were normal with 360º of microcystoid present bilaterally.
We took stereo-optic nerve photos of the optic disc and Heidelberg Retina Tomograph-3 (HRT-3, Heidelberg Engineering) images of his optic nerves. HRT-3 images confirmed neuroretinal rim erosion OD (in the inferotemporal sector) as well as the cup-to-disc asymmetry between the eyes.
Given that this was the patient’s first visit to the office, and without any previous records to gauge his stability, I asked him to continue his current therapy and return in three months for further evaluation.
Follow-up
The patient returned as scheduled in November 2012 for threshold field studies, gonioscopy, and optic nerve and posterior pole SD-OCT imaging. At this visit, IOP was 16mm Hg OD and 15mm Hg OS at 2:30 p.m. Heidelberg Edge Perimetry (HEP, Heidelberg Engineering) demonstrated a pronounced arcuate field defect OD and a normal field OS. Reliability indices were good, indicating functional vision loss OD with no loss OS.
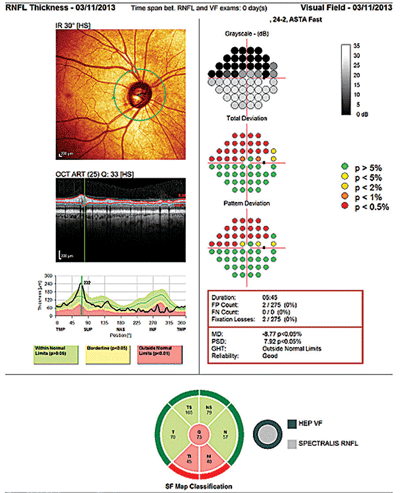
This patient’s optic nerve head photographs did not correspond with his objective test results, which showed thinning of the neuroretinal rim and corresponding field loss.
Spectralis OCT (Heidelberg Engineering) imaging showed a depressed RNFL in the inferotemporal sector in the right eye, consistent with the HRT-3 images and the clinical optic nerve appearance observed at the last visit. OCT of the left eye demonstrated a normal TSNIT double hump appearance with normal RNFL thicknesses 360º around the nerve.
My intern noted that the optic nerve photograph of the right eye, with what he estimated to be a cup-to-disc ratio of only 0.40 x 0.45, did not correspond to the HRT-3 and the Spectralis OCT image of the right eye.
By this visit, I had received a copy of the patient’s record. Threshold standard automated perimetry showed a couple of non-continuous points of field depression in the superior arcuate area OD, and a clean field OS. Cirrus OCT imaging also demonstrated a slightly depressed inferotemporal segment RNFL TSNIT graph in the right eye, and a normal RNFL appearance in the left.
The previous provider described the cup-to-disc ratios as 0.50 x 0.60 OD and 0.45 x 0.50 OS.
Discussion
This case raises the typical questions when a patient transfers care to your office: Is the patient stable? How severe is the glaucoma, and the resultant structural and functional damage? Are there compounding issues that threaten stability, such as vasculopathic disease or narrow angles?
What is the patient’s overall health? What is the patient’s compliance record? All of these are legitimate concerns.
How do you handle such a case? Here’s my advice.
First, be cautious about making any significant changes right away to the patient’s therapy or frequency of visits. For instance––although I had questions about the stability of this patient’s right optic nerve––I didn’t make any changes at the initial visit simply because, without his prior record, I had no documentation of his progress over the past few years. But I felt confident enough that, given the findings of the initial visit, there was no imminent threat to the optic nerve.
One exception to this rule is when you are firmly convinced that continuing the status quo would be detrimental to the patient. For example, if the patient has been seen only once a year, that is certainly something you need to change.
Also, realize that the patient’s perceptions of his or her situation may not actually reflect the severity of the situation. This patient mentioned that his previous provider implied that he had early glaucoma. That may have been what the doctor actually said—or it may have been his interpretation of what the doctor said. My take on the situation was that this was not early glaucoma, at least in the right eye.
So, we have to look to objective test results to tell us where the patient has been, and where he is possibly heading. (And that is the reason prior records are important in continuing the care of glaucoma patients.)
In a perfect world, objective tests should yield the same results on the same eye if nothing has changed. But the reality is, at least in objective testing of glaucoma, we have many different instruments available to us, produced by different manufacturers, which can look at the same optic nerve and “image” different things, and so produce different results.
In this case, for instance, my intern noted that the ONH photo OD did not match the HRT-3 and Spectralis OCT’s grading of the optic nerve OD. Obviously, we’re comparing apples to oranges here, but the patient’s right neuroretinal rim certainly appeared more robust in the optic nerve photos.
So, in looking at just one imaging technology compared to another, the results can and sometimes do look different, even when assessing the same nerve.1
Not surprisingly, this causes us to rely heavily on our own physical assessment of the optic nerve, and characterize that optic nerve based upon our experience.
Technology can play a tremendous role in helping us to determine stability over time, which is essential to successful glaucoma management.
Objectivity aside, keep in mind that one instrument may flag an optic nerve as “abnormal” whereas another objective instrument may flag the same optic nerve as “normal.”
But just how do we define what actually is (and isn’t) the optic nerve? I’ll address that question in a future column.
1. Yang B, Ye C, Yu M, et al. Optic disc imaging with spectral-domain optical coherence tomography: variability and agreement study with Heidelberg retinal tomograph. Ophthalmology. 2012 Sep;119(9):1852-7.

