 |
Hyphema is a common sequelae associated with blunt ocular trauma.1,2 It is a condition in which blood is present in the anterior chamber, including when it is suspended and no clot forms (microhyphema).1,3,4 Major complications of a traumatic hyphema include increased intraocular pressure (IOP), secondary hemorrhages, secondary glaucoma and blood staining of the cornea with decreased visual function.1,2,4 Management of these patients is directed at accelerating absorption of the blood to prevent complications; however, there are no current guidelines for treatment.
Examination
A 23-year-old Caucasian male presented from the emergency room after being hit in the right eye with a racquetball. He complained of mild pain, blurred vision and photophobia. A computed tomography (CT) scan was performed at the hospital and no orbital fractures were noted.
He was taking Flonase (fluticasone, GlaxoSmithKline) for seasonal allergies, but no other medications. The patient did have a history of strabismus surgery as a child with no lasting visual impact.
The patient had an entering uncorrected visual acuity of counting fingers at three feet with pinhole improving vision to 20/100 OD. A dilated and unreactive right pupil was detected with pupillary testing, and extraocular muscles showed a full range of motion with the patient reporting mild pain in right gaze. His IOPs were 14mm Hg OU. Anterior segment examination revealed 3+ diffuse conjunctival injection with two small subconjunctival hemorrhages. The cornea had 2+ diffuse microcystic edema and scattered punctate epithelial erosions. His anterior chamber was deep with 4+ cells and flare with a 0.5mm high hyphema settling at the bottom of the angle. The eye was dilated with one drop of atropine 1% in office. Posterior segment views were difficult due to the severe anterior chamber reaction, so a B-scan was performed to confirm the retina was attached.
Diagnosis
The patient was diagnosed with a traumatic hyphema and secondary iridocyclitis. He was placed on atropine 1% BID OD and Pred Forte (prednisolone acetate, Allergan) in his right eye every two hours. He was instructed to limit physical activity, sleep with his head elevated and avoid aspirin products. He returned the next day with improved vision of 20/30 but had a persistent hyphema and anterior chamber reaction. A posterior view was obtained and a three disc diameter area of commotio retinae was noted in the superior nasal retina. Treatment was continued as directed and the patient was followed closely over the next nine days until the hyphema and anterior chamber reaction resolved. At that time, the steroid was tapered appropriately with no rebound inflammation. At the one-month mark, gonioscopy showed no angle recession was noted. Vision returned to 20/20 and he had no lasting ocular damage.
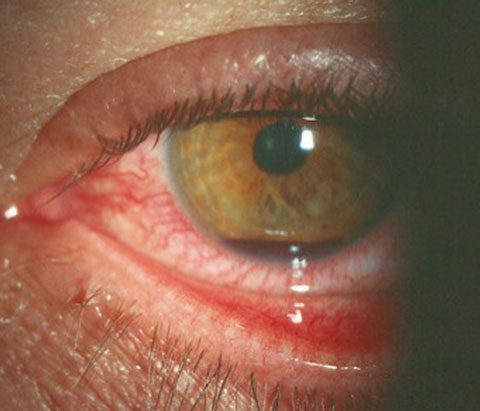 |
| Hyphema, seen here, is common after athletic injury or other trauma. Photo: Alan Kabat, OD. Click image to enlarge. |
Discussion
The estimated annual incidence of hyphema is 17 per 100,000, with males being impacted more often than females 3:1.1,4-7 Athletic injuries have become a common source for hyphemas, with a study showing that 39.2% of hyphemas occur from athletic injuries whereas work-related injuries only accounted for 9.9%.8 Rupturing of the iris and ciliary body vessels leading to a hyphema is thought to be caused either by compressive forces creating damage to the angle or rapidly rising pressure within the vasculature.1,9
Hyphemas are graded clinically by the amount of blood in the anterior chamber. If the blood cells are still suspended in the chamber, it is referred to as a microhyphema. Once the blood starts to settle in the anterior chamber, the hyphema is graded 1 to 4. A grade 1 hyphema is defined as blood filling less than one third of the chamber; one third to one half is a grade 2; and greater than one half is a grade 3 hyphema. When the blood completely fills the anterior chamber, it is considered a grade 4 hyphema. When a grade 4 hyphema turns dark it is considered an “eight-ball hyphema” and carries a much worse prognosis than a bright red grade 4 hyphema.1
Investigators estimate that about 30% of all traumatic hyphemas will present with an increase in IOP, which can be a significant risk factor for vision loss.10 Increased IOP is caused by anterior synechiae formation, increased outflow resistance and fibrosis of the trabecular meshwork. Secondary glaucoma may develop weeks to years after a hyphema and occurs in up to 20% of cases.1,4 Patients with larger hyphemas have an increased risk of secondary glaucoma; however, any amount of blood in the anterior chamber can be associated with elevations in IOP.4
Secondary hemorrhages usually occur two to seven days after the initial trauma and are a result of lysis and retraction of the blood clot and fibrin at the ruptured blood vessel. Patients have a 35% chance of having a rebleed during this time frame, and it can be noted clinically by an increase in the size of the hemorrhage or by fresh red blood overlying the darker clot.4,9,11 Secondary hyphemas can increase the risk of IOP spikes and corneal blood staining. The incidence of corneal blood-staining varies between 2% and 11% with an increased risk in patients with larger hypehmas, rebleeding, prolonged clot duration, sustained increased IOP and previous corneal endothelial cell dysfunction.1,4,11 Research shows that patients with an IOP equal to or greater than 25mm Hg for six or more days are at a significantly higher risk of having corneal blood staining and therefore reduced visual function.1,4,11
Treatment
Numerous controversies in management of hyphemas exist, and standardized guidelines for treatment have yet to be determined. However, the most important factor in treating traumatic hyphemas is to stabilize the eye and accelerate the absorption of the blood to prevent complications. Patients should be advised of quiet ambulation and resting at a 30-degree angle to promote settling of the hyphema. Patients should avoid any substances that will delay clotting, including aspirin.
Cycloplegics are often used in treatment of a traumatic hyphema (atropine 1% BID). They help improve comfort in patients with a secondary iridocyclitis, decrease the risk of posterior synechiae and theoretically reduce secondary hemorrhages by immobilizing the iris and ciliary body and stabilize the blood-aqueous barrier.1 Studies show, however, that cycloplegics do not improve visual outcomes or reduce the risk of rebleeding.4
Corticosteroids, such as prednisolone acetate 1% QID to Q2H, are also important tools when managing hyphemas. Steroids work by stabilizing the blood-aqueous barrier and decreasing the amount of plasminogen, a mediator of fibrinolysis, into the anterior chamber. It can also prevent posterior synechiae formation and reduce concurrent inflammation.1,4 One study shows patients treated with topical steroids had a 5% rebleeding rate whereas the non-treated group had a 12% incidence of rebleeding.12
Ocular hypotensive agents are an indicated treatment in patients who have an increase in IOP.1 Topical beta-blockers (timolol 0.5%), alpha agnoists (brimonidine 0.1%) and carbonic anhydrase inhibitors (brinzolamide 1%) can be used to control elevated IOPs. Prostaglandins are avoided due to the amount of inflammation already associated with the traumatic event. Oral acetazolamide is also avoided as it promotes sickling of erythrocytes in patients with the sickle-cell trait.1
The last and most controversial treatment option is antifibrinolytic agents such as aminocaproic acid. These systemic medications can significantly lower the rate of rebleeding by stabilizing the interface between the clot and vessel wall by inactivating plasmin and preventing clot lysis.1,4 Studies show a decrease in rebleeding rates from 4% to 33%; however, aminocaproic acid can cause nausea and vomiting and also prolongs clot duration, which could put patients at an increased risk for prolonged IOP elevation or blood staining.1,13
Dr. Schuiteman finished her primary care residency last July at Indiana Optometry. She currently practices in South Bend, IN.
1. Bansal S, Gunasekeran D, Ang B, et al. Controversies in the pathophysiology and management of hyphema. Surv Ophthalmol. 2016;61(3):297-308. 2. Ghafari A, Siamian H, Aligolbandi K, Vahedi M. Hyphema caused by trauma. Medical Archives. 2013;67(5):354. 3. Vincent S, Alt J, Robinson T. Traumatic hyphema in an intercollegiate baseball player: a case report. J Athletic Training. 1999;34(1):25-8. 4. Walton W, Hagen S, Grigorian R, Zarbin M. Management of traumatic hyphema. Surv Ophthalmol. 2002;47(4):297-334. 5. Shingleton B, Hersh P, Kenyon K, Cook L. Eye trauma. 1999. St. Louis, MO: Mosby Year Book;104-114. 6. Filipe J, Barros H, Castro-Correia J. Sports-related ocular injuries. Ophthalmology. 1997;104(2):313-8. 7. Schein O, Hibberd P, Shingleton, et al. The spectrum and burden of ocular injury. Ophthalmology. 1988;95(3):300-5. 8. Kearns P. Traumatic hyphaema: a retrospective study of 314 cases. Br J Ophthalmol. 1991;75(3):137-41. 9. Romano P, Robinson J. Traumatic hyphema: a comprehensive review of the past half century. Binocular Vision & Strabismus Quarterly. 2000;15(2):175-86. 10. Crouch ER Jr, Williams PB. Trauma: ruptures and bleeding. In:Tasman W, Jaeger EM (eds). Duane’s Clinical Ophthalmology. Philadelphia; JB Lippincott;1993:1–18. 11. Yanoff M. Ophthalmology. 3rd ed. Philadelphia. Elsevier Mosby;2009:1188. 12. Ng C, Strong N, Sparrow J, Rosenthal A. Factors related to the incidence of secondary haemorrhage in 462 patients with traumatic hyphaema. Eye. 1992;6(3):308-12. 13. Crouch E. Topical aminocaproic acid in the treatment of traumatic hyphema. Arch Ophthalmol. 1997;115(9):1106. |

