 How can I differentiate between diffuse lamellar keratitis (DLK) and central toxic keratopathy (CTK) in a post-LASIK patient?
How can I differentiate between diffuse lamellar keratitis (DLK) and central toxic keratopathy (CTK) in a post-LASIK patient?
DLK and CTK are somewhat similar complications following a LASIK procedure, but they are distinct entities that require different treatment approaches.
• DLK. Of the two conditions, DLK is more common and typically appears within one to three days after LASIK. It presents as a diffuse or patchy infiltration in the interface under the flap. It is confined to the interface and does not extend anterior or posterior to it. Additionally, it is not focal; rather, it is spread throughout the interface––hence the term diffuse. DLK often produces foreign body sensation, and patients may experience blurred vision.
Ophthalmologist Robert K. Maloney, MD, of Los Angeles, says that the etiology of DLK is currently unknown, but it’s “probably caused by some debris or foreign material that gets into the interface and causes an inflammatory response.”
“When you see DLK, you have to differentiate it from infectious keratitis,” Dr. Maloney says. Infectious keratitis classically presents with one or several areas of inflammation that extend anteriorly into the flap and posteriorly into the remaining stroma. Additionally, you’ll see a “halo of inflammatory cells because these cells are migrating to the site of infection,” he says.
| |
|
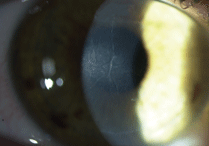
Central toxic keratopathy (CTK), shown here, is distinguished from diffuse
lamellar keratitis (DLK) because it is focal. DLK, as its name implies, is diffuse. Photo: Robert K. Maloney, MD. |
• CTK. Far less common than DLK, CTK typically starts three to nine days after LASIK and presents as a dense, central opacification of the cornea with striae. The opacity extends either anteriorly into the flap, posteriorly into the stroma, or both.
CTK is usually associated with a hyperopic shift—perhaps as high as +12—although +1 to +3 is far more common. Patients may also have a reduction in best-corrected vision to 20/40 or so due to the irregularity of the cornea.
CTK is generally non-inflammatory, so when doctors see it three to five days following surgery, they naturally believe that they are dealing with an infection due to the white discoloration of the central cornea. However, it can be differentiated from an infection because its boundary appears sharply demarcated (in contrast to infectious keratitis) and there are very few inflammatory cells. Additionally, the peripheral cornea is relatively clear with CTK.
“What’s confusing about CTK is that it often coexists with DLK, so frequently patients will have a few days of DLK and then show up with CTK,” Dr. Maloney says. This has led some authors to consider CTK as an advanced form of DLK.
However, Dr. Maloney believes that CTK is a different entity, as it’s been observed in patients who didn’t have DLK or who had very mild DLK. “Rather than CTK being a manifestation of DLK, more likely it’s the opposite,” says Dr. Maloney.
Unlike DLK, CTK is not treated with corticosteroids. But do treat any coexisting DLK with steroids until it resolves, then discontinue steroid use.
While DLK resolves in a week or less, CTK can last much longer—up to nine months in some cases. “The cornea clears up eventually,” Dr. Maloney reassures, though he adds that some patients are still left with a hyperopic shift. If that occurs, LASIK enhancement can be performed without fear of CTK recurrence.
Dr. Maloney’s approach to CTK is simply to follow it. “The hardest part for doctors is to explain to the patient that it’s going to last for three to nine months. Counsel them to be patient. It will get better—it’s just a matter of time.”

