 On July 6, I received a call from a local urgent care doctor concerned about a 46-year-old white female patient he had seen over the July 4 holiday weekend.
On July 6, I received a call from a local urgent care doctor concerned about a 46-year-old white female patient he had seen over the July 4 holiday weekend.
The patient initially presented to him eight days earlier with a right eye that had been red for the previous four days. At that time, the eye was not painful nor was the vision blurred, so the doctor diagnosed a nondescript conjunctivitis. He prescribed Polytrim (polymyxin B/trimethoprim, Allergan) one drop q.i.d. O.D.
The patient apparently was compliant with her drops, and presented again to the urgent care doctor on July 5. This time, however, she complained of blurred vision and a painful, achy sensation in the right eye. In addition, there was no reduction of the redness that precipitated her initial visit to the urgent care center.
The physician gave her a prescription for Vigamox (moxifloxacin, Alcon) to use q4h until she saw me the next morning for evaluation.
I received the call from the urgent care doctor advising me of her appointment. When she presented to our office on the morning of July 6, the history she gave matched what I’d already been given. She reported that she began to notice a decline in her vision on July 4 with increasing pain. Current medications included only paroxetine q.d., and she reported no allergies to medications.
Diagnostic Data
Her entering visual acuity was 20/50+ O.D. and 20/20- O.S., with no improvement in the right eye through pinhole. Pupils were somewhat unequal—the right was 5.5mm and the left was 4mm in ambient light. The right pupil did not constrict briskly, but there was no afferent defect by direct and reverse Marcus Gunn pupil testing. Extraocular motilities were full in all positions of gaze.
Slit lamp examination of the anterior segment of the left eye was unremarkable. That of the right showed a mildly cloudy cornea with mild striate keratopathy and keratic precipitates on the visual axis. The anterior chamber was characterized by 3+ cell and 2+ flare.
Estimation of anterior chamber angles by Van Herick method was open +4 in each eye. Intraocular pressure measured 53mm Hg O.D. and 19mm Hg O.S. at 9:48 a.m. Her crystalline lenses were clear in both eyes.
I deferred a dilated fundus examination at this visit due to time constraints, but a nondilated fundus exam did not reveal any posterior segment inflammation, including vitritis, pars planitis or posterior pole inflammation. I estimated her cup-to-disc ratios to be 0.20 x 0.20 O.D. and O.S. Although macular details were difficult to assess in the right eye, there were no apparent posterior pole abnormalities.
Diagnosis and Management
When receiving another provider’s referral of a patient with a stubborn red eye, many possibilities exist as to the etiology of the problem.
But when a patient isn’t responding to treatment, and pain and blurriness are increasing, most primary care doctors are quick to refer the patient out—usually with a concern about the possibility of angle closure glaucoma.
More often than not, when I’ve seen patients referred in similar circumstances, the diagnosis usually is not acute angle closure. Nor was it in this case, as her angles were grade 4 open and essentially unoccludable. In this case, I was expecting a viral etiology—probably herpes simplex viral keratitis—based on the history reported by the referring physician.
However, as the clinical examination indicated, the patient presented with an anterior uveitis that had mushroomed to the point where the keratic precipitates and elevated IOP were interfering with her vision and causing increased discomfort.
So, although this is not a primary case of glaucoma, it is a (hopefully) temporary form of glaucoma related to the uveitis.
In further questioning the patient, she did report a flare-up of bilateral hip bursitis, but this flare was “nothing more than a usual” flare-up, she said, indicating that this may be a more chronic condition. There was no history of rheumatoid, sarcoid, scleroderma or other collagen vascular disorders, nor did she have any physical complaints associated with these conditions.
While it is known that patients with a propensity to develop glaucoma are at a higher risk of being steroid responders, we must also realize that when patients have a significant anterior uveitis, physical changes occur in the trabecular meshwork that result in diminished outflow. These changes typically are from accumulation of cellular debris and possibly inflammation of the trabeculum, further impairing outflow. So it’s important in such cases to begin aggressive topical steroid therapy. The worry that IOP may increase even further should be secondary to reducing the inflammation.
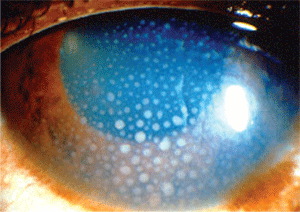
This patient presented with intraocular pressure of 53mm Hg. The referring doctor suspected angle closure glaucoma.
Photo: William Potter, O.D.
That said, pressure reduction must also be achieved, and with IOPs in the 50s, it’s prudent to begin a course of IOP-lowering agents as well. Accordingly, I gave the patient two drops of 0.25% scopolamine and one drop of Travatan (travoprost, Alcon) in the office. I also gave her a prescription for 0.25% scopolamine t.i.d., Pred Forte (prednisolone acetate 1%, Allergan) q1h while awake and 0.5% timolol q.d. I asked her to return in three days.
The patient presented for follow-up five days later, at which time uncorrected visual acuity was 20/25- O.D. and 20/20- O.S. The right pupil was pharmacologically dilated. Intraocular pressure measured 18mm Hg O.D. and 16mm Hg O.S at 9:55 a.m.
Her right cornea demonstrated no striate keratopathy, and the keratic precipitates were greatly reduced in size, density and number. The anterior chamber was characterized by 2+ cell and 1+ flare.
Dilated fundus examination revealed healthy, plush, well-perfused neuroretinal rims with 0.20 x 0.20 cupping O.D and O.S. As in the initial visit, there was no evidence of posterior segment inflammation, and her peripheral retinal examination was unremarkable.
At this point, I discontinued the 0.5% timolol, reduced the 0.25% scopolamine to q.h.s. and reduced the Pred Forte to q4h, and asked her to return in three days.
On follow-up, uncorrected acuity was 20/20- O.D. and 20/20 O.S. IOP was 13mm Hg O.D. and 14mm Hg O.S. There was no striate keratopathy visible, and the keratic precipitates were further reduced. The anterior chamber was characterized by 1+ cell and trace flare. I asked her to continue the Pred Forte q4h and to decrease the 0.25% scopolamine to q.o.h.s., and to come back again in two weeks.
I also took this opportunity to summarize my consultation findings in a letter to the referring physician, and to report that the patient is doing well. Though she currently has no overt symptoms out of the ordinary related to collagen vascular diseases, I did suggest to the referring physician that he should keep in mind that an underlying systemic etiology might be at play here, and to follow his clinical intuition as to whether or not she needs to be systemically evaluated for underlying disease.
Discussion
Uveitis is a common finding in clinical practice that may be caused by many different etiologies.1 The hallmark presentation is a painful, photophobic, red eye. Clinical findings include cells and flare in the anterior chamber, circumlimbal injection and poorly reactive pupils.
Elevated IOP can become an issue when the uveitis progresses significantly either in duration or severity. When this happens, it’s critical to understand that the elevated IOP is due to the inflammation, and the inflammation must be controlled—usually with steroids and cycloplegics. If need be, IOP-lowering agents may be required until the inflammation is reduced and the pressure declines secondary to inflammation reduction.
Many of the first-line glaucoma agents available can be used to lower IOP in these cases. We tend to use beta blockers (when not contraindicated) as well as prostaglandin analogues because recent studies show that prostaglandins are safe to use with a concurrent uveitis.2
1. Kanski JJ, Bowling B. Clinical Ophthalmology: A Systematic Approach. 7th ed. Edinburgh: Elsevier Saunders; 2011:402-4.
2. Chang JH, McCluskey P, Missotten T, et al. Use of ocular hypotensive prostaglandin analogues in patients with uveitis: does their use increase anterior uveitis and cystoid macular oedema? Br J Ophthalmol. 2008 Jul;92(7):916-21.

