A patient presents after being exposed to dust mites in her office building. The allergen exposure causes substantial amounts of histamine to be released, dilating her conjunctival microvasculature and creating conjunctival hyperemia and chemosis. She’s suffering with intense ocular itching, burning and profuse tearing, and she wants relief now.

It’s likely you encounter patients like this in your office frequently—some recent studies suggest that up to 40% of the population in developed countries experience symptoms of ocular allergy, or allergic conjunctivitis (AC).1 Unfortunately, this common condition is often underdiagnosed and undertreated until it reaches severe levels.2
Just a decade ago, mast cell stabilizers and antihistamines were the primary therapy for AC––with steroids reserved for non-responsive cases. Today, with our understanding of ester steroids and their efficacy of breaking the allergic cascade in both early and late phases of the allergic response, many astute optometrists are using steroids as first-line therapy.
In this article, we’ll review the use of anti-inflammatory therapy for ocular allergies, particularly the judicious use of topical steroids and nonsteroidal anti-inflammatories (NSAIDs) in AC.
Stepping It Up
When patients present with rhinitis, itching, foreign body sensation, conjunctival chemosis, hyperemia, papillary conjunctivitis, tearing and discharge, we need to consider AC. Acute and chronic symptoms and signs need to be evaluated by thorough patient history and exam.
Because ocular allergies can present with such a wide array of symptoms at varying levels of severity, the best route to take is often a stepwise approach to treatment—from non-medical treatment, including cold compresses and artificial tears, to antihistamine/mast cell stabilizers, NSAIDs and ester-based steroids.
Typically used as the first line of defense, antihistamine/mast cell stabilizers are fast and effective. These dual-acting medications block the effects of histamine and prohibit mast cells from releasing the chemicals responsible for allergy symptoms. When symptoms continue to persist or are particularly severe, adding an anti-inflammatory can help enhance the effects of the antihistamine/mast cell stabilizers until the patient’s condition improves.
For severe symptoms, a top-down approach or combination therapy allows you to target symptoms effectively without overmedicating the patient.
Steroids
For mild, chronic AC, continuous use of combination antihistamine/mast cell stabilizers typically is the treatment of choice because of its safety profile. However, when the patient is experiencing more frequent or more severe symptoms, that’s when you may want to consider a steroid. Because of its safety profile and efficacy against inflammatory cells, loteprednol etabonate in ophthalmic suspensions of 0.2% (Alrex, Bausch + Lomb) or 0.5% (Lotemax, Bausch + Lomb) is a steroid of choice for many doctors.3
A new addition to the market, Lotemax gel has quickly become another popular choice because of several advantages it offers: It does not require shaking; contains 70% less preservatives than its suspension; and contains two moisturizers, propylene glycol and glycerin.4-6 The engineered mucoadhesive technology turns the gel into a liquid when placed on the eye, helping it to adhere and reducing gel-related blur.4,5,7,8

Another option is fluorometholone, a steroid with low intraocular absorption. In a study of patients with seasonal AC, fluorometholone was found to be highly effective in reducing itching, tearing and conjunctival hyperemia over time and did not exhibit any statistically significant changes in IOP.9
Steroids block most mediators of inflammation and work effectively in the acute phase of AC. By inhibiting phospholipase A, they block the arachidonic acid pathway, preventing the synthesis of prostaglandins and leukotrienes.10 They impede the migration of leukocytes to inflammatory sites, minimizing the release of inflammatory mediators from macrophages.
NSAIDs
But what do you do when a steroid is contraindicated and an antihistamine/mast cell stabilizer just isn’t effective enough to treat acute severe symptoms? Here’s where a combination approach may work best. Topical NSAIDs can be a useful, short-term treatment option for AC, relieving the pain associated with inflammation.11
Using topical NSAIDs along with cold compresses for one week can help make the patient more comfortable, while you can manage the chronic allergies with antihistamines and antihistamine/mast cell stabilizers, such as Bepreve (bepotastine besilate, Bausch + Lomb), Lastacaft (alcaftadine, Allergan), Patanol and Pataday (olopatadine hydrochloride, Alcon) and Elestat (epinastine, Allergan).
NSAIDs relieve itching, but they don’t block histamine and hamper only a portion of the inflammatory cascade. They inhibit cyclooxygenase, an enzyme that converts arachidonic acid into lipid mediators of inflammation, such as prostaglandins.11 This mechanism of action reduces prostaglandin synthesis.12,13
Research has shown that Acular LS and Acuvail (ketorolac tromethamine, Allergan) is effective for allergy treatment because of its secondary effects on the production of lipid inflammatory mediators and itch symptoms.14,15
In 2009, researchers in Japan looked at Bromday (bromfenac, Bausch + Lomb), an NSAID indicated for the treatment of postoperative inflammation and reduction of ocular pain in patients who have undergone cataract extraction.16
This examiner-blinded study involved 22 patients with seasonal AC signs and symptoms. They treated one eye with bromfenac and the other eye with Alamast (pemirolast potassium, Vistakon), a standard mast cell stabilizer. Their results indicated that bromfenac is as safe and effective as pemirolast potassium for the treatment of seasonal AC.16 (Note: This does not constitute endorsement by the manufacturers outside of the approved indication. Consult package insert for important safety information.)
How Much and How Often?
Dosage and frequency should be based on inflammatory severity. Pulsed therapy is appropriate if a more aggressive approach is needed—an effective dose must be used for the shortest time course. Pulse dosing for no longer than 14 days with steroids is efficacious for severe AC, but there are some patients who are resistant and require other forms of initial therapy.
One
of the concerns for many practitioners in treating allergic
conjunctivitis with steroids is the potential for IOP increase. You
should monitor IOP after 10 days when prescribing any steroid—even those
we affectionately know as “kinder, gentler” ester-based steroids, such
as loteprednol. Any topical steroid use, including use of ester-based
steroids, with contact lenses can cause a rise in IOP with prolonged
use. While it’s always best to err on the side of caution by taking
these safety measures, some recent research has suggested that IOP
elevation is not a major problem with ester steroids.3
NSAIDs can be used successfully for moderate to severe AC if steroids are contraindicated. However, NSAIDs are not as effective as steroids because they do not directly decrease histamine release from mast cells.15 They can successfully reduce pain associated with inflammation and, when used synergistically with an antihistamine/mast cell stabilizer, can serve as an effective therapy. Acular used QID has shown effectiveness for allergic conjunctivitis.17
Under Pressure
Clinical Presentations
Vernal keratoconjunctivitis (VKC), atopic keratoconjunctivitis (AKC), giant papillary conjunctivitis (GPC), seasonal allergic conjunctivitis (SAC) and perennial allergic conjunctivitis (PAC) are the main types of ocular allergies that challenge eye care providers.
Keratoconjunctivitis
VKC and AKC are usually chronic, bilateral and severe—in extreme cases, these conditions can cause damage to the ocular surface resulting in corneal scarring. Aggressive treatment is recommended for both of these forms of allergic conjunctivitis.
• VKC. Usually diagnosed in the juvenile and teen years during the springtime, VKC occurs more commonly in males than females. Manifesting conjunctival chemosis and hyperemia of the lower eyelid more than the upper palpebral conjunctiva, in extreme cases VKC can scar the cornea and lead to vision loss, if not treated. Symptoms include itching, burning, discharge, cobblestone appearance of the tarsal conjunctiva, and Horner-Trantas dots at the limbal area.18
Oral and topical antihistamines and mast cell stabilizers are indicated, but are most useful after initial inflammation is minimized.19 Depending on presentation severity, Lotemax or Pred Forte may be used QID for several weeks, followed by BID or TID dosing for several weeks. Alrex may be used longer term due to its improved safety profile and/or initially in cases of less severity.3
• AKC. AKC may be a hereditary condition, an allergic hypersensitivity to an allergen prompting an IgE-mediated reaction. It can affect patients year round, particularly those who are hypersensitive or hyperallergenic. Atopic syndrome patients often have asthma, food allergies, eczema or atopic dermatitis, involving the eyelids and face. Conjunctival chemosis and papillae are common, and aggressive treatment is recommended because of the potential for conjunctival scarring and loss of vision due to frequent corneal complications.18,20-22
While this is a rare condition, it is the most debilitating type of allergic conjunctivitis—patients suffer with AKC for many years and have high rates of visual impairment.22 In addition to prophylactic use of antihistamine/mast cell stabilizers, topical corticosteroids remain the standard treatment for AKC in addressing acute symptoms and exacerbations.22

1. Vernal keratoconjunctivitis. Photo: M.S. McMeekin, OD.
However, because of the chronic nature of this disease, there is concern about the complications of long-term topical steroid use in these patients. Recent research has suggested that topical cyclosporine A may be useful as a corticosteroid-sparing agent and effective in improving AKC symptoms.22,23
Giant Papillary Conjunctivitis
GPC may occur in the presence of soft, silicone hydrogel and gas-permeable contact lens wear, exposed sutures, scleral and prosthetic contact lenses, and with floppy eyelid syndrome. Papillae occur on the upper lids’ tarsal plate area. Papillae larger than 0.3mm in diameter are considered abnormal, and are considered giant at 1mm diameter or more.
Symptoms and signs include itching and redness, mucous discharge, contact lens discomfort and intolerance, and contact lens coating and excessive movement.
The causative factor must be addressed. If the condition is contact lens induced, standard care involves refitting the patient into daily disposables or recommending hydrogen peroxide care systems with frequent lens replacement. Mast cell stabilizers were once the mainstay of topical medication therapy.
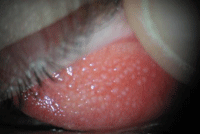
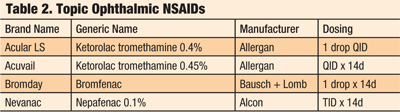
2. Giant papillary conjunctivitis. Photo: Tim Welton, OD.
Today, antihistamine/mast cell stabilizers and short-term steroid use are preferred treatments. In moderate, severe or persistent cases, topical steroids effectively reduce the inflammatory response. Typical dosage of
Lotemax is four to six times per day for one week or longer, followed by BID dosing until the condition is effectively controlled. FML also has demonstrated effectiveness in treating GPC.24
Seasonal Allergic Conjunctivitis
SAC is mostly due to airborne pollens produced by plants that cause hay fever. The allergens attach to IgE receptors, releasing histamine and other inflammatory mediators that cause hyperemia, itching, burning, swelling and tearing of the eyes and often irritation of the nasal mucosa.19 Allergic rhinoconjunctivitis is more common in patients who have other allergic conditions or atopy.25
Severe symptoms often require the use of topical NSAIDs or steroids, along with antihistamine/mast cell stabilizers. Alrex is valuable for the temporary relief of seasonal allergies, and is the only topical steroid approved for the relief of SAC and PAC.3 If patients have trouble instilling drops or have medication preservative issues, nighttime application of Lotemax preservative-free ointment can be used as an alternative.
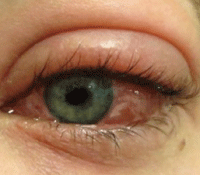
3. Seasonal allergic conjunctivitis. Photo: Michael Murphy, OD.
Perennial Allergic Conjunctivitis
While PAC tends to be milder than the seasonal variety, it is a chronic condition. Because it is commonly related to indoor allergens like dust mites, molds, detergents, carpeting, fabrics, indoor plants and animal dander, consulting an allergy specialist is often recommended to help identify potential causes and triggers.
Environmental modifications are the mainstay of treatment—helping the patient avoid or limit exposure to the allergen. In the home, this may include the use of indoor air filters, air conditioning, isolating pets to certain areas and thoroughly cleaning dust, dander and molds. On the road, replacing auto cabin air filters can help reduce indoor air pollution and driving with the windows up can help reduce exposure to other types of allergens.
Teaching patients not to rub their eyes and to use copious amounts of artificial tears and cool compresses can help reduce initial ocular allergy symptoms, but many patients require medical intervention during allergy distress, including short-term pulse therapy (three to four days) with a steroid or an NSAID.
The array of available anti-inflammatory medications has enhanced the treatment of ocular allergies. Combining the advantages of anti-inflammatory therapy with traditional antihistamine/mast cell stabilizers has evolved the treatment protocol. Severe ocular allergies presentations can be “tamed” with anti-inflammatory application, allowing effective use of antihistamine/mast cell stabilizers. Less severe presentations may also acheive maximal therapy with these full topical medication combinations. Ophthalmic practitioners and patients can benefit from these newer therapeutic techniques. n
Dr. DeVivo is a clinical director of Lasik Vision Centers of Cleveland in Independence, Ohio, and the staff optometrist at Ophthalmic Physicians Inc., a private group ophthalmology practice in Mentor, Ohio. Dr. Scheid is an associate clinical professor at SUNY College of Optometry in New York and is in private practice in Merrick, NY.
1. Bartlett J. Treatment of seasonal allergic conjunctivitis [Promotional supplement supported by Bausch + Lomb. 2011. Available at:
http://walmartod.com/suppliers/bausch-and-lomb/pdf/Alrex_ODinsertion.pdf.
2. Singh K, Axelrod S, Bielory L. The epidemiology of ocular and nasal allergy in the United States, 1988-1994. J Allergy Clin Immunol. 2010 Oct;126(4):778-83.
3. Ilyas H, Slonim CB, Braswell GR, et al. Long-term safety of loteprednol etabonate 0.2% in the treatment of seasonal and perennial allergic conjunctivitis. Eye Contact Lens. 2004 Jan;30(1): 10-3.
4. Fong R, Leitritz M, Siou-Mermet R, Erb, T. Loteprednol etabonate gel 0.5% for postoperative pain and inflammation after cataract surgery: results of a multicenter trial. Clin Ophthalmol. 2012;6:1113-24.
5. Lotemax gel [package insert]. Tampa, FL: Bausch + Lomb; 2012.
6. Lotemax [package insert]. Tampa, FL: Bausch + Lomb; 2006.
7. Shaikh R, Singh TR, Garland MJ, et al. Mucoadhesive drug delivery systems. J Pharm Bioallied Sci. 2011 Jan-Mar;3(1):89-100.
8. Coffey MJ, Davio SR. Viscoelastic and sedimentation characterization of loteprednol etabonate ophthalmic gel 0.5%. Poster presented at: Association for Research in Vision and Ophthalmology (ARVO) meeting; May 6-9, 2012; Fort Lauderdale, Fla.
9. Leonardi A, Papa V, Milazzo G, Secchi AG. Efficacy and safety of desonide phosphate for the treatment of allergic conjunctivitis. Cornea. 2002 Jul;21(5):476-81.
10. Sorenson DK, Kelly TM, Murray DK, Nelson DH.
Corticosteroids stimulate an increase in phospholipase A2 inhibitor in human serum. J Steroid Biochem. 1988 Feb;29(2):271-3.
11. McAuley DF. Ophthalmic—nonsteroidal anti-inflammatories, 1993-2012. GlobalRPh Inc. Available at: www.globalrph.com/ophthalmic_nsaid.htm. Accessed January 24, 2013.
12. Kim SJ, Flach AJ, Jampol LM. Nonsteroidal anti-inflammatory drugs in ophthalmology. Surv Ophthalmol. 2010 Mar-Apr;55(2):108-33.
13. Mieler WF. Update regarding use and benefit of NSAIDs in ophthalmology. Presented at: the International Symposium on Ocular Pharmacology and Therapeutics (ISOPT); December 9-11, 2010; Macau, China.
14. Raizman MD. Results of a survey of patients with ocular allergy treated with topical keratolac tromethamine. Clin Ther. 1995 Sept-Oct;17(5); 882-90.
15. Pflugfelder S, O’Brien TP, Donnenfeld ED, Karpecki PM, et al. Prevention and management of ocular inflammation across the ophthalmic spectrum: proceedings from expert roundtable discussion. Georgetown, Conn: MedEdicus. Nov 1, 2012.
16. Miyake-Kashima M, Takano Y, Tanaka M, et al. Comparison of efficacy of bromfenac sodium 0.1% ophthalmic solution and 0.1% pemirolast potassium for the treatment of allergic conjunctivitis. Jpn J Ophthalmol. 2004 Nov-Dec;48(6):587-90.
17. Raizman MB. Results of a survey of patients with ocular allergy treated with topical ketorolac tromethamine. Clin Ther. 1995 Sep-Oct;17(5):882-90.
18. Khurana AK. Comprehensive Ophthalmology. 4th ed. Kent, UK: Anshan Publishers;2007.
19. Bielory L, Friedlaender MH. Allergic conjunctivitis. Immunol Allergy Clin North Am. 2008 Feb;28(1):43-58, vi.
20. Ono SJ, Abelson MB. Allergic conjunctivitis: update on pathophysiology and prospects for future treatment. J Allergy Clin Immunol. 2005 Jan;115(1):118-22.
21. Bielory L. Allergic and immunologic disorders of the eye. Part II: ocular allergy. J Allergy Clin Immunol. 2000 Dec;106(6):1019-32.
22. Akpek EK, Dart JK, Watson S, et al. A randomized trial of topical cyclosporin 0.05% in topical steroid-resistant atopic keratoconjunctivitis. Ophthalmology. 2004 Mar;111(3):476-82.
23. González-López JJ, López-Alcalde J, Morcillo Laiz R, et al. Topical cyclosporine for atopic keratoconjunctivitis. Cochrane Database Syst Rev. 2012 Sep 12; 9:CD009078. doi: 10.1002/14651858.CD009078.pub2.
24. Khurana S, Sharma N, Agarwal T, et al. Comparison of olopatadine and fluorometholone in contact lens-induced papillary conjunctivitis. Eye Contact Lens. 2010 Jul;36(4):210-4
25. Sullivan JB, Jr., Krieger GR. (2001). Clinical Environmental Health and Toxic Exposures. 2nd ed. Philadelphia: Lippincott Williams & Wilkins; 2001:341.
26. Gong L, Sun X, Qu J, et al. Loteprednol etabonate suspension 0.2% administered QID compared with olopatadine solution 0.1% administered BID in the treatment of seasonal allergic conjunctivitis: a multicenter, randomized investigator-masked, parallel group study in Chinese patients. Clin Ther. 2012 Jun;34(6):1259-72.

