Thinking has literally gotten deeper in refractive surgery with the release of studies on penetrating procedures that appear to optimize visual outcomes while treating diseased corneas. Conventional refractive surgery also continues to move forward on the research front, focusing on the needs of presbyopes and the importance of osmolarity for refractive surgery candidates. Of course, cataract—the leading cause of blindness worldwide that is expected to affect an estimated 40 million people by 2020—remained a primary concern. Important studies focused on prevention.
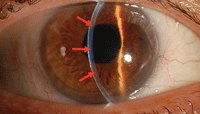
New research suggests that the optical quality might be better in DALK because of less peripheral irregularities. This photograph illustrates a post-surgical DALK eye following suture removal. The arrows identify the graft-host interface.
Photo: Holly Hindman, M.D.
Improving Penetrating Corneal Procedures
Deep anterior lamellar keratoplasty (DALK) does not involve the full transplantation used during penetrating keratoplasty (PKP). The patient’s endothelium is left in place, resulting in less risk of rejection, faster healing and improved tissue stability.
DALK has not always produced ideal optical results. However, surgeons from Seoul, Korea, reported positive visual outcomes on keratoconus patients who had undergone DALK.13/A156
The medical records of 26 transplantation patients were retrospectively reviewed, revealing the results of nine DALK procedures with same-size grafting, five PKP procedures with same-size grafting and 12 PKP procedures with 0.25mm oversize grafting (PKPo) for keratoconus. Astigmatism tended to be lower in DALK than in PKP or PKPo, a difference that was marginally significant. Corneal irregularity indices measured at 3mm or 5mm in the DALK group were less than those in the PKP groups at the final follow-up. Highlighting these findings, the surgeons said the optical outcomes of DALK with same-size grafts for keratoconus were comparable to those of PKP. The optical quality might be better in DALK because of less peripheral irregularities.
In a related study, Descemet’s membrane endothelial keratoplasty (DMEK) was used with some success for corneal endothelial diseases through the selective replacement diseased endothelium.20/A163 The case series involved nine consecutive patients and relied on intraoperative OCT (iOCT) to visualize the graft within the anterior chamber during orientation and attachment to the posterior cornea.
The research, based in Germany, found that the use of iOCT helped locate and orientate DMEK grafts within the recipient’s anterior chamber. This procedure, although challenging, appeared to offer the potential for good visual acuity because no interface was present in the stroma, such as what would be found in Descemet’s scraping endothelial keratoplasty (DSEK).
A new surgical procedure, superficial anterior lamellar keratoplasty (SALK), transplants only the anterior corneal stroma in the treatment of corneal dystrophies, such as epithelial basement membrane dystrophy, stromal dystrophy, and lattice dystrophy.
One study showed that the procedure can greatly improve vision, producing results that peak six months after surgery.18/A161
Conventional Refractive Surgery
As always, numerous reports covered conventional surgical correction of vision. One examined the benefits of corneal inlays for the correction of presybyopia.1720 The inlays can be implanted in the non-dominant eyes of emmetropes or ametropes concurrently with LASIK. Three approaches were reported to be in various stages of clinical investigation:
1. Near centered multifocal effect by means of anterior corneal surface reshaping.
2. Bifocal approach using an inlay with intrinsic power.
3. Extension of depth-of-focus by means of a pinhole.
Researchers say all three are improvements over standard monovision because of improved distance vision retention in the treated eye.
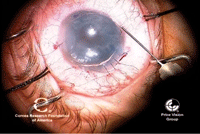
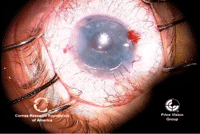
DMEK was used with some success for corneal endothelial diseases. Once the graft is unrolled, air is injected to push the graft up to the host stroma (left). DMEK is complete, with the endothelial graft in good position (right). Photo: Francis Price, M.D.
Another study evaluated stereopsis in patients implanted monocularly with the KAMRA small aperture corneal inlay.1392/A64 Under the findings, the KAMRA small aperture corneal inlay did not affect stereopsis and contrast sensitivity remained within normal limits.
A study of 128 refractive surgery patients from eight sites showed the importance of measuring osmolarity with the TearLab device before refractive surgery. The study also revealed the importance of treating hyperosmolarity with drops (Blink Tears) to achieve a faster quicker recovery.1286 Patients with preoperative hyperosmolarity (≥ 308 mOsm/L) demonstrated significantly worse refractive outcomes at three months than their normal counterparts. For hyperosmolar patients, continuing postoperative therapy for at least three months may be important.
Preventing Cataracts?
A lot of discussion at ARVO centered on the possibility of preventing or delaying cataract onset with drops and oral agents. A study out of New Zealand and Germany looked at ex vivo permeation of cystine across bovine corneas. Seeking to develop an antioxidant drop, the researchers added ethylenediaminetetraacetic acid (EDTA), which opens tight junctions of bovine corneas to facilitate increased penetration of the drops into cystine, the limiting factor for glutathione synthesis.
Over a 24-hour period, 45nmol of cystine permeated across the bovine cornea. This amount almost tripled (118nmol over 24 hours) when the researchers incorporated 0.5% EDTA. Further penetration enhancers in combination with other delivery approaches, such as in situ gel eye drops, will be further evaluated before testing the most promising formulations in vivo.
A dietary supplement called sulforaphane is also being investigated for cataract prevention. According to one study, it can protect the human lens cells against oxidative stress and may delay the onset of cataracts.1066/D1271 In an experiment that used the human lens epithelial cell line FHL124, application of 30μm H2O2 to FHL124 cells caused a reduction in cell viability and increased cytotoxicity and apoptosis. These effects were significantly inhibited by 24-hour pre-treatment with 1μm of sulforaphane. The use of 30μm H2O2 also caused an elevation in lactate dehydrogenase (LDH) levels in the medium relative to control, which were suppressed by sulforaphane treatment.
The molecule guggulsterone is also being studied as a possible agent in cataract prevention. An in vitro cell culture model was used to investigate the effects of guggulsterone on prevention of toxicity in human lens epithelial cells.1070/D1275 Researchers observed H2O2-induced dose and time-dependent decline in the cells’ viability, which was prevented by guggulsterone. Guggulsterone also suppressed a dose-dependent and significant increase in LDH release from human lens epithelial cells, suggesting H2O2-induced alteration of membrane integrity as well as cell death.
Meanwhile, researchers at McMaster University in Ontario, Canada, have looked into a method for possibly preventing posterior capsular opacification (PCO) after cataract surgery.1069/D1274 Inhibition of matrix metalloproteinases by the antibiotic sulfadiazine has been shown to potentially decrease the incidence of PCO. Now, the investigators must determine the most effective therapeutic dose, which will be crucial when considering further tests involving in vivo studies and drug delivery devices such as IOLs.
Updates on Femtosecond Lasers
A femtosecond laser can be used to correct astigmatism via intrastromal arcuate incisions, ensuring that no break in the tissue occurs and that the entire procedure is performed within the corneal stroma. In one study involving rabbit and human cadaver eyes, the laser was shown to allow for the creation of a single, intrastromal incision, unlike a free hand or mechanical diamond blade incision.6622/A611 No morphologic changes were detected above and below these intrastromal incisions. Benefits included decreased risk of infection, no epithelial plug formation, and no need for topical antibiotics.
OCT features were found to be similar across all studies. Advantages over the use of diamond blades include predictability of incision depth, arc length and ability to modify the side-cut angle.

Femtosecond lasers were a hot topic at ARVO, as their utility continues to expand. This photo demonstrates lens fragmentation performed by the LensAR femtosecond laser system.
Another study showed the benefits of rapid healing and precision when using the femtoscond laser.1505/A461 The goal of the California-based trial was to review the initial results of an intrastromal arcuate keratotomy (ISAK) performed with an IntraLase femtosecond laser (iFS, Abbott Medical Optics).
In this prospective single center study, two groups of patients with astigmatism (naturally occurring or post-cataract surgery) were treated with the femtosecond laser, which was used to perform arcuate cuts completely placed within the corneal stroma on the steep axis.
Twenty-one eyes had been treated with this method and completely followed. Seventeen patients showed naturally occurring astigmatism, most of them selected prior to cataract surgery. Four additional patients presented with astigmatism following cataract surgery. The iFS-laser allowed the creation of precise, purely intrastromal incision patterns that were not readily achievable by standard diamond blade techniques. These preliminary outcomes indicated an excellent safety profile, the possibility of highly precise pattern placement and very rapid recovery and stability of vision.
LASIK with the femtosecond laser was shown to provide outcomes equal to those associated with the mechanical microkeratome. In a randomized, paired-eye study sponsored by the National Institutes of Health, LASIK with the femtosecond laser was shown to provide outcomes equal to those associated with the mechanical microkeratome. Twenty-one patients underwent LASIK for myopia or myopic astigmatism.1491/A447 Eyes were randomized by ocular dominance to LASIK with the flap created by a femtosecond laser (15 kHz [IntraLase FS, IntraLase]) in one eye and to LASIK with the flap created by a mechanical microkeratome (Hansatome, Bausch + Lomb) in the fellow eye.
Researchers found no effect on the endothelium of patients treated with the femtosecond versus those treated with the mechanical microkeratome. Five years after surgery, corneas that had undergone either method of flap creation could be accepted as donor tissue for endothelial keratoplasty.
Managing Postoperative Patients
Once more, a study has shown the benefit of using brominidine (Alphagan) to keep pupil size small to eliminate or reduce postoperative night vision problems in patients who have undergone surgical procedures. Thirty candidates for LASIK between 20 and 40 years of age in Turkey were included in the trial.
OPD-Scan (Nidek ARK-10000) was used for baseline and serial measurements at low mesopic and photopic luminance levels (10cd/m2 and 100cd/m2) 30 minutes after instillation of one drop of brimonidine tartrate 0.2% in one eye vs. administration of a placebo in the contralateral eye.
At all time intervals, brimonidine tartrate 0.2% produced a moderate miotic effect ranging from 5.65±1.01mm to 6.48±1.01mm, which was most significant 90 minutes after instillation at low mesopic conditions.
Meanwhile, research explored the use of a new formulation of loteprednol etabonate gel 0.5% for post-cataract inflammation and pain.6690/D710 Two multicenter, randomized, double-masked studies were conducted. In each study, patients with anterior chamber cell (ACC) severity greater than or equal to grade 2 after cataract surgery were randomized to receive the gel or a vehicle q.i.d. for 14 days.
The intention to treat population included 406 patients (203 per treatment group) in the first study and 407 patients (n=206 for loteprednol gel 0.5%, n=201 for vehicle) in the second study.

Research seeks to reduce post-cataract inflammation.
In the first study, 30.5% and 16.3% of patients in the loteprednol gel and vehicle groups, respectively, experienced complete resolution of ACC at day eight; whereas 72.9% and 41.9% patients, respectively, had no (grade 0) pain at day eight. In the second study, 31.1% and 13.9% of patients in the loteprednol gel and vehicle groups, respectively, benefitted from complete resolution of ACC at day eight; whereas 75.7% and 45.8% patients, respectively, had no pain at day eight.
Another study based in Inglewood and Torrance, Calif., evaluated the effects of a low concentration of modified bromfenac (Bromday, ISTA Pharmaceuticals) for inflammation and pain associated with cataract surgery.6684/D704 Patients were randomized to receive either bromfenac ophthalmic solution (n=110) or placebo (n=110), dosed once daily, one day before cataract surgery, on the day of surgery, and continuing through 14 days post-surgery.
A significantly larger proportion of patients in the bromfenac group had cleared ocular inflammation by day 15, compared to the placebo group. The number of patients who were pain-free at days one, three, eight and 15 was also significantly higher in the bromfenac group, compared to the number in the placebo group. From a safety standpoint, the incidence of adverse events was significantly lower in the bromfenac group compared to the placebo group.
A third medication that showed good results with lower dosing and a tolerable safety profile was difluprednate (Durezol, Alcon) for glaucoma patients after cataract surgery.6695/D715 A retrospective chart review of 65 patients was performed on glaucoma patients who underwent cataract surgery by one surgeon between June 2010 and June 2011 in Bronx, N.Y. Only those who were treated with difluprednate 0.05% immediately post-operatively at four times daily and then tapered according to level of inflammation were included in the study.
Difluprednate 0.05% was found to be an alternative to generic prednisolone acetate 1%, possibly offering more drop uniformity and requiring less frequent dosing for anterior uveitis.
The effects of systemic medication on ocular health were also reviewed. The association between intraoperative floppy iris syndrome (IFIS) and the use of medication for benign prostatic hyperplasia (BPH), such as tamsulosin (Flomax, Boehringer Ingelheim), and the use of some hypertensive medications, is well established.
Now, a study at the University of Texas has suggested that the use of warfarin (Coumadin, Bristol-Myers Squibb) may also result in IFIS.6707/D727 Thirteen eyes of nine patients who had taken or were actively taking warfarin were identified as having IFIS during phacoemulsification surgery.
This complication makes cataract surgery significantly more difficult, requiring surgeons to operate through a much smaller pupil. As a result, surgeons may require additional instruments to assist them in the procedure.

