
|

|
With advanced technology and excellent results, we run the risk of becoming complacent about adverse events. We don’t see continuing education courses on LASIK complications any more because it is hard to fill an hour with something so rare. However, as this is still the most common surgery many of us will see, it is important to be mindful of potential complications. Just last month, ASCRS informed its members that the delivery vehicles of certain topical drugs, when used intraoperatively, may become sequestered beneath the LASIK flap and remain unabsorbed, causing inflammation and delayed epithelial healing.
The most prevalent risk is dry eye. LASIK induces temporary dry eye in everyone. For the majority of healthy eyes, it is not a protracted issue. If patients have pre-existing dry eye, the post-op symptoms can be very bothersome and decrease vision. It is important to screen every LASIK candidate very closely for dry eye, and treat aggressively when encountered. If managed appropriately prior to surgery, most dry eye patients can still have successful outcomes.
| Multimedia
|
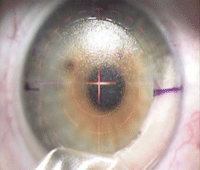
|
| Click
here to view a narrated video of a LASIK procedure.
|
Post-op complications are rare, but prompt action can save several lines of vision. The most immediate complication is a dislodged flap, which often occurs when the patient rubs their eye. If significant, the patient will notice decreased vision. You will see folds in the flap and a gutter around the edge. This needs to be referred back to the surgeon immediately for a flap refloat to ensure the best visual outcome.
Diffuse lamellar keratitis, although very rare, is still a possibility after LASIK. You will see a sandy/grainy inflammatory response in the flap interface within the first several days following surgery. The treatment for this continues to be high-frequency topical steroids and daily monitoring. If the patient loses a line of vision, they should be referred back to the surgeon for a flap relift and wash out.
The last major complication we worry about is infection (again, very rare). Because of the risk of an infection spreading through the flap interface, any suspected infectious keratitis should be referred back to the surgeon for treatment.
With the increased safety and efficacy of LASIK, ODs are more comfortable than ever recommending and comanaging the procedure. But be sure to remain vigilent for its key risks and complications.

