 |  |
As of April 2016, we finally have an FDA approval for a specific method of corneal collagen crosslinking (Avedro), a procedure indicated for the treatment of progressive keratoconus and corneal ectasia following refractive surgery. Investigators believe the mechanism of action involves the creation of new corneal collagen crosslinks, shortening and thickening the collagen fibrils, and strengthening corneal collagen by activating absorbed riboflavin with an ultraviolet light. This makes the collagen resistant to thinning and deformation.
Who Is Eligible?
Although the FDA study was confined to patients with progressive keratoconus and corneal ectasia following refractive surgery, research shows crosslinking is effective in most types of corneal ectasia.1 Candidates are identified using visual acuity, retinoscopy and manual keratometry. Ultimate patient candidacy should be confirmed by topography to assess posterior corneal curvature. Patients in the FDA clinical study were at least 14 years old, and no subjects were 65 or older.
Setting the expectations for the procedures is important. Patients need to understand that contact lenses or spectacles will still be required. Healing time may vary per patient, but on average, steepening of the Kmax is observed at one month, followed by flattening through 18 months.
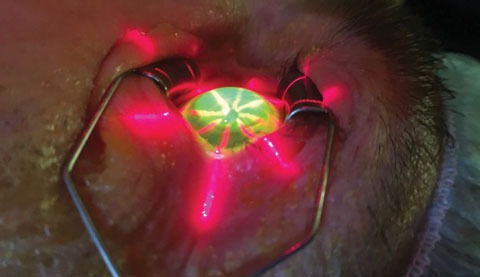 |
| Avedro’s KXL system uses laser crosshairs to align the optical head. |
How it’s Done
A central 9mm corneal epithelial defect is debrided on the cornea followed by one drop of Photrexa Viscous (riboflavin 5’-phosphate in 20% dextran ophthalmic solution, Avedro) applied to the cornea every two minutes for 30 minutes. Full absorption of the riboflavin is confirmed by the presence of yellow flare in the anterior chamber. The eye is then irradiated for 30 continuous minutes at 3mW/cm2 at 365nm while riboflavin is instilled every two minutes. After the procedure, a bandage contact lens (CL) is placed on the cornea and antibiotic, steroid and, possibly, nonsteroidal anti-inflammatory drops are prescribed.
Postoperative
Due to the removal of the central corneal epithelium, comanaging clinicians can expect a healing course similar to photorefractive keratectomy. One significant difference is increased discomfort the first night after the procedure, which may be due to the light energy absorbed by the corneal nerves. Corneal re-epithelialization will typically take place in three to five days after the procedure, but occasionally takes longer due to the steep nature of the cornea and the apical bearing of the cornea on the bandage CL. Patients should be advised to not rub their eyes ever again, as it can contribute to breaking collagen bonds and the progression of keratoconus. Once the cornea re-epithelializes, the comanaging OD can remove the bandage CL and discontinue the antibiotics and steroids. Normal CL wear can then be resumed.
In 1% to 2% of patients, adverse effects including corneal epithelial defect, corneal edema, corneal opacity and scar continued to be observed for 12 months.2 The only unique complication seems to be deep corneal haze, but in most cases this was temporary and rarely visually debilitating.
Our experience has shown that, although there is typically a slight thinning of the cornea immediately post-op, ectasia progression is halted in roughly 98% of cases. The FDA study for this procedure also shows significant improvement in corneal flattening as well as BCVA and UVCA when compared with sham treatment groups at one year.3
|
1. Bayraktar S, Cebeci Z, Oray M, Alparslan N. Corneal collagen cross-linking in pellucid marginal degeneration: 2 patients, 4 eyes. Case Reports in Ophthalmological Medicine. 2015;2015:840687. 2. Avedro. Package Insert. 3. Hersh PS, Greenstein SA, Fry KL. Corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results. J Cataract Refract Surgery. 2011;37(1):149-60. |

