The classic symptoms of ocular allergy—itching, redness and chemosis—can be a trifecta of trouble for eye care practitioners (ECPs). Although we can help our patients when the condition is appropriately identified, there continues to be no uniform management protocol to address this atopic population’s signs and symptoms.1,2
| With seasonal and perennial allergic conjunctivitis, superior involvement may indicate a more chronic or severe form of allergy. |
This is also a growing problem, with incidence increasing worldwide; ocular allergy now represents a full one-third of referrals and is one of the most commonly encountered conditions for ECPs.2,3 The underlying mechanism for this increase has yet to be fully understood, but researchers suspect it is multifactorial, including genetics, air pollution in urban areas, pets and early childhood exposure.4 Prescribing for the condition has also surged by 20%, inflating what was already a six billion dollar industry.5,6
In the context of these increases, failure to appropriately manage these patients is a mounting problem, which may ultimately lead to decreased quality of life. Studies indicate that more than 50% of patients reported an inability to comfortably go outdoors, difficulty driving or trouble sleeping.7 This article summarizes the landscape of allergy treatment, while emphasizing novel approaches to an age-old problem.
Classification
Ocular allergic disease is an umbrella term which encompasses myriad hypersensitivity disorders of the ocular surface; affected structures include the eyelids, cornea and, most frequently, the conjunctiva.8,9 Seasonal allergic conjunctivitis (SAC) and perennial allergic conjunctivitis (PAC) together comprise about 95% of clinical presentations, with atopic keratoconjunctivitis (AKC), vernal keratoconjunctivitis (VKC), giant papillary conjunctivitis (GPC) and other contact-lens related allergic conjunctivitis comprising the balance of cases.1,10 SAC and PAC are similar in their clinical presentation but vary in their inciting agents: SAC is mediated by grass and pollen allergens and tends to peak seasonally, whereas PAC is rooted in allergies to commonly encountered allergens year-round, including dust mites and feather and animal dander, which tends to make PAC chronic.9,10 Chronic forms of the disease are more likely to involve the lid and cornea and may require comanagement with other specialists such as allergists, dermatologists and pediatricians. The remainder of the conditions—AKC, VKC, GPC and contact conjunctivitis—have some common markers of allergy, but differ from SAC/PAC in clinical features and presentations. Vernal and atopic disease need to be aggressively managed to prevent complications such as corneal scarring and consequent vision loss.3
Pathophysiology
All ocular allergies represent a localized type 1 hypersensitivity reaction, wherein an antigen binds to immunoglobulin E, crosslinking the molecules on the mast cell surface and causing degranulation of inflammatory mediators from the mast cell. Histamine—long-established as a principal harbinger of ocular allergy symptoms—is among these mediators and is released from the mast cells, causing vasodilation and fluid transudation. This results in redness, swelling and itching, as fluid in the perivascular area stimulates adjacent nerve endings.11 Histamine exerts these effects via a number of distinct histamine receptors: stimulation of the H1 receptor causes itching, while stimulation of the H2 receptor causes vasodilation of conjunctival vessels.9,11 Researchers suspect H3 and H4 receptors are expressed on the ocular surface as well.11 This immediate histamine response lasts 20 to 30 minutes and is amplified by a late-phase response through a different set of mediators and cascades.3
Clinical Examination
History is a critical part of the examination. Itching is the cardinal symptom of ocular allergy, and practitioners should seek alternative differentials for patients who do not exhibit this complaint. Itching at the nasal aspect of the eye near the caruncle, which may be worse because it is a lymphoid tissue, should confirm your suspicion of allergy.12 It may also be accompanied by other symptoms such as redness, inflammation, stinging, tearing and burning. Watery or mucoid discharge may be present as well.3,13 Because patients with seasonal allergies may not present at the time of peak symptomology, clinicians should probe regarding symptoms during other times of the year and initiate treatment prophylactically.A search for signs of allergy should include a thorough slit lamp examination, paying special attention to the conjunctiva, as it is the principal ocular immunologic tissue that responds to allergens. In the case of SAC or PAC, there may be a papillary response, which is more likely to present inferiorly than superiorly.13,14 Papillae are nonspecific and may also be noted in healthy children and teenagers and should not be considered a pathognomonic sign.11 Conjunctival injection, conjunctival chemosis and inflammation of surrounding structures (including the lids) may be present.
Comorbidities
Because a number of allergic conjunctivitis symptoms are relatively nonspecific, comorbidities such as dry eye disease or blepharitis should be ruled out. Clinically, it is not uncommon for a patient to present with both allergic disease and a secondary condition, which may exacerbate the former.15
The tear film is an important innate defense against allergens, and a dry eye (whether evaporative or aqueous deficient) has less of this important defense. As a result, more allergens come in contact with the ocular surface at higher concentrations for longer amounts of time. This relationship becomes increasingly important, as treatment for one condition can deteriorate another if not appropriately identified.
For example, punctal plugs for dry eye hold allergens on the ocular surface, and oral antihistamines have a well-established history of worsening ocular dryness. The association of the conditions necessitates a thorough ocular surface examination—including vital dyes, tear break-up time and examination of the tear meniscus and lid margins—as well as a management plan that treats each condition independently while being mindful of the overall impact. A good rule is to treat the prevailing symptomology first, whether dryness or allergy, with the understanding that failure to manage associated conditions will lead to difficulty in achieving full symptomatic relief. Crossover therapies—including artificial tears and avoidance of inciting agents—may be of particular utility. Emerging wisdom indicates that failure to address comorbidities may be what underlies much of the therapeutic failure of allergy treatment.
In addition to a thorough ocular examination, new point-of-care testing is available for allergy sufferers in the form of an in-office skin test known as Doctor’s Allergy Formula (Bausch + Lomb).1,16 ECPs have started performing this test—typically the realm of allergists—to corroborate their diagnosis and comanage with other specialties.
 |
| Click image to enlarge. |
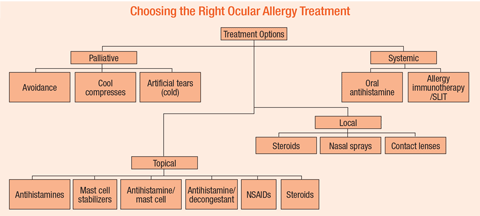
Treatment
It serves to identify sensitivities to specific allergens and can be customized to include allergens specific to your geographic location. It may be performed by a nurse or technician, but is currently only billable for ODs practicing in a multidisciplinary setting associated with an MD or DO. Hopefully the test will become available for more widespread use in the optometric community. Along with other point-of-care diagnostic testing, it will allow practitioners to make more objective and informed decisions about the etiology of symptoms and formulate comprehensive management strategies.
• Palliative Therapy. The most elementary and effective management plan for ocular allergy is avoidance of inciting allergens. Functionally, it may also be the most challenging for patients. The conjunctiva is, relatively speaking, a vast surface area for allergens, and minimizing contact is paramount.3 Staying indoors when the allergen count is high, keeping windows closed, wearing wrap-around sunglasses, cleaning filters and ducts, replacing allergen-harboring items such as pillows or carpet and even washing one’s hair before going to sleep can all be effective at reducing exposure.1,7,13 Cool compresses also provide palliative relief and should be recommended along with artificial tears to minimize eye rubbing, which leads to further histamine release and worsening symptoms.7,15
Artificial tears on their own are not only palliative but can also be therapeutic, helping to diffuse ocular allergens and preventing them from interacting with the ocular surface.1 Many practitioners recommend patients refrigerate the artificial tears to provide more immediate relief of symptoms. Preservative-free artificial tears should be the product of choice, as they avoid the complication of a preservative in a patient already predisposed toward atopy.1
• Topical Therapeutics. A multitude of topical therapeutic options are on the market for the management of ocular allergy. They can be used as monotherapy or in combination, though simpler dosing generally correlates with increased compliance. Each of the agents remain effective at targeting allergy in some capacity—the real skill, as always, is in the art of prescribing.
Many antihistamine (e.g., emedastine, levocabastine) and mast cell stabilizer (e.g., pemirolast, neocromil, lodoxamide, cromolyn) monotherapy mainstays are on the market. These drops are most effective for acute and preventative treatment, respectively. Antihistamines reversibly block the histamine receptor and provide rapid relief of redness and itching. They suffer from a more limited duration of action (dosed at four times per day, same as mast cell stabilizers) and do not prevent the action of other pro-inflammatory mediators, including prostaglandins and leukotrienes.3 Although antihistamines are effective at acute relief, they have less ability to prevent allergies in a prophylactic capacity by targeting the mast cells.
Mast cell stabilizers, on the other hand, are especially effective at decreasing or eliminating symptoms of an attack when taken in advance.1 Using a mast cell stabilizer after the patient is exhibiting symptoms is like repairing the hole in the bucket after the water has drained—the damage (and degranulation) is already done. Eye care practitioners can prescribe a mast cell stabilizer weeks or months in advance of a patient’s peak symptoms to target and mitigate impending histamine release.1 For acute attacks, an antihistamine or combination agent should be considered instead.
Topical combination antihistamine/mast cell stabilizers (e.g., alcaftadine, azelastine, bepotastine, epinastine, ketotifen, olopatadine) are key agents in the management of allergic conjunctivitis, and there have been a number of recent changes in this market segment. These agents have the combined benefit of immediate relief—owing to the antihistamine properties—as well as the long-term benefit of mast cell stabilization. An added advantage is the once-daily dosage a number of medications offer.
The newest combination therapy drug is a higher concentration of olopatadine (0.7% vs. 0.2%), and research shows it improves relief compared with previous iterations.19
Bepotastine is a prescription-only twice-daily drop that is unique in its high specificity for the histamine 1 receptor, meaning that it is particularly effective at preventing ocular itch.1 Furthermore, one study shows it reduces nasal congestion, rhinorrhea, ear/palate itching and nasal itching.17 This top-down, gravity-driven influence of ocular agents on the nasal mucosa is an area of significant research and will likely be exploited to improve cardinal symptoms of allergy without initiating oral or systemic treatment.18
A number of ketotifen-based drops are now available over-the-counter (OTC) for use twice a day, such as Zaditor (Alcon), Alaway (Bausch + Lomb), Refresh Eye Itch Relief (Allergan) and TheraTears Eye Itch Relief (Akorn). The release of these OTC options allow us to provide a safe and effective long-term therapy for allergy sufferers, with low risk for harm and abuse.20 The once-daily dosage of the prescription-only agents, however, continues to be an advantage to prescription medications over the twice-daily dosing of OTC products.
Although decongestants (e.g., oxymetazoline, tetrahydrozoline and naphazoline) compounded with antihistamines have traditionally been a cornerstone of allergy therapy, they are decreasing in popularity due to their adverse effects—mydriasis, rebound hyperemia and a contraindication in patients with narrow angle glaucoma—and the advent of newer agents with better safety profiles and efficacy.11 They remain effective at decreasing redness and itch, but because their use should be limited to a maximum of 10 to 14 days, their utility in chronic allergic conditions is limited.20
Topical nonsteroidal anti-inflammatory drugs (NSAIDs) are another allergy treatment option whose usage is less prevalent than in the past. While effective at decreasing the irritation associated with ocular allergy, they do not address other symptoms and have complications with long-term use, including risk for corneal melt. In addition, they have the potential to incite a leukotriene-mediated enhancement of the inflammatory response, which runs counter to the goal of effective allergy management.12
Topical steroids used for allergy relief typically include loteprednol, fluorometholone or prednisolone acetate 0.125% because of their propensity for effective control of inflammation and low side effect profile. Steroids exert their action early and often in the inflammatory cascade and are the single most effective agent at combating the inflammation associated with ocular allergy.12 They are typically reserved for cases nonresponsive to conventional therapy, or in cases of acute, pronounced allergic response. Be aware of the side effects, including the chance of IOP elevation and cataracts; these agents should not be used for long-term therapy.3 More potent steroids such as Pred Forte and difluprednate may be used in advanced and nonresponsive cases.
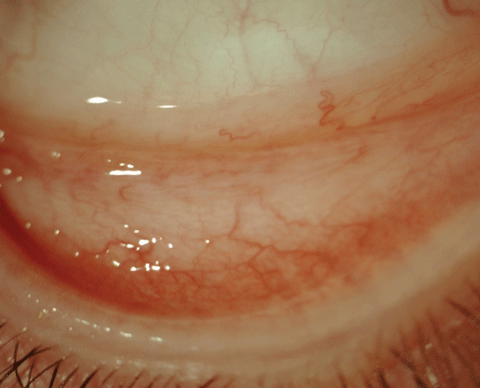 |
| Papillae on lower lid eversion in a patient with moderate allergy symptoms. Photo: Elyse Chaglasian, OD, and Jennifer Harthan, OD |
There are numerous areas of research in topical therapy for allergy. Building on our current arsenal of topical agents, research on the off-label use of topical cyclosporine has shown its promise as an alternative to steroids for patients with severe or chronic forms of the disease.11 Also, research shows MMP-9 activity is elevated in patients with allergic conjunctivitis and dry eye, indicating promise for a novel topical agent targeting this activity.11 Investigation into the use of conjunctival injections into the upper tarsal area as a means for managing more serious, chronic cases of allergy such as VKC has shown promise, as have glucocorticoid receptor agonists, an investigative class of drugs that target inflammatory disease.11 Finally, researchers are also investigating vaccinations (peptide and cDNA), adjuvants, anti-IgE antibodies and intracanalicular dexamethasone depots, which may represent the future of allergy treatment.
• Local Therapeutics. Inflammation is often concentrated in, but not limited to, the conjunctival surface in ocular allergy. Research shows that allergic inflammation of the eyelid skin in conditions such atopic dermatitis or eczema is unresponsive to topical antihistamines and mast-cell stabilizers.15 Instead, the practitioner should consider a topical steroid, keeping in mind the possible side effects of skin-thinning and discoloration. In an effort to decrease these side effects, investigators are looking into the use of pimecrolimus or tacrolimus off-label as a safe, nonsteroidal alternative for long-term therapy.15
A secondary area of frequent inflammation is the nasal mucosa, where reports indicate that roughly 14.5 million Americans have a combined rhinoconjunctivitis.21 Nasal and ocular mucosa show similar characteristics and symptoms, and research has discussed the crossover effect of some topical ocular therapeutics on the nasal mucosa.13,15 What is perhaps more surprising is that steroidal and nonsteroidal nasal sprays also show a beneficial impact on reducing symptoms at the ocular mucosa.18 To this end, triamcinolone and fluticasone nasal sprays have recently become available OTC, making treatment more accessible for comprehensive management of the various aspects of allergic symptoms. Most patients require dual therapy (ocular and nasal) for full symptomatic relief.
• Prophylactic measures. Contact lenses have emerged as a possible treatment modality for ocular allergy. The lenses provide protection against allergens, and symptoms of itching, burning, stinging, dryness and discomfort were all shown to be reduced in patients wearing “enhanced moisturizing” daily disposable lenses.22 This was attributed to a barrier effect, similar to the effect on tearing for the wearer when cutting onions.22 Drug-infused contact lenses would combine this protection with an additive therapeutic effect. There are no such lenses currently on the market; however, with the continued investigation into infusing contact lens materials with medicinal agents, it is easy to imagine great potential for an allergy-targeted therapeutic lens moving forward. We strongly emphasize frequent replacement (ideally daily disposable) and good lens hygiene for all of our contact lens-wearing patients with allergy.23 If treating with drops, patients should instill them at least 10 minutes before inserting their contact lenses to prevent accumulation of the active ingredients—as well as the attendant preservatives—in the material of the lens.7
• Systemic Therapeutics. Oral antihistamines remain a pillar of allergy treatment and generally provide moderate relief of ocular symptoms. While the newer second- and third-generation formulations are less sedating that older formulations, they can still contribute to dryness of the ocular surface, with some studies showing tear flow reduction of up to 30%.15,24 Furthermore, oral agents may be unsuccessful at relieving the itch associated with ocular allergy.15 Depending on the predominant symptomology, if the patient is getting minimal relief of ocular symptoms with an oral agent, it might be prudent to discontinue the oral agent and replace it with a more targeted topical or local therapy.18 One exception would be a patient suffering from allergic sinusitis, who likely needs an oral agent containing a decongenstant.7
Allergy immunotherapy is another treatment modality with proven systemic relief.11 It consists of giving the patient injections of increasing quantities of allergens in order to decrease the patient’s own allergic response to that allergen. It has shown variable success in managing a patient’s ocular symptoms.11
More recently, however, a new alternative to subcutaneous injections has emerged. Sublingual immunotherapy is gaining popularity and shows effectiveness against allergic rhinitis and, to a lesser extent, allergic conjunctivitis.13,25 Oralair (Greer) is the first approved sublingual allergy extract for patients sensitive to grass pollens.1 While its impact on allergic conjunctivitis is inconsistent, further forays into this research may prove promising in successfully managing both systemic and ocular symptoms.9
Ocular allergy is a clinical problem with a many solutions. For now, proper understanding of the pathophysiology and the available agents are critical to tackling a patient’s symptomology. Updated treatments and wider availability of current therapeutics should make solving the problem easier than ever.
Dr. Fromstein is an assistant professor at the Illinois College of Optometry, where she splits her time between didactic education and clinical teaching in the Cornea and Contact Lens, Urgent Care and Primary Care Services.
|
1. Trubo R. Seasonal ocular allergy: new options for a recurring problem. Cornea. 2015 Mar:31-3. 2. Wong AH, Barg SS, Leung AK. Seasonal and perennial conjunctivitis. Recent Pat Inflamm Allergy Drug Discov. 2009;3:118-27. 3. La rosa M, Lionetti E, Reibaldi M, et al. Allergic conjunctivitis: a comprehensive review of the literature. Italian Journal of Pediatrics. 2013;39:18. 4. Leonardi S, del Giudice Miraglia M, La Rosa M, et al. Atopic disease, immune system, and the environment. Allergy Asthma Proc. 2007;28(4):410-17. 5. Origliery C, Bielory L. Emerging drugs for conjunctivitis. Expert Opin Emerg Drugs. 2009;14(2):523-36. 6. Bielory L. Update on ocular allergy treatment. Expert Opin Pharmacother. 2002;3(5):541-53. 7. Karpecki P. Contact lens wear and ocular allergy. Contact Lens Spectrum. 2012;27: 26-32. 8. Abelson MB, Smith L, Chapin M, et al. Ocular allergic disease: mechanisms, disease sub-types, treatment. The Ocular Surface. 2003;1(3):127-49. 9. Berdy GJ. New strategies in the diagnosis and management of ocular allergy. Cataract & Refractive Surgery Today. 2012. 10. Slonim CB, Boone R. The ocular allergic response: a pharmacotherapeutic review. Formulary. 2004;39:213-22. 11. Raizman MB, Luchs JI, Shovlin J, Wolf RL. Ocular allergy: a scientific review. Review of Opthalmology. 2012 May. 12. Thoughts on the management of ocular allergy. Ocular Surgery News. 2009. 13. Bowling E. What’s trending in ocular allergy treatment. Optometry Times. 2015. 14. Bielory L, Friedlaender MH. Allergic conjunctivitis. Immunol Allergy Clin North Am. 2008;28:43-58. 15. Raizman MB. Ocular allergy, nasal allergy, and dry eye disease. Advanced Ocular Care. 2010 Mar:48-9. 16. Cooper MS. A new player in point-of-care allergy testing. Optometry Times. 2015. 17. Macejko TT, Meier EJ, Bergmann MT, et al. Bepotastine besilate ophthalmic solution 1.5% for up to 8 hours following dosing reduces total non-ocular symptoms, rhinorrhea, and tearing in a multi-site clinical model of allergic conjunctivitis. Poster presented at 2009 American Academy of Allergy Asthma and Immunology Annual Meeting, March 3-17, 2009; Washington, DC 18. Karpecki PM. Anti-allergy eye drops can effectively treat nonocular symptoms. Primary Care Optometry News. 2011. 19. Alcon. Pazeo Package Insert. Fort Worth, TX, 2015. 20. Mandese MJ, McCann W, Croteau V. When to ‘prescribe’ an OTC allergy drop. Review of Optometry. 2010;147(8):31-6. 21. Bousqet J, Khaltaev N, Cruz AA, et al. Allergic rhinitis and its impact on asthma (ARIA) 2008 update. Allergy. 2008;63(8)160. 22. Wolffsohn JS, Emberlin JC. Role of contact lenses in relieving ocular allergy. Contact Lens & Anterior Eye. 2011;34:169-72. 23. Byrne J. Help allergy sufferers wear contact lenses more comfortable. Primary Care Optometry News. 2005. 24. Welch D, Ousler G, Nally L, et al. Ocular drying associated with oral antihistamines (loratidine) in the normal population - an evaluation of exaggerated dose effect. Adv Exp Med Biol. 2002;506:1051-5. 25. Vitaliti G, Leonardi S, Miraglia Del Giudici M, et al. Mucosal immunity and sublingual immunotherapy in respiratory disorders. J Biol Regul Homeost Agents. 2012;26:S85-S93. |

