Q: I have a 74-year-old patient with the onset of a branch retinal vein occlusion (BRVO) that started a month ago, and she is just getting in now. She has 20/200 best-corrected acuity from macular edema. What are her treatment options?

A: “She has a few different options,” says Jessica McCluskey, M.D., a prominent retina specialist in Atlanta. These include:
• Observation. The first, and most traditional, option is to do nothing. “You would simply observe and wait for the heme to resolve,” Dr. McCluskey says.
But this strategy is a holdover from when there were few, if any, effective options for treatment. “We all have these old studies in our head that we were taught in school: just watch and observe,” she says. “But only about one-third of the patients will resolve on their own.”1
• Grid laser. Grid laser photocoagulation, which can improve visual acuity by three lines in 28% of patients, was previously considered the standard of care for branch retinal vein occlusion, Dr. McCluskey says.2,3
• Intravitreal triamcinolone. Steroid injection with triamcinolone looked to be a promising treatment to reduce macular edema in BRVO. “But the SCORE study has shown that, although intravitreal triamcinolone is good, it doesn’t offer a huge improvement over grid laser.”2 Also, the steroid puts the patient at risk for developing cataract and glaucoma.
• Anti-VEGF. “We’re now much more aggressive in treating these patients,” Dr. McCluskey says. “In our office, the first choice for the patient in this case would be an anti-VEGF injection, hands down.”
Six-month results from the BRAVO study bear this out. In this phase III study, visual acuity improved three or more lines in 61% of the subjects given 0.5mg ranibizumab compared with 29% of the subjects in the sham group.4
“The nice thing about this treatment is you’ll see improvement in vision in the first week, so we can get these people back to their normal lives very quickly,” she says. “More than likely, they may still need another injection in four to six weeks. But in the short-term, we’re doing something quickly to get rid of that edema, so we typically perform the injection on the first day that they’re seen.”
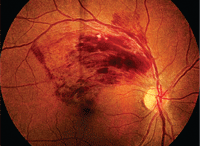
Treat retinal vein occlusion right away.
Often, patients require multiple injections, Dr. McCluskey says. “The problem is that sometimes the macular edema keeps recurring and the patient needs many injections, which is why they came out with the steroid implant.”
• Corticosteroid implant. “Like all steroids, the Ozurdex (dexamethasone intravitreal implant, Allergan) helps stabilize the breakdown of those endothelial tight junctions and down-regulate VEGF expression, which is the cause of macular edema,” she says. “So this is a great thing to use in a patient with chronic recurring macular edema to decrease the number of injections.”
No matter what treatment the patient receives, the retina specialist will follow the patient closely and make sure she is stable for at least three months before sending her back to the referring doctor.
Bottom line: “I think there are some referring physicians out there who still aren’t familiar with these studies and are watching these vein occlusion patients for a long time before they refer them,” Dr. McCluskey says. “But the earlier we treat that macular edema, the better their long-term results are going to be.”
1. Rogers SL, McIntosh RL, Lim L, et al. Natural history of branch retinal vein occlusion: an evidence-based systematic review. Ophthalmology. 2010 Jun;117(6):1094-1101.
2. Scott IU, Ip MS, VanVeldhuisen PC, et al; SCORE Study Research Group. A randomized trial comparing the efficacy and safety of intravitreal triamcinolone with standard care to treat vision loss associated with macular Edema secondary to branch retinal vein occlusion: the Standard Care vs Corticosteroid for Retinal Vein Occlusion (SCORE) study report 6. Arch Ophthalmol. 2009 Sep;127(9):1115-28.
3. Argon laser photocoagulation for macular edema in branch vein occlusion. The Branch Vein Occlusion Study Group. Am J Ophthalmol. 1984 Sep 15;98(3):271-82.
4. Campochiaro PA, Heier JS, Feiner L, et al; BRAVO Investigators. Ranibizumab for macular edema following branch retinal vein occlusion: six-month primary end point results of a phase III study. Ophthalmology. 2010 Jun;117(6):1102-1112.

