 History
History
A 43-year-old black female presented with a red, painful left eye that had persisted for four months. The patient explained she had not experienced normal vision in that eye since she was injured in an automobile accident 10 years ago. She had visited the emergency room the day prior to her visit in our department and was diagnosed with a corneal abrasion O.S. The ER staff treated her with a topical fluoroquinolone and instructed her to schedule a follow-up examination with an eye doctor. Her systemic history was noncontributory, and she reported taking no systemic medications.
Diagnostic Data
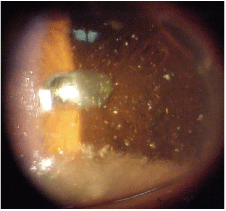
This 43-year-old patient presented with a red, painful left eye. What is your diagnosis?
Her best-corrected acuity was 20/20 O.D. and 20/40 O.S. at distance and near. External examination was normal, and there was no evidence of afferent pupillary defect. Her intraocular pressure measured 19mm Hg O.U. The pertinent anterior segment findings are illustrated in the photograph. Dilated fundus examination was normal in both eyes.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? Whats the likely prognosis?
Discussion
The diagnosis in this case is synchysis scintillans, which is characterized by vitreous opacification secondary to severe or recurring vitreous hemorrhage.1,2 Crystal-like opacities may be observed in the vitreous as the bulk hemorrhage dissipates, or they may appear as flat, freely mobile, brown-white, refractile bodies in the anterior chamber (as in this case). The opacities are associated with liquid vitreous, and they may settle in the most degenerated portion of the corpus vitreous when the eye is motionless.1,2
Chemical studies demonstrate the presence of cholesterol crystals in these opacitiesa condition sometimes referred to as cholesterolosis bulbi.2 The condition is frequently seen in degenerating eyes before the onset of phthisis bulbi. The cellular response to vitreous hemorrhage has been compared to a "low-turnover" granuloma. Unique clinicopathologic features of long-standing vitreous hemorrhage include cholesterolosis bulbi (synchysis scintillans), hemoglobin spherulosis and vitreous cylinders.2
An additional uveitis or vascular work-up may be required to rule out either active or lingering inflammation, which can produce vitritis. Because vitreous hemorrhage is associated with degenerative processes that can raise intraocular pressure, patients must also be monitored for glaucoma. Since synchysis scintillans is often associated with previous or chronic vitreous hemorrhage secondary to neovascularization or trauma, vision and overall ocular health is generally poor.
With the exception of pars plana vitrectomy for cases with poor visual outcome, there is no effective management option for this condition.2
1. Sebag J. Vitreous anatomy and pathology. In: Yanoff M, Duker JM. Opthalmology.
2. Spraul CW, Grossniklaus HE. Vitreous Hemorrhage. Surv Ophthalmol 1997 Jul-Aug;42(1):3-39.

