 A 43-year-old white male presented in May 2007 for a comprehensive examination as a new patient. His chief complaint was of significant blur at near. His last eye examination was two to three years ago.
A 43-year-old white male presented in May 2007 for a comprehensive examination as a new patient. His chief complaint was of significant blur at near. His last eye examination was two to three years ago.
Significant medical history included left rotator cuff surgery in 2005, seasonal allergic sinusitis and occasional flare-ups of tendonitis. His personal and family ocular history was unremarkable.
Diagnostic Data
His best-corrected acuity was 20/20 O.D. and O.S. at both distance and near through minimal hyperopic and presbyopic correction. Pupils were equal, round and reactive to light and accommodation, with no afferent pupillary defect. Extraocular muscles were full in all positions of gaze.
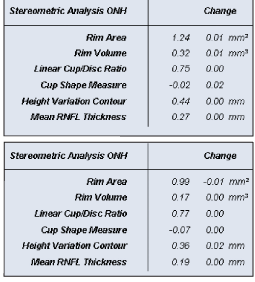
There was virtually no measurable progression between his May and December visits (O.D. top, O.S. bottom).
A slit lamp examination of the anterior segments was unremarkable. Intraocular pressure measured 18mm Hg O.D. and 16mm Hg O.S. Through dilated pupils, his crystalline lenses were clear O.U. His cup-to-disc ratio was 0.75 x 0.75 O.D. and 0.70 x 0.70 O.S. His optic nerves were large. The bilateral vascular, macular and peripheral retinal examinations were completely normal.
I initially diagnosed him as a low-risk glaucoma suspect, which I based on his large cup-to-disc ratios and concurrent large optic nerves, and the absence of other significant findings. Still, he warranted a baseline examination, which we scheduled for three weeks later.
At the return visit, his IOP measured 19mm Hg O.D. and 21mm Hg O.S. Pachymetry readings were 594m O.D. and 579m O.S. His threshold visual fields were unremarkable, and reliability indices were good.
Gonioscopy demonstrated grade 4+ open angles at 360 O.U., with minimal trabecular pigmentation. Evaluation of the optic nerves with the Heidelberg Retina Tomograph-3 (HRT-3) revealed the presence of large discs, measured at 2.79mm squared O.D. and 2.43mm squared O.S. (Average disc size by HRT-3 ranges from 1.63mm squared to 2.43mm squared). His rim volume measurements, however, were significantly outside normal limits.
Discussion
Interestingly, even though the HRT-3 findings supported the presence of large discs, the neuroretinal rim characteristics were outside normal limits, given the large size of the optic nerves. I now faced the classic glaucoma management question: Should I initiate treatment or closely monitor this patient?
The answer to this question is not always clear-cutas in this case. While some parameters indicate an optic nerve outside normal limits (HRT-3 findings), others do not (visual fields, intraocular pressure, pachymetry readings, and lack of other risk factors, such as family history, race, etc).
The HRT-3 findings, primarily those pertaining to the specific characteristics of the neuroretinal rim and the perioptic nerve fiber layer (NFL), provide the strongest argument for treating this patient. HRT-3 has the capability of predicting glaucomatous optic neuropathic changes several years prior to actual visual field loss in patients with ocular hypertension. Whether one would define the patients IOP as elevated is a matter of discussion, since his highest reading from only two examinations was 21mm Hg.
The diurnal curve measurements have not yet been evaluated; the results may suggest whether this patient can be classified as an ocular hypertensive. If he is found to be hypertensive, the HRT-3 results are, therefore, more ominous.
While threshold visual fields were normal, the field-testing strategy was conventional white-on-white. It is possible that blue-on-yellow studies or other visual field strategies aimed at detecting visual field loss at an earlier stage may indicate the presence of a field defect.
However, there are several arguments for monitoring this patient instead of medicating him. For one, I have not evaluated his IOP fluctuation or the stability of his visual field. Most importantly, the stability of his optic nerve characteristics (rim area, NFL stability, etc.) has not yet been ascertained.
While this patient is clearly at risk for glaucoma, the initial and most pressing question is whether there is active disease; is he stable? The best way to determine stability is to evaluate the appropriate parameters at timely intervals and watch for change. If you can determine that the patient is not stable after subsequent evaluations, immediate intervention is necessary.
I initially chose to monitor this patient to determine his stability. After additional consideration and evaluation, I flagged him for having a moderate-to-high risk for frank glaucoma progression.
I most recently saw the patient in December 2007. His IOP, visual fields and HRT-3 imaging was unchanged. There was precise symmetry of the right and left NFL thickness maps between the visits in May and December, as shown.
Considering the patient demonstrated virtually no progression at the December visit, I am reassured that continued monitoring is the appropriate option. However, depending upon future examination results, my approach may change.
When initially evaluating new patients for glaucoma, especially borderline cases such as this one, do not rush to treat unless there is considerable evidence that patient harm may occur. Develop a comfort level with the patients overall stabilityand that, by its very nature, takes time.

