The eyelids provide several important functions: they protect the globe from external threats, supply lipid secretions necessary to create and maintain a healthy tear film, and they distribute and drain the tears. Unfortunately, when evaluating a patient at the slit lamp, it is altogether too easy to overlook the lids and zoom in on the ocular surface. A thorough examination of the lids can be critical for systemic health in addition to ocular integrity. Let’s review some of the critical factors to consider and signs to look for.
Position
Lid examination begins during the patient intake. While reviewing the patient history, note the position of the lids. When the eye is open, the upper lid should cover 1/6th of the cornea, with the lower lid just touching the inferior limbus. The lid should approximate the globe along the entire lid margin, without turning in or out.
|
|
|
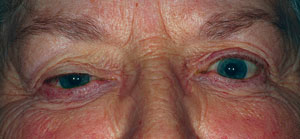
Left/right asymmetry in lid apertures can be secondary to proptosis, as seen here OS.
|
|
Unequal apertures could indicate a serious condition such as thyroid disease or a space-occupying lesion. It must be determined whether there is proptosis or an enophthalmos of the contralateral eye. A Hertel ophthalmometer is useful for determining globe position disparity; a difference of 2mm is considered abnormal.
Entropion and Ectropion
A turning in of the lid margin represents
entropion, which is one cause of lashes dragging across the ocular surface (trichiasis). Symptoms include redness and pain around the eye, sensitivity to light and wind, sagging skin around the eye, epiphora and decreased vision, especially if the cornea is damaged. Causes include congenital abnormalities, aging (which creates loose skin), stretched and loose ligaments and muscles, scarring, trauma, trachoma and involution spasms.
Entropion may not be seen when the patient is at rest in the chair but generally can be elicited when the patient squeezes the lids.
|
|
|
|
|
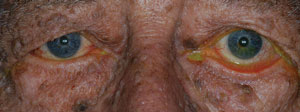
Age-related cicatricial ectropion of the left eye with symptomatic dryness.
|
Ectropion, by contrast, is a condition in which the eyelid margin turns outward. A myogenic ectropion in particular is caused by a weakness in the lid muscles. Ectropion may be a natural result of age or a consequence of facial paralysis caused by Bell’s palsy or tumor. Other potential etiologies include scarring from burns or trauma, benign or cancerous lid lesions, blepharoplasty, radiation for neoplasms or cosmetic laser skin resurfacing, cicatrizing conditions like Stevens-Johnson syndrome or ocular cicatricial pemphigoid; or it may be congenital, as in Down’s syndrome.
Blepharoptosis
Ptosis can be either congenital or acquired. Congenital ptosis
is present at birth and is prevalent equally in both males and females. It is caused by levator development abnormality, resulting in fibrosis and fatty infiltration of the muscle. A congenital ptosis may be either unilateral or bilateral. The lid crease will be poorly formed in the affected eye(s) and individuals with congenital ptosis may suffer from nocturnal lagophthalmos. Bilateral cases develop a chin-up posture to see under the drooping lid, while unilateral cases are at risk for amblyopia. Sixteen percent of congenital ptosis cases will have abnormal superior rectus function.1
|
A Systematic Approach to Eyelid Examination and Documentation
|
|
Acquired ptosis may arise from floppy lid syndrome, levator dehiscence from contact lens wear or aging, mechanical/ traumatic conditions or neurogenic causes.
Floppy lid syndrome is defined by easily everted eyelids with a thickened, elastic tarsal plate and lash ptosis. It has been associated with giant papillary conjunctivitis and keratoconus, chronic eye rubbing and obesity.2 Up to 85% of patients with floppy eyelids may have obstructive sleep apnea, a potentially life-threatening condition, and therefore should be evaluated in a sleep clinic.3
The majority of levator dehiscence is associated with rigid contact lens wear. It is generally accepted that removal of lenses by tugging on the upper lid and harsh blinking is the cause.4
Slippage of the aponeurosis is the most common cause of mild to moderate ptosis in the elderly. It should be differentiated from neurogenic causes of ptosis. Other conditions that mimic lid ptosis are dermatochalasis and brow ptosis. Patients with ptosis may complain about vision loss (especially when reading), headaches, eyebrow strain and cosmesis. The palpebral aperture should be documented, and it may be helpful to compare the lid position to old photographs. Medicare requires at least 20 degrees of documented visual field restriction to pay for repair.
Other, more rare, causes of acquired ptosis include neoplasm, neurofibromas and cicatricial disease.
Innervation
The eyelids are innervated by the oculomotor nerve (CN III), the facial nerve (CN VII), the trigeminal nerve (CN V) and sympathetic fibers.
The orbicularis oculi is responsible for shutting the eye and is innervated by the facial nerve. The oculomotor nerve innervates the levator and tarsal plate and opens the eye. The ophthalmic division of the trigeminal nerve is purely sensory. Sympathetic nerve fibers of the lids innervate Müller’s muscles.
|
|
|
|
|
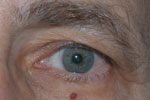
Dermatochalsis and brow ptosis reducing the visual field, while lid margin remains in the proper position.
|
Marcus-Gunn jaw winking is an aberrant connection of the oculomotor nerve fibers that innervate the levator and the trigeminal nerve fibers of the muscles of mastication (motor nerve). Jaw winking is present in approximately 5% of congenital ptosis cases, with nearly 4% being bilateral.5
A seventh, or facial, nerve palsy causes an inability to close the eyelid. Bell’s palsy is the most common subset of conditions causing facial nerve paralysis. Bell’s palsy affects 11 to 40 persons per 100,000 each year, with peak incidence between the ages of 15 and 50.6-8
Reactivation of herpes simplex and herpes zoster is postulated to account for the majority of cases of Bell’s palsy.9 The condition typically presents with a sudden and rapid onset of unilateral facial weakness, often within a few hours. Less than 1% of cases are bilateral. While the majority of cases are self-limiting with complete recovery, recent evidence shows the early treatment with corticosteroids may improve recovery results.9 Antiviral therapy does not improve chance of recovery.10 Differential diagnosis includes brain tumor, stroke, myasthenia gravis and Lyme disease.
In contrast to facial nerve palsy, several conditions result in the inability to open the eyes.
Horner’s syndrome is impaired innervation of sympathetic to Müller’s muscle. It is often associated with the classic triad of ptosis, miosis and anhydrosis, although patients rarely present with all three signs. It can be either congenital or acquired, and the risk to patient health varies from benign to life threatening based on the underlying cause.11 Patients should undergo a thorough neurological work-up.
Third nerve palsy also results in an inability to open the lid. Examination may show a dilated, poorly reactive pupil; reduced ocular movements; and ocular misalignment, where the eye is located down and out. Pupil-sparing third nerve palsy involves ischemic cranial neuropathy (such as in diabetes or hypertension), while pupil-affecting third nerve palsy involves compressive lesions or aneurysm.
Acquired myasthenia gravis involves inability to open the eye, which may be variable throughout the day and worsen when tired. This autoimmune condition affects 20 in 100,000 people and is caused by a reduction in acetylcholine receptor sites. Common symptoms of myasthenia gravis include a drooping eyelid, blurred or double vision, slurred speech, difficulty chewing and swallowing, weakness in the arms and legs, chronic muscle fatigue and difficulty breathing.12
Lesions
Skin lesions found around the eye can be confusing—benign ones may have a dramatic appearance while malignant lesions look unassuming.
|
|
|
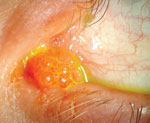
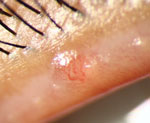
Lid papillomas may not always be as obvious as that seen in the left image. They may in fact be more subtle and difficult to spot, as in the lid margin papilloma at right.
|
|
Papillomas most commonly present in middle-aged adults and the elderly. Squamous papillomas represent a benign hyperplasia of squamous epithelium. Viral papillomas are associated with local infection involving the human papilloma virus (HPV). Papillomas on the skin will appear skin-colored, tan or brown. They may be round or pedunculated. They are easily removed with excision. On the conjunctiva, a papilloma may appear as a mass of vessels or a cluster of hyperemic cells and must be differentiated from a squamous cell carcinoma.13
Actinic keratosis is rare under 30 years of age. It presents as a flat, light tan lesion, most common on the face, trunk and upper extremities, which becomes pigmented, elevated and warty over time. There is a 20% risk of progression to squamous cell carcinoma. The etiology is presumed to be sun exposure and the treatment is biopsy, excision and cautery.14
Epidermal inclusion cysts can occur at any age and are equally prevalent in males and females. They arise from hair follicles and appear as smooth, round elevated cysts filled with keratin. Ablation of entire cyst walls is necessary for eradication.
|
|
|
|
|
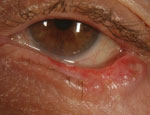
Lid notching, ectropion and missing lashes accompany this case of eyelid basal cell carcinoma.
|
Sebaceous cysts clinically look like epidermal inclusion cysts; however, they arise from blocked glands of Zeis, meibomian or sebaceous glands. They are filled with epithelial cells, keratin, fat and cholesterol crystals. They are treated with expression or surgical excision.
Acquired nevus begins in childhood when the basal epithelium migrates to the dermis surface. They may appear deeply pigmented or amelanotic. The lesion may be flat or pedunculated. A key characteristic is maintenance of lashes through the lesion. While lid nevi are benign, about 5% will transform to malignant melanoma and therefore should be photo-documented and closely monitored.15
Sebaceous cell carcinoma arises from the glands of Zeis at the lid margin or the meibomian glands in the deep tarsus. Sebaceous cell carcinomas account for 2% to 7% of eyelid tumors.16 Clinically, they appear as a solitary lesion with diffuse lid thickening. There is a loss of lashes. They are frequently misdiagnosed as recurrent chalazion, chronic meibomitis or blepharoconjunctivitis.16 These can be aggressive tumors, with orbital extension in 17% of cases and systemic metastasis in 8% of cases. Biopsy/excision is recommended for suspected sebaceous cell carcinomas.16
Basal cell carcinoma is the most common tumor of the skin with >400,000 people treated annually.17 It has been associated with sunlight exposure and Demodex infestation. On the eyelids, 65% will involve the lower lid, 15% the medial canthus, 15% the upper lid and 5% the lateral canthus.17 They appear as pearly, waxy translucent lesions with rolled borders. There is often telangiectasia near borders and loss of lashes. Tumor extensions are possible, but no distant metastasis. The mortality rate is <1%.17
Primary malignant melanoma accounts for only 1% of malignant eyelid tumors.18 They may be either a primary lesion or a metastasis from another location. They generally appear in sun-exposed areas as a variably pigmented mass, which can bleed or ulcerate. Malignant melanoma must be histopathologically proven, and early diagnosis is critical, since prognosis depends on if the lesion metastasizes.18
Disorders of the Lashes
Growth of lashes from within the meibomian glands is distichiasis. Congenital distichiasis is caused by the epithelial germ cell’s failure to differentiate completely to meibomian glands. It is dominantly inherited with complete penetrance and may be isolated or associated with ptosis, strabismus or congenital heart defects. Acquired distichiasis is seen on the lower lid, where the lashes may be either pigmented or non-pigmented. It is associated with chronic inflammation.
|
|
|
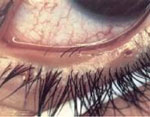
Distichiasis results when lashes grow outward from within the meibomian glands.
|
|
Madarosis is a decrease or loss of lashes. It is commonly seen in patients with long-standing anterior blepharitis, but is also seen with tumor, thermal burns and trichotillomania. It can be associated with alopecia, atopic dermatitis, systemic lupus and icthyosis.
Hypertrichosis is a benign condition with excess or abnormally long lashes. It can either be congenital or drug induced. Some drugs that have been known to cause hypertrichosis include: prostaglandins (e.g., latanoprost, travoprost, bimatoprost), phenytoin, acetazolamide, streptomycin, cyclosporine, psoralen, diazoxide and minoxidil.
Poliosis is premature whitening of the hair, lashes and eyebrows. It is associated with vitiligo, Waardenburg syndrome (iris heterochromia, white forelock) or chronic lid margin inflammation.
Infection
The eyelids are prone to infection from multiple sources. Molluscum contagiosum
is an itchy viral infection (poxvirus) of the skin that presents with white/pink dome-shaped, smooth, waxy or pearly umbilicated papules 2mm to 5mm in diameter. It is spread either by direct contact or via fomites. Immunocompromised individuals may have more widespread infection and can be difficult to treat. Lesions generally regress spontaneously after one to two years, and treatment is only indicated for cosmesis and prevention of spread. The condition is most common in children as a benign childhood entity; when seen in adults, it may represent a sexually transmitted disorder and should be treated as such until discovered otherwise.
Blepharitis is a common condition (found in 70% of the population) affecting the eyelid margins. Because of its ubiquity, it is often overlooked in the early stages. Associated morbidities include dry eye, loss of visual function and loss of well being and ability to carry out activities of daily living. Over time, damage to the lids occurs, including trichiasis, notching, entropion and ectropion. The cornea may be damaged due to inflammation and limbal stem cell deficiency, leading to scarring, loss of surface smoothness and optical clarity. Other signs of chronic blepharitis include crusting and collarettes, margin telangiectasia, marginal keratinization, decreased and brittle lashes, poliosis and distended or blunting of meibomian glands.
|
|
|
|
|
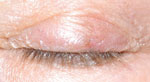
Mild actinic keratitis may go unnoticed without careful attention to the lid exam.
|
|
|
|
|
|
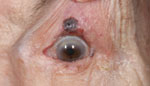
Malignant melanoma. Be sure to raise the upper lid if you suspect a lesion is within the folds of skin.
|
Blepharitis has been separated into anterior vs. posterior blepharitis. Anterior blepharitis involves the anterior portion of the lid margin, including the lash follicle, while posterior blepharitis involves the meibomian glands.
Normal (common) bacteria of the eyelids include Staphylococcus epidermidis (95.8%), Proprionibacterium acnes (92.8%), Corynebacterium sp. (76.8%), Acinetobacter sp. (11.4%), and Staphylococcus aureus (10.5%).19 The lids may also be colonized with Demodex.
Demodex is an eight-legged mite that lives in hair follicles and oil glands. There are 65+ species of Demodex, only two of which live on humans (D. folliculorum and D. brevis), with a life span of two to three weeks. They are spread either through direct contact or in dust and towels containing eggs. They eat skin cells, hormones and oils in the follicles and glands. In addition to lid margin dysfunction, Demodex has been implicated in rosacea, seborrheic dermatitis and other skin conditions.20
Demodex signs include cylindrical dandruff around a “volcano-like” lash base. Dry eye symptoms increase with Demodex infestation with more than 85% of patients showing evaporative dry eye.21
Demodex is acquired shortly after birth, and bio load increases with age. Demodex has been correlated with other inflammatory ocular states such as Salzmann’s nodular degeneration, ocular rosacea and peripheral ulcers. Studies show nearly 90% to 100% of people with blepharitis have Demodex.22
Blink and You’ll Miss It
The eyelids are easy to pass over during an ocular exam. The periorbital region feels oddly foreign to many eye care professionals. Yet, the lids are vitally important to not only the health of the eye, but can indicate systemic health integrity as well. A systematic approach to lid examination, which begins chairside, ensures the eyelids will not be overlooked.
2. Diaper CJ. Wake up to floppy eyelid syndrome. Br J Ophthalmol. 2013;97(11):1363-4.
3. Muniesa MJ, Huerva V, Sánchez-de-la-Torre M, et al. The relationship between floppy eyelid syndrome and obstructive sleep apnoea. Br J Ophthalmol. 2013;97(11):1387-90. doi: 10.1136/bjophthalmol-2012-303051.
4. Thean JH, McNab AA. Blepharoptosis in RGP and PMMA hard contact lens wearers. Clin Exp Optom. 2004;87(1):11-4.
5. Sobel RK, Allen RC. Incidence of bilateral Marcus Gunn jaw-wink. Ophthal Plast Reconstr Surg. 2014;30(3):e54-5. doi: 10.1097/IOP.0b013e31829bb405.
6. De Diego-Sastre JI, Prim-Espada MP, Fernandez-Garcia F. The epidemiology of Bell’s palsy. Rev Neurol. 2005;41:287–90.
7. Holland NJ, Weiner GM. Recent developments in Bell’s palsy. [Review] BMJ. 2004;329(7465):553–57.
8. Prescott CA. Idiopathic facial nerve palsy (the effect of treatment with steroids) J Laryngol Otol.1988;102:403–7
9. Zandian A, Osiro S, Hudson R, et al. The neurologist’s dilemma: a comprehensive clinical review of Bell’s palsy, with emphasis on current management trends. Med Sci Monit. 2014;20:83-90. doi: 10.12659/MSM.889876.
10. Turgeon RD, Wilby KJ, Ensom MH. Antiviral treatment of Bell’s palsy based on baseline severity: A systematic review and meta-analysis. Am J Med. 2014;pii: S0002-9343(14):01215-7. doi: 10.1016/j.amjmed.2014.11.033. [Epub ahead of print].
11. Davagnanam I, Fraser CL, Miszkiel K, et al. Adult Horner’s syndrome: a combined clinical, pharmacological, and imaging algorithm. Eye (Lond). 2013;27(3):291-8. doi: 10.1038/eye.2012.281.
12. Renton AE, Pliner HA, Provenzano C, et al. A genome-wide association study of myasthenia gravis. JAMA Neurol. 2015. doi: 10.1001/jamaneurol.2014.4103. [Epub ahead of print].
13. Mlakar J, Kocjan BJ, Hošnjak L, et al. Morphological characteristics of conjunctival squamous papillomas in relation to human papillomavirus infection. Br J Ophthalmol. 2014;pii: bjophthalmol-2014-306087. doi: 10.1136/bjophthalmol-2014-306087. Epub ahead of print.
14. Chetty P, Choi F, Mitchell T. Primary Care Review of Actinic Keratosis and Its Therapeutic Options: A Global Perspective. Dermatol Ther (Heidelb). 2015. [Epub ahead of print].
15. Loghavi S, Curry JL, Torres-Cabala CA, et al. Melanoma arising in association with blue nevus: a clinical and pathologic study of 24 cases and comprehensive review of the literature. Mod Pathol. 2014;27(11):1468-78. doi: 10.1038/modpathol.2014.62. Epub 2014 Apr 18.
16. Sullivan TJ. Squamous cell carcinoma of eyelid, periocular, and periorbital skin. Int Ophthalmol Clin. 2009;49(4):17-24. doi: 10.1097/IIO.0b013e3181b7ecd1.
17. Allali J, D’Hermies F, Renard G. Basal cell carcinomas of the eyelids. Ophthalmologica. 2005;219(2):57-71.
18. Sanchez R, Ivan D, Esmaeli B. Eyelid and periorbital cutaneous malignant melanoma. Int Ophthalmol Clin. 2009;49(4):25-43.
19. Osato MS. Normal ocular flora. In: Pepose JS, Holland GN, Wilhelmus KR, eds. Ocular Infection and Immunity. St Louis: Mosby;1996:191–9.
20. Hom MM, Mastrota KM, Schachter SE. Demodex. Optom Vis Sci. 2013;90(7):e198-205. doi: 10.1097/OPX.0b013e3182968c77.
21. Rusiecka-Ziółkowska J, Nokiel M, Fleischer M. Demodex - an old pathogen or a new one? Adv Clin Exp Med. 2014;23(2):295-8.
22. Bhandari V, Reddy JK. Blepharitis: always remember Demodex. Middle East Afr J Ophthalmol. 2014;21(4):317-20. doi: 10.4103/0974-9233.142268.

