Download PDFClick here to download a PDF of this article from our July issue. |
A condition as pervasive as dry eye is sustained by the rhythms of modern life. Our reliance on digital screens, our poor sleep habits and dietary choices, the harsh climates we expose our eyes to, the medications we take as well as the conditions they treat, the cosmetics and contact lenses we wear—all these are on-ramps for the family of conditions we call ocular surface disease, chief among them dry eye.
Against this backdrop, in late 2020 the Tear Film and Ocular Surface Society (TFOS) created a new workshop comprised of 158 clinical and academic researchers from 38 countries to systematically evaluate the scientific literature on how a patient’s day-to-day experiences—some volitional, some not—give rise to dry eye, digital eye strain, microbial keratitis, pterygia and a host of other conditions.
The TFOS Lifestyle Workshop, as it’s called, is in the process of publishing 10 reports in The Ocular Surface journal that will surely be the most definitive statement attempted thus far on these often-unavoidable triggers for ocular surface disease. In advance of that, the society released a series of summary videos on May 6 that sketch out the efforts and the insights of the workshop’s eight subcommittees.
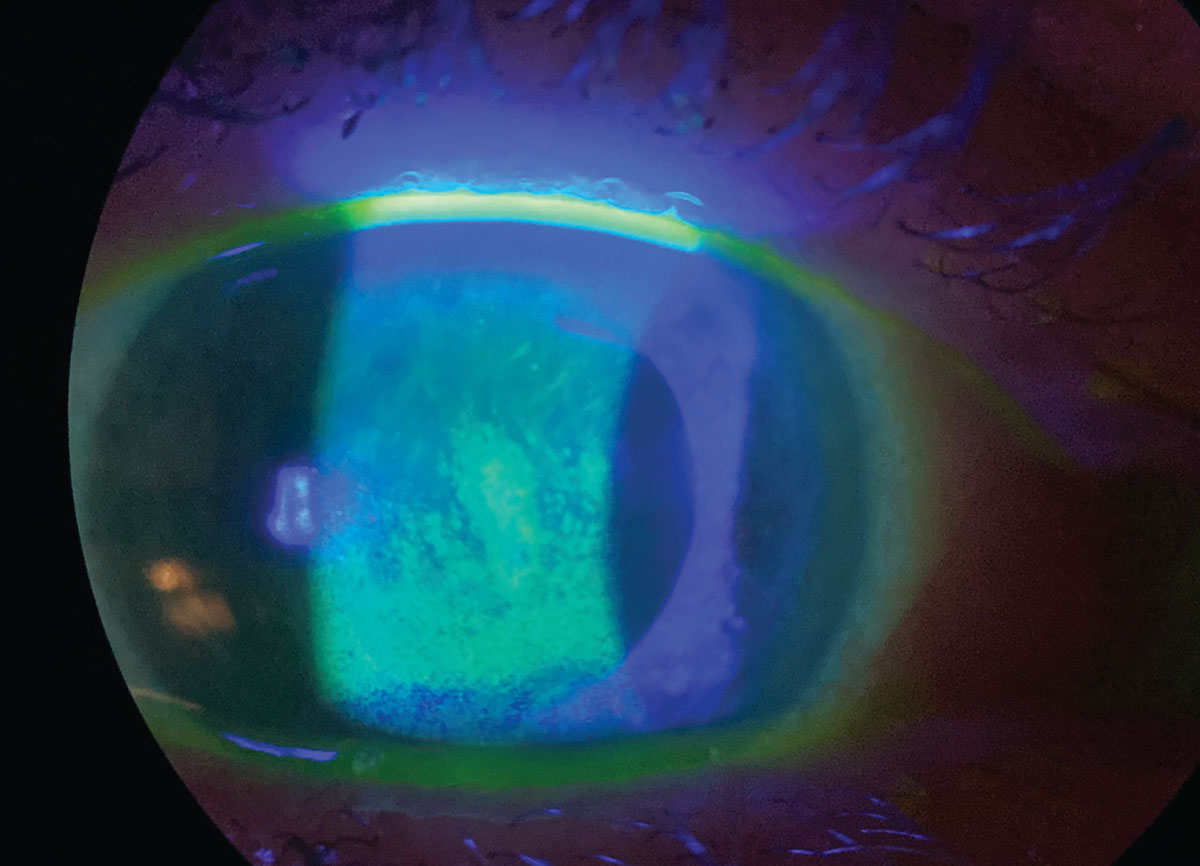 |
| An example of dry eye compromising the ocular surface, seen with sodium fluorescein staining. Dr. Craig believes upon the release of the full reports, education on topics like dry eye will be reciprocally exchanged by clinicians and their patients, leading to increased awareness. Click image to enlarge. |
Below, we’ll walk you through those summaries using quotes from the video presentations as well as original interviews conducted with several participants for added context. This article will be expanded upon following publication of the reports in the coming weeks.
“People are exposing themselves to so many ocular risk factors nowadays,” says Dr. Jennifer Craig, a professor at New Zealand’s University of Auckland and Chair of the TFOS Lifestyle Workshop. With the ubiquity of digital screens, this is starting at such a young age; furthermore, people are living longer. “If we’re causing damage at a younger and younger age, we’ve got a lot of years to live with the consequences of that damage.”
Here’s what Dr. Craig and her colleagues advocate in response.
Contact Lens Wear
Those who wear contact lenses consistently will likely point to convenience and cosmesis as motivators, and this is corroborated in this specific subcommittee’s section. Patients wearing contacts reported better quality of life scores when compared with those wearing glasses in demographics of kids, adults and elderly alike, citing better vision quality and comfort leading to increased satisfaction.
Despite this modality’s obvious advantages, especially when playing sports, contact lenses may contribute to or exacerbate dry eye disease signs or symptoms. This subcommittee identified nine different areas of lifestyle choices regarding contact lens use and wear that could affect dry eye and other ocular surface effects.
The first category as it relates to contact lenses is how lenses are obtained. “Purchasing lenses from unregulated outlets in particular is a concern for patients wearing cosmetic lenses or sort of party type lenses that certainly impact the risk of microbial keratitis. There’s very good evidence around that fact, and some of the issue relates to them being shared with friends,” Dr. Lyndon Jones, of the School of Optometry and Vision Science at University of Waterloo, Canada and the primary author of this report, states.
Age is a significant risk factor in ocular surface health and continued contact lens success. Young children have fewer complications than adults, likely due to parents managing their wear. As the ocular surface worsens with age, so does the contact lens complication rate, to some extent. Complications with contact lenses are highest in young adults, attributed to less people in this age-range adhering to proper hygiene of the device. As such, the subcommittee recommends that safety education and continual connection with an eyecare provider are integral parts of ensuring hygiene compliance in patients. Dry eye disease, meibomian gland dysfunction and presbyopic contact lens wearers are all at risk of decreased success.
The COVID-19 pandemic brought with it unforeseen complications in all aspects of life and will be discussed in other subsections of this article. However, as it related to contacts, the subcommittee highlighted that there is a great lack of existing evidence for what patients should do when unwell in general, but especially with viral upper respiratory tract infections such as COVID. Some evidence points to unwellness mapping onto corneal inflammatory events associated with contact lens wear, prompting Dr. Jones to suggest affected patients “refrain from contact lens wear until they are fully better.”
Despite this potential link, COVID did not end up directly impacting typical contact lens–associated risk factors; instead, performance may have been lessened from mask-associated dry eye, increased screen time and hand sanitizer use.
Other health concerns such as thyroid eye disease and diabetes, both in their ocular manifestations and the medications used, can complicate lens wear. Complications can also result after cosmetic or refractive surgeries, due to potential corneal shape changes, eyelid configuration or contour modifications.
Vision and comfort decline as the tear film thins, leading environmental factors like decreased air temperature and relative humidity to increase dryness of the eyes through a less stable tear film and subsequent tear film evaporation. Also having the ability to impact lens wear negatively are factors of high altitude, pollution, wind, dust and fumes.
Reliance on digital devices results in a compromised environment of the ocular surface and exacerbates difficulties in contact lens wear, as reduced blink frequency and blink amplitude lead to complaints of eye strain, dry eyes, burning, irritation and blurry vision. The contact lens subcommittee report stresses that it is important to remember that full correction is needed for contact lens wearers to achieve maximal performance, especially when heavily using digital devices. Multifocal performance is better than with monovision lenses and low-level astigmatism should be fully corrected for as well.
With industrial occupations, contact lens wearers should be cautious of foreign bodies, chemical fumes, vapors and aerosol droplets, as these can pose problems. Flying is also well-known to decrease contact lens performance from the low humidity and resultant dry environment.
Interestingly, a high risk-taking personality was found to be a better predictor of compliance than factors of age, sex or practitioner perception, with those that possess this trait being much less compliant than their counterparts.
The report notes that 99% of contact lens wearers admit they engage in at least one hygienic risk behavior, so it is no wonder that microbial keratitis and other contact complications account for one million US doctor visits each year. Risk of microbial keratitis development increases with sleeping in lenses, which is the single largest risk factor for serious complications. Others include topping off lens solutions in cases, using tap water to store lenses and infrequent cleaning or replacing of lenses.
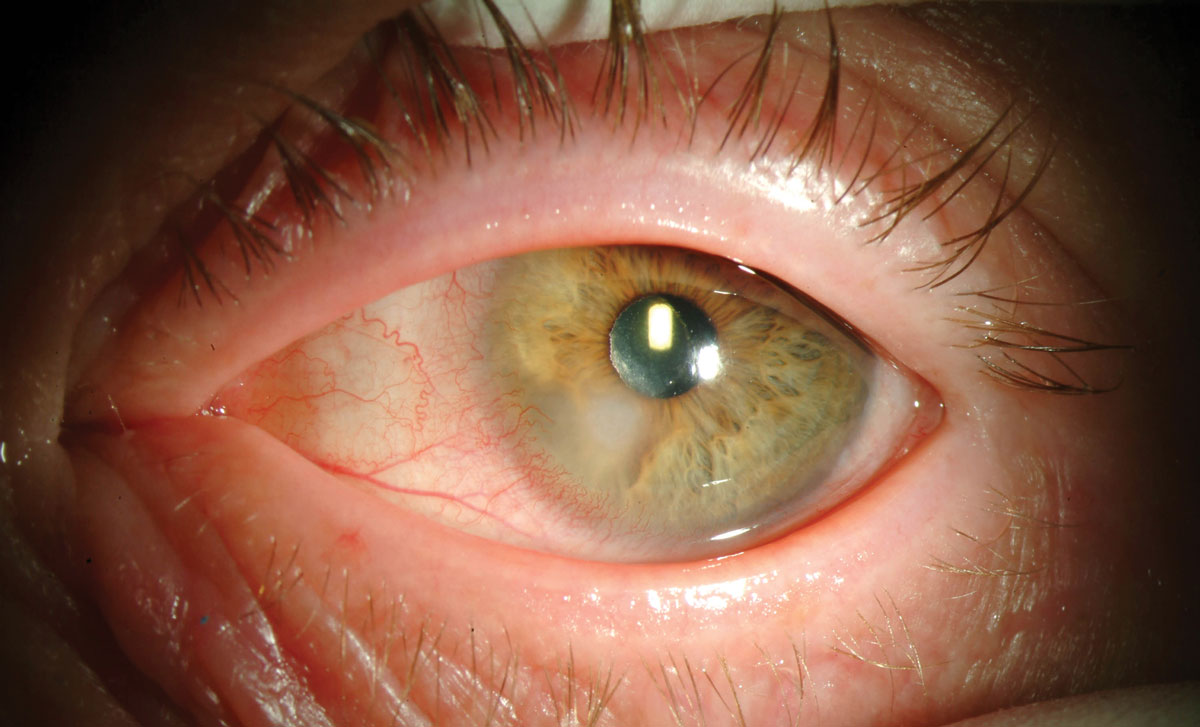 |
| An example of Pseudomonas microbial keratitis infection, a class of infection which can be exacerbated by contact lens non-adherence. Click image to enlarge. |
Other lens complications have been reported in wearers after smoking tobacco, marijuana or e-cigarettes and those under the influence of drugs or excessive alcohol consumption. These included increased inflammatory and infective rates and decreased performance.
A new conversation has been at the forefront of consumers’ mind—how their use of contact lenses impacts the environment. The increased popularity of daily disposables has naturally increased the volume of blister packs and lenses disposed. Fortunately, environmentally friendly options are now available for disposal and recycling of dailies, with the contact lens industry making increasing efforts to step toward end-of-life options for contacts. On the OD’s end, the patient’s provider of contacts plays an important role in informing them of options to dispose and recycle their contacts locally, explicitly noting that flushing lenses down the drain is harmful for the environment.
Daily disposables are more convenient for patients, since there is no upkeep, which is also probably why they display the highest rate of compliance with replacing lenses on time and display lowest complication rates. However, if patients are reusing daily disposables, they are actually most at risk of developing complications, since the practitioner doesn’t go over proper hygiene with these types of lenses, as they’re meant to be disposed of
Perhaps related to patients reusing dailies is that they “don’t think about contact lenses as being medical devices. They think of them as being a commodity product, so I think the big thing for me is to give practitioners the opportunity to be able to get that message across to patients that lenses are safe—unless you don’t do what you’re supposed to. In which case, the outcome can be not so nice,” Dr. Jones points out. This could also have been exacerbated by what he explains as the pandemic causing patients to avoid frequent follow-up to save time and costs, but ultimately contributing to reduced satisfaction with lenses and increased risk. This could potentially have driven daily users to start reusing their lenses.
The systematic review covered by this subcommittee looked at the association of lifestyle factors and soft contact lens dropout. They found, not surprisingly, that the most common reason for dropout was lens discomfort. The most common reason for dropout among presbyopes using multifocals was vision quality. However, the complaints of discomfort suggest contact lenses are contributing to dry eye symptoms in a substantial patient base.
Cosmetics
Few consumer products are as problematic as cosmetics—used worldwide and all throughout history but defined, manufactured and regulated in very inconsistent ways. As the eye makeup industry alone is valued at $15.5 billion, the prominence with which these cosmetics are used should prompt more stringent safety protocols when it comes to ingredients. Unfortunately, this is not the reality of the industry right now, with TFOS outlining a “number of these ingredients can act as allergens, carcinogens, endocrine disruptors, immunosuppressants, irritants, mutagens, toxins and/or tumor promoters and may damage the ocular surface and adnexa.”
Covered in the report are the most deleterious offenders known so far that have made their way into cosmetic products, including benzalkonium chloride, chlorphenesin, formaldehyde-releasing compounds, parabens, phenoxyethanol, phthalates, prostaglandin analogues, retinoids (vitamin A metabolites), salicylic acid, tea tree oil (terpinen-4-ol).
Benzalkonium chloride may induce tear film instability, goblet cell loss, conjunctival squamous metaplasia and apoptosis as well as a disrupted corneal epithelial barrier. Application of this on the eyes can result in irritation, burning, itching, foreign body sensation, conjunctival hyperemia, blepharitis, meibomian gland loss, DED, glaucoma surgery failure and anaphylaxis. It’s not surprising, based on these manifestations, that the compound has been found toxic to corneal, conjunctival and meibomian gland epithelial cells in vitro at levels much, much lower than approved for eye makeup use.
Formaldehyde-releasing compounds and parabens have similarly been found toxic to corneal, conjunctival and meibomian gland epithelial cells in vitro. There has been increased attention in public health on the potential for formaldehyde to cause damage due to its mutagenic, carcinogenic and pro-allergenic properties, and has even been classified as carcinogenic for humans by the International Agency for Research on Cancer. Parabens, used in over 22,000 US cosmetics, act as allergens and endocrine disruptors, the latter owing to their estrogen potency and anti-androgen activity. These compounds may also increase malignancy risk.
Phthalates are compounds used as solvents in cosmetics removers or fragrances and are sometimes found as plasticizers in packing materials that can leach into cosmetics unintentionally. They, like parabens, are linked to endocrine disruption with anti-androgen activity, as well as to reproductive disorders, hepatotoxicity, neurotoxicity and more. They negatively impact corneal endothelial cell growth and viability, consequently leading to dibutyl phthalate being banned in Europe for cosmetic use, although it still exists in many US products.
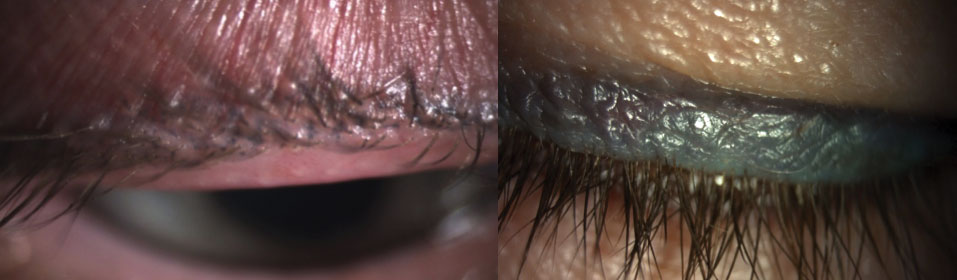 |
| Pigment fade (left) and spread (right), with the tattooed eyeliner extending upward further than the thin line originally applied, of permanent makeup. Both patients have dry eye with MGD. Click image to enlarge. |
Tea tree oil is yet another endocrine disruptor with anti-androgen activity, specifically linked to promoting meibomian gland dysfunction. However, unlike the others listed above, it does possess some valid medical uses, like in relieving Demodex blepharitis. However, its active ingredient, terpinen-4-ol, should be used judiciously since it may contribute to antibiotic resistance in human pathogens, may induce gynecomastia in boys and has been found to kill all meibomian gland and corneal and conjunctival epithelial cells at one percent concentration after only 90 minutes in vitro. However, it should be noted that epithelial cells in the living eye are never exposed to 90 minutes of direct exposure, so the clinical implications are far less well understood. Nevertheless, the European Cosmetic Toiletry and Perfumery Association recommends “tea tree oil should not be used in cosmetic products in a way that results in a concentration greater than 1% oil being applied to the body.”
It is not just which specific kinds of makeup are applied that can cause problems, but how. Sharing eye makeup can encourage bacterial and viral Demodex transmission. Repeatedly using multi-use cosmetic products can introduce microbes into containers; this has been corroborated by 79% of used mascaras testing positive for Staphylococcus aureus and 13% for Pseudomonas aeruginosa. Even further, contamination rates are linked to amount of use, product age and the number of users.
This subcommittee’s systematic review question tackled if eyelash growth products are linked to ocular surface disease signs or symptoms, but based on the current literature, it was unable to come up with clear conclusions.
However, the subcommittee was able to provide some concrete recommendations:
Provide information about a cosmetic’s function, toxicity, indications, contraindications, durability and expiration date, as well as concentration.
Perform well-controlled, high-quality studies to examine acute and chronic effects of eye cosmetic ingredients and procedures on the ocular surface and adnexa.
Develop guidelines to assess safety and tolerability of eye cosmetic products.
Establish more stringent and rigorous oversight of eye makeup industry.
Develop standardized and universally accepted definitions of the words ‘clean’ and ‘natural’ as they relate to cosmetics.
Educate eye care providers and consumers about risks associated with ingredients in eye cosmetic products.
Digital Device Use
It has been widely discussed that our dependence on modern technology is likely causing all sorts of problems, from cognitive changes in children to sleep problems and more. While digital eye strain is one of these effects, this subcommittee refreshingly does not try to offer solutions in terms of lowering your digital load. The ostensible recommendation is just not feasible in today’s world, and they seem to recognize that.
Instead, this report covers how digital eye strain is often exacerbated by other underlying conditions and offers solutions as they relate to those. First, though, the group had to define digital eye strain, which has been floated around with a multitude of other ill-defined phrases to describe the phenomenon, such as ‘computer vision syndrome’. The subcommittee defines digital eye strain as the development or exacerbation of recurrent ocular symptoms and/or signs, related specifically to digital device screen viewing.
This report looked at many different types of displays and characteristics of using them, such as size, resolution, refresh rate and viewing distance, all of which can have an effect on the ocular surface.
Diagnosing digital eye strain comes with challenges, one of which is in relation to the questionnaires used. Two of the most popular, the Computer Vision Syndrome Questionnaire (CVS-Q) and the Computer-Vision Symptom Scale (CVSS17), both possess the problems of not addressing if symptoms are experienced outside of digital device use. They look at frequency and severity of symptoms, but as subcommittee chair James Wolffsohn, FCOptom, PhD, of the College of Health and Life Sciences’ School of Optometry, explains, “there are no criteria to link the questionnaire responses specifically to digital device use and many require only one symptom to be reported, hence we see a very high prevalence.”
With the questionnaires asking about symptoms of burning, eye pain, headache, eye redness, photophobia, tearing, repeated/frequent blinking, heavy eyelids, itching, blurred vision at distance and near, double vision, eyestrain and foreign body sensation, it's recognized that many of these could be indications of other underlying problems. Reported rates of digital eye strain vary widely, from 32% to 98%, depending on diagnostic criteria and occupation.
Based on the widely used questionnaires and such variable rates reported, the subcommittee concluded that “currently there is no robust algorithm to diagnose digital eye strain and many people ‘diagnosed’ with digital eye strain probably have dry eye disease, uncorrected/not fully corrected refractive error and/or a binocular vision anomaly, each of which has their own diagnostic criteria and established evidence-based management strategies.”
Hoping to improve how true digital eye strain is diagnosed in the future, the subcommittee suggested how to adequately assess the condition. This involves individuals reporting development or exacerbation of recurrent ocular symptoms (and possibly signs) specifically when using digital devices. It is important for eyecare providers to check with their patients that any increase in ocular symptoms (or signs) while using digital devices are not also occurring with non-digital tasks.
 |
| While device use can lead to digital eye strain, underlying conditions need to be checked in order to determine if the strain is a symptom originating elsewhere. Click image to enlarge. |
Reasons for digital eye strain occurring are mainly due to mechanisms of blink abnormalities that cause ocular surface and tear film alterations. This may be caused by underlying vision or accommodation deficiencies as well as oculomotor function that can induce visual disturbances like asthenopia, blurred vision and focusing and accommodative difficulties.
The report did cover possible therapies or management strategies that could improve symptoms of digital eye strain, and this was their topic of systematic review.
“Oral omega 3 supplementation does seem to have a beneficial effect on digital eye strain,” Dr. Wolffsohn says. “We know that omega 3 is good for ocular health in terms of anti-inflammatory effects, and as we know that ocular discomfort generally has an inflammatory component, so this may explain its benefit.”
Likely effective management strategies include blink and break reminders, which can be set up on devices, probiotics, eyelid warming, humidifiers and using e-paper when possible (like a Kindle). Notably, however, the blue-light blocking lenses that have become popular in some circles were shown to be ineffective—or, rather, to lack solid scientific evidence of support for recommended use—as was antioxidant supplementation.
Future research to clarify what is actually effective will hopefully combat the productivity lost through this condition and improve quality of life. For practitioners, be mindful not to recommend patients invest in blue-light blocking lenses when they are often costly and have thus far failed to show documented clinical benefits.
Elective Medications & Procedures
Just as with cosmetics, elective or semi-elective procedures and medications are meant to enhance quality of life and lifestyle. However, no surgical or pharmaceutical intervention is without potential side effects, and those targeting the ocular surface are certainly no exception.
Elective medications can cause ocular surface disease through ocular toxicity of preservatives, ingredients or excipients like surfactants, co-solubilizers and preservative aids, pH or tonicity of the formula or from medication abuse.
Benzalkonium chloride is the main preservative known to cause toxic effects, outlined in the Cosmetics section. Preservatives can also cause allergic and immune-inflammatory effects. Artificial tears, gels and ointments often used for dry eye disease, while offering benefits, can cause their own adverse reactions even if non-preserved. Alternative medicines like aloe vera and manuka honey have both been recommended for dry eye disease. Aloe use can result in ocular allergies, redness, irritation or burning, and manuka honey or honey eye drops or gels can produce conjunctival inflammation and should not be used if patients have an allergy to bee products.
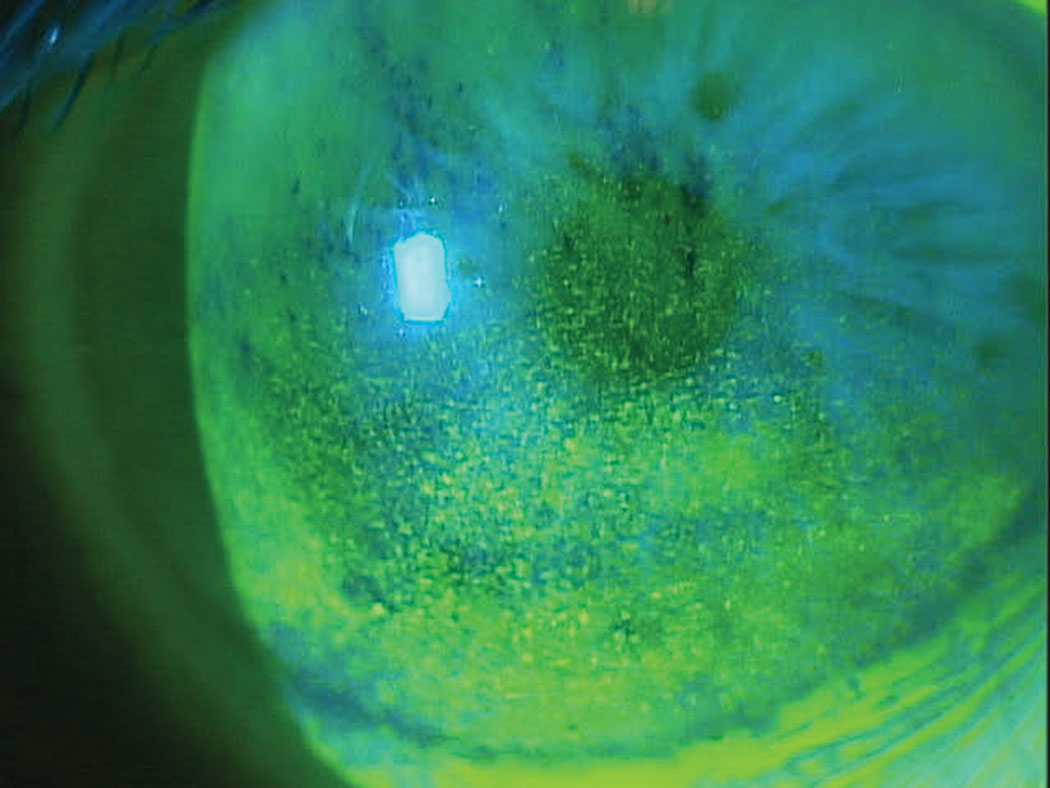 |
| Benzalkonium chloride can cause a host of problems to the ocular surface; in this case, toxicity is present. Click image to enlarge. |
Antihistamines, mast cell stabilizers and dual-acting drugs are all anti-allergic ocular therapies identified to cause a wide range of negative effects on the eye, as can topical alpha-adrenergic receptor agonists and non-steroidal anti-inflammatory drugs.
Changing gears slightly to periocular topical products, eyelid hygiene is practiced with antimicrobials like tea tree oil, linalool, hypochlorous acid and aloe vera. Tea tree oil can cause discomfort and other effects outlined in the Cosmetics section. There has been evidence suggesting that compliance with eyelid scrubs was more likely for those who reported recent dry eye symptoms as opposed to those with longstanding symptoms, which may indicate different processes in new vs. long-term disease processes.
Sunscreens, topical steroids or ointments, and creams can cause negative ocular surface effects. Mainly, ones to look out for are topical medications used for acne and rosacea containing alpha hydroxy acid (glycolic acid), beta hydroxy acid (salicylic acid), retinoids and Ivermectin.
Systemic medications can equally contribute to ocular surface problems, with emphasis placed on conditions of Stevens-Johnson syndrome and toxic epidermal necrolysis. Dr. José Gomes, the main author of this subcommittee, works in the Department of Ophthalmology and Visual Sciences at the Federal University of Sao Paulo. He brings attention to the fact that these conditions “develop after patients with genetic predispositions take medications to treat a specific infection and develop an acute reaction that can evolve to chronic cicatricial changes in the ocular surface, compromising the vision of the patient.” Going along with this, stress should be placed on balancing the potential risks and benefits of systemic medications like cold meds, which are commonly used in the population.
Procedures focused on or around the eyes, which include blepharoplasties, ptosis repair, canthoplasty and brow lifts, can cause various types of ocular surface damage. Botulinum toxin injection is a first-line therapy for blepharospasm and hemifacial spasm and has led to ptosis in 8.4% to 13.4%, transient tearing in 5% to 10%, dry eye disease in 3% to 7.5%, photophobia in 2% and ectropion in 1%. Preventative measures to minimize these effects are specified as using smaller volumes, seating the patient an upright position, avoiding rubbing or massaging and exercising the treated muscles.
Using CO2 or Er-YAG lasers can result in conjunctival hyperemia, corneal ulceration and bullous keratopathy or ectropion. Refractive surgery is well-known in its postoperative potential to induce dry eye. With LASIK, dry eye persists in up to 94.8% of patients at one day, 85.4% of patients at seven days and 59.4% of patients at 30 days. More worrying is LASIK-induced neuropathic epitheliopathy, which develops in up to 4% of post-LASIK patients. Photorefractive keratectomy patients had dry eye up to six months post-op in 43% in one study. However, risk factors are known, being pre-existing dry eye, female sex, Asian race, contact lens use and older age.
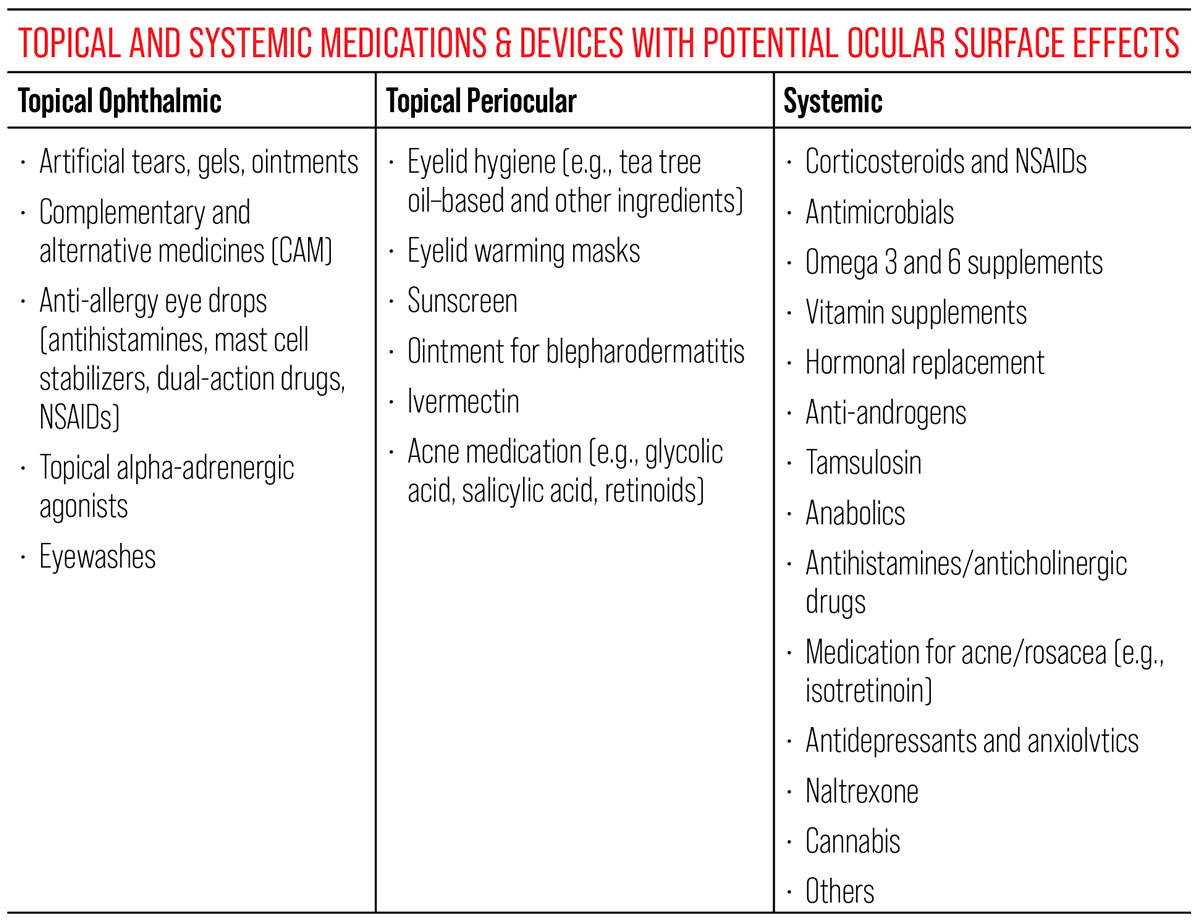 |
| Topical and systemic medications and devices can contribute to ocular surface effects; here is an overview. Click image to enlarge. |
There has been some questioning around the type of refractive tool used and if different dry eye outcomes exist between their use. What is clear is that flap configuration parameters like flap depth and size and hinge location do affect dry eye development. However, results are mixed when looking at whether a femtosecond laser or a mechanical microkeratome provides better results. What else is apparent is that SMILE does result in less corneal nerve damage than LASIK due to no need for flap creation, which may make it less prone to cause dry eye after surgery.
Other procedures that have resulted in dry eye are corneal crosslinking, with epi-on procedures displaying better OSDI scores than epi-off, cataract removal and gamma knife radiosurgery for trigeminal neuralgia. With cataract removal, improvement in dry eye typically occurs by three months post-op, although may take up to six months for patients with diabetes. Conventional phacoemulsification should be used rather than femto laser–assisted cataract surgery for people who already have dry eye and they should also be treated preoperatively.
Taking the multitude of procedures and medications into consideration, Dr. Gomes points to a couple ways to prevent or reduce dry eye and other ocular surface problems caused by this large class of products.
“Adverse events may be reduced by changing to a different class of topical medication, using corticosteroids, lubricating the eyes frequently and reducing exposure to preservatives.”
He also puts responsibility on practitioners to “stress that increasing the awareness of the potential risks, benefits and consequences will help patients to make the right decisions when considering when to undergo elective procedures and use medications.”
Environment
We cannot always change the environment we live and exist in, but at least the knowledge of which factors are contributing to ocular surface health can aid in developing solutions and therapies.
The climate itself offers many factors that can contribute to ocular surface health. Extreme high or low temperatures both in- and outdoors has been associated with dry eye, and temperature variations may be related to allergic conjunctivitis. Low relative humidity has been linked to greater ocular irritation, with one study showing improvement of OSD symptoms with indoor humidity of 30% to 40%. Dry eye symptoms are exacerbated in low humidity environments like in deserts, airplane cabins and during dry seasons. Wind speed is not well-documented in relation to ocular surface effects, but cases of corneal freezing and frostbite exist in ultra-marathon runners exposed to high wind speed and military freefall parachutists experiencing high wind, respectively. Dew point—the temperature at which air must be cooled to reach maximum water saturation—may serve as a protective factor against dry eye at higher levels.
High altitude is known for causing short-term effects of corneal thickness and long-term effects of dry eye and pterygium due to hypobaric conditions, stronger ultraviolet (UV) radiation compounded by higher number of sunshine hours, low air pressure and dry and cold air. Often coinciding with high altitude, UV radiation is associated with conjunctival and eyelid malignancies and climatic droplet keratopathy and primarily affects outdoor workers.
Recently, more extreme weather conditions like increased temperatures and precipitation have caused longer pollen seasons and higher indoor and outdoor mold spore concentrations, resulting in more allergic conjunctivitis and ocular allergic symptoms.
Pollution is another source of negative health effects, whether indoor or outdoor. This subcommittee’s systematic review determined whether specific chemical pollution compounds are related to dry eye incidence. They found it to be greater with exposure to air pollutants of NO2 and CO, as well as with soil pollution from chromium. However, there was no increased dry eye prevalence with particulate matter. Dry eye disease and conjunctivitis have also been associated with pollution.
Indoor pollution can be caused by factors of humidity, illumination, temperature, air velocity, air conditioning, toluene and paint thinners, construction materials, particles and mold, gaseous and particulate matter. Ocular symptoms can occur from these factors, mostly including strain, dry, itching or irritated eyes and are correlated with dry eye symptoms and signs. Two conditions of note are “sick building” and “sick house” syndromes, which display ocular symptoms. Similar in nature, both describe a scenario where the occupant experiences acute health effects directly linked to spending time in a work building or the home and symptoms subside once away from the premises.
The report devotes some attention to the common finding of pterygia, which has a fairly high prevalence of 10% to 12%, with higher incidence closer to the equator line. This is unsurprising as it is linked to prolonged sunlight exposure, higher altitude and time spent outdoors.
| Pterygia are fairly common among those living in higher altitudes or closer to the equator. Click image to enlarge. |
Covered last in this section is the range of ocular surface injuries that can occur. Chemical injuries can occur from occupational exposure, especially from construction and agricultural work. Household exposure can result from cleaning agents and hydrogen peroxide. Thermal injuries happen from direct flames, scalding liquid, burning items, curling irons or fireworks. Many of these are risks that people are exposed to daily, so informing patients of the risks of these agents or exposures may help them to be cautious especially toward their eyes.
Nutrition
Like some of the other topics explored, this report found the scientific grounding to be lacking overall in solid evidence across many facets of nutrition. However, there was still enough to look at a variety of aspects and possible associations with dry eye.
The most solid evidence exists for dietary components of omega-3 and omega-6 polyunsaturated fatty acids. Omega-6 does not generally benefit the ocular surface, while omega-3 does. Greater omega-6 consumption was mapped to a 2.5 times higher risk of dry eye, while a 30% reduction in risk was observed with each gram of omega-3 consumed each day. This may be due to omega-6 being more pro-inflammatory, while omega-3 exhibits greater anti-inflammatory properties. As such, the ideal ratio of consumption of omega-6 to omega-3 is less than 4:1. Despite this, Dr. Maria Markoulli, the primary author of this subcommittee report, and a member of UNSW Sydney’s School of Optometry and Vision Science, still points out that “what we don’t yet know is what the optimal dietary intake needs to be to prevent and manage dry eye disease.”
Micronutrients most important in maintaining ocular surface health include vitamins A2,3, B12, C and D. Selenium and lactoferrin may play a role in maintaining the ocular surface, as decreased levels of selenium in tears and decreased lactoferrin levels were linked with dry eye.
Although hydration offers plenty of benefits for many organs and organ systems, increasing intake does not seem to be indicative of a protective factor against dry eye or other ocular surface outcomes.
Endocrine-disrupting chemicals may be ingested, or consumed via leaching from food containers, and can end up changing gut microbiome diversity. Blood concentration of mercury is linked to dry eye symptoms, with main consumption happening through contaminated fish. Alcohol is weakly associated with dry eye, but with no increased risk of dry eye seen in heavy drinkers. Other factors increasing the risk of dry eye are anorexia nervosa, food intolerance and food allergy.
As far as specific diets are concerned, only the Mediterranean diet is directly linked to the ocular surface by decreasing dry eye symptoms and risk of Sjogren’s syndrome, likely due to anti-inflammatory properties from olive oil and nuts.
Dietary additive or supplementation of certain agents have been studied on their effects on the ocular surface. Caffeine may actually have a slight protective effect against dry eye, as might manuka honey, which decreased allergic symptoms with dietary birch pollen honey. Dr. Markoulli points to “oral ingestion of multiple Chinese herbs that have been reported effective against Graves ophthalmopathy and dry eye, and curcumin has been found to reduce oxidative stress, angiogenesis and inflammation.”
Vitamin A supplements reduce dry eye symptoms compared with no treatment or cyclosporine therapy. Omega-3, as well as being effective from ingestion in the diet, is also effective in the form of a supplement to decrease dry eye symptoms and signs. But, optimal dosage, composition and duration of supplementation treatment still needs to be determined.
The impact of nutrition extends beyond the food we eat to include effects relating to the gut microbiota. As Dr. Markoulli notes, “the gut microbiome plays an important role in the regulation of low-grade chronic inflammation and ecological shifts within the gut microbiome can induce imbalance or dysbiosis, which is associated with chronic disease.” One of these chronic diseases is dry eye, which has been associated with severe gut dysbiosis and reduced microbiome diversity. Luckily, pre- and probiotics may help with this issue to improve dry eye symptoms. This approach to dry eye may be something to look out for in the future, as Dr. Markoulli mentions “the field of modulating the gut microbiome as an intervention to treat dry eye disease is relatively in its infancy.”
Diseases related to nutrition can also impact the ocular surface. Dry eye is linked with obesity, pre-diabetes and type 2 diabetes. Ocular complications can result more often after bariatric surgery due to resulting malabsorption. For some reason, hypertension is inversely linked with dry eye prevalence.
Societal Challenges
This section comprises factors that are out of personal control and instead are what might be considered issues that need to be addressed by entire countries or cultures.
Perhaps the most obvious factor outside of our control is our biology. Age, sex and genetic factors can predispose certain populations to develop ocular surface diseases like dry eye, especially impacting prevalence and severity of the disease and subsequent access to and use of care.
Also outside of many people’s capabilities are fixing issues of malnutrition or food insecurity, as without proper nutrition, the eye (as well as the rest of the body) cannot function optimally. Issues with water, sanitation and housing are all factors associated with trachoma development and other waterborne diseases.
Dr. Fiona Stapleton, also a part of UNSW’s School of Optometry and Vision Science and this subcommittee’s head, specifies that “there’s also a very strong link between education and poverty, socioeconomic class and access to health services which will affect both the prevalence and severity of many ocular diseases.”
Remoteness, geography and seasonality can all impact the types of ocular surface diseases seen and the severity displayed. Along with this, the availability and affordability of services will vary by region. Ocular surface disease presence will be compounded with these factors with the cost of diagnostics and treatment, with options of national health services, insurance or out-of-pocket expense weighing on patients with how likely they will be able to afford treatment.
Occupation will affect the likelihood of patients developing ocular surface diseases. Jobs with radiation or harmful chemical exposure, as well as outdoor occupations, are all associated with ocular injuries. Prison populations experience poorer health outcomes from lack of services, nutrition limitations and lack of awareness of disease. Conjunctivitis, xerophthalmia and pterygia are all conditions overrepresented in this population.
As society has increasingly relied on digital technology, this has come to pervade the healthcare industry as well. Patients are increasingly seeking health information from the internet, which could affect their interactions with practitioners in positive or negative ways. However, computers can benefit providers by offering ways of checking compliance, administering questionnaires or in undertaking telehealth to provide access to care for those who may not be able to reach an office. As Dr. Stapleton elaborates, “the digital environment may also support practitioners in their continuing education, which may lead them to provide better levels of health services and provide other options for health including telehealth which may enhance access to healthcare for those in regional or remote communities.”
With COVID having disrupted lives since 2019, this subcommittee wanted to clarify how the pandemic has impacted ocular surface diseases. First, they looked at screen time use, implementation of online classes and digital device use during the pandemic. Eye symptoms were found to worsen with increased exposure to screen time and online learning as a consequence of the pandemic. As well, there was worsening or no change associated with signs and symptoms of dry eye directly, when exposed to the virus.
Strategies to mitigate virus spread, like facemasks, were also analyzed. Their use was found to worsen or induce no change on most signs and symptoms with exposure. However, one study did report improved allergic ocular symptoms with mask use, potentially from creating a barrier for allergens to have to pass.
Dr. Stapleton explains that since remote, hybrid and flexible work are likely to continue, it is reasonable to assume that frequency and severity of ocular surface diseases will continue along with this. As such, practitioners, she believes, “can be proactive with their patients to mitigate these effects.” She also puts into perspective how these larger, societal factors are at play with the ocular surface. “Focusing on social determinants and their interactions, rather than just the cause of the disease, encourages the development of more comprehensive, holistic solutions and a whole of society approach to reducing disease morbidity. It encourages practitioners to have a broader discussion with their patients about lifestyle and social determinants.”
Lifestyle Challenges
In the last of the reports, more personal issues are addressed, covering mental health, physical health and social health as it relates to lifestyle choices and challenges. Although these factors may not initially seem relevant to the ocular surface, there are some surprising associations.
There has been an increasing awareness of the importance of mental health, and now is an opportunity to increase our knowledge of how mental health disorders affect the rest of the body. This report covers mainly the conditions of depression, anxiety and generalized stress. Although this a great start in clarifying the brain’s relationship with modulating the physiology of the rest of the body, more work will need to be done on other conditions such as bipolar disorder or schizophrenia.
First discussed was depression. An alarming 29% of individuals with dry eye disease also had depression, as one meta-analysis concluded. A different one was able to determine that dry eye disease patients had a higher frequency of depression. Interestingly, dry eye symptom scores were associated with depression severity scores, but data are found to be much weaker when looking at dry eye signs. Of note, both depression and antidepressant medications may be linked to dry eye with a biologic basis.
Anxiety disorders saw a similar trend as with depression. Several studies reported a link between anxiety and a dry eye diagnosis. In US veterans, dry eye disease, post-traumatic stress disorder, antidepressant and anxiolytic use were all associated with dry eye. Similarly to depression, there is an association between dry eye symptoms with anxiety, but not signs. Coping measures are also related with symptoms but not signs.
The effects of stress on the eye are apparent, as worse self-perceived health status and more psychological stress were both linked with increased susceptibility of aqueous deficient and evaporative dry eye and its symptoms.
When sleep is interrupted, it can cause serious issues to the body. The ocular surface suffers with dry eye patients’ sleep, as they have poorer sleep quality, spend less time asleep and experience more sleep disturbances. Sleep-related factors like excessive sleepiness and insomnia are associated with dry eye symptoms, showing a clear connection between the need for proper sleep and maintenance and repair of the body. Primary Sjögren's syndrome similarly exhibits increased sleep disturbances, more night awakenings and obstructive sleep apnea presence. However, being able to get adequate rest may revert some observed ocular surface changes, as has been described in animal models.
Obesity may put patients at risk of worsening dry eye, as it has been connected to evaporative dry eye, tear film instability and meibomian gland abnormalities in function and architecture. Unfortunately, treatment for often-comorbid obstructive sleep apnea in patients with obesity has also been linked to dry eye disease, and been shown to cause greater ocular irritation upon initiation.
While covered in the previous report as well, this report specified that mask wearing may be a new and emerging risk factor for exacerbation of dry eye symptoms. This was linked directly to how much time was spent wearing the mask, with wear of six or more hours per day, five days a week showing greater dry eye symptoms. The greater the number of months a mask was worn, the more dry eye symptoms were reported. Masks are specifically linked to evaporative dry eye and meibomian gland disease, as well as increasing the risk of chalazion.
This subcommittee undertook a systematic review of chronic pain conditions and whether they are contributive risk factors to dry eye disease. They reviewed many conditions, but found that some were indeed found with an increased risk of dry eye. These included migraine with a 1.61 increased risk, fibromyalgia with a 1.91 increased risk, irritable bowel syndrome with a 2.16 increased risk and back pain with a 1.60 increased risk. All these observations suggest a comorbidity between chronic pain conditions and dry eye, but mostly with symptoms.
Drugs can affect the ocular surface differently, depending on the type. Kelly Nichols, OD, PhD, dean of University of Alabama Birmingham’s School of Optometry and one of the authors of this report, points to the adverse effects of smoking on ocular surface health.
“Surprisingly, there’s not a lot of good data to support that, even though everyone would suggest that probably you shouldn’t smoke because it could impact your eyes. It doesn’t mean the association isn’t there, just that the literature gives us less guidance than we may want.” She advises ODs to look a little more carefully at the tear film, and tear film stability in particular, in a patient who’s a smoker. “It could potentially have more impact on the ocular surface, whereas symptoms in that individual may not play as significant a role, or at least they’re not telling you that.”
Cannabis use long-term may decrease corneal endothelial density. Alcohol intake is a contributory factor to dry eye, but may be part of a wider issue of poor nutrition. Caffeine, however, actually shows evidence of increasing tear meniscus height and Schirmer test values two hours after intake, suggesting it may encourage better tear production.
Dr. Nichols offers some key takeaways to carry into your practice from the findings of this section. “Many patients are either taking anti-anxiety or antidepressant medications. These therapies, and the underlying conditions, also overlap with sleep disorders, and all of these have potential consequences for the ocular surface. So, asking them about their sleep and the comfort of their eyes might be a really important thing to do. Creating conversations around some of these less obvious connections to dry eye might be a positive outcome of the report.”
Takeaways
One of the recurring themes throughout all sections of this massive report is that doctors may need to change some of the recommendations they’re giving to patients. “We have to be very careful that we’re giving patients the most accurate advice, that we actually have the evidence behind it to support our actions, and we don’t have patients investing money in things that might not work,” Dr. Craig cautions.
This might be most evident when reviewing the subcommittees’ findings on blue-light blocking lenses, hydration or caffeine and their effects on the ocular surface.
“It’s a really important area to find out more information—we need better quality studies,” Dr. Craig notes. “We don’t have enough evidence yet. We need to interpret the existing study outcomes carefully, and use that information to help drive future research until we do have enough evidence to decide whether such things cause a problem.”
Dr. Craig is excited for change and, upon the release of the full reports, thinks that education on these topics will be reciprocally exchanged by clinicians and their patients, citing that patients now more than ever are engaging themselves in becoming informed about their health.
She hopes that these sort of integral conversations between patients and doctors will “help drive better standards in industry for products like cosmetics. If there’s resistance from the professions and from the public, then it may encourage change in some of the components within cosmetics if they’re no longer accepted. If it becomes recognized that they cause problems, I think we need to see changes happening there.”
Cosmetics is one of the most apparent industries in which regulations and manufacturing processes may need to change to reflect what is currently known about their effects on health, but this is not the only area that needs change.
Through the combined efforts of all the subcommittee reports, we now know more than ever about a wide range of factors that contribute to ocular surface health. Heed the advice and tips given by the researchers of this report, continue to adapt your recommendations as the literature evolves, and you’ll be in the best position to help your patients.

