 |
A 45-year-old Hispanic male presented to clinic with a chief complaint of progressive blurry vision that started approximately four days earlier in his right eye. Accompanying symptoms included light sensitivity and ocular irritation. The patient denied any ocular discharge, ocular trauma or recent illness.
The patient’s ocular history was remarkable for penetrating keratoplasty (PK), which was performed 25 to 30 years ago in both eyes. At this visit, the patient denied using a topical steroid for maintenance therapy. His best-corrected visual acuity (BCVA) was 20/70 OD, 20/50 OS. His anterior segment findings are provided (Figure 1). We observed no palpable preauricular node (PAN) at that visit. The rest of the exam was unremarkable.
Given the patient’s presentation of unilateral subepithelial infiltrates (SEIs) and temporal graft edema, with a chief complaint of acute progressive blurry vision, we considered diagnoses of corneal graft rejection, herpes simplex keratitis (HSK), epidemic keratoconjunctivitis (EKC) and corneal graft failure (CGF).
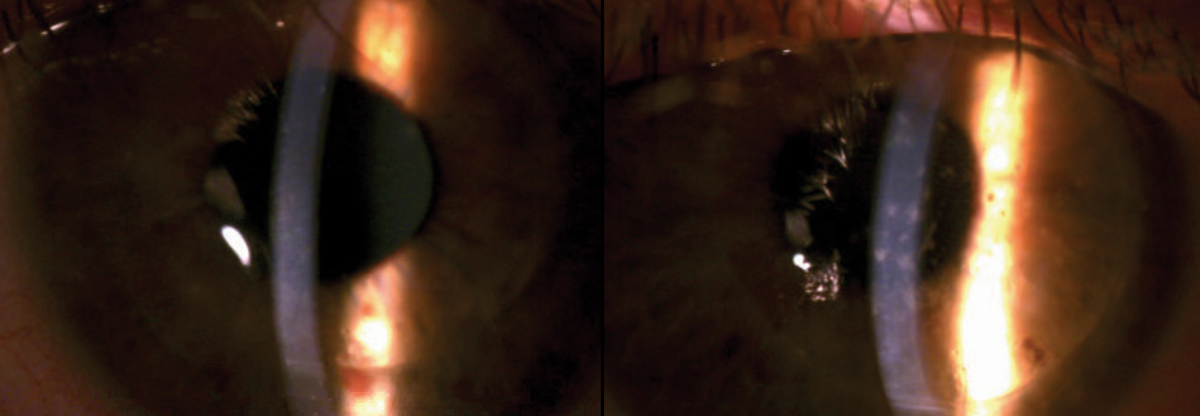 |
| Fig. 1. Upon presentation, scattered SEIs were noted throughout the right corneal graft along with temporal graft edema (left). The left corneal graft was remarkable for scattered SPK; no SEIs or graft edema were noted (right). Click image to enlarge. |
Differential Diagnosis
The patient denied any previous history of herpes simplex treatment or previous episodes of HSK. The exam showed stromal edema. It was non-centralized and did not appear disc-formed. In addition, an anterior chamber reaction was absent.
In a patient with a corneal graft rejection, the presence of scattered SEIs can mimic EKC. In addition, the absence of EKC characteristics, such as conjunctival follicles, pseudomembranes or PANs, were noted. Though SEIs were present, they were limited strictly to the graft cornea. Unlike this case, EKC does not present with corneal edema. Though treatment for EKC and epithelial/stromal corneal graft rejection would be similar (moderate to aggressive use of topical steroids), corneal graft rejection seemed likely due to the presence of graft edema and SEIs that were limited to the graft cornea in the absence of any pseudomembranes or PANs.
CGF is the result of any loss of graft structural integrity, which leads to irreparable vision loss. Classically, graft failure presents as gradual onset of graft edema in the absence of inflammation or keratic precipitates.1 In this case, though graft edema was evident, inflammation was noted in the form of SEIs. Because the patient’s findings were attributed to active inflammation and because the integrity of the corneal graft did look adequate, we attributed the findings to corneal graft rejection, not graft failure. Since graft rejection could lead to failure, timely action was required.
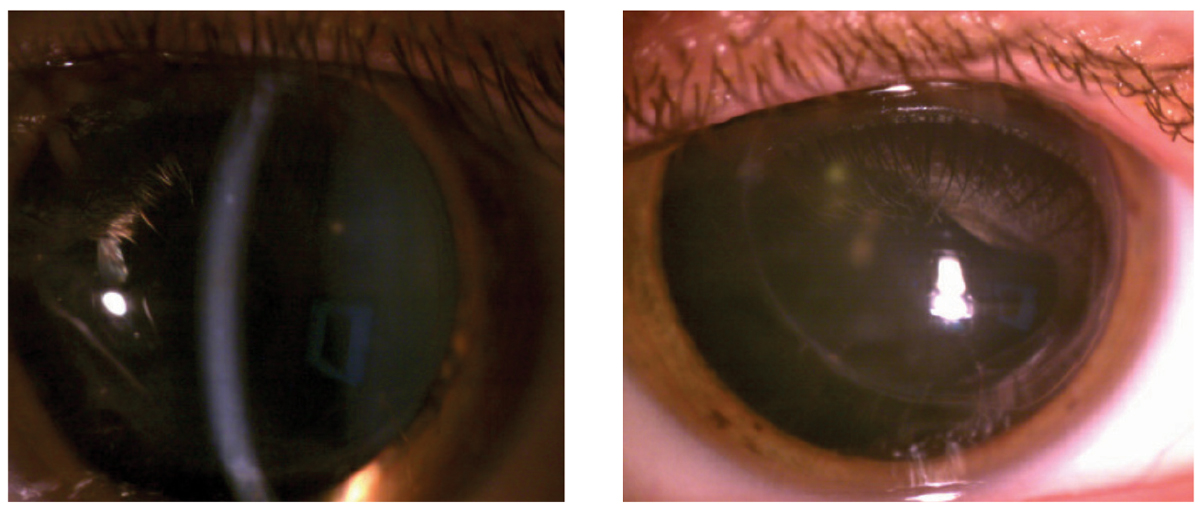 |
| Fig. 2. At left, after aggressive steroid use and several visits with ophthalmology, this right corneal graft was finally clear. Though the left graft did not undergo rejection throughout this case, a photo of the left eye was provided for contrast. Click image to enlarge. |
Assessment and Plan
Based on the clinical presentation, we suspected either a combined form of graft rejection; specifically, chronic stromal rejection with possible endothelial graft rejection or endothelial graft rejection.
Scattered SEIs limited to the corneal graft are typical of chronic stromal rejection, but corneal edema is not characteristic of this form of rejection. The presence of corneal edema in an eye with a previously clear and quite graft should raise suspicions of endothelial graft rejection regardless of the presence of an endothelial rejection line.
When handling combined forms of rejection (or endothelial graft rejection), administer a systemic steroid. Given that the PK in this eye was 30 years old and, most likely would require systemic steroids, we consulted with a cornea specialist and scheduled the patient for a next day consultation.
Presentation
Corneal graft rejection is an immune mediated process wherein a graft that has been clear for at least two weeks suddenly succumbs to graft edema in addition to anterior segment inflammatory signs.2 Early symptoms include blurry vision, mild discomfort, redness, photophobia and ocular irritation; late-stage symptoms include markedly deceased vision, irritation, ocular pain and tearing.
Corneal graft rejection can present with a combination of signs and is classified into four subcategories: epithelial graft rejection, chronic stromal rejection, hyperacute stromal rejection and endothelial graft rejection (See Corneal Graft Rejection Categories).2
Corneal Graft Rejection Categories1. Epithelial graft rejection – In these cases, patients are typically asymptomatic with mild inflammation. Clinically, it presents as an elevated, undulating line that stains with sodium fluorescein or rose bengal. This linear pattern presents in the graft periphery (near the graft-host junction) and progresses toward the center of the graft epithelium. The epithelium behind the rejection line will presents a hazy and irregular.2,3 The average onset of an epithelial rejection line is three months.2 One manifestation which bears little clinical significance is the presence of Kaye’s dots: punctate epithelial opacities located anterior to the suture line of the corneal graft. Although this form of rejection is self-limiting, prompt treatment is required due to its approximately 74% association with other forms of rejection.2 2. Chronic stromal rejection – This form of rejection presents with scattered SEIs, which are limited to the donor graft tissue. The presence of scattered SEIs can mimic EKC in a patient who presents with an episode of graft rejection. One way to differentiate the two would be based on the amount of conjunctival injection noted and the presence (or absence) of a PAN. Chronic stromal rejection will present with mild injection without a PAN. Although this form of rejection would unlikely lead to graft failure, the presence of SEI indicates that the host tissue is sensitized to the donor tissue and endothelial rejection may be impending.2 3. Hyperacute stromal rejection – This is typically seen in conjunction with or immediately following endothelial rejection. Early signs include ciliary congestion and engorgement of the corneal vessels. It presents as sudden onset of peripheral full-thickness haze in a previously clear corneal graft that spreads to the corneal center of the graft within 24 to 48 hours.2 4. Endothelial graft rejection – In terms of severity, endothelial graft rejection is the most symptomatic and ruinous type of rejection. Endothelial rejection is more commonly seen in younger patients and is directly correlated to the degree of corneal vascularization prior to transplantation. These patients will present with pain, redness and decreased vision. Findings will include Khodadoust line (a chain-like configuration limited to the donor endothelium which consist of white blood cells), stromal edema, keratic precipitates limited to the donor tissue and an anterior chamber reaction. In addition, endothelial graft rejection is classified into the three following categories: possible, probable and definite.2 Such a form of rejection requires immediate emergency treatment.2-4 The rate of reversal for severe endothelial rejection in a patient who underwent PKP is as high as 63% when proper timely treatment is initiated.5 |
Therapeutics
Treatment must be individualized. In cases of isolated epithelial or chronic stromal rejection, both of which have a higher rate of reversibility, topical prednisolone acetate 1% can be dosed up to six times per day with a tapering schedule that extends six to eight weeks.6
A more aggressive approach must be taken when handling endothelial, acute stromal or combined forms of corneal graft rejection. In these cases, use topical corticosteroids in conjunction with systemic therapy—prednisone acetate 1% Q1hr (or difluprednate 0.05% Q2hrs) in combination with either, with 40mg to 80mg of oral prednisone daily or a single (or three) IV dose of methylprednisolone 500mg.6 This may be given in conjunction with subconjunctival betamethasone 3mg in 0.5ml. Topical antibiotics and cyloplegics should be prescribed for prophylactic coverage and if there is an iritis present, respectfully.7
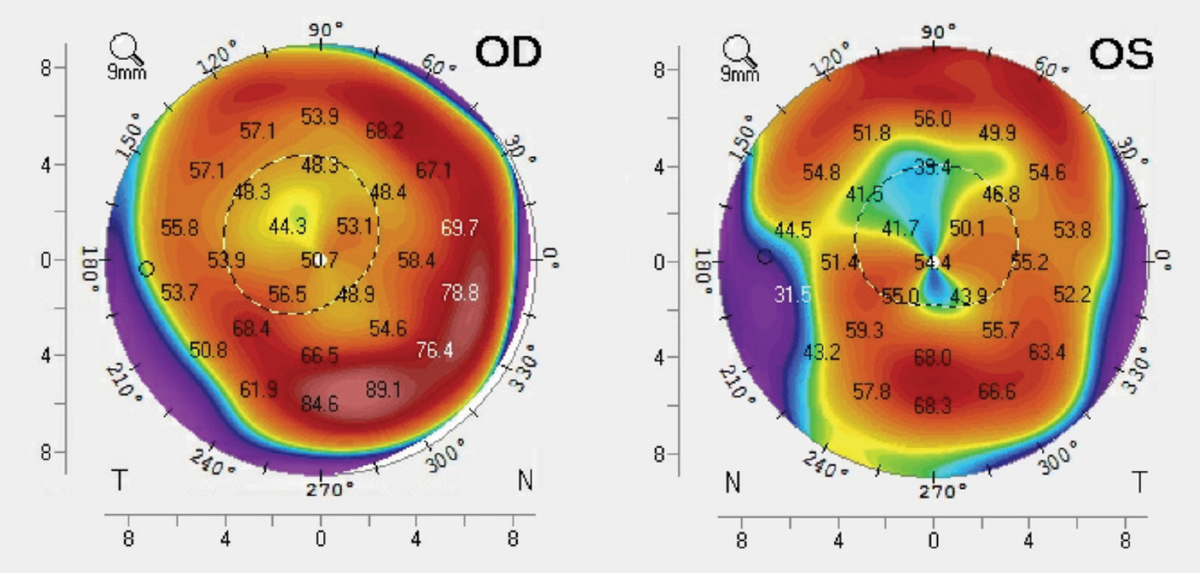 |
| Fig. 3. These tangential curvature maps show our patient’s corneal topography. Click image to enlarge. |
Regardless of the type of corneal transplant surgery a patient undergoes, the patient should be placed on a daily topical steroid (such as loteprednol or fluorometholone) for life to decrease the risk of rejection; patients demonstrating a steroid response should be treated accordingly with IOP-lowering medications.
In addition, our care expands beyond the scope of managing active cases of graft rejection: we are tasked with helping to mitigate the risk factors that can lead to episodes of rejection. For example, consider placing patient on a prophylactic antiviral (such as acyclovir) if the patient has previously reported an incidence of HSK and is currently not on oral antivirals. Lid disease compounded by ocular surface disease (such as severe dry eye) can incite epithelial damage and could trigger inflammation. Other conditions that should be treated accordingly include, but are not limited to; exposed/loose sutures, poorly fitting post-surgical contact lenses, trichiasis and entropion. Managing such comorbidities will prevent possible episodes of corneal graft rejection.
Endothelial Rejection SeverityPossible: Graft edema only. Probable: Edema, cells/flare, keratic precipitates on donor button. Definite: Edema, cells/flare, keratic precipitates on donor button, Khodadoust line. |
Our patient was diagnosed with early epithelial/stromal rejection and placed in the following treatment regimen: Durezol (difluprednate 0.05%, Novartis) Q1hr OD, Besivance (besifloxacin, Bausch + Lomb) TID OD, and one Medrol (methylprednisolone, Pfizer) pack PO as direct and scheduled for a next-day follow up. After three more visits with the cornea specialist, the graft rejection had resolved (Figure 2).
When a patient presents with graft rejection, proper classification and prompt initiation of treatment is crucial. In most cases, failure to reverse rejection results from delayed treatment. This can lead to significant donor endothelial cell loss, which can in turn lead to permanent graft damage and loss of recoverable vision.8 Patients who undergo corneal transplantation, regardless of procedure type, require daily maintenance with immunosuppressive therapy to prevent graft rejection, hence the importance of routine exams to evaluate patient compliance with medications. Patients should be evaluated and treated for any comorbidities to decrease risk of an episode of rejection.
| 1. Price M, Thompson R, Price F. Risk factors for various causes of failure in initial corneal grafts. Arch Ophthalmol. 2003;121(8):1087-92. 2. Panda A, Vanathi M, Kumar A, Priya S. Corneal graft rejection. Surv Ophthalmol. 2007;52(4):375-95. 3. Alldredge O, Krachmer J. Clinical types of corneal transplant rejection: their manifestations, frequency, preoperative correlates and treatment. Arch Ophthalmol. 1981;99(4):599-604. 4. Tham V, Abbott R. Corneal graft rejection: recent updates. Int Ophthalmol Clin. 2002;42(1):105-13. 5. Khodadoust AA. The allograft rejection: The leading cause of late graft failure of clinical corneal grafts, in Porter R, Knight J, eds. Corneal Graft Failure. Ciba Foundation Symposium 15. Amsterdam, Elsevier, 1973:151-64. 6. Qazi Y, Hamrah P. Corneal allograft rejection: immunopathogenesis to therapeutics. J Clin Cell Immunol. 2013;2013(Suppl 9):006. 7. Gerstenblith AT, Rabinowitz MP. The Wills Eye Manual, Office and Emergency Room Diagnosis and Treatment of Eye Disease. Lippincott Williams & Wilkins; 2012. 8. Mahabadi N, Czyz C, Tariq M, Havens S. Corneal graft rejection. StatPearls Publishing. www.ncbi.nlm.nih.gov/books/NBK519043. October 26, 2019. Accessed December 1, 2019. |

