 A patient of mine presented with a dense, unsightly leucoma. My local corneal specialist recently recommended a corneal tattooing procedure. How does one perform such a procedure in this scenario, and what are some potential complications to prepare for?
A patient of mine presented with a dense, unsightly leucoma. My local corneal specialist recently recommended a corneal tattooing procedure. How does one perform such a procedure in this scenario, and what are some potential complications to prepare for?
Using pigment to mask unsightly corneal scars is not a novel concept. In fact, it was first introduced by Galen, a Greek physician, in 160 AD; however, the technique was used infrequently for centuries thereafter.1 The process was not readily adopted until the early 20th century, when Frederick H. Verhoeff reported the safe and effective use of India ink to darken corneal scars.2
The most frequent indication for corneal tattooing over the years has been cosmetic—patients who present with a corneal leucoma or scar may have these aesthetically unpleasing conditions masked by the procedure.
According to James Aquavella, MD, professor of ophthalmology at the University of Rochester Flaum Eye Institute, who has performed variations of corneal tattooing over the past 50 years, it has also “occasionally been beneficial in creating a pupillary effect in aniridia, surgical or traumatic iridectomies, or post-traumatic mydriasis.” This can reduce glare, diplopia and photophobia, he says, resulting in improved visual acuity.
| |
|
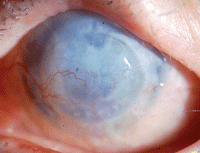
Corneal tattooing can mask unsightly corneal leucoma and, in some cases, improve visual acuity. Photo: Barry Lee, MD, FACS
|
While the availability of cosmetic soft contact lenses has reduced the use of corneal tattooing in recent decades, there are still a number of cases in which insertion and removal of these lenses can be problematic. Additionally, some patients are intolerant to contact lenses, making them ideal candidates for corneal tattooing.
Early corneal tattooing procedures involved using a hypodermic needle, a sharp, pointed instrument or a suture needle held on a forceps.3 Procedures such as these were performed under topical anesthesia through the existing epithelium.
To create the masking effect, a metallic dye is applied to each lesion. Typically, titanium dioxide pigments were used; Dr. Aquavella says he often used Chinese or India ink (the same inks discussed in the literature by Verhoeff) in addition to gold pigments. Corneal tattooing procedures that use needles often require “hundreds of superficial microstromal punctures,” says Dr. Aquavella.
Another technique involves the creation of an interlamellar pocket with a keratome.4 This is then followed by the introduction of filter paper that has been soaked in platinum chloride salts. “Subsequently, a syringe needle is introduced beneath the filter paper and a small amount of hydrazine hydrate is injected, which then causes precipitation of the dye,” says Dr. Aquavella.
A more recent technique involves the use of a femtosecond laser to create pockets and channels, which are then followed by the introduction of a number of colored dermatological patterns.5
While corneal tattooing is relatively safe, some complications may occur, such as allergic reaction to the dyes used, secondary infection, delayed epithelialization, recurrent erosion, perforation and intrastromal hemorrhage if vessels are damaged. However, Dr. Aquavella says complications are “extremely rare in the hands of an experienced corneal surgeon.”
1. Dougan C, Hill G, Villaverde N, Hill J. Seeing better through someone else’s eyes. Brown University. Available at: http://biomed.brown.edu/Courses/BI108/2006-108websites/group11corneal%20implants/. Accessed June 29th, 2014.
2. Verhoeff FH. India ink infiltration: a simple and effective substitute for corneal tattooing. Journal of the American Medical Association. 1917 Oct 24;LXIX(17):1420-21.
3. Pitz S, Jahn R, Frisch L, Duis A, Pfeiffer N. Corneal tattooing: an alternative treatment for disfiguring corneal scars. Br J Ophthalmol. 2002;86:397-99.
4. Khan AO, Meyer D. Corneal tattooing for the treatment of debilitating glare in a child with traumatic iris loss. Am J Ophthalmol. 2005 May; 139(5):920-21.
5. Kim JH, Lee D, Hahn TW, Choi SK. New surgical strategy for corneal tattooing using a femtosecond laser. Cornea. 2009 Jan; 28(1):80-4.

