|
|
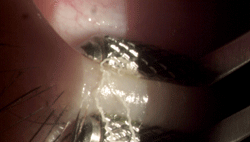
Meibomian fluid produced by using the Maskin meibom
ian gland expressor.
|
Not long ago, we had very few effective treatments for dry eye disease—and so, our time and effort in the office often provided little relief for patients and minimal revenue for our practices. In the past several years, new research has given us a much better understanding of this chronic condition, leading to a number of exciting clinical advances in dry eye evaluation and treatment.
The result is an expanded tool
box to help us more accurately diagnose and successfully treat dry eye. And that means better quality of life for our patients and improved reimbursement for our practices. Of course, we must always operate on the tenet that patient care is the number one priority—we are doctors first, and the business comes second.
With that in mind, we should run our practices efficiently and look at the most cost-effective way to deliver the highest level of care. In this article, we’ll look at how you can provide an approach to dry eye evaluation and treatment that yields both clinical and financial gains.
Take a Good Look
A business-savvy approach to dry eye must begin with a clinically sound understanding of this complex, multifaceted disease process. Let’s start by referring to the definition of dry eye that came from the 2007 International Dry Eye WorkShop:
“Dry eye is a multifactorial disease of the tears and ocular surface that results in symptoms of discomfort, visual disturbance, and tear film instability with potential damage to the ocular surface. It is accompanied by increased osmolarity of the tear film and inflammation of the ocular surface.” 1
In light of this definition, we need to get our staff and our patients to view ocular surface disease (OSD) as a chronic, multifactorial disease—not a secondary issue that’s lumped into a routine eye exam.
|
|
|
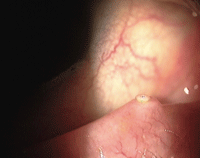
Surface occlusion punctal plug.
|
|
Many optometric offices suffer because of a failure to differentiate between medical and refractive exams. Both are comprehensive and are part of your daily routine, but should not be considered part of the same examination.
Some doctors make the mistake of prescribing a dry eye treatment as part of the comprehensive exam—but handing the patient a sample or writing a prescription without an evaluation and follow-up is just not good care. A patient with any type of OSD deserves a medical workup.
In our practice, if we uncover a medical issue like dry eye during a routine eye exam, we reschedule the patient for a medical OSD evaluation, which is billed to the medical insurance plan. This approach ensures that you get fairly compensated for your time, and that the patient gets a thorough and complete dry eye evaluation, which is necessary if you’re going to make any difference in this disease process.
The OSD evaluation allows you to get a complete history of contributing factors and medical conditions, and to examine the ocular surfaces and adnexa. Some clinicians use tear osmolarity testing as part of their evaluation. Instruments such as the LipiView Ocular Surface Interferometer (TearScience) aid in a clinical evaluation of the tear film, providing a measure of lipid layer thickness. You may also wish to perform Schirmer’s testing, corneal staining and tear film break-up time (which are considered part of the overall evaluation, not as separately billable procedures).
Develop a Long-term Relationship
Once you’ve determined that the patient has dry eye, take the time to educate them about the nature of the condition and prepare them for what’s ahead. Patients often do not understand that dry eye is a chronic and progressive disease.
Many of our patients have a “single-visit” mentality, so one of the most important steps in effective dry eye practice is to educate the patient that dry eye is not a condition that can be solved in one session. Nor will it necessarily be solved with one approach. Instill in your patients a mindset that treating dry eye is a process that you will work through together over a number of visits, trying various options to find a combination that works.
|
Does Dry Eye Treatment Pay Off?
| |
|
While many
practices don’t think of dry eye treatment as a revenue generator, it
actually has the potential to produce more revenue than some other
expected profit centers in the eye care office.
Let’s take at the total fees generated to see how it stacks up.6 | |
|
Contact lenses
Eyeglass patient Eye exam Dry eye |
$150-$200
$125-$200 $60-$225 (depending on payer) $300-$800 (can be upwards of $1,300-$1,600) |
| *All figures reflect profit per year. | |
Choose the appropriate E/M code that corresponds with the visit—many providers use 99213 or 99214 for mild to moderate dry eye evaluation.
Let’s take a look at the numbers in my state (Alabama) to get an idea of how these medical office visits add up.
Medical Office Visit: OSD Evaluation
99212 $48.00
99213 $64.93
99214 $98.65
Medical Office Visit: Follow-up
99212 $48.00
99213 $64.93
If you anticipate three follow-up visits during the year, here’s what the revenue would look like:
Follow-up Revenue per Year
99212(x3) $144.00
99213(x3) $194.79
It’s easy to see that follow-up is not only key for clinical success, but can also produce significant revenue for your practice.
Embrace a Combination Approach
For few patients, artificial tears may be enough to relieve their dry eye symptoms, but most require a treatment strategy that involves several different therapies to see real improvement. Our job is to make sure we’re providing our patients with the treatment options they need. In a Gallup poll of dry eye sufferers, results indicated that:2
- 72% of patients had physicians recommend artificial tears for their dry eye problem (n=541).
- 82% of patients somewhat agreed or strongly agreed that they wish there was something more effective to treat their dry eye (n=751).
- 97% of patients reported that their dry eye condition is frustrating (n=751).
These results suggest that the majority of patients want more from us. Again, this gives us an opportunity to not only improve patient care and satisfaction, but also to enhance our revenue stream. Advances in the last decade have given us a number of effective procedures to add to a comprehensive dry eye treatment strategy—many of which are reimbursable (
see “Reimbursable Dry Eye Evaluation and Treatment”). Let’s take a look at some of the most common approaches:
• Meibomian gland expression. As it’s now been established that meibomian gland dysfunction is probably the single most common cause of dry eye, we know that meibomian gland expression is one of the most valuable treatment options we have.3 The first step in MGD treatment is to perform an in-office expression procedure. In addition to hot compresses, a number of instruments are available to aid in therapeutic lid expression—several of which we use in our office.
 |
|
| Clogged and atrophied meibomian glands. |
|
When you’re using a procedure that does not have a medical procedure code, remember to have the patient sign an Advance Beneficiary Notice of Noncoverage (ABN) so that the patient agrees to be financially responsible for the treatment if it’s not covered. (You can download the forms for free at www.corcoranccg.com.)
One of the procedures we have instituted involves the use of a Maskin expressor (Rhein Medical). We choose to do three in-office expressions over a six-week period, and we have developed a global fee for the procedure. We also use the Maskin meibomian gland intraductal probe (Rhein Medical) to open up each of the meibomian glands in both upper and lower lids. This procedure is also based on private pay fees, as there is no medical code.
The LipiFlow Thermal Pulsation System (TearScience) is also becoming more popular in meibomian gland expression. The device applies heat to the palpebral surfaces of the upper and lower eyelids directly over the meibomian glands to aid in expression. In the absence of prior authorization, it’s best to use an ABN form to ensure payment for this procedure as well.
• Punctal plugs. Once the ocular condition has been treated for a minimum of six to 12 weeks and you feel that the tear film is free of debris and byproducts, you may decide to add a punctal plug to the treatment regimen. (When plugs are inserted too soon, they may actually increase the cytokines, recruiting more T-cells and inflammatory debris contributing more to the dry eye and allergic response.)
Punctal plugs diminish tear drainage from the ocular surface and enhance contact time between tears and ocular surface. There are multiple modalities, manufacturers and products, such as collagen, silicone and acrylic polymers as well as intracanalicular and surface punctal occlusion. I prefer surface punctal occlusion for ease of removal.
|
|
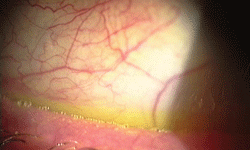
Frothing, as seen here, is an early sign of meibomian gland dysfunction.
|
• Scleral contact lenses. For those patients who have failed with other modalities for dry eye treatment, scleral contact lenses can be an excellent addition. When fit properly, they create a bathing effect on the cornea and alleviate most chronic dry eye signs and symptoms. This is an extremely lucrative profit center when time and expertise are considered in establishing a proper fee structure. Make sure you employ a comprehensive contact lens evaluation and follow-up program.
• Nutritional therapy. Another new profit center is adding nutritional therapy to your product inventory. Omega-3s suppress meibomitis, decrease apoptosis, improve neural signal transduction, stimulate tear production and augment the oil layer.4 Population studies show omega-3s prevent dry eye.5
• Sunglasses and spectacles. The use of sunglasses and spectacles can be a valuable supplemental treatment for the dry eye patient. When prescribing sunglasses, it is important to create a mini moisture chamber by using a wrap design or specialty inserts.
In addition to the revenue you generate through dry eye testing, follow-up visits and treatment, the patient’s satisfaction may earn you more referrals. Financial rewards come when you change the lives of your patients. When we put the patient first, the rest falls into place.
Dr. Schaeffer is the president and CEO of Schaeffer Eye Center in Birmingham, Ala., a 13-location practice that offers laser vision correction, comprehensive contact lens services, high fashion eyewear and sunglasses.
1. The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007 Apr;5(2):75-92.
2. The Gallup Organization, Inc. The 2008 Gallup Study of Dry Eye Sufferers. Princeton, NJ: Multi-Sponsor Surveys, Inc; 2008.
3. Nichols KK, Foulks GN, Bron AJ, et al. The international workshop on meibomian gland dysfunction: executive summary. Invest Ophthalmol Vis Sci. 2011 Mar 30;52(4):1922-9.
4. Dry Eye Science For Practitioners. How an omega-3 supplement treats dry eye. December 9, 2010.
5. Miljanovic B, Trivedi KA, Dana MR. Relation between dietary n-3 and n-6 fatty acids and clinically diagnosed dry eye syndrome in women. Am J Clin Nutr. 2005 Oct;82(4):887-93.
6. Wright M. Know the five biggest profit drains in your practice. MBA Essentials for Practice Management & Business Growth. February 28, 2013.

