Q: I have a 47-year-old white female patient with previously diagnosed dry eye and chronic ocular irritation. She reports constant mucus discharge throughout the day. Artificial tears have not helped. What’s the next step?

A: Ask the patient about the discharge—specifically, is she pulling long strands of mucus out of her eye? If so, this patient may have mucus fishing syndrome.
It’s a vicious cycle that can last months, even years, until the patient is treated. “Often patients don’t spontaneously volunteer this,” Dr. Slagle says. “I don’t know if it’s out of embarrassment or what, but they almost never come in saying that they’re pulling these strands of mucus out of their eyes.”
If you don’t ask, they won’t tell. They can end up at the anterior segment specialist when they could have been helped much earlier by their primary eye care practitioner.
Two elements are needed to diagnose mucus fishing syndrome, Dr. Slagle says:
• A history of recurrent production of mucus and its removal from the ocular surface.
• An objective correlation between the area of digital extraction and a staining pattern using rose bengal.
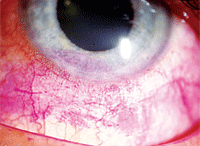
Staining on the ocular surface matches where the patient pulls away mucus.
When taking the history, “patients may say there’s some discharge, irritation or blur from the mucus. But you have to kind of prompt them to elaborate,” Dr. Slagle says. “Patients describe these impressive mucous strands that may be inches in length that they’re pulling off the ocular surface.”
Also, patients may not realize that they are actually touching the ocular surface when they remove the mucus. “So it’s important to have them demonstrate how they remove it,” he says.
Once you’ve done that, stain the ocular surface with rose bengal to see if the staining pattern matches the area where the patient demonstrated removal.
If you diagnose mucus fishing syndrome, “then it’s mandatory to treat the underlying irritant appropriately,” Dr. Slagle says. “Once this initial irritant is addressed, then the patient should be educated and strongly encouraged to not touch the ocular surface. It’s better to rinse the ocular surface with saline or an ocular lubricant than to pull the mucus out with the fingers.”
If the patient doesn’t respond to conservative treatment, then Dr. Slagle opts for off-label use of N-acetylcysteine solution, a mucolytic agent used for respiratory conditions. For mucus fishing syndrome, the solution is diluted to 10% and transferred into an ophthalmic dropper. Start at q.i.d. and taper it over a month until it’s used only when the patient notices the mucus.
Also, “I think there is a humoral immunity that factors into the pathogenesis of the syndrome,” Dr. Slagle says. “So I add a histamine blocker/mast cell stabilizer along with the N-acetylcysteine solution.”
Regarding comanagement, he says, “unless there’s an initial irritant such as a large pterygium that requires a surgical consult, mucus fishing syndrome can—and should—be managed very appropriately by the optometrist.”
1. Slagle WS, Slagle AM, Brough GH. Mucus fishing syndrome: case report and new treatment option. Optometry. 2001 Oct;72(10):634-40.

