As doctors, we would like to think that our patients genuinely listen to us and follow all of our instructions. Often, it’s nothing more than a matter of keeping them safe, comfortable and healthy. In a perfect world, we wouldn’t see an emergency case of red eye on a Sunday morning in a patient who failed to heed our recommendations about not sleeping in daily disposable contact lenses. Nor would we receive the phone call from a patient who is begging us to give him another set of trial contacts for those two-week lenses that were prescribed more than two years ago!
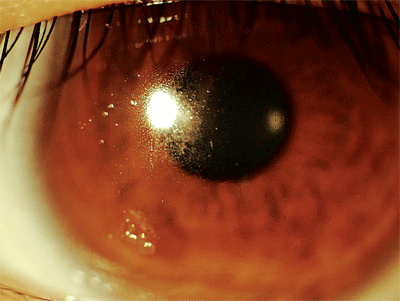
Contact lens wearers who exhibit poor compliance habits are highly prone to the development of corneal ulceration, as seen in this patient.
For patients, contact lenses truly are a modern enhancement to their daily visual experience. Contact lens technology has become so advanced that it’s easy for patients to assume most of their care habits will keep them visually successful––even if those habits carry over from old-school technology.
So, how can we prevent these avoidable mishaps? Further, can we actually predict who is more likely to be non-compliant?
Contact lenses are medical devices, and patients need to be reminded of that consistently to promote better compliance. Many patients with poor care habits are fortunate to never deal with ocular morbidities. This is due, in large part, to rigorous testing standards established by the FDA for both contact lenses and contact lens solutions.1-3 However, to ensure the lowest risk, there are still several key compliance steps patients should follow. The struggle lies in making your instructions to patients complete, easy and concise, so they will not be forgotten or mistaken.
The Battle is Ongoing
The fight to gain patient compliance with contact lens care is not a new one. The first peer-reviewed article addressing this issue was published more than 25 years ago.4 A 2009 poll question posted on
www.siliconehydrogels.org asked eye care practitioners to consider in which area of contact lens care and maintenance their patients were least compliant.5 Of 78 participants, the most frequent responses were “failure to replace lenses when scheduled” (55%), followed by “failure to wash hands prior to handling lenses” (18%), “switching care products” (13%) and “inappropriate use of care products” (9%).
Does personal perspective from practitioners in the trenches ring true? What are patients really doing, and can we evaluate their behavior in these recent years of advanced contact lens technology? The booming use of silicone hydrogel (SiHy) and daily disposable (DD) lenses certainly adds a new spin on patient care habits.
Eye care practitioners need to make a conscientious effort to individually address each patient on a case-by-case basis, due to the variety of new lens materials and care products, instead of just making blanket recommendations for wear and replacement.
A recent study conducted at the University of Waterloo’s Centre for Contact Lens Research sought to investigate these very issues.7 The authors assessed current recommendations for replacement frequency of SiHy and DD lenses, determined compliance (or noncompliance) with manufacturer-recommended replacement frequency, evaluated contact lens care and investigated reasons for noncompliance.6,7
Compliance with recommended replacement frequency varied with modality of lens type. When subjects were asked which replacement frequency had been recommended by their eye care practitioner, the greatest rate of non-compliance was reported for two-week SiHy lenses (22%), followed by DD lenses (10%) and one-month SiHy lenses (2%). Just 4% of patients reported that their practitioner gave no replacement frequency recommendation.8
Additional Steps To Improve Compliance
• Put a basket of contact lens cases on your front desk and encourage
patients to take them for FREE, because you care about their lens
safety.
• Place a message in each dispensed bag of contact lenses that indicates
that you will guarantee satisfaction with their lenses if the wearer
promises to follow your instructions. Then, have your staff simply fill
in those instructions that are particular to that lens and patient.
• Highlight selected portions of articles or studies that show why one
solution may be more effective and safer than another, and place these
in your reception area and contact lens rooms.
• Offer incentives for patients to switch from old modalities into newer
lens types. Ultimately, this will promote patient comfort as well as
help reduce patients’ chances of experiencing adverse events.
And, if patients experience adverse events, they need to know that they
can come to you for help. So, take the time to educate them about the
steps to take in the event of an occurrence, and reiterate that these
occurrences are unlikely if they follow your care and compliance
instructions.
• Any lens prescription needs to include instructions about care and replacement––both verbal and written.
Remember, confusion may occur if doctors’ recommendations are not in accordance with manufacturers’ recommendations. Patients are savvy researchers. If what you tell them contradicts the prevailing opinion/recommendation, what incentive do they have to follow the remainder of your instructions?
Patients reportedly recognized the significance of replacing lenses on schedule, with 94% of DD wearers, 71% of two-week replacement SiHy wearers and 80% of one-month replacement SiHy wearers rating replacement schedules as either “extremely important” or “important.”7
However, even though most patients deemed replacement schedule an important consideration, there was still a 40% non-compliance rate with replacement frequency compared to manufacturers’ recommended replacement schedules. Even if you remove patients whose doctors prescribed a different replacement schedule from the manufacturer, there was still a 38% rate of non-compliance. The survey found the worst replacement schedule compliance was with the two-week lens modality, followed by monthly and then daily disposable lenses.6,7
What about contact lens care regimens? About half of those patients surveyed who were wearing SiHy lenses reported using a brand-name solution, and another 9% reported a hydrogen peroxide-based solution. A startling 40% reported they could not recall or did not know the name of their solution, which begs the question of possible generic usage or frequent switching of solutions due to cost and convenience. About half reported replacing lens cases either every three months or sooner, while 36% percent replaced the case every six to 12 months. A surprising 14% said they never replaced their lens case.7
Signs of Non-Compliance
Here are some methods you might consider to help garner information from your patients about lens care compliance.
• Ask patients which solution they are using. Don’t ask if they are using the solution you prescribed, because it is too easy for them to simply reply “yes.” Alternatively, you can keep a variety of solutions on hand and when patients remove their lenses, ask them to use the solution that they have at home.
If certain patients hesitate or don’t know which solution to use, you may need to further educate these individuals. Having a colored picture of what most major brand and generic solution bottles look like may also be a useful way to identify current habits.
• Ask patients how often they sleep in their lenses. For most, it’s not an “if,” but a “when.” Acknowledging that it does happen is a safe way to broach the topic with your patient. Most patients don’t like to “get in trouble” at the eye doctor, so encouraging candid communication will only elevate trust levels with your patients. Then, you can gently remind them “when and why” sleeping in certain contact lenses is appropriate or inappropriate.
• Keep patients up to date. It might seem obvious, but talking to a patient who bought less than a year’s supply of lenses from you, has taken two years to come back to you and has no reliable back-up spectacles may reveal some poor wear habits. Take this opportunity to discuss other lenses that may better match patients’ current wear and care habits, the advantages of fresh and sterile lenses, and how technology continues to improve. If they see you as a brand new source of information every year, and understand more about their ocular health and wellness, patients will be more likely to return as you prescribe.
• Discuss removal and cleansing habits. The confusion with rubbing lenses during the cleaning process needs to be clarified, especially with your long-term lens wearers. Ask patients what they do when removing their lenses. Be sure to leave your questions open-ended. You may learn that they are plopping those lenses back into their cases with old solution.
• Ask them to bring in their lens case. One look at its cleanliness will probably give you a better understanding of their care habits than any personal reports.
Steps to Improve Compliance
Now that we have refreshed ourselves on what signs of non-compliance to look for, what can we do to improve compliance?
1. Identify those who are likely to be compliant. The more simplistic the contact lens care regimen, the easier is it to be compliant. Additionally, the better the material technology, the less likely that complications will arise. And, it is important to note that patients who are fit in monthly or daily lenses often will have better compliance rates.6
Brand new contact lens wearers may be more compliant because they have not yet had any personal or outside influence to alter their care responsibilities. Take the time to foster positive compliance habits in new wearers as well as reinforce the reasons why they should heed your advice.
2. Identify those who are likely to be non-compliant. Patients who are new to your practice and have been fitted elsewhere may have received advice about contact lens care and replacement that contradicts either your advice or what is in their best interest for health and comfort.
Additionally, long-term contact lens wearers are most likely to slip into poor habits, such as choosing a different cleaning solution because they never did understand why one solution was different from another. Price, convenience or “whatever their spouse bought at the pharmacy” may override a meek recommendation by their eye care practitioner. Overall, being aware of possible ingrained habits will enable your practice to properly unteach non-compliant patients.
3. Educate EVERY time. It may seem mundane and repetitive, but repeating why a lens needs to be replaced on a specific schedule, why a particular solution should be used with advanced lens materials and why a case should be replaced frequently is important each and every time a patient is in your office. Explanations don’t need to be complex, but should be straightforward clarifications that the patient can relate to.
Here are some simple, yet effective, recommendations:
––“Replace your lenses every month to reduce your risk for infection, improve comfort and guarantee better vision.”
––“This particular cleaning and disinfecting solution is more compatible with the advanced material I fit you in, and other solutions have proven to be less effective.”
––“Replace your case every couple of months to ensure that it isn’t a major source of contamination for your lenses.”
These steps will serve to enlighten your contact lens patients as well as add tremendous value to their experience each and every time they are in your office. These simple recommendations are of very little cost to you, but the experience for the patient is priceless.
Compliance with contact lenses ultimately depends upon patients following our instructions. Make it easy for them to succeed. With advanced technology, a multitude of lenses and modalities and new care options, you can guide most patients to safe, comfortable and successful experiences with their contact lenses.
Dr. Wesley practices in Medina, Minn., where she focuses on primary eye care optometry with an emphasis on contact lenses. She is a fellow of the American Academy of Optometry and was recently awarded the 2011 Minnesota Young Optometrist of the Year award.
Dr. Wesley is a consulting lecturer and research investigator for Alcon, Allergan, Revolution EHR and Vistakon.
1. Karpecki PM, Schechtman DL. Microbial threats in CL wear. Rev Optom. 2010 Dec;147(12):69-70.
2. United States Food & Drug Administration. Guidance for Industry: Premarket Notification (510(k)) Guidance Document for Contact Lens Care Products. Available at:
www.fda.gov/downloads/MedicalDevices/DeviceRegulationandGuidance/GuidanceDocuments/UCM080218.pdf (accessed July 6, 2011).
3. International Standards Organization ISO 14729. Ophthalmic Optics––Contact Lens Care Products. Microbiological requirements and test methods for products and regimens for hygienic management of contact lenses, 2001.
4. Collins MJ, Carney LG. Patient compliance and it’s influence on contact lens wearing problems. Am J Optom Physiol Opt. 1986 Dec;63(12):952-6.
5. Silicone Hydrogels. Quick vote results––2009. Available at:
www.siliconehydrogels.org/vote_3/vote_history.asp (accessed July 6, 2011).
6. Dumbleton K, Woods C, Jones L, et al. Comfort and vision with silicone hydrogel lenses: effect of compliance. Optom Vis Sci. 2010 Jun;87(6):421-5.
7. Dumbleton K, Woods C, Jones L, et al. Patient and practitioner compliance with silicone hyrogel and daily disposable lens replacement in the United States. Eye Contact Lens. 2009 Jul;35(4):164-71.
8. Dumbleton K, Woods C, Jones L, Fonn D. How compliant are today’s lens wearers? Available at:
www.clspectrum.com/article.aspx?article=104344 (accessed July 6, 2011).

