Characteristics of IFIS
This loss of iris muscle tone results in the condition known as IFIS that occurs during phacoemulsification cataract surgery, and was first described by Drs. David Chang and John Campbell in 2005.1 IFIS is characterized by a triad of factors: a flaccid or floppy iris that billows in response to normal irrigation current in the anterior chamber during the standard phacoemulsification cataract surgery; a marked propensity for the iris to prolapse in the main phacoemulsification and side-port surgical incisions in the eye; and progressive pupil constriction during surgery that makes it significantly more difficult to proceed with the cataract extraction.2
Most of these patients do not dilate well during the initial eye examination, and this may be the first clinical clue to the referring optometrist that the patient has IFIS. During surgery, the pupil also has a tendency to not dilate sufficiently or, if it does dilate, it quickly and progressively becomes more miotic as the cataract surgery progresses.

A closeup view of one of the Malyugin ring’s
four circular coils. This device creates a
rounded pupil in patients with IFIS who
undergo cataract surgery. Courtesy:
MicroSurgical Technology
The iris floppiness is usually identified during the hydrodissection (injection of balanced salt solution between the natural lens layers and the capsule to loosen the lens within the capsular bag) and phacoemulsification steps of the cataract extraction. From a surgeon’s perspective, the iris demonstrates a poor structural consistency, similar to that of a wet dishrag.3 The poor iris tone allows the iris tissue to move easily with the intraocular irrigation currents of the phacoemulsification probe. This causes the atonic iris to prolapse into the surgical incision sites and potentially get aspirated into the phacoemulsification probe, causing rips, tears or even significant loss of iris tissue.
Red Flags
A medical history and a review of current and past medication use can help identify the patient with IFIS. This syndrome is associated with medications that are used to treat men with benign prostatic hyperplasia (BPH) and may also be prescribed in women to treat urinary retention or urinary hesitancy.
The oral medication Flomax (tamsulosin, Boehringer Ingelhein) is currently the most commonly prescribed agent for patients with BPH.4 Tamsulosin is just one of a number of systemic alpha-adrenergic receptor antagonists that are used to improve urinary outflow by relaxing the smooth muscle tissue in the prostate and urinary bladder neck.2
Unfortunately, this high specificity for smooth muscle tissue also results in this drug causing a loss of the normal iris dilator smooth muscle tone.5 A recent study found that on average, iris dilator muscle tissue was 23% thinner in individuals who used tamsulosin than in those who were never exposed to this medication.6
Rapaflo (silodosin, Watson Pharma) is another alpha-1 blocker that has recently been introduced for the treatment of BPH symptoms. Silodosin closely resembles tamsulosin in its strong affinity and specificity for the iris dilator muscle. Both tamsulosin and silodosin are highly selective for the alpha-1A receptor subtype, which appears to predominate in both the prostate and the iris dilator muscle.7

Although these two medications may be the most problematic when it comes to causing IFIS, there are a number of others that can result in miotic and floppy irides during cataract surgery.
Other prescription medications used to treat BPH include Cardura (doxazosin, Pfizer), Hytrin (terazosin, Abbott Laboratories) and Uroxatral (alfuzosin, Sanofi-Aventis).
Although these drugs are alpha-antagonists like tamsulosin and silodosin, they are not specific for the alpha-1A receptor subtype and may not always exhibit the extreme form of IFIS. However, because it is impossible to identify beforehand which patient taking one of these medications will exhibit the entire spectrum of the syndrome, be sure to warn the surgeon if the patient is on one of these drugs.
Other prescription medications implicated in IFIS that are not used for the treatment of BPH but for various other systemic conditions include Requip (ropinirole, GlaxoSmithKline), which is a dopamine agonist and is used in the treatment of Parkinson’s disease and restless leg syndrome; labetalol hydrochloride, which is a mixed alpha/beta adrenergic antagonist and is used in the treatment of systemic hypertension; and mianserin (Bolvidon, Norval, Tolvon), which is an alpha-2 adrenergic receptor antagonist that is used to treat depression.8-10
A non-prescription drug, saw palmetto (Serenoa repens), an herb extract, has been used as a holistic method to treat BPH and was found to cause IFIS.11,12 The exact mechanism of saw palmetto is not clear, but it appears to inhibit human alpha 1-adrenoreceptors in vitro, an action that parallels the mechanism of action of alpha 1-adrenergic blockers such as tamsulosin.13
Recently, a comprehensive antioxidant supplement named All One Powder (All One Nutritech) has been found to be a possible cause of IFIS.14 One of its ingredients, choline, is hypothesized to be the component that causes the IFIS as it may lead to enough parasympathetic stimulation to permanently affect the iris.14
Stopping these medications prior to surgery may be of some benefit in relieving the IFIS that accompanies their use—or maybe not. At least for tamsulosin, IFIS has still been observed in patients who discontinued therapy as long as nine months or even three years before cataract surgery.1,15
The persistence of IFIS several months after stopping tamsulosin implies that the atrophic iris changes resulting in an atonic pupil are probably permanent. In some studies, IFIS developed as soon as three months after the patient started taking tamsulosin— I had one patient who developed all the intraoperative changes after taking only two doses of tamsulosin.16
The other factor to consider is that patients themselves are hesitant to stop using these agents. Many patients obtain significant relief from their disease (BPH) when taking one of the alpha-1 blockers and are not willing to stop the medication even for brief periods of time. The other non-BPH related medications are also impractical to discontinue since stopping them can result in significant morbidity to the patient.
Patient Screening
The prevalence of IFIS is estimated to be as high as 2% in the cataract surgery population.1 Male patients exposed to tamsulosin develop the syndrome at a rate of 57% to 100%.1,17-18 Half of men older than 50 years and 90% of men older than 85 years have BPH and may be taking one of the alpha-1 blocking agents.19 Cataracts also have a common occurrence in this population and the incidence increases with age, affecting 20% of people aged 65 to 74 years and 50% of those older than 75 years.20
Because BPH and cataracts appear to occur frequently in the same male population, screen these patients for these medications. Inform the ophthalmic surgeon to be prepared to take decisive action to increase the chances of a successful surgical outcome.
A recent study found that if the cataract surgeon was aware beforehand of the potential risk of IFIS occurring, and then implemented appropriate compensatory surgical techniques to minimize the impact of the IFIS changes during the surgery, there was a significant decrease in the overall complication rate.21 This study found that although 73% of patients evaluated had moderate to severe IFIS, the rate of posterior capsular rupture and vitreous loss was only 0.6%, and 95% of eyes achieved a best corrected visual acuity of at least 20/40.21
Surgical Strategies
Because there is no simple solution to decrease the risk of IFIS, preoperative and intraoperative management strategies need to be used. These can be divided into three main categories: pharmacological, viscoelastic agents, and mechanical pupil-expansion devices.
• Pharmacologics. The pharmacological approach to improve pupil dilation in patients with IFIS includes the preoperative application of atropine sulfate 1% starting one week before the cataract surgery for sustained mydriasis of the pupil.22 Intracameral (direct injection into the anterior chamber) of epinephrine has also been a suggested strategy.23
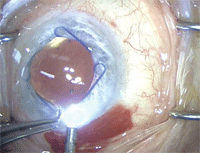
Placement of flexible iris retractors.
Courtesy: MSI Precision
• Viscoelastics. More retentive ophthalmic viscoelastic agents, such as Healon5 (sodium hyaluronate 2.3%, Abbott Medical Optics), can be used to viscodilate the pupil mechanically, preventing it from prolapsing to the surgical incisions.2 These high-density viscoelastic agents are more difficult to remove from the eye at the conclusion of the surgery, increasing the risk of a postoperative intraocular pressure spike. The comanaging optometrist should be aware if their operating surgeon is routinely using them.
• Mechanical devices. Beyond medications and viscoelastics, mechanical devices that expand and support the pupil diameter during surgery are the most reliable means of maintaining a safe and consistent pupil diameter.2 These include iris retractors and a variety of pupil expansion rings. These devices are most safely placed before the capsulorrhexis creation. Because the capsulorrhexis is made early during the cataract surgery, the surgeon will need to decide whether to use such a device before starting the actual surgery.
Flexible iris retractors are inserted through paracentesis incisions made in the cornea, close to the limbus. Four equidistant paracentesis sites are used. The iris hook end of the retractor is then used to engage the pupillary margin and the retractor is then secured with an adjustable silicone sleeve.24 These retractors are removed from the eye after the cataract surgery is completed.
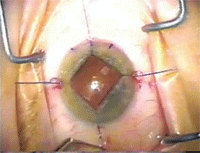
Malyugin ring positioned in the eye.
Courtesy: MicroSurgical Technology
Various pupil ring expanders have also been used [(Graether, Eagle Vision), (5S Morcher, Morcher GmbH) and (Perfect Pupil, Milvella)]. The one most recently introduced to the market is the Malyugin ring (MicroSurgical Technology), which is a foldable, square device made of polypropylene that is much thinner than earlier versions of similar expansion rings. This flexible ring is injected into the anterior chamber, where its four circular coils engage the pupil edge, thus expanding it. This creates a rounded pupil during the cataract surgery.
As with the iris retractors, all these pupil expansion rings need to be removed at the conclusion of the surgical case.
Follow-up Care
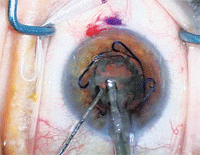
Phacoemulsification with Malyugin ring maintaining the pupil. Courtesy: MicroSurgical Technology
Assuming the IFIS cataract surgery was uneventful––even if one or more of these surgical management maneuvers were used––you should be able to use the standard postoperative drug regimen and follow-up schedule as with patients who underwent a more routine surgery.
However, pay closer attention to the intraocular pressures if a high-density viscoelastic agent was used. You may also notice more anterior chamber inflammation secondary to additional intraoperative iris manipulation by the surgeon, especially if one of the pupil expansion devices was used. This may require you to increase the dose of anti-inflammatory drugs.
Finally, closely evaluate the eye for any potential iris tissue entrapment in either the main surgical incision or the side-port incision. It is not unusual to see small notches in the pupil margin, especially if the surgeon used iris retractors. These are harmless and should not affect the final postoperative visual
outcome.
As most successful ophthalmology practices realize, comanagement of cataract surgery cases with optometrists is not only mutually beneficial to both the ophthalmologist and optometrist; but, more importantly, it is often in the best interest of the patient. Ophthalmic surgeons like me who comanage many cataract patients believe that today’s optometrist is well versed in pathology and conscientious in the care of the patient.
Dr. Skorin is the senior staff ophthalmologist at the Albert Lea Eye Clinic, Mayo Health System in Albert Lea, Minn.
1. Chang DF, Campbell JR. Intraoperative floppy iris syndrome associated with tamsulosin. J Cataract Refract Surg 2005;31:664-73.
2. Chang DF. Intraoperative floppy iris syndrome. In: Agarwal A (ed): Phaco Nightmares: Conquering Cataract Catastrophes. Thorofare, NJ: Slack, Inc.; 2006: 131-9.
3. Skorin L, Larsen K. A newly identified miotic syndrome associated with the use of a popular prostate drug. Clin Surg Ophthalmol. 2005;23(4):122-8.
4. Kaplan SA. Use of alpha-adrenergic inhibitors in treatment of benign prostatic hyperplasia and implications on sexual function. Urology. 2004 Mar;63(3):428-34.
5. Chang DF, Braga-Mele R, Mamalis N, et al. ASCRS White Paper: Clinical review of intraoperative floppy-iris syndrome. J Cataract Refract Surg. 2008 Dec;34(12):2153-62.
6. Santaella RM, Destafeno JJ, Stinnett SS, et al. The effect of alpha 1-adrenergic receptor antagonist tamsulosin (Flomax) on iris dilator smooth muscle anatomy. Ophthalmology. 2010 Sep;117(9):1743-9.
7. Chang DF. What is the best way to manage intraoperative floppy iris syndrome? In: Chang DF (ed): Curbside Consultation in Cataract Surgery: 49 Clinical Questions. Thorofare, NJ: Slack, Inc.; 2007: 121-5.
8. Fine IH, Dworetzky J, Hoffman RS, Packer M. Range of drugs associated with IFIS. J Cataract Refract Surg. 2009 Jan;35(1):202.
9. Calotti F, Steen D. Labetolol causing intraoperative floppy-iris syndrome. J Cataract Refract Surg. 2007 Jan;33(1):170-1.
10. Ugarte M, Leong T, Rassam S, Kon SH. Intraoperative floppy-iris syndrome, alpha 1-adrenergic antagonists, and chronic intake of mianserin: is there an association? J Cataract Refract Surg. 2007 Jan;33(1):170.
11. Bent S, Kane C, Shinohara K, et al. Saw palmetto for benign prostatic hyperplasia. N Engl J Med. 2006 Feb 9;354(6):557-66.
12. Yeu E, Grostern R. Saw palmetto and intraoperative floppy-iris syndrome. J Cataract Refract Surg. 2007 May;33(5):927-8.
13. Goepel M, Hecker U, Krege S, et al. Saw palmetto extracts potently and noncompetitively inhibit human alpha 1-adrenoceptors in vitro. Prostate. 1999;38:208-15.
14. Seth A, Truscott S, Chew J. Health supplement associated with intraoperative floppy-iris syndrome. J Cataract Refract Surg. 2010 Jun;36(6):1050-1.
15. Chapple C, Andersson KE. Tamsulosin: an overview. World J Urol. 2002 Apr;19(6):397-404.
16. Cheung CM, Awan MA, Saudramouli S. Prevalence and clinical findings of tamsulosin-associated intraoperative floppy-iris syndrome. J Cataract Refract Surg. 2006 Aug;32(8):1336-9.
17. Chandha V, Borooah S, Tey A, et al. Floppy iris behavior during cataract surgery: associations and variations. Br J Ophthalmol. 2007 Jan;91(1):40-2.
18. Pärssineu O, Leppäneu E, Keski-Rahkonen P, et al. Influence of tamsulosin on the iris and its implications for cataract surgery. Invest Ophthalmol Vis Sci. 2006 Sep;47(9):3766-71.
19. Ziada A, Rosenblum M, Crawford ED. Benign prostatic hyperplasia: an overview. Urology. 1999 Mar;53(3 Suppl 3a):1-6.
20. Blouin M-C, Blouin J, Perreault S, et al. Intraoperative floppy-iris syndrome associated with alpha 1-adrenoreceptors: Comparison of tamsulosin and alfuzosin. J Cataract Refract Surg. 2007 Jul;33(7):1227-34.
21. Chang DF, Osher RH, Wang L, Koch DD. Prospective multicenter evaluation of cataract surgery in patients taking tamsulosin (Flomax). Ophthalmology. 2007 May;114(5):957-64.
22. Bendel RE, Phillips MB. Preoperative use of atropine to prevent intraoperative floppy-iris syndrome in patients taking tamsulosin. J Cataract Refract Surg. 2006 Oct;32(10):1603-5.
23. Schulze R. Epi-Shugarcaine with plain balanced salt solution for prophylaxis of intraoperative floppy-iris syndrome. J Cataract Refract Surg. 2010 Mar;36(3):523.
24. Espaillat A, Rowe SG. The small pupil. In: Pineda R, Espaillat A, Perez VL, Rowe SG (eds): The Complicated Cataract. Thorofare, NJ: Slack, Inc.; 2001: 15-38.

