|
 |
The retina is among the most delicate and unforgiving tissues to operate on in the human body. It does not regenerate and is surrounded by a dense vascular supply, which carries constant risk for scarring and inflammation. The slightest disruption of only several microns of retinal tissue can produce devastating and permanent vision loss. These inherent limitations have laid the foundation for how we understand and, in turn, counsel our patients on retinal trauma, disease and surgical repair.
With the advent of new surgical techniques, we now have second chances to repair complex retinal surgical issues that may not respond to a single surgery. Traditionally, if a retinal surgery resulted in sub-optimal results, the heavily invasive and blunt nature of subsequent retinal surgeries did not justify the risk of additional repairs. Now, micro-incisional techniques and high-speed vitrectomies enable surgeons to attempt repairs in even the most challenging cases.
The patient in this video had retinal trauma from a firework explosion to the eye. The retina was initially reattached with silicone oil tamponade and peripheral laser. Subsequent recurrent epiretinal membrane formation occurred, leading to decreased vision and further retinal traction.
Until recently, the prognosis at this point would have been bleak. Further surgical intervention would have been extensive and invasive, with higher risk and potentially minimal benefit.
But in the past five to 10 years, we’ve adopted a minimally invasive approach that uses microincision technology within the silicone oil-filled eye to perform the tissue dissection and retinal reattachment. This technique bypasses lengthy and invasive steps traditionally performed, such as oil removal and subsequent re-replacement or scleral buckling procedures. The reattachment rate with the minimally invasive approach is between 80% to 90%, compared with 50% reported for the more invasive, traditional approach.
What’s a Retinotomy?A retinotomy is an advanced technique in which the surgeon removes nonessential or peripheral retinal tissue. It is typically done to relieve retinal traction or limit intractable retinal foreshortening in post-traumatic proliferative vitreoretinopathy. |
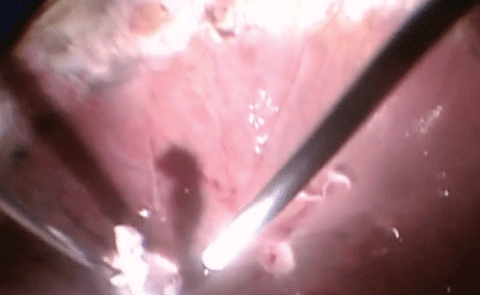
In the accompanying video, the tenacious epiretinal membranes are removed underneath the silicone oil. Keep in mind that without the obstruction of silicone oil, epiretinal membrane removal is incredibly difficult and delicate in an otherwise healthy eye. However, the oil tamponade assists in gently holding the retina in position while overlying or underlying scar tissue is removed.
The video also shows removal of excess fibrosis near the previous retinotomy site. Then, laser applied around the previous retinotomy site reduces the risk of detachment. The vitreous cavity is then topped up with silicone oil to provide an effective tamponade, achieving long-term functional and anatomical success.
This patient will require close follow-up care by the retinal specialist. Eventually, an optometrist will provide vision correction. The optometrist and retinal specialist then often share responsibility for monitoring the retina. They’ll watch for long-term complications such as retinal detachments, subretinal neovascular membranes, band keratopathy, high or low intraocular pressure, and cataracts in phakic patients.
As surgical innovation continues to push the boundaries of retinal intervention, be sure to consult your retina specialist on patients who have had previous retinal surgery and may not have achieved an optimal visual result—yet.