 In July 2006, a 43-year-old white male presented as a new patient for a wellness examination. His ocular history was significant for bilateral LASIK in 2000, and he had an enhancement procedure in the left eye approximately one year later. Pre-LASIK correction was in the -4.50D range O.U. with minimal corneal cylinder. He reported good uncorrected distance vision as well as good near vision through his reading glasses.
In July 2006, a 43-year-old white male presented as a new patient for a wellness examination. His ocular history was significant for bilateral LASIK in 2000, and he had an enhancement procedure in the left eye approximately one year later. Pre-LASIK correction was in the -4.50D range O.U. with minimal corneal cylinder. He reported good uncorrected distance vision as well as good near vision through his reading glasses.
He also reported a positive family history of glaucoma; his mother and older brother were both medicated for it. His only medication was hydrochlorothiazide (HCTZ) for hypertension, and he reported an allergy to penicillins.
Diagnostic Data
Best-corrected visual acuity was 20/15- O.D. and O.S. through minimal myopic astigmatic correction. Pupils were equal, round and reactive to light and accommodation with no afferent defect.
A slit lamp examination of the anterior segments was unremarkable—his corneas were clear, with well-centered flaps, no edge defects or ingrowth, no striae, and pristine interfaces O.U.
Intraocular pressure measured 19mm Hg O.D. and 21mm Hg O.S. by applanation tonometry.
Dilated exam showed that his crystalline lenses were clear in both eyes. His optic nerves were characterized by cup-to-disc ratios of 0.40 x 0.65 O.D. and of 0.45 x 0.55 O.S. Both discs were tilted and both perioptic regions were characterized by marked peripapillary atrophy. The vascular and macular examinations of both eyes were unremarkable, as were the peripheral retinal evaluations. We obtained baseline stereo-optic nerve photos.
I asked the patient to return for a glaucoma evaluation (I didn’t use the word “glaucoma,” of course), which included baseline visual field testing, gonioscopy and pachymetry. At that time, standard automated perimetry (SAP) fields were clear in both eyes, gonioscopy demonstrated grade IV+ open angles 360° in both eyes with mild trabecular pigmentation. Pachymetry measured 531μm O.D. and 502μm O.S. I asked him to come back again in one year.
Since 2006, the patient has been compliant with annually scheduled follow-up visits.
Discussion
We know that post-laser refractive corneas are thinner than preoperative corneas, and we know that thinner corneas result in artificially lower IOP readings when using Goldmann applanation tonometry.
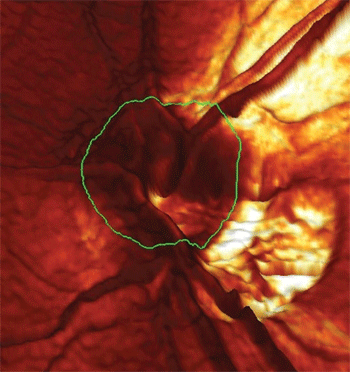
3-D topographic image of the left eye showing a large area of zone Beta peripapillary atrophy inferotemporally.
We also know that tilted discs often are accompanied by peripapillary atrophy, and that peripapillary atrophy—and progression of peripapillary atrophy in particular—is associated with neuroretinal rim changes in the sectors of the optic nerve that correspond to peripapillary atrophic progression. Furthermore, we know that tilted discs in and of themselves can be associated with a variety of visual field defects.
This patient presented with all of these confounding factors, along with a relatively strong history of glaucoma. So, how does one make an initial determination as to whether glaucoma coexists with these other findings?
Certainly, our analysis of risk factors is important in helping form a framework upon which to build an individualized management plan for each patient. Aside from the physical characteristics of this patient’s eyes, (asymmetric cups, tilted discs, peripapillary atrophy, iatrogenically-induced thin corneas and probably “true” ocular hypertension), his only other risk factor is the family history of glaucoma.
While these confounders certainly make critical evaluation of optic disc characteristics difficult, at least in the context of the presence or absence of glaucoma, formulating a management plan in this case is relatively simple. While this patient certainly can be considered to be at risk for glaucoma, there was no clear evidence that he actually had glaucoma.
The operational words here are “clear evidence.” In these cases, it is truly difficult to assess these optic nerves simply by appearance (structure) and field testing (function).
(By the same token, there was also no clear evidence that he did not have glaucoma, other than perhaps the absence of visual field defects.)
So, here is an instance in which we can take advantage of the fact that open-angle glaucoma develops and progresses slowly over time. While this patient may have actually had glaucoma when he first presented, my initial treatment plan was simply to monitor rather than to medically intervene because he did not appear to actually manifest glaucoma. And fortunately for the patient, he continues to comply with scheduled visits.
Since his initial presentation in 2006, the patient’s IOP has ranged from 15mm Hg to 20mm Hg O.D. and 16mm Hg to 23mm Hg O.S. Meanwhile, SAP fields have remained stable. Most recently, the patient underwent field studies using the Heidelberg Edge Perimeter (HEP, Heidelberg Engineering), which also were essentially normal. Heidelberg Retina Tomography-3 (HRT-3, Heidelberg Engineering) imaging of both optic nerves was performed and has remained stable since July 2010.
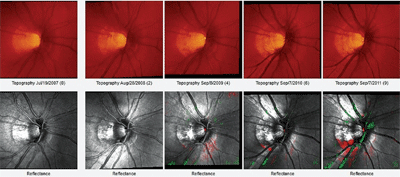
Topographic change analysis of the right eye, from July 2007 to September 2011, showing progression of zone Beta peripapillary atrophy in the inferotemporal aspect of the nerve.
Now What?
But, when seen most recently in July 2011, HRT-3 Topographic Change Analysis indicated early changes to the inferior temporal (IT) neuroretinal rim areas O.U. as well as the corresponding IT regions of the retinal nerve fiber layer.
Could this be the first manifestation of structural conversion in this patient? Absolutely. Accordingly, I asked the patient to return in three months for repeat HEP field studies, HRT-3 imaging and IOP measurement.
In the interim, I still have not medicated this patient in either eye simply because of the confounding nature of the optic nerve characteristics and the lack of consistent, documented change (either to the structure or the function of the optic nerve) over time.
In time, however, that too may change.

