An 18-year-old black female presented with a chief complaint of dim and occasionally blurry vision. She was uncertain if this occurred in one or both eyes, but stated that, when it did occur, it usually lasted several seconds. Otherwise, her vision was good, and she believed that she did not need glasses. Her medical and ocular histories were unremarkable.

On examination, her entering visual acuity was 20/20 O.U. Confrontation visual fields were full to careful finger counting O.U. Her pupils were equally round and reactive, with no afferent defect. Extraocular motility testing was normal. The anterior segment examination was unremarkable in both eyes. Her IOP measured 16mm Hg O.U.
On dilated fundus exam, the vitreous was clear. The posterior pole and optic nerves can be seen in figures 1 and 2. The macula, vessels and peripheral retina were normal. We also obtained an OCT scan as well as additional imaging studies (figures 3 and 4).
Take the Retina Quiz
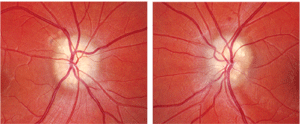
1, 2. Here are the fundus photographs of our patient (O.D. left, O.S. right).
1. How do you explain her symptomatology?
a. Nonspecific in nature, and probably just normal.
b. Transient visual obscurations related to her condition.
c. Impending retinal vascular occlusion.
d. Probably from a severely reduced visual field.
2. What is the correct diagnosis?
a. Optic nerve head drusen (ONHD).
b. Papilledema.
c. Optic atrophy.
d. Astrocytic hamartoma.
3. What do figures 3 and 4 show?
a. Leakage secondary to atrophic optic nerves.
b. Autofluoresence of hyaline bodies.
c. Swollen optic nerves.
d. Hyperfluorescence from a mass lesion.
4. How should this patient be managed?
a. Observation.
b. Periodic visual fields.
c. Refer for an MRI and lumbar puncture (LP).
d. Anti-VEGF therapy.
Retina Quiz Answers: 1) b; 2) a; 3) b; 4) b.
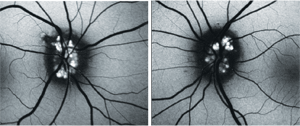
3, 4. What are these images and what do they reveal?
Discussion
The most striking feature in our patient is the elevated appearance of her optic nerves, combined with the lumpy/bumpy appearance of the disc margins. Based on the clinical appearance, it should come as no surprise that our patient had ONHD. The drusen were very apparent, especially superior and inferior in each eye where the appearance of the drusen has often been described as a having a “rock candy” appearance. In fact, the word “drusen” was used in the mining industry more than 500 years ago to describe a crystal-filled space in a rock.1 And, you could clearly see that our patient’s drusen had a crystal-like appearance.
ONHD are usually detected as an incidental finding during a routine eye exam and are perhaps the most common cause of pseudopapilledema––an anomalous optic disc elevation that can have a striking resemblance to true optic disc swelling or papilledema.2 ONHD consist of homogenous, globular concretions that are composed predominately of a mucoprotein matrix with significant quantities of acid mucopolysaccharides, small amounts of ribonucleic acid and occasionally iron.1
It is thought that the ONHD develop as a result of axonal crowding secondary to a congenitally abnormally small optic canal. ONHD have a prevalence of about 3.4 per 1,000, but increase to more than 3% when there is a family history. Additionally, ONHD are bilateral in 86% of cases.1,3
Patients with ONHD may present in one of two ways: The ONHD may be visible (as was the case in our patient) or they may be “buried” (in which case, the drusen are not visible due to their more posterior location within the optic nerve). Buried drusen cases are often the most worrisome because of the suspicion that the patient may have true disc edema or papilledema. In this instance, ancillary testing is required to rule out the presence of an intracranial mass and/or confirm the presence of drusen.
In cases where the drusen are not clearly visible––but there is a high suspicion of their presence––fundus autofluorescence may be helpful, because the individual drusen hyperfluoresce. This was performed on our patient, and the autofluorescence of the drusen was quite striking. In the absence of fundus autofluorescence, the drusen may also be more visible when viewing with red-free filters.
The evolution of ONHD is a dynamic process that starts early in life. In infants and children, the drusen tend to be buried, but will slowly migrate anteriorly as the patient ages. One study showed that the mean age in which ONHD was first visible was 12.1 years.1 Over time, the drusen will enlarge and calcify, resulting in more of a scalloped appearance in the disc margin.
Because the ONHD were obvious on clinical exam in our patient, an extensive work-up was not necessary. However, secondary complications can occur. Up to 75% of affected patients experience visual field defects that can be nonspecific in nature or can occur in an area where there is a retinal nerve fiber layer (RNFL) defect.1
Interestingly, an inferior RNFL defect could be seen in the left eye of our patient. We obtained a visual field and there was a small defect; however, it did not correspond to the RNFL defect. Additionally, there was a visual field defect in the right eye that was larger than what we saw in the left eye. Specifically, it was an inferior arcuate defect that was more typical for a patient with an RNFL defect. Even though there was no RNFL defect seen on clinical exam in the right eye, a denser area of ONHD could be seen superior-temporal that corresponded to the area of the defect. We obtained OCT imaging of the optic nerve, which showed areas of RNFL thinning corresponding to the field defects. Keep in mind, the visual field defects in patients with ONHD tend to progress very slowly.
Other complications with ONHD include perpapilary or peripapillary hemorrhages; ischemic optic neuropathy; retinal vascular occlusion; and peripapillary subretinal neoascularization (however, these are very rare).1,3
So, what is going on with our patient? Interestingly, about 8.6% of patients with ONHD will complain of transient visual loss, as was the case with our patient.1 We do not completely understand why this occurs. It is believed that the drusen may produce increased interstitial pressure and decreased perfusion pressure in the intraocular portion of the optic nerve, which may result in minor fluctuations in arterial, venous and even cerebrospinal fluid pressure. This, in turn, may result in a brief decrease in optic nerve perfusion, causing the transient changes in vision.
Unfortunately, we could not do anything for this patient other than make her aware of her condition. We educated her about the findings and will continue to follow her with semi-annual visual field tests.
This Retina Quiz is in memory of Dr. J. Lawton Smith, a charismatic neuro-ophthalmology giant who, for most of the second half of the 20th century, was considered to be the best-known ophthalmologist in the world. Dr. Smith was one of the founding five at the Bascom Palmer Eye Institute. He passed away on January 10, 2011 at the age of 81.
1. Brodsky MC. Congenital anomalies of the optic nerve. In: Miller NR, Newman NJ, Biousse V, Kerrison JB (eds.). Walsh & Hoyt”s Clinical Neuro-Ophthalmology, 6th ed. Vol I. Philadelphia: Lippincott Williams & Wilkins; 2005, 151-95.
2. Stiefel JW, Smith JS. Hyaline bodies (drusen) of the optic nerve and intracranial tumor. Arch Ophthalmol. 1961 Jun;65(6):814-6.
3. Auw-Haedrich C, Staubach F, Witschel H, Optic disk drusen. Surv Ophthalmol. 2002 Nov-Dec;47(6):515-32.

