 Q: I have a vernal keratoconjunctivitis patient who has a persistent shield ulcer that just doesn’t seem to be healing. Topical medications, including steroids and antihistamine/mast cell stabilizers, aren’t working. Any suggestions?
Q: I have a vernal keratoconjunctivitis patient who has a persistent shield ulcer that just doesn’t seem to be healing. Topical medications, including steroids and antihistamine/mast cell stabilizers, aren’t working. Any suggestions?
A: Persistent shield ulcers in patients with vernal disease are vision threatening and need to be resolved as quickly as possible before they cause scarring in the visual axis. Most clinicians agree it is best to start with conservative therapy, including topical antihistamines/mast cell stabilizers, corticosteroids, antibiotics and preservative-free lubrication.
“Very often, these patients are young and tear copiously—when they do not respond to first-line therapy then I find corticosteroid ointments to be very effective,” says Eric Donnenfeld, M.D., clinical professor of ophthalmology at NYU School of Medicine. “The increased contact time on the ocular surface can often be the difference that helps these ulcers to resolve.” Additionally, he finds Restasis (cyclosporine ophthalmic emulsion 0.05%, Allergan) four times a day can be beneficial.
A hydrophilic bandage lens, along with systemic antihistamines, may also be helpful, says Jim Aquavella, M.D., professor of ophthalmology at the University of Rochester. “In difficult cases with significant inflammation, you may want to administer a sub-Tenon’s injection of soluble dexamethasone adjacent to the lesion,” he adds.
But some patients may have a fibrotic or calcified surface that simply won’t respond to medical therapy alone—in these cases, the corneas need aggressive scraping to remove the fibrotic/calcified tissue.
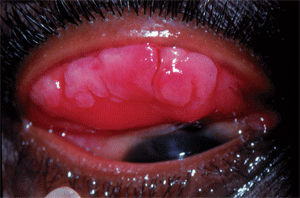
Giant papillary conjunctivitis in a patient with vernal conjunctivitis. Courtesy: Eric Donnenfeld, M.D.
When Christopher J. Rapuano, M.D., performs a scraping procedure, he prepares the cornea with a topical anesthetic and inserts an eyelid speculum, then takes a #15 blade and aggressively scrapes the redundant, necrotic epithelium down to Bowman’s layer. Bowman’s may appear slightly gray-white, but it should be fairly smooth. This allows a clean surface for the normal epithelium to repopulate. He then continues treatment with topical steroids, cyclosporine, antihistamine/mast cell stabilizers and antibiotics.
“In my experience, the epithelial defect now has a much better chance of healing,” says Dr. Rapuano, director of the Cornea Service Department and co-director of the Refractive Surgery Department at the Wills Eye Institute in Philadelphia. “If it doesn’t heal over the following week, a bandage soft contact lens, a ProKera (BioTissue) device or a glued/sutured amniotic membrane graft can be placed to aid in re-epithelialization.”
In patients with large cobblestone papillae, an injection of triamcinolone into the bed of the superior tarsal conjunctiva can resolve the offending mechanical aspect of this disease. Systemic antihistamines and corticosteroids can be helpful in the most difficult of cases.
“Of course, you always need to be concerned about infection,” Dr. Rapuano says. “If the shield ulcer appears infected, scrapings should be taken for smears and cultures, and the patient should be treated with intensive topical antibiotics (and no steroids) until infection is ruled out.”
In addition to these treatment strategies, the patient will likely have to make some lifestyle changes. Dr. Donnenfeld says it’s often helpful for the patient to see an allergist to undergo testing and learn about environmental modifications to remove or reduce allergens, which are frequently found in carpets, feather pillows and window drapes. Following resolution, long-term lubrication is essential.

