
Differentiating between dry eye and allergic conjunctivitis can be a complicated and frustrating task for many clinicians. Signs and symptoms of both dry eye and allergic conjunctivitis can be subjective and vague, and may appear to overlap.
The two conditions, however, do not share the same etiology, and treatment methods are different. Whether an individual has dry eye, allergy or a combination of both disorders, understanding the etiology and pathophysiology of each condition is essential for correctly diagnosing and treating patients.
Pathophysiology of Dry Eye
Despite the similar symptoms, dry eye and allergy each have a distinctive pathophysiology. Dry eye is caused by tear film instability resulting from insufficient or unhealthy production of one or more tear film components, namely:
Lipids. Lipid layer abnormalities often stem from meibomian gland disorders or blepharitis. These can cause rapid tear evaporation. As we age, our lacrimal glands produce fewer tears, which can result in reduced tear volume or tear flow.
Mucins. Ocular mucins are found both on the surface of the eye and freely floating in the aqueous. Underproduction of mucins by goblet cells and conjunctival epithelial cells can affect the ability of the tear film to adhere to the hydrophobic ocular epithelium.
Aqueous. The aqueous layer is generated by the lacrimal glands, and accounts for 90% of the tear film. The accessory glands are responsible for tear production, while the primary gland is associated with reflex tearing. Reflex tearing can sometimes be stimulated by the appplication of Schirmer I strips, which are used to measure tear volume. Some physicians believe reflex tears can render unanesthetized Schirmer measurements inaccurate. Fluorophotometry can provide more accurate measurements of tear volume and tear flow; however, it is also more time consuming.
Because these tear film abnormalities could be related to various environmental or biological influences, pinpointing the underlying cause of a patients dry eye symptoms may require a work-up that ranges from an extensive history to laboratory studies.
Blinking replenishes and maintains the integrity of the tear film; yet environmental, activity-related, psychological, and physiological factors can alter the blink rate.
When the blink rate is diminished, the tear film can become instable. Rapid tear film break-up caused by tear film instability can lead to ocular surface exposure, especially when combined with abnormal blink rates.
When tear film break-up occurs before a blink can replenish the tear film, some portion of the ocular surface will be exposed to the air. Over time, insufficient protection may promote surface cell desiccation and damage.
A detailed patient history is essential for subjective diagnosis and treatment of dry eye. Diagnosis of dry eye often incorporates fluorescein and lissamine green staining, which highlights damaged areas on the ocular epithelium, in the cornea and conjunctiva respectively.
Tear film break-up time (TFBUT), as measured following fluorescein dye instillation, can reveal tear film instability. Symptom or lifestyle questionnaires may offer a better understanding of a particular patients disorder.
Pathophysiology of Ocular Allergy
The ocular allergic reaction is a hypersensitivity response to pollen, animal dander, dust, or any other normally benign particle or substance. Initial exposure to an allergen primes the Th2-favoring immune system of the susceptible individual, and immunoglobulin E (IgE) antibodies bind to Fc (fragment crystallizable) receptors on conjunctival mast cells.
Mast cells are granulocytes that contain preformed mediators of allergy, most notably histamine. Subsequent exposure to the allergen induces cross-linkage of the allergen to the IgE receptors on the mast cells. The mast cells then degranulate, releasing both histamine and pro-inflammatory cytokines.
Histamine is the only allergic mediator that can cause the full range of allergic signs and symptoms, namely itching, redness, lid swelling, chemosis and tearing.1 It binds to both the H1 and the H2 receptors on the vascular endothelium, inducing dilation (redness) and endothelial gaping (swelling). Histamine that binds to the H1 receptor alone induces itching, redness and swelling.2
Since histamine is the only mediator of ocular allergy that produces itching, it is the key symptom for identifying ocular allergy.3 Diagnosis of allergy depends upon the appearance of ocular symptoms, patient history, allergy skin testing and the existance of ocular itch.
Dry Eye Etiology
Dry eye has always been linked to environmental factors, such as dry, windy conditions that rapidly desiccate the tear film. In this sense, dry eye can present either as an acutely exacerbated condition or as a chronic disorder.
Other factors associated with dry eye symptomatology include:
Autoimmune diseases. In diseases such as Sjgrens syndrome, immune system-induced inflammation attacks and destroys the lacrimal glands. Today, enhanced medical knowledge and treatments have allowed us to manage autoimmune diseases, such as Sjgrens syndrome and rheumatoid arthritis, that often cause dry eye.
LASIK and other surgical procedures. Although these may ultimately enhance a patients quality of life, such surgeries can produce temporary dry eye symptoms.
Blepharitis. This lid disorder, which is characterized by a dermatologic seborrhea and altered meibomian gland secretions, can destabilize the lipid layer of the tear film, causing poor lipid spreading and increased evaporation.4
Contact lens movement and irritation. Up to 52% of contact lens wearers report some signs and symptoms of dry eye.5
Use of systemic medications. Oral antihistamines and numerous other medications can result in ocular dryness.6
Age and gender. Postmenopausal women are particularly susceptible to developing dry eye.
Excessive visual tasking. For example, either watching a televison or staring at a computer monitor for eight hours a day.
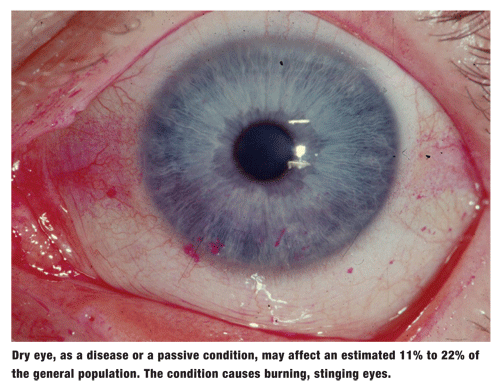
With all of these instigators of ocular dryness, dry eye, as a disease or a passive condition, may affect an estimated 11% to 22% of the general population.7
The many symptoms of dry eye include foreign-body sensation, general dryness, stinging, burning, grittiness and photophobia.
Nevertheless, discerning the underlying causes of a patients discomfort is vital to effectively manage the disorder and minimize both its signs and symptoms.
Allergy Etiology
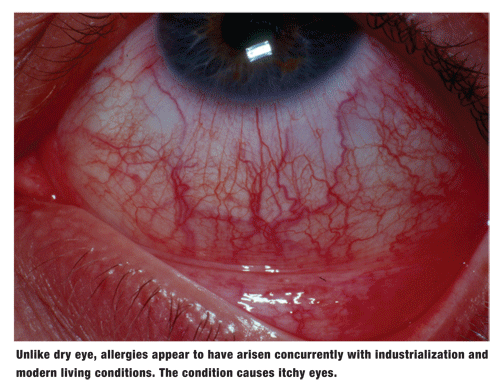
Unlike dry eye, allergies appear to have arisen concurrently with industrialization and modern living conditions. The hygiene and urban allergy hypotheses are both based on the idea that the surrounding environment can alter the immune systems Th1-Th2 balance.
Cohort studies in African children who harbor helminthes, such as Schistosoma haematobium, have revealed that the parasites induce production of IL-10, an anti-inflammatory cytokine.8 Consequently, these children often have a lower prevalence of atopy than non-infected children.
This discovery suggests that city dwellers, who have not been exposed to the soil or the forest, may be more prone to allergy. This theory has been supported by epidemiological studies of rural farmers and their children, who, like children infected with helminthes, have a lower prevalence of allergy than their urban counterparts.9-10
Given the inherent filth that comes with thousands of people living in close contact, however, one may find it difficult to believe that cities are more conducive to hygienic practices than farms.
Indeed, city-dwellers often have extraordinarily high rates of asthma, and non-atopic children who grew up on the farm can develop itchy, red, swollen eyes when they move to the city.11,12
Of course, the epidemiology of allergy extends beyond hygienic concerns and involves genetic influences in conjunction with the surrounding environment.
Differential Diagnosis
Dry eye and allergic conjunctivitis are two seperate conditions, with different epidemiologies, pathophysiologies and treatments. We must correctly differentiate between the two in order to provide the proper treatment.
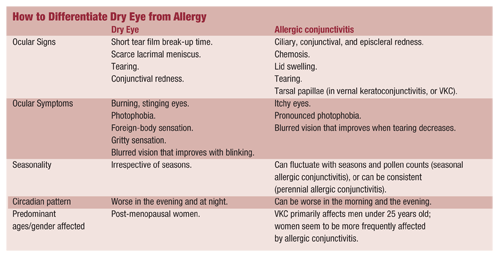
The differential diagnosis of the conditions can be simplified by dividing the patient population into two groups: the burnies and the itchies. Simply put, if a patients eyes burn, the diagnosis is dry eye; if they itch, its allergy.
Be aware that semantics can confound the diagnosis. One patient may describe burning as itching and vice versa. This stems from the misconception that wanting to rub the eye means the eye is itchy. Itchy eyes are the result of histamine release, caused by allergen-induced degranulation of mast cells. The desire to rub ones eyes, however, can also be a response to dryness, as rubbing can increase reflex tearing and meibomian gland secretions, helping to temporarily relieve ocular discomfort.
It is known that the tear film deficiencies that are characteristic of dry eye can expose the eye to more allergens than normal, thereby eliciting allergic signs and symptoms.
This confusion has resulted in many years of misdiagnoses, even though dry eye and allergy tend to affect different age groups, occur in different seasons, and have different causes, signs and symptoms. The combination of the two conditions does not imply the existence of an entirely new ailment, but rather these separate conditions require individualized treatment.
Treatment
Once a patient learns about his or her condition and its associated causes, he or she can try to avoid situations that will exacerbate discomfort. For example, dry eye patients may choose to avoid prolonged computer use and should minimize exposure to dry, sandy environments. Patients with allergy may have to avoid mowing the lawn and hugging the family cat.
Complete avoidance is often unreasonable or impossible; however, several pharmaceuticals can provide relief.
Artificial tears, such as Systane (Alcon), are often used as a first-line defense against dry eye. Through a pH-dependant polymerization of the gelling agent hydroxyl-propyl guar (HP-guar), Systane coats the ocular surface, allowing for tear retention and epithelial self-repair. Optive (Allergan) is a recently released artificial tear that contains two standard demulcents (lubricants): glycerin and carboxymethylcellulose (CMC).
There is currently only one prescription drug for dry eye, Restasis (cyclosporine ophthalmic emulsion, Allergan), which incorporates cyclosporine A, a partial immunomodulator. The product is indicated specifically for aqueous deficient dry eye. Though it only has seen efficacy in 17% of patients, data suggest the effects of Restasis are improved when a tear substitute is used concomitantly.13 Various other non-prescription treatment and management options are available to dry eye patients, ranging from punctal occlusion or cauterization to ingestion of fish oil capsules, tea tree oil or omega-3 fatty acids.
Ocular allergy treatments include antihistamines, mast cell stabilizers and combination antihistamine/mast cell stabilizer drugs. Systemic antihistamines are known to cause ocular dryness, which is counterproductive when treating patients with allergic conjunctivitis or allergy/dry eye.14 Although probioticsspecifically, members of the genus Lactobacillus-have been suggested as possible remedies for allergy, to date, clinically significant reductions in both allergy signs and symptoms have only been described with any degreee of consistency for atopic eczema.15-16
Topical antihistamine/mast cell stabilizers are the preferred treatment option because they address the release of histamine from the mast cells and work to prevent further mast cell degranulation without causing ocular dryness.
 Pataday (olopatadine hydrochloride 0.2%, Alcon) is a recently introduced once-daily formulation of the olopatadine molecule. The once-daily dosing regimen is a long-awaited advancement in the treatment of ocular allergy. Contact lens wearers can instill the solution 10 minutes prior to lens insertion.
Pataday (olopatadine hydrochloride 0.2%, Alcon) is a recently introduced once-daily formulation of the olopatadine molecule. The once-daily dosing regimen is a long-awaited advancement in the treatment of ocular allergy. Contact lens wearers can instill the solution 10 minutes prior to lens insertion.
 Elestat (epinastine hydrochloride 0.05%, Allergan) is a prescription H1 receptor antagonist/mast cell stabilizer, indicated for twice-daily dosing. Its antihistaminic capabilities reduce ocular itching, and its effects can for last up to 12 hours.
Elestat (epinastine hydrochloride 0.05%, Allergan) is a prescription H1 receptor antagonist/mast cell stabilizer, indicated for twice-daily dosing. Its antihistaminic capabilities reduce ocular itching, and its effects can for last up to 12 hours.
 Optivar (azelastine hydrochloride 0.05%, MedPointe) is another prescription H1-receptor antagonist/mast cell stabilizer that is indicated for twice-daily dosing. It also has been shown to decrease the activity of other allergic mediators, such as leukotrienes.
Optivar (azelastine hydrochloride 0.05%, MedPointe) is another prescription H1-receptor antagonist/mast cell stabilizer that is indicated for twice-daily dosing. It also has been shown to decrease the activity of other allergic mediators, such as leukotrienes.
 Zaditor (ketotifen fumarate 0.035%, Novartis) has also been recently released over-the-counter, providing another
Zaditor (ketotifen fumarate 0.035%, Novartis) has also been recently released over-the-counter, providing another
treatment option for allergy sufferers. It does not contain vasoconstrictors, lasts for up to 12 hours, and is the same formulation that has previously only been available with a prescription.
 Alaway (ketotifen fumarate 0.025%, Bausch & Lomb). Like Zaditor, this is another brand of ketotifen which is now available over- the-counter.
Alaway (ketotifen fumarate 0.025%, Bausch & Lomb). Like Zaditor, this is another brand of ketotifen which is now available over- the-counter.
For those patients who experience concurrent dry eye and signs and symptoms of allergic conjunctivitis, combining a tear substitute with an antihistamine/mast cell stabilizer can concentrate the tear film while minimizing allergic discomfort.
The only similarities between dry eye and allergic conjunctivitis are that they both affect the eyes, have environmental components, produce redness and tearing, and that patients find both conditions annoying. Therefore, one may believe that differential diagnosis ought to be simple.
Start by obtaining a detailed patient history to determine the possible causes of the signs and symptoms, and perform a slit lamp exam. If a patient complains of burning, gritty-feeling eyesespecially if the individual is older or spends a lot of time performing high-intensity visual tasksthen it is probably a form of dry eye. If an individual complains of itchinessespecially after exposure to an allergenthen the patient is most likely experiencing allergic conjunctivitis. Avoiding the environmental offender along with proper therapy enhances quality of life for both dry eye and allergy patients.
Dr. Abelson, an associate clinical professor of ophthalmology at
ophthalmic pharmaceuticals. Ms. Lilyestrom is a medical writer at Ophthalmic Research Associates in
1. Abelson MB, Allansmith MR. Histamine in the eye. In: Silverstein A, OConnor G, eds. Immunology and Immunopathology of the Eye.
2. Abelson MB, Udell IJ. H2-receptors in the human ocular surface. Arch Ophthalmol 1981 Feb;99(2):302-4.
3. Abelson MB, Smith L, Chapin M. Ocular allergic disease: Mechanisms, disease sub-types, treatment. Ocul Surf 2003 Jul;1(3):127-49.
4. Millar TJ, Mudgil P. The effect of human meibomian lipids and tear proteins on evaporation rate under controlled conditions. IOVS 2007;48: ARVO E-Abstract 431.
5. Riley C, Young G, Chalmers R. Prevalence of ocular surface symptoms, signs, and uncomfortable hours of wear in contact lens wearers: The effect of refitting with daily-wear silicone hydrogel lenses (senofilcon a). Eye Contact Lens 2006 Dec;32(6):281-6.
6. Ousler GW, Workman DA, Torkildsen GL. An open-label, investigator-masked, crossover study of the ocular drying effects of two antihistamines, topical epinastine and systemic loratadine, in adult volunteers with seasonal allergic conjunctivitis. Clin Ther 2007 Apr;29(4):611-6.
7. Brewitt H, Sistani F. Dry eye disease: The scale of the problem. Surv Ophthalmol 2001 Mar;45:199-202.
8. Van den Biggelaar AHJ, van Ree R, Rodrigues LC, et al. Decreased atopy in children infected with Schistosoma haematobium: a role for parasite-induced interleukin-10. The Lancet 2000 Nov;356(9243):1723-7.
9. Duramad P, Harley K, Lipsett M, et al. Early environmental exposures and intracellular Th1/Th2 cytokine profiles in 24-month-old children living in an agricultural area. Environ Health Perspect 2006 Dec;114(12):1916-22.
10. Eder W, Klimecki W, Yu L, et al. Association between exposure to farming, allergies and genetic variation in CARD4/NOD1. Allergy 2006 Sep;61(9):1117-24.
11. Grant R, Bowen S,
12. Viinanen A, Munhbayarlah S, Zevgee T, et al. The protective effect of rural living against atopy in
13. Sall KN, Cohen SM,
14. Ousler GW, Wilcox KA, Gupta G, et al. An evaluation of the ocular drying effects of 2 systemic antihistamines: loratadine and cetirizine hydrochlorids. Ann Allergy Asthma Immunol 2004 Nov;93(5):460-4.
15. Kalliomki M, Salminen S, Arvilommi H, et al. Probiotics in primary prevention atopic disease: a randomized placebo-controlled trial. Lancet 2001 Apr;357(9262):1076-9.
16. Xiao JZ, Kondo S, Yanagisawa N, et al. Effect of probiotic Bifidobacterium longum BBS36 in relieving clinical symptoms and modulating plasma cytokine levels of Japanese cedar pollinosis during the pollen season. A randomized double-blind, placebo-controlled trial. J Investig Allergol Clin Immunol 2006;16(2):86-93.

