Colleagues have told me that irrigation of the lacrimal system is too complicated, too messy and too invasive for them to include as a routine service for their patients. But, when I look at this procedure, I see a simple and efficient way to relieve a variety of patient complaints. Hardly a week goes by that I don’t perform irrigation, and patients are almost always pleased with the process and its results.
Get Your Ducts in a Row
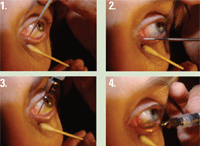
1. Insert dilator into vertical portion of duct. 2. Continue dilation to horizontal portion of duct by turning dilator 90°. 3. Insert irrigating canula into vertical portion of duct. 4. Rotate canula 90° to insert into horizontal portion of duct.
A brief review of the lacrimal anatomy will help with accurate diagnosis and proper irrigation technique. The puncta open to a vertically oriented shaft of the tear duct.
From there, the duct turns horizontally and the superior and inferior canaliculae join to form the common duct.1 I have found significant variability in the anatomy of these anterior structures. The puncta range from a pinpoint in diameter to several tenths of a millimeter in size. Likewise, the canaliculuae can show great variation in size.
When performing irrigation, it is also wise to note the variability of the “elbow” in the duct. The turn from the vertical to the horizontal aspect can be anything from a sharp corner to a gradual bend. Your ability to evaluate the anatomical uniqueness of each patient will, in part, determine the ease of performing irrigation.
Lastly, the common duct empties into the middle meatus of the sinuses, behind the nose.1 This explains why performing irrigation with the patient’s head tilted forward yields drainage through the nose, while irrigation with the head tipped back leads to drainage down the throat.
Indications for Irrigation
Lacrimal irrigation is performed to improve flow through the tear ducts. The vast majority of patients who require irrigation fall into one of three categories:
• Canalicular obstruction. Although anyone can present with this condition, it most often affects middle-aged individuals. They will complain of a sudden onset of excessive tearing in one eye. Tearing will be painless and their eyes generally appear white.
Patients with canalicular obstruction have developed either a plug of mucous or a dacryolith (small stone) in the tear ducts. Canalicular or punctal stenosis also fits into this category. The majority of these patients are easily irrigated. But, large stones require surgical intervention in the form of dacryocystorhinostomy (DCR).
Patients who produce stones often require irrigation every 12 to 18 months, because these formations tend to naturally recur. And, because a small dacryolith will likely grow larger over time, I encourage these patients to return for irrigation yearly––or at least to return as early as possible after the onset of symptoms.
• Removal of intracanalicular (punctal) plug. This is an iatrogenic condition. If lacrimal plugs are inserted into the ducts and lead to excessive tearing, then they generally should be removed. Most intracanalicular plugs are readily removed with gentle irrigation.

In rare instances, patients are allergic to plug materials (which is another good reason to remove them). In such cases, itching in the medal canthal area starts after two to three days after implantation.
• Canaliculitis. There is some controversy in irrigating a patient with canaliculitis. While I have successfully irrigated many patients who presented with this painful condition, extreme care must be taken.
First, the correct diagnosis must be made. It is critical to remember that dacryocystitis should not be irrigated.2 Dacryocystitis involves swelling and pain nasal and inferior to the orbit, with an elevated, tender mass under the skin.2 It is usually treated with oral antibiotics. Remember, if you’re uncertain about the diagnosis, always refer the patient to a specialist.
Canaliculitis, on the other hand, presents as tenderness in the inner canthal area, with the classic “pouting punctum.” Rolling a finger over the top of the tear duct (temporally, toward the punctum) expresses a small amount of mucopurulent discharge at the punctum. This is most often seen at the inferior punctum.2
Pathogens most likely to cause canaliculitis include species of Staph., Strep. and Actinomyces.3 Once you have confirmed that a patient has canaliculitis, you can perform a careful irrigation.2
Performing Irrigation
Unless the patient has unusual tear duct anatomy, I almost invariably perform dilation and irrigation without the slit lamp. This allows for unhindered access to the lids. Irrigate using the largest canula that comfortably fits through the punctum. Sizes range from 27-gauge to 19-gauge.
If the punctum is too small to easily insert the smallest canula in your instrument tray, dilation of the punctum is necessary. Often, the smallest dilator is the best. When dilating, a gentle twisting of the dilator keeps the tissue from sticking to the instrument, and I have found this technique to be much less irritating to the patient.
If I expect to dilate or irrigate in a more aggressive way, I’ll also apply a topical anesthetic to the punctum. A large or easily dilated punctum (usually seen in older patients) can be comfortably irrigated without an anesthetic.
Generally, I don’t apply anesthetic to the punctum when performing dilation or irrigation. A gentle approach can be well tolerated by patients. If the punctum is very small, and I expect a more vigorous dilation or irrigation, topical proparacaine can be applied. I use a cotton-tipped applicator doused with anesthetic and apply it twice for 20 seconds. If done carefully, both the upper and lower puncta can be numbed simultaneously.
Access to the puncta is much better when a patient reclines his or her head backwards. This, however, forces saline to flow back to the throat, and the patient may gag slightly. Leaning the patient’s head forward causes saline to drip from the nose. That also can be annoying to the patient. I opt for best punctal access, and therefore have the patient lean back. In either position, patients appreciate a towel to catch stray saline.
Proper technique requires respecting the anatomy of the lacrimal system. A dilator or syringe is inserted into the punctum and rotated temporally (figures 1-4). If the open end of the syringe is impinging on the wall of the duct, you won’t be able to irrigate at all. So, be sure that the syringe is directed down the middle of the duct’s lumen.
At least 3cc of saline should be emptied into the lacrimal system to establish good flow. I use a 3cc syringe and empty all of it. If I feel resistance, I continue to irrigate with a second or third syringe until I can feel a smooth and easy flow.
With idiopathic plugs or intracanalicular plug removal, irrigation should be painless. Some irritation may be generated by dilating or inserting a canula, but patients usually tolerate this without much complaint.
Patients with canaliculitis, however, will be very sensitive to the canula and saline flow due to the rawness of the tissue caused by the bacterial infection. If you choose to irrigate these patients, topical anesthetic must be applied beyond the punctum to the duct. Furthermore, you may have to introduce anesthetic through the syringe and canula very gradually. Typically, 0.1cc to 0.2cc proparacaine can be placed at increasing depths until the patient can comfortably tolerate saline irrigation. This process is irritating, and will produce a burning sensation as it is performed. Do this only if you are confident and can keep the patient focused on the goal of improved comfort afterwards. Also, with these patients, I irrigate with an anti-bacterial once I have established good lacrimal flow.
Lacrimal irrigation can be a great benefit to patients, a worthy addition to optometric practice and a chance to advance your clinical skills. If performed properly and on the right patients, lacrimal irrigation can become as routine as any other optometric procedure.
Dr. Jensen is in private practice in the Seattle area and is majority partner in Dry Eye University, LLC, an eye care education corporation. Additionally, he has a minority interest in Optspace.com. He thanks Alan Homestead, O.D., for technical contributions to this article.
1. Wolff E. Anatomy of the Eye and Orbit, 7th ed. Philadelphia: W.B. Saunders Co.; 1981:227-8.
2. Kunimoto DY. The Wills Eye Manual, 4th ed. Philadelphia: Lippincott Williams & Wilkins; 2004:116-7.
3. Zaldívar RA, Bradley EA. Primary canaliculitis. Ophthal Plast Reconstr Surg. 2009 Nov-Dec;25(6):481-4.
4. Kushner BJ. Congenital nasolacrimal system obstruction.
Arch Ophthalmol. 1982 Apr;100(4):597-600.

