 Q: A patient contacted me regarding his keratoconus and his inability to wear contact lenses. I attempted several different lens designs and materials, and he has seen several other practitioners, who have also failed. His corneal specialist recommended Intacs (Addition Technology) or deep anterior lamellar keratoplasty (DALK). What are some advantages and disadvantages of each procedure?
Q: A patient contacted me regarding his keratoconus and his inability to wear contact lenses. I attempted several different lens designs and materials, and he has seen several other practitioners, who have also failed. His corneal specialist recommended Intacs (Addition Technology) or deep anterior lamellar keratoplasty (DALK). What are some advantages and disadvantages of each procedure?
A: If the patient is a candidate for Intacs, it should be considered first, says Brian S. Boxer Wachler, M.D., of Boxer Wachler Vision Institute in
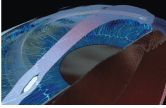
Consider Intacs as a possible solution for a patient with mild keratoconus.
Courtesy: Brian S. Boxer Wachler, M.D.
A patients candidacy for Intacs, says Dr. Boxer Wachler, depends on the stage of keratoconus he or she is in. If advanced, Intacs will likely be contraindicated.1 Those patients would benefit more from a more extensive corneal surgery, such as DALK, Dr. Boxer Wachler says. If someone is very advancedsay, their K values are near the 70.00D rangetheyre almost too far gone; Intacs wouldnt improve the corneal topography enough.
DALK has been proven effective in cases of keratoconus; however, patients run the risk of rejection, graft failure or infection.2-4 Likewise, six out of 20 eyes in a small study of Intacs for advanced keratoconus experienced ring exposure due to corneal thinning.5
But, if the patient proves a viable candidate for Intacs based on the level of his or her keratoconus, Dr. Boxer Wachler recommends opting for this procedure over DALK. Intacs have saved many patients from having to undergo fairly invasive eye surgeries, he says. The results are positive and get patients to their end goal without having to take a more involved path. Research demonstrates better results and higher success rates with Intacs in patients with lower K values and mild to moderate keratoconus.1,6
The insertion of Intacs, says Dr. Boxer Wachler, is minimally invasive. Its only about a 10-minute procedure. Patients topographies are improved by the next day. Also, he adds, risk of infection is minimized by the small incision size and short procedure duration.
But, what happens in cases of progressive keratoconus? We can actually combine two procedures: Intacs and corneal cross-linking with riboflavin (C3-R), Dr. Boxer Wachler says. In a study of Intacs alone vs. Intacs with C3-R, we found that we get better results when we combine the procedures.7
If DALK is the indicated procedure, however, expect a longerand perhaps significantly more complicated follow-up period than you can expect with Intacs.2-4 It takes about three months for the cornea to heal after DALK, says Dr. Boxer Wachler. Patients can go about their normal daily routine, but they cant be fitted for lenses. The corneal surface is still changing during this period of time.
The bottom line: Discuss all options with your patients. In the past, patients with keratoconus were told by their eye doctors that a corneal transplant and gas-permeable contacts were their only options, Dr. Boxer Wachler says. Doctors who [still] tell their patients that those are the only two options are living in the Dark Ages of keratoconus management. Today, we have many different ways to help these patients.
Dr. Boxer Wachler recently published a comprehensive book about keratoconus that covers topics from contacts to Intacs: Modern Management of Keratoconus. The book is available, along with more information about Intacs, C3-R, and other options, at his website: www.keratoconusinserts.com.
1. Ali JL, Shabayek MH, Belda JI, et al. Analysis of results related to good and bad outcomes of Intacs implantation for keratoconus correction. J Cataract Refract Surg 2006 May;32(5):756-61.
2. Fontana L, Parente G, Tassinari G. Clinical outcomes after deep anterior lamellar keratoplasty using the big-bubble technique in patients with keratoconus. Am J Ophthalmol 2007 Jan;143(1):117-24.
3. Eberwein P, Auw-Hdrich C, Birnbaum F, et al. Corneal melting after cross-linking and deep lamellar keratoplasty in a keratoconus patient. Klin Monatsbl Augenheilkd 2008 Jan;225(1):96-8.
4. Kanavi MR,
5. Kanellopoulos AJ, Pe LH, Perry HD, Donnenfeld ED. Modified intracorneal ring segment implantations (Intacs) for the management of moderate to advanced keratoconus. Cornea 2006 Jan;25(1):29-33.
6. Levinger S, Pokroy R. Keratoconus managed with Intacs: one year results. Arch Ophthalmol 2005 Oct;123(10):1308-14.
7. Chan CC, Sharma M, Wachler BS. Effect of inferior-segment Intacs with and without C3-R on keratoconus. J Cataract Refract Surg 2007 Jan;33(1):75-80.

