 |
A 23-year-old white male presented as a new patient for a contact lens examination in April. He complained of blur at distance and near, and said that everything runs together when reading.
The patient also complained of headaches in the morning upon awakening. He attributed these to sinusitis, for which he saw a primary-care physician a few weeks earlier. He was taking Claritin (loratadine, Schering-Plough) p.r.n. for allergic sinusitis.
He had his eyes checked by his regular optometrist three months earlier. He reported at that time that his contact lens prescription had changed a lot.
Diagnostic Data
Entering visual acuity was 20/40 O.D and O.S. through his contact lenses. He wore Acuvue Advance (Vistakon) lenses with an 8.7mm base curve and a -3.75D correction O.U. He wore his contact lenses on a daily wear basis, and the present contact lenses were four to five days old.
Pupils were equal, round and reactive to light and accommodation with no afferent pupillary defect. Extraocular motilities were full in all diagnostic positions of gaze.
A contact lens over-refraction of plano -0.75 x 180 O.D. and plano -0.75 x 005 O.S. yielded visual acuity of 20/25 O.D. and 20/40 O.S. Pinhole test did not improve acuity in either eye.
A slit lamp examination of the anterior segment was unremarkable. His corneas were clear, and the endothelium demonstrated no pleomorphic changes or polymegathism. The contact lenses were mildly coated with mucoid debris.
Upon removal of the contact lenses, applanation tensions were 16mm Hg O.D. and 15mm Hg O.S. at 4 p.m. Pachymetry was not performed.
Prior to dilation, I performed the red cap test, primarily due to the slightly reduced acuity and history of a rather sudden pronounced change in vision. The patient reported a 50% red desaturation in the left eye. A recheck of his pupils confirmed the absence of any pupillary abnormality.
Based on the red desaturation O.S., I performed threshold visual fields out to 70 degrees O.U. (Normally, when the initial examination reveals glaucomatous or suspect optic nerves, I schedule fields at a later date, simply for office flow reasons.) Visual fields were completely normal in the central 30 degrees O.U. but demonstrated mild defects at 70 degrees O.U. that did not cross either neurological hemi-meridian.
Through dilated pupils, his crystalline lenses were clear O.U. Stereoscopic examination of the optic nerves demonstrated cup-to-disc ratios of 0.50 x 0.50 O.D. and 0.60 x 0.70 O.S. Close examination of the neuroretinal rims showed diffuse thinning of the temporal rims with adjacent zone beta peripapillary atrophy; this was greater O.S. than O.D.
Furthermore, rim character lacked a plush and well-perfused appearance, but there was no frank pallor in either nerve. Perioptic vasculature was of normal caliber and free from hypertensive or atherosclerotic changes that often accompany non-plush neuroretinal rims. Spontaneous venous pulsations were present. The patients macular and peripheral retinal examinations were unremarkable O.U.
My assessment at this point: subjectively decreased visual acuity that was greater O.S. than O.D., and a normotensive glaucoma suspect, again greater O.S. than O.D.
Discussion
Several findings didnt add up, which aroused my suspicion. Foremost is a significant change in visual acuity in a short period. The change in vision is not unusual in itself, especially in a contact lens wearer. Various corneal issues can readily change vision in contact lens wearers, especially if there is evidence of overwear syndrome. But, the patient denied overwear, and his corneal evaluations were normal.
I considered the possibility of diabetic fluctuations. Given the absence of retinal findings, however, visual acuity should still be close to 20/20, even if there are large swings in refractive error. This, too, did not add up.
The key finding in his initial evaluation was the color desaturation in his left eye. In the absence of media opacities and macular asymmetry, the presence of color desaturation in one eye is a strong predictor of optic nerve dysfunction. But often in cases of optic nerve disease, the presence of color desaturation coincides with an afferent pupillary defect and/or a visual field defect, such as a cecocentral scotoma. Neither finding was present. Then again, red desaturation is not usually found in cases of normotensive glaucoma.
I discussed my findings with the patient at length. I felt we had two issues to rectify: to determine the presence or absence of normotensive glaucoma, which may or may not explain the reduced acuity O.S., and to reassess visual acuity in both eyes after the patient discontinues contact lens wear for several days.
But, the nagging question about the red desaturation remained: Was there compromise to the optic nerve on the left side?
We scheduled an MRI of the brain, orbits and optic nerves to rule out occult disease. The MRI order specified transient visual blur O.S. and red desaturation O.S. Rule out optic nerve disease. The MRI was scheduled for three days later. We also scheduled another refraction, visual field examination, pachymetry and repeat IOP check in two weeks.
 |
|
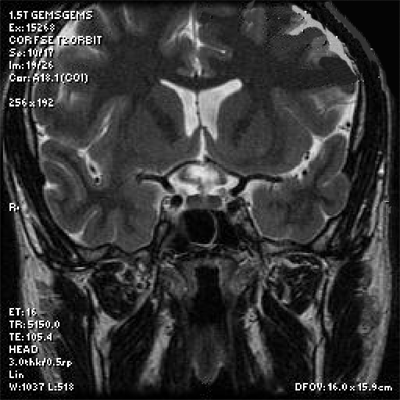
MRI provides a coronal view of the lesion (white, ovoid enhancement below the ventricles). Note its proximity to the optic chiasm. |
The diagnosis of normal-tension glaucoma is straightforward in most cases but not always. Many non-ophthalmic conditions may result in structural or functional changes of the optic nerves. In my experience, normal-tension glaucoma is seen more commonly in patients who have thin corneas and significant vascular issues that result in decreased peripheral perfusion (such as cardiac dysrythmias, peripheral vascular disease, diabetes, atherosclerosis, hypertension, sleep apnea and congestive heart failure to name but a few), and it generally occurs in older patients. Normal-tension glaucoma in a 23-year-old patient should be a diagnosis of exclusion, especially in an overtly healthy patient such as this.
 |
|
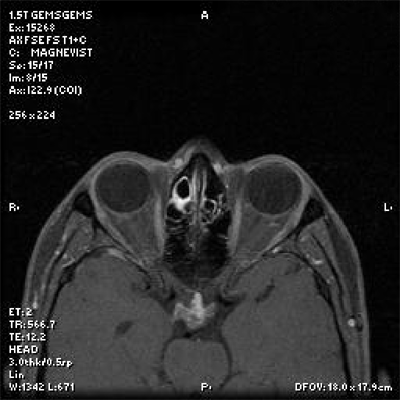
Axial view of the lesion taken at a level slightly above the pituitary gland. |
Do not overutilize neuroimaging in the workup of a normotensive glaucoma suspect, as the yield is low.
On the other hand, the cost of underutilization can be severe for the patient. One prospective observational study of 62 normal-tension glaucoma patients and 70 primary open-angle glaucoma patients found that 6.5% of the normal-tension glaucoma patients had clinically relevant intracranial compressive lesions compared with no primary open-angle glaucoma patients.1 Use your clinical intuition and level of suspicion to guide your imaging utilization.
As for the patient in this case, one week after imaging, he underwent neurosurgery to remove the mass. He tolerated the procedure well, and is currently recovering.
1. Ahmed II, Feldman F, Kucharczyk W, Trope GE. Neuroradiologic screening in normal-pressure glaucoma: study results and literature review. J Glaucoma 2002 Aug;11(4):279-86.

