
As the American population continues to age, the number of elderly patients who live in assisted-living facilities and nursing homes is growing rapidly. The current number of nursing home residentsabout 1.5 millionis expected to double by the year 2030.1
Many of these people used to be your patients and received their refractive and ocular health care in a traditional eye-care office setting. Some of them still do.
But, because of the expense and the coordination required to schedule an appointment, as well as to arrange transportation outside of their new living situation, many (if not most) of these patients are unable to receive their eye care in a traditional office setting.
Indeed, nursing home residents in the United States have higher rates of vision impairmentup to 15 times higher than corresponding rates of older adults who arent in nursing homes.2 Unfortunately, more than half of nursing home residents dont receive eye care even though the facility has contracted for eye-care services.2 As few as one in eight nursing homes have optometric services on-site.3
Another underlying reason for higher rates of vision impairment in nursing homes: Staff, health-care providers and family members dont believe that nursing home residents may benefit from vision care because of residents cognitive impairment and/or physical frailty.
This is not true, of course. Treating uncorrected refractive error in nursing home residents improves quality of life and reduces symptoms of depression.2 This as an opportunity for optometrists to help a large and growing underserved population. How you approach a nursing home or assisted-living facility about providing care for its residents may be different for every facility and setting, but the bottom line is that these patients need to be seen in their facility in order to receive the regular and routine care that they need and deserve.
Ive been providing on-site nursing home care for more than a decade, and its been a very rewarding (both emotionally and financially) part of my practice life.
Tools of the Trade This is a basic set of equipment youll need to bring to a nursing home: Wall-mounted acuity charts (Snellen and Tumbling E, or other alternate chart) Lensmeter Handheld slit lamp (a true slit lamp, not just an adapter for a battery handle) Binocular indirect ophthalmoscope and condensing lenses Direct ophthalmoscope Retinoscope and lenses (preferably a lens rack in both plus and minus powers) Epilation forceps Dilating agents Anesthetic agent Trial lenses Tonometer (handheld Goldmann or Tono-Pen) Gonioscopy lens and cushioning agent Pachymeter Basic hand tools for frame adjustments/dispensing/repairs Nose pads and screws Retinoscopy is the primary refractive measurement tool for many patients.

Administration and Billing
I currently provide care one day a week at only one nursing home. But, its a very large home, with almost 800 beds, and I provide care to about 80% of these patients. I have the advantage of providing these services through a company (HealthDrive, based in
While the administrative requirements of providing on-site nursing home care are different from those in an optometric office, they dont have to be overwhelming. Patients must indicate that they want you to be their eye-care provider in the facility. Most facilities have a social worker who helps coordinate this arrangement.
Once patients have indicated that they would like you to provide services to them in their facility, you need to gather the patients third-party information and other payment information, just as you would in your own office.
Billing for services rendered in a long-term care facility is a bit different from doing so in your office. There are separate evaluation and management codes that pertain to care provided in these settings, as well as a different location that needs to be indicated on the insurance claim. However, you bill the ophthalmic codes (920x4, 920x2, 92015, 92225, 92020, etc.) as you would bill them in your office.
Many of these patients need to be seen several times per year. Between epilating misdirected lashes to ease the symptoms of trichiasis, to inserting punctal plugs for a dry eye patient, to regular follow-up visits for glaucoma patients, youll find yourself seeing these patients frequently for procedures and visits which, when properly documented and billed for, result in a nice financial return.
Youll also have minimal overhead, other than the initial financial outlay for the
necessary equipment and supplies, which makes this a fairly high net business opportunity.
Of course, before you schedule your first day of patient appointments, be sure to research the billing requirements in your area to avoid a longer-than-necessary pay cycle for services rendered. Your state may also have specific Medicaid requirements for care rendered in a facility vs. a typical office setting, so be sure to follow those requirements at all times.

Nursing home exams are different from those that you provide in your office. While some patients can give you a comprehensive health history, many can not.
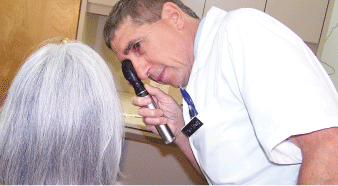
Start the exam by evaluating visual acuity, pupils, confrontation visual fields, ocular alignment and tracking. Next, measure intraocular pressure and examine the anterior segment.
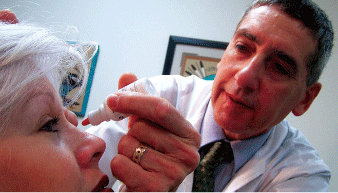
Then, dilate the patient. Perform refractive testing using retinoscopy after the patient is dilated.
A Different Kind of Patient
The vast majority of these patients suffer from one or more ocular pathologies. Rarely does a patient have a normal exam. Chronic conditions, such as diabetes and hypertension, need to be monitored, but most of these patients have a specific problem that needs to be addressed. Blurred vision, ocular discomfort, epiphora and ocular irritation and/or redness are some of the most frequent presenting symptoms and patient complaints.
Because of both the setting and the type of patients that youll see, nursing home exams tend to be different from those that you provide in your office. Much of the history comes from the patients health record. While some patients are quite capable of giving you a comprehensive health history, many are not.
Knowing how to interpret the facilitys health-care chart is a must. Most facilities follow a similar (if not identical) documentation protocol with easy-to-use tabs for different sections of the record.
The master problem list is a good place to start your chart review and history. There youll find the patients chronic/systemic issues, as well as his or her ocular health-care issues. The patients medications and dosing schedule will also be clearly listed.
Lastly, there will be a section in the record that contains any past consultations; your notes and reports should be stored in this section of the chart at the conclusion of your visit.
Because nursing home patients often have ocular pathologies, I use a very problem-focused approach to caring for them. (See Tools of the Trade, above.) I start the exam by evaluating visual acuity, pupils, confrontation visual fields, ocular alignment and tracking. Next, I measure intraocular pressure and examine the anterior segment.
Then I dilate the patient. I dont usually perform refractive testing until after the patient is dilated. Retinoscopy is my primary refractive measurement tool for many of these patients and I get much better results after dilation. I then perform binocular indirect ophthalmoscopy and use the hand-held slit lamp and 78D condensing lens to carefully evaluate the fundus and optic nerve. (I find that I frequently get a better view with a condensing lens than with a direct ophthalmoscope due to media opacities.)
Document carefully. Keep in mind that the nursing home staff will need to read and understand your findings.
Document Clearly

When documenting your examination findings, be as complete as possible. Remember that you and your staff wont be the only ones looking at your documentation for information. The nursing home staff and attending physicians will all be relying on your report to tell them what you found and what youre planning to do for the patient.
If you use abbreviations, be sure that they are abbreviations commonly used throughout health care, not just among eye-care providers. Your office staff may know that DM w/out DR O.D., mild BDR O.S. means that the patient has diabetes with no retinopathy in the right eye and mild background retinopathy in the left eyebut this may make no sense at all to the nursing home staff.
The same goes for medications that you order. Spell out the entire medication name, the dosage and the frequency, as well as the indication. Most facilities require an indication for every medication that they dose, so be sure to clearly indicate why youre prescribing a medication.
If you use an electronic health record (EHR) in your primary practice, do your best to use the same EHR at the nursing home. Youll be more comfortable documenting your encounters, as well as coding and billing, if you can use the same system as in your primary patient care setting.
If you cannot use your EHR in the facility or if you use pen and paper, choose an exam form that allows you to document as much as possible on a single page. While you might have to squeeze everything on the page (since these patients frequently have several ophthalmic issues to address), it greatly improves your ability to keep both the facility chart and your chart in sync.
Communication is Essential
At a minimum, include a summary letter in the record. Better yet, put a copy of your exam document in the chart. This aids compliance with any internal or external documentation/ examination requirements. More importantly, it improves communication between you and the facility staff. You can photocopy your handwritten documentation, use a multi-part carbon form or, if youre using an EHR, provide a printed copy of the EHR summary report.
Communication with the patient, the patients family and the facility staff is of utmost importance. While a typical patient in your office is usually self-sufficient, patients in a long-term care facility rarely provide much, if any, of their own care. You must ensure that the facility staff understands and carries out your orders for tasks as simple as blepharitis treatment.
So, be sure to not only document your recommended treatments on your own encounter form (and leave a copy at the facility), but also fill out any internal order documentation forms that the facility uses. Each facility has its own way of ensuring that a consulting doctors orders are recognized, understood and followed.
The payment for medications varies by the type of facility and even from one facility to another within the same type. When prescribing medications, know whats included in the formularies for the facility and for your state Medicaid program. If you usually use one prostaglandin analog but the formulary doesnt include it, youll have to answer many requests for medication changes or substitutions.
So, try to keep treatments simple and use as many generic medications as possible to minimize these issues. But, when a generic wont do, be ready to defend your choice and stick to your guns when necessary.
Theres a lot of talk about the oversupply of optometrists. Theres no oversupply of them in nursing homes. So, I encourage you to reach out to provide care in the facilities near you. Not only will it keep you busy, but the patients will really appreciate your effortsand youll appreciate the patients, too.
Dr. Warren spends each Tuesday at a nursing home facility and also operates a full-time private practice in Racine, Wisc.
1. Sahyoun NR, Pratt LA, Lentzner H, et al. The changing profile of nursing home residents: 1985-1997. Aging Trends 2001 Mar;(4):1-8.
2. Owsley C, McGwin G Jr, Scilley K, et al. Effect of refractive error correction on health-related quality of life and depression in older nursing home residents. Arch Ophthalmol 2007 Nov;125(11):1471-7.
3. Agency for Healthcare Research and Quality. Medical Expenditure Panel Survey. Nursing Home Component, file NHC-003. Available at: www.meps.ahrq.gov/mepsweb/data_stats/download_data/pufs/nhc01/nhc3cb.shtml (Accessed March 10, 2008).

