While a staple in the average diet, “fat” has long had negative connotations in society; however, not all types are bad. Omega-3 essential fatty acids (EFAs) are key constituents in human growth and function, particularly in the brain and cell membranes. Omega-6s, the other category of dominant essential fatty acids, also play a role in brain function, as well as skin and hair growth, metabolism and the reproductive system.
Humans must rely on food or supplements to meet their omega-3 and omega-6 fatty acid needs and learn to balance the two to prevent adverse effects. It’s up to practitioners to understand the differences in source, form, delivery and dosage to help patients select the best option.
Omega-3 Varieties
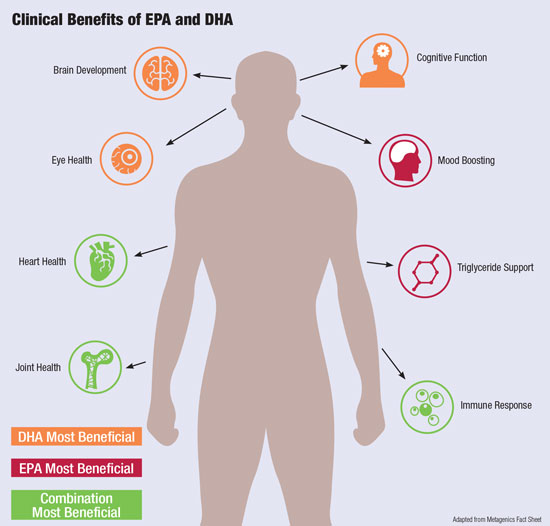
Two varieties of omega-3s exist: long chain and short chain. Long chain, polyunsaturated omega-3 fatty acids include eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), which can be found in cold-water oil fish like herring, mackerel, salmon, sardines, trout, bluefin and albacore tuna. As the most important and most bioactive of the EFAs, EPA and DHA are known to play vital roles in heart, circulatory, brain, mental and eye health, and are associated with anti-aging, longevity and good immune function.1 EPA and DHA may also be effective pharmacological anti-inflammatories; however, the specifics remain under debate.2 A recent study found that macrophages (a type of white blood cell) use DHA to produce maresins, which fight inflammation.4
What to Look for When Buying Fish Oil Supplements
|
The short chain omega-3 fatty acids include alpha linolenic acid (ALA) from plants (e.g., flax and chia seeds, walnuts and algae) and stearidonic acid (SDA) from plant-sourced oil (e.g., echium oil, black currant seed oil and genetically modified soybean oil). ALA is the primary source of omega-3 in the diet; both it and SDA must undergo a metabolic conversion to function in the body as EPA and DHA. The rate varies depending on enzymes and other factors such as genetic influences, gender, health status and quality of diet.
Types of omega-6 fatty acids include linoleic acid (LA), arachidonic acid (AA), gamma-linolenic acid (GLA) and dihomo-gamma-linolenic acid (DGLA). Rich sources of omega-6s include seeds and grains, sunflower, safflower and corn oils.
Balanced Fatty Acids
Investigators believe an imbalance between omega-3 and omega-6 levels leads to certain inflammatory and autoimmune diseases.3 While omega-6s are essential for certain body processes, they also produce inflammatory eicosanoids, initiate more blood vessel constriction and create more pain and mucus. If a patient has excessive omega-6 intake compared with omega-3 intake, the omega-6s can saturate enzyme activity and prevent the manufacturing of anti-inflammatory substances, even when omega-3 fatty acids are available.
Many Americans have an imbalance of omega-6 to omega-3 between 20:1 and 40:1—a healthy ratio is believed to be anywhere from 1:1 to 5:1.3 Thus, lowering omega-6, along with increasing omega-3, should be a consideration in the standard American diet.
How Much Do You Need?
Patients can achieve adequate intake of omega-3s either by eating fish, through supplementation or a combination of both. In 2002, the Institutes of Medicine set the dietary reference intakes (DRIs) for adults for adequate intake of ALA omega-3 at 1.6g a day for men and 1.1g per day for women.5 Subsequent recommendations made by the Academy of Nutrition and Dietetics in 2014 suggest all Americans include a non-fried fatty fish in their diet two or more times a week, providing at least 500mg of EPA and DHA per day.6
In clinical trials, dosages vary depending on the condition being studied. National health organizations recommend at least 1,000mg/day of EPA and DHA for support of cardiovascular and mental health. For interventions such as hypercholesterolemia and hypertriglyceridemia, the recommendations go up to 4g per day. The FDA has established a generally regarded as safe (GRAS) level of 3g of EPA and DHA per day.7
Balanced Fatty Acids
If obtaining omega-3s via food, the method of cooking fish is important, as omega-3 levels can be affected if the fish is cooked over high heat. Deep fried fish, for example, will have minimal amounts of omega-3 because the frying process transforms the polyunsaturated fatty acids into trans or saturated fatty acids. The fish’s diet also makes a difference in omega-3 availability. Wild fish eat algae, plankton and even other fish, all of which contribute to the total concentration of EPA and DHA. Farmed fish, however, typically eat grain and soy, which are high in omega-6s, thus leading to low omega-3s in oil from farmed fish.
Marine oil supplements are better absorbed when taken with a fat-containing snack such as eggs or nuts. Finding a high quality, pure and potent product is imperative, as is taking the appropriate amount. (See “What to Look for When Buying Fish Oil Supplements,” above.)
 |
The relative bioavailability of omega-3 fatty acids from different sources (e.g., fish, supplements or functional foods) and when consumed from different structural forms (i.e., triglyceride, ethyl ester, free fatty acid or phospholipid) is of considerable importance as well. A two-week study in 2010 showed the re-esterified triglyceride form to be more bioavailable than the ethyl ester form.8
Generally, plasma levels of EPA and DHA increase within hours of ingestion, but this is considered a poor biomarker of long-term omega-3 intake, especially when compared with red blood cell levels, which reflect a longer-term intake. Changes in the red blood cell membranes, by comparison, can take three to five months, thus requiring consistent dosing. Bioavailability can be increased if patients ingest their EPA/DHA supplements at or around mealtime rather than on an empty stomach, as absorption of fatty acids is enhanced by pancreatic enzyme (lipase) and bile salts.
What are its Effects?
- Cardiac Effects. Higher doses of fish oil result in a lower risk of death from cardiovascular disease and up to 62% lower risk of fatal heart attack.9 Additionally, the American Heart Association has concluded that omega-3s decrease arrhythmias, triglyceride levels, atherosclerotic plaque growth rate and blood pressure.
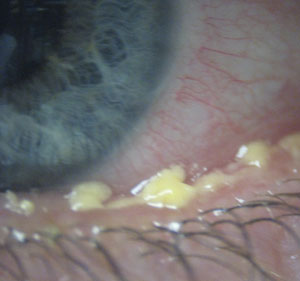
Omega-3 dietary supplements may improve OSDI, TBUT and meibum scores in patients with blepharitis. Photo: Christine W. Sindt, OD. - Prostate Cancer. A 2013 study suggests an increased prostate cancer risk among men with a high blood concentration of long-chain omega-3s who participated in the Selenium and Vitamin E Cancer Prevention Trial (SELECT); however, controversy over the study’s results exists.10,11 A separate study suggests EPA and DHA intakes may reduce the risk of total and advanced prostate cancer.12
- Blood Thinning. EPA and DHA doses greater than 3g per day may increase prothrombin time and risk of bleeding.5 The omega-3s may work by lowering thromboxane A2 supplies within the platelets and decrease clotting factor VII, so should not be recommended for those on warfarin or heparin.13 Supplementing isolated DHA without EPA, which inhibits platelet aggregation, can be considered if necessity arises.
- Pregnancy and Infants. DHA is known to play an essential role in maternal health and fetal development (i.e., brain, eyes, nerve and immune systems). Several studies have linked higher maternal intake of omega-3s with lower risk of child suboptimal verbal IQ, better visual function and long-term function of the visual parvocellular pathway in school-aged children.14,15 The FDA recommends that pregnant women avoid fish that contain high levels of mercury, particularly shark, swordfish, king mackerel and tilefish.15
- Memory. DHA stimulates the growth of new neurons in our brains, leading to improved memory by activating the production of brain-derived neurotrophic factor, a protein important for neuronal survival and long-term memory. Supplementation has been shown to support cognitive health with aging.8
- Dry Eye Syndrome. Omega-3 intake is a well-known method to lower the incidence of dry eye.16 Additionally, taking sea buckthorn oil containing omega-3 and omega-6 has been shown to attenuate tear film osmolarity and decrease redness and burning associated with dry eye.17 Omega-3s can block the gene expression of the inflammatory cytokines tumor necrosis factor alpha (TNF-α), interleukin-1 alpha (IL-1α) and leukin-1 beta (IL-1β). This can be helpful in the case of Sjögren’s syndrome, in which the lacrimal glands have increased TNF-α.
- Meibomian Gland Dysfunction (MGD) and Blepharitis. Omega-3 dietary supplementation for blepharitis and MGD may decrease the red blood cell and plasma ratios of omega-6 to omega-3 and improve overall ocular surface index (OSDI) score, tear break-up time (TBUT) and meibum score.18
- Macular Degeneration. Studies have suggested eating fish more than twice a week may cut risk of developing macular degeneration in half.19 Additionally, a diet low in trans- and unsaturated fat and rich in omega-3 fatty acids and olive oil may reduce the risk of age-related macular degeneration.20
- Combining Compounds. Carnitine is the delivery system for long-chain fatty acids. The less available carnitine, the fewer fatty acids get into the cell. A combination of acetyl-l-carnitine, omega-3 fatty acids and coenzyme Q-10 can improve visual functions, including visual field mean defect, visual acuity and foveal sensitivity in patients with early age-related macular degeneration. They also can improve fundus alterations by decreasing drusen.21
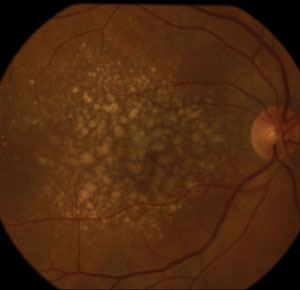
Omega-3 fatty acids, in combination with other dietary supplements, may reduce risk of AMD. Photo: Jay M. Haynie, OD. - Retinitis Pigmentosa. Patients with X-linked retinitis pigmentosa have low levels of DHA in red blood cells compared with normal sighted control subjects.22 DHA supplementation may correct a fatty acid deficiency and rod ERG functional loss in X-linked retinitis pigmentosa.23
- Glaucoma. A small study found that primary open-angle glaucoma patients have reduced blood levels of DHA and EPA compared with normal controls.24 EPA and DHA appear to modulate impaired systemic microcirculation, ocular blood flow and optic neuropathy associated with glaucoma.24
- Cataracts. The Nurses’ Health Study showed women with the highest EPA/DHA intake had 12% lower risk for cataract extraction.25 Those who had more than three servings of fish per week had a 19% lower risk.25
- Uveitis. In vivo EPA inhibits multiple inflammatory molecules. In animal models, oral EPA showed a decrease in leukocyte adhesion to retinal vessels, a decrease in leukocyte infiltration into the vitreous cavity along with a decrease in pro-inflammatory cytokines.26
Dr. Summerton is a certified nutrition specialist and a clinical nutritionist at the University of Miami. She serves as secretary and chair for the fellowship committee for the National Ocular Nutrition Society. She is also a member of the American College of Nutrition.
1. Swanson D, Block R, Mousa SA. Omega-3 fatty acids EPA and DHA: health benefits throughout life. Adv Nutr 2012 Jan;3(1):1-7.2. Calder PC. Omega-3 polyunsaturated fatty acids and inflammatory processes: nutrition or pharmacology? Br J Clin Pharmacol. 2013 Mar;75(3):645-62.
3. Simopoulos AP. The importance of the ratio of omega-6/omega-3 essential fatty acids. Biomed Pharmacother. 2002 Oct:56(8):365-79.
4. Dalli J, Zhu M, Vlasenko NA, et al. The novel 13S,14S-epoxy-maresin is converted by human macrophages to maresin 1 (maR1), inhibits leukotriene A4 hydrolase (LTA4H), and shifts macrophage phenotype. FASEB J. 2013 Jul;27(7):2573-83.
5. Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein and Amino Acids (Macronutrients). Washington, DC: The National Academies Press, 2005.
6. Vannice G, Rasmussen H. Position of the academy of nutrition and dietetics: dietary fatty acids for healthy adults. J Acad Nutr Diet. 2014 Jan;114(1):136-53.
7. US Food and Drug Administration. Substances affirmed as generally regarded as safe. Federal Register. 1997;62(108):30757-7.
8. Yurko-Mauro K, McCarthy D, Rom D, et al. Beneficial effects of docosahexaenoic acid on cognition in age-related cognitive decline. Alzheimers Dement. 2010 Nov;6(6):456-64.
9. de Goede J. Geleijnse JM, Boer J, et al. Marine (n-3) fatty acids, fish consumption, and the 10-year risk of fatal and nonfatal coronary heart disease in a large population of Dutch adults with low fish intake. J Nutr. 2010 May:140(5):1023-28.
10. Brasky TM, Darke AK, Song X, et al. Plasma phospholipid fatty acids and prostate cancer risk in the SELECT trial. J Natl Cancer Inst. 2013 Aug 7;105(15):1132-41.
11. Council for Responsible Nutrition. CRN Says New Study on Omega-3 Conclusions are Overblown. Available at: http://www.crnusa.org/CRNPR13-Omega3071113.html. Accessed: June 14, 2015.
12. Leitzmann MF, Stampfer MJ, Michaud DS, et al. Dietary intake of n-3 and n-6 fatty acids and the risk of prostate cancer. Am J Clin Nutr. 2004 Jul:80(1):204-16.
13. Salonen R, Nikkari T, Seppänen K, et al. Effect of omega-3 fatty acid supplementation on platelet aggregability and platelet produced thromboxane. Thromb Haemost. 1987 Jun 3:57(3):269-72.
14. Hibbeln JR, Davis JM, Sterr C, et al. Maternal seafood consumption in pregnancy and neurodevelopmental outcomes in childhood (ALSPAC study): an observational cohort study. Lancet. 2007 Mar 19;99(6A):44C-46C.
15. Jacques C, Levy E, Muckle G, et al. Long-term effects of prenatal omega-3 fatty acid intake in school aged children. J Pediatr. 2011 Jan;158(1):83-90, 90.e1.
16. Bhargava R, Kumar P, Kumar M, et al. A randomized controlled trial of omega-3 fatty acids in dry eye syndrome. Int J Ophthalmol. 2013 Dec 186(6):811-6.
17. Larmo PS, Järvinen RL, Setälä NL, et al. Oral sea buckthorn oil attenuates tear film osmolarity and symptoms in individuals with dry eye. J Nutr. 2010 Aug;140(8):1462-8.
18. Macsai MS. The Role of Omega-3 Dietary Supplementation in Blepharitis and Meibomian Gland Dysfunction (An AOS Thesis). Trans Am Ophthalmol Soc. 2008 Dec;106:336–56.
19. SanGiovanni JP, Chew EY, Clemons TE, et al. Age-Related Eye Disease Study Research Group. The relationship of dietary lipid intake and age-related macular degeneration in a case-control study. AREDS Report No. 20. Arch Ophthalmol. 2007 May:125(5):671-9.
20. Chong EW, Robman LD, Simpson JA, et al. Fat consumption and its association with age related macular degeneration. Arch Ophthalmol. 2009 May;127(5):674-80.
21. Feher J, Kovacs B, Kovacs I, et al. Improvement of visual functions and fundus alterations in early age related macular degeneration treated with a combination of acetyl-L carnitine, omega-3 fatty acids and coenzyme Q10. Ophthalmologica. 2005 May-June;219(3):154-66.
22. Hoffman DR, Birch DG. Docosahexaenoic acid in red blood cells of patients with X-linked retinitis pigmentosa. Invest Ophthalmol Vis Sci. 1995 May;36(6):1009-18.
23. Hoffman DR, Locke KG, Wheaton DH, et al. A randomized, placebo-controlled clinical trial of docosahexaenoic acid supplementation for X-linked retinitis pigmentosa. Am J Ophthalmol. 2004 Apr;137(4):704-18.
24. Ren H, Magulike N, Ghebremeskel K, Crawford M. Primary open-angle glaucoma patients have reduced levels of blood docosahexaenoic and eicosapentaenoic acids. Prostaglandins Leukot Essent Fatty Acids. 2006 Mar;74(3):157-63.
25. Lu M, Cho E, Taylor A, et al. Prospective study of dietary fat and risk of cataract extraction among US women. Am J Epidemiol. 2005 May 15;161(10):948-59.
26. Suzuki M, Noda K, Kubota S, et al. Eicosapentaenoic acid suppresses ocular inflammation in endotoxin-induced uveitis. Mol Vis. 2010;16:1382-8.

