For many people, the eyes are the most important facial feature and one of the first to show cosmetic signs of aging. Droopy lids often prematurely age a person as well as impair vision. Blepharoplasty corrects these problems and also removes puffiness and bags from under the eyes that can create a worn, tired look.
Although there is a great deal of overlap, patients who desire blepharoplasty generally fall into two broad categories. The first category includes people who wish to accentuate their eyes, improve their overall appearance, and reduce the tired look of excess and redundant eyelid tissue. People in this category are good candidates for cosmetic blepharoplasty.
In the second category, patients complain of visual difficulties related to heavy upper eyelid tissue. Often, the skin of the upper eyelids rests across the lashes and obscures vision. Patients in this category notice improved vision when they elevate the flaps of skin with their fingertips and are candidates for functional blepharoplasty.
Brow Ptosis vs. Dermatochalasis
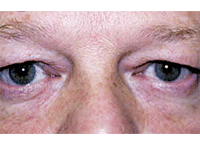
Blepharoplasty
can remove excess
skin in cases of dermatochalasis,
as seen here.
Dermatochalasis is a condition in which there is excess upper eyelid skin. A mild to moderate amount of excess eyelid skin results in a tired, sad appearance. An advanced amount of excess eyelid skin can block parts of a patient’s peripheral vision, especially at the top and sides. Dermatochalasis is corrected by removal of excess skin through a procedure known as upper eyelid blepharoplasty, commonly known as an eye lift. An eye lift may be performed for cosmetic reasons, to improve a patient’s appearance, or for functional reasons, to improve a patient’s peripheral vision.
In contrast to dermatochalasis, ptosis refers to an abnormal position of the eyelid margin. A person may be born with drooping of one or both eyelids, a condition known as congenital ptosis. However, the vast majority of patients have normal eyelids when they are born and develop droopy eyelids in adulthood, a condition known as acquired ptosis. Patients with ptosis require a thorough evaluation, as this condition may be caused by neurologic or neuromuscular disorders such as myasthenia gravis, Horner’s syndrome, myotonic dystrophy, or even a type of brain aneurysm.
It is also necessary to evaluate the position of the brow when evaluating patients with a droopy lid. A droopy eyebrow is referred to as brow ptosis and often coexists with dermatochalasis and ptosis. In most men, the optimal position of the brow is at the bony rim above the eye. In women, the optimal position of the brow is above this rim, especially on the lateral side.
The objective of this article is to discuss the diagnosis and surgical management of patients in need of functional blepharoplasty in which the primary goal is restoring vision.
Most major insurance companies will pay for surgery when excess eyelid skin produces a functional visual impairment.
Etiology
Patients who need blepharoplasty procedures often present complaining of tired eyes, sad eyes, or extra tissue around the eyes. When the skin of the upper lids rests across the eyelashes, it is an indication that the vision may be compromised by the eyelid configuration. Dermatochalasis, fat herniation or protrusion, brow ptosis, and eyelid ptosis secondary to disinsertion or dehiscence of the levator aponeurosis all contribute to patient perceptions of the need for upper lid blepharoplasty.1
Dermatochalasis is loose skin of the upper or lower eyelids and is considered part of the normal aging process. It is bilateral, often asymmetric, and may be cosmetic and/or the cause of functional visual impairment. Weakened connective tissue, gravity, decreased skin elasticity and various systemic conditions are all responsible for the development of this excess skin.
It is essential to differentiate dermatochalasis from the less common blepharochalasis, which is the expansion of the orbital septum and preseptal muscles secondary to repeated angioneurotic edema and is seen less commonly in younger patients. This recurrence causes loose skin and orbital fat herniation. Involvement of the lower eyelids can be quite dramatic; this protruding tissue is known as malar bags or festoons (figure 1).
The etiology of blepharoptosis can be classified based on whether it is true ptosis or pseudoptosis, and whether it is congenital or acquired. Acquired senile eyelid ptosis, also known as involutional ptosis, is a common condition in the elderly population. It is often accompanied by varying amounts of dermatochalasis. Acquired senile ptosis is produced by the disinsertion of the levator aponeurosis and is characterized by a high or absent eyelid crease, thinning of the upper eyelid tissue and abnormal levator function.2 Blepharoplasty of the ptotic lid, without repair of the ptosis, may result in exaggeration of the drooping eyelid postoperatively.
Proper management requires a meticulous preoperative analysis with special regard to brow position, lid crease and lid fold, levator function, tightness of the canthal ligaments, tarsal plate and orbital septum, because these factors will determine the type and extent of procedure.
It is important to note that the relationship between adnexal structures and upper eyelid function is delicate, but critical. Additionally, the insertion of the septum is very different in Asian lids than in Caucasian lids and recognizing this is critical for a good surgical outcome. There is also a marked difference between males and females.
Thorough Pre-op Testing
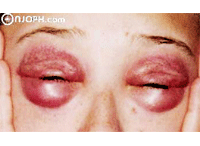
1. Involvement of the lower eyelids can be quite dramatic; this protruding tissue is known as malar bags or festoons.
A comprehensive eye examination should be performed on all prospective blepharoplasty patients to determine the best-corrected visual acuity and to prevent any question of decreased postoperative visual acuity.
Begin with a thorough medical and ocular history. This should include inquiries of any periorbital trauma, thyroid conditions, dry eye syndrome and skin conditions.
Perform formal visual field testing twice—first with the eyelids in a natural position and then with the skin held off (elevated from) the eyelids. Often, this will confirm significant visual field loss.
Dry eye syndrome can be a postoperative complication of blepharoplasty. Therefore, a dry eye evaluation must be part of the preoperative work-up. Risk of dry eye should be objectively measured by evaluating the patient’s tear film break-up time (TFBUT) and by performing a Schirmer’s tear test.
A standard Schirmer test uses a strip of Whatman #41 filter paper, 5mm in width x 30mm in length, with a fold 5mm from the end. Normal wetting is 10mm to 30mm in five minutes in patients less than 50 years of age. If the patient only wets 5mm to 10mm in five minutes, he or she is at risk for dry eye. At less than 5mm of wetting, the patient has clinically significant dry eye.
The TFBUT measures the quality and stability of the tear film. A deficient time is considered any TFBUT of less than 10 seconds. The patient must be aware that lubrication may be needed temporarily after the blepharoplasty until the lids loosen a bit. However, a recent review of 141 medical records of patients with dermatochalasis found that nearly 87% of patients with keratoconjunctivitis sicca (KCS) had subjective improvement of symptoms after upper lid (UL) blepharoplasty.3 This suggests that UL blepharoplasty may be a useful element in the treatment of patients with both dermatochalasis and dry eye.
Brow and lid ptosis are other important criteria for the preoperative evaluation. Note the shape and location of the brow; it should be at the orbital rim. You can determine lid ptosis using three measurements:
• First, measure the vertical palpebral fissure (interpalpebral fissure or IPF) in primary gaze,
ascertaining that the patient’s brow and forehead are relaxed.
• Next, measure the margin reflex distance. This is a measurement of the center of the pupil to the upper lid margin. It indicates how close the upper lid is to the visual axis.
• Finally, maximal levator function shows how high the patient can lift his or her lid voluntarily. The fissure height can range from 7mm to 12mm, with an average height of 10mm.
The upper lid margin should fall 1mm to 2mm below the superior limbus, while the lower lid margin should rest at the level of the lower limbus. If there is traumatic or neurologic dysfunction, then simply shortening the levator aponeurosis will not fix the problem. In those cases, a frontalis suspension must be performed. In the majority of cases of involutional ptosis (senile or age-related), patients have good levator function, allowing for levator resection procedures.
Post-op Instructions
Blepharoplasty can be performed either in the physician’s office or in the hospital operating room. Surgery often lasts less than an hour and produces minimal pain.
Following surgery, patients should be advised to apply ice to the eyelids for 15 minutes per hour for the first 72 hours. Appropriate pain management includes Tylenol, ice and ophthalmic antibiotic/steroid ointments.
At no time should patches be placed on the eyes. And, warn patients not to wear contact lenses or eyelid makeup for one week following blepharoplasty surgery. Patients also must be advised to avoid vigorous exercise for one week following surgery.
Patients typically return to work several days following the operation. Let them know that they can expect a minimal to moderate amount of bruising and swelling for seven to 10 days after surgery.
A complete recovery is said to take approximately six weeks, but patients will look even better at three months and better still at six months.
Case Report: Solving Functional and Cosmetic Complaints
History A 75-year-old white female, who had been under my care for three years, presented for an emergency visit with a chief complaint of “red eye.” The patient was undergoing treatment for several months by her otolaryngologist for a blocked salivatory gland on the right side. The otolaryngologist prescribed eardrops that were compounded at a local pharmacy. The patient complained of constant headaches, bloodshot eyes and tearing. Furthermore, she had been using artificial tears copiously with no improvement.
Her medical history was also positive for diabetes mellitus, long-term heterotopic ossification joint pain (>45 years).
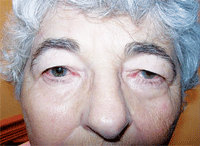
This patient presented for a red-eye exam, but further investigation revealed
significant ptosis and dermatochalasis.
Her ocular history was positive for non-proliferative diabetic retinopathy, posterior vitreous detachment, O.D., and asteroid hyalosis, O.S.
Diagnostic Data
Best-corrected visual acuity measured 20/20 O.D. and 20/40 O.S., with no improvement upon pinhole testing.
Biomicroscopy revealed Grade 2+/3 bulbar hypermia and follicular hypertrophy, droopy lids (dermatochalasis O.U.), scant tear meniscus, and Grade 2+/3 nuclear sclerotic and posterior subcapsular cataracts in both eyes.
The patient also expressed an interest in being able to wear eye makeup again. She reported frustration that she had been unable to do so for at least five years.
I informed the patient that her droopy lids were a factor in her ocular discomfort and perceived diminished distance vision and recommended that she have an oculoplastic consult with a local ophthalmologist. Central 30-2 threshold visual field testing showed markedly improved visual fields with eyelids taped, which underscored the medical necessity of blepharoplasty in this patient.
In the meantime, I wanted to rule out allergic versus bacterial conjunctivitis O.U., so I prescribed Zylet (loteprednol and tobramycin, Bausch + Lomb) t.i.d. O.U. for 10 days. For the dry eye syndrome, I prescribed Systane Ultra Preservative-Free (Alcon) b.i.d. O.U.
Discussion
In my state (New Jersey), optometrists are not permitted to comanage functional or cosmetic blepharoplasty. However, a thorough knowledge of the conditions that require this procedure is critical, given that blepharoplasty requires close communication between the referring optometric physician and the oculoplastic surgeon.
The surgeon to whom I referred my patient confirmed the significant ptosis and dermatochalasis. His precise measurements of the patient’s bilateral ptosis included the following findings:
• Interpalpebral fissure: 8mm O.D., 6mm O.S. (average IPF is 10mm).
• Margin Reflex Distance: 0.5mm O.D., 0.0mm O.S.
• Maximal Levator Function: 12mm O.D., 12mm O.S.
A functional levator resection and blepharoplasty were scheduled.
The patient was brought to the operating room and placed on the operating table in the supine position. She was sedated, but awake during the entire procedure because the surgeon needed to ask her to look in different positions of gaze to check the symmetry of the lid margins between the right and left eye.
The patient was marked with a sterile tip marking pen on the upper lids. The area of excision of skin and muscle was outlined and compared for symmetry. The patient was then sedated heavily by the anesthesiologist. Local anesthetic was infiltrated into each upper lid. Approximately 2cc to 3cc were used in each upper lid. The anesthetic consisted of a 2:1 mixture of 2% lidocaine with epinephrine and 0.75% marcaine. The patient was then prepped and draped in the usual sterile fashion.
Attention was first directed to the right upper lid. A #15 blade was used to incise the skin in the previously demarcated area. Hemostasis was established here and throughout the procedure with a Bovie Cautery and cotton-tipped applicators. A skin muscle flap was then elevated and excised entirely over the extra skin of the upper lid.
This exposed the underlying orbital septum.
The septum was incised with a Westcott scissor, allowing the preaponeurotic fat pad to prolapse forward. Prolapsing fat pads were clamped over with a hemostat and excised. The pedicle was cauterized before the clamp was released. Careful attention to hemostasis was carried out here. This was done for the superior and nasal fat pads.
The dissection was then carried inferiorly to expose the anterior surface through the tarsal plate. A 6-0 vicryl suture on an S-29 needle was then passed through the anterior surface of the tarsal plate over the pupil. This was then carried through the exposed levator aponeurosis several millimeters superiorly. This was tied with an adjustable suture.
A similar procedure was now performed on the left upper lid to bring the left upper lid to the same point in surgery as the right upper lid. This was performed without complication. Now, with both upper lid levators ressected on adjustable sutures, the patient was asked to open her eyes and the lids were checked for height, contour and symmetry. Little or no adjustment was needed because good height and contour and symmetry were achieved.

|
| Following functional levator resection and blepharoplasty, the patient is doing great and continues to be pleased with her surgical result. Further, her visual acuity remained stable at its pre-operative level.
|
Tobradex (tobramycin and dexamethasone, Alcon) ointment was placed over the wounds. The patient tolerated the procedure well and was moved to recovery room in stable condition.
Follow-up revealed that the patient’s visual acuity remained stable at its pre-operative level. Overall, she is doing great and continues to be pleased with her surgical result.
She is able to wear eye makeup again and feels rejuvenated. In addition, after being divorced for many years, and choosing not to date, the patient has met a widowed gentleman, and they are a couple.
In closing, it is important not to assume that patients over age 70, whether they are male or female, are not interested in functional oculoplastic procedures that will also greatly improve their cosmesis. However, since Medicare will only pay for functional dermatochalasis or ptosis, a visual field is necessary before a referral can be made for a functional eyelid lift.
Dr. Boname is in private practice in Skillman, N.J.1. Castro E, Foster JA. Upper lid blepharoplasty. Facial Plast Surg. 1999;15(3):173-81.
2. Millay DJ, Larrabee WF Jr. Ptosis and blepharoplasty surgery. Arch Otolaryngol Head Neck Surg. 1989 Feb;115(2):198-201.
3. Vold SD, Carroll RP, Nelson JD. Dermatochalasis and dry eye. Am J Ophthalmol. 1993 Feb 15;115(2):216-20.

