Contact lens wear is the preferred method of correcting anisometropia in children, especially due to the risk of amblyopia a risk that increases if the child is premature or has a family history. The type and amount of refractive error determines if amblyopia will develop, although amblyopia is more prevalent in uncorrected hyperopes than in myopes due to the close working distance of children. Isoametropia will result in amblyopia if the child is greater then 10D myopic or 5D hyperopic. Amblyopia, the cause of 2-4% of vision loss in children, is preventable if diagnosed and treated early.
Children who have anisometropia may not show any symptoms if the fellow eye is close to emmetropic. For the very young, parents should note any preferential looking, eye turn, headaches or failure to reach developmental milestones especially with mobility. Ideally, you should examine the child by 6 months of age and then at 24 months if the child is non-symptomatic. If you note a high refractive error or anisometropia, begin treatment promptly.
Reviewing correction options
Spectacles. Spectacles, the easy alternative for the compliant child, have many disadvantages, including:
- induced prismatic effects with eye movements
- minification of the eye and of the image if high minus
- poor compliance
- prevention of fusion leading to suppression.
Contact lenses. Contacts reduce many of these disadvantages, but compliance and available lens parameters can be problems. Ill often fit a child with only one lens to equalize the power of the eyes at the near plane. Insertion and removal can be traumatic, making extended or continuous wear preferred if the parents are compliant.
Keep these pearls in mind:
- Hyperopic corrections are more readily available with the use of aphakic silicone lenses than with high minus powers.
- Custom-designed soft lenses (Kontur Kontact Lens Company) will accommodate smaller diameters (12.0) and steeper base curves (6.80), but can become expensive if the lens needs to be replaced often.
- A frequent replacement silicone hydrogel lens such as CIBA Visions Focus Night & Day lens is available in several base curves and in plus and high minus powers, making it well-suited for the younger eye. The diameter (13.8 mm) is still the main obstacle. For a small aperture, .2-.4 mm really makes a difference.
Refractive surgery. If spectacle or contact lens therapy fails, refractive surgery may be an option for children with anisomyopic amblyopia. Refractive surgery on children has been performed as an investigational procedure. At the University of Chicago, our surgeons have performed LASEK on 2 children (one was 14 months old). LASEK is essentially PRK, but due to the aggressive healing of children, rather than scraping the epithelium, the surgeon creates a mini-pseudo-flap with a trephine that lifts only the epithelium. Similar to a LASIK flap, the LASEK surgeon replaces the flap after the ablation. LASEK, an aggressive approach requiring general anesthesia, should be considered only when traditional methods fail. There is much to learn about the pediatric globe, as well as the nomograms and surgical instruments used for these techniques.
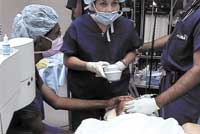

LEFT: Dr. Sclafani takes corneal measurements of an infant about to undergo LASEK. General anesthesia adds to the risk, but is well tolerated. RIGHT: Adhesive patches are more difficult for the patient to remove or to peak around. You can make the patch fun by encouraging an older sibling, for example, to wear a patch as well.
Correction only the beginning
Once the refractive error is corrected, amblyopia therapy is necessary to promote the use of the affected eye. Traditionally, the main option is patching of the good eye or its spectacle lens. I prefer adhesive patches to the pirates patch because theyre more difficult for the patient to remove or to peak around. Inherent problems include resistance or allergy to the adhesive patch, as well as non-compliance. An alternative is an occluder contact lens with a total occlusion in the pupil zone, usually 6 mm. I recommend Kontur Kontact Lens.
You may patch on a full- or part-time basis. Total occlusion requires careful monitoring usually every one week for every one year of life. If strabismus is present, consider full-time patching. Reserve part-time patching for those who have the ability to fuse. I tend to be more conservative, using part-time occlusion of the good eye for all conditions and greater periods of time for more severe cases.
Another option is penalization, in which the daily use of atropine (.5%-1% 1 drop) degrades the image of the good eye. Because the good eye cant accommodate, the amblyopic eye is forced to focus at demanding near targets. A recent study by the National Eye Institute has determined that this may be more effective then patching.
Dr. Sclafani (lsclafan@uchospitals.edu) is an Associate Professor of Clinical Ophthalmology and Director of Optometric Services and Contact Lenses at the University of Chicago.
What Causes Anisometropia?
Unilateral cataract extraction
Trauma with resultant corneal changes
Developmental conditions that lead to axial length or lenticular disparity

This infant is wearing an occluder contact lens OS for amblyopia therapy and a Silsoft aphakic lens OD.

