 Q: A number of my glaucoma patients have become concerned with dark circles and a “sunken look” to their eyes after using a prostaglandin for a period of time. This is particularly noticeable among patients on unilateral therapy. What's going on?
Q: A number of my glaucoma patients have become concerned with dark circles and a “sunken look” to their eyes after using a prostaglandin for a period of time. This is particularly noticeable among patients on unilateral therapy. What's going on?
A: A recent study by Louis R. Pasquale, MD, and colleagues at the Glaucoma Service at Massachusetts Eye and Ear confirmed that some glaucoma patients who take a prostaglandin analog (PGA) can develop a constellation of symptoms referred to as prostaglandin-associated periorbitopathy (PAP). This includes deepening of the upper eyelid sulcus, upper lid ptosis, enophthalmos and loss of the inferior orbital fat pads.1
These symptoms “can be easily dismissed as age-related adnexal findings in bilateral users, [but have] been recognized in several small case series involving both unilateral and bilateral PGA users,” the authors write.1 These findings were associated with the three original PGAs.
How PGAs cause or contribute to PAP is unknown, but the deepening of the upper eyelid sulcus and the loss of inferior orbital fat seems to involve the PGAs’ effects on periorbital fat cells.
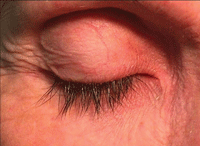
Prostaglandins may cause periorbital problems, such as sulcus deepening (above) or upper lid ptosis, that might even affect vision.
“The exact mechanism of action is still being investigated on why PGAs are causing this sunken appearance,” says Brett King, OD, who is part of a large glaucoma practice near Kansas City.
Dr. King points to an earlier study (also by researchers at Mass. Eye and Ear) that suggested that “FP-prostanoid receptor activation by the PGA inhibits differentiation in several cell lines, preventing fat cell specific gene expression. This results in denser tissue with less fat,” he says.2
This may not just be a cosmetic problem, either. In the recent study, Dr. Pasquale and colleagues concluded that PGA-associated levator muscle dysfunction and upper lid ptosis “represent significant side effects that could impact visual function in glaucoma patients.”
Q: If patients complain, what should I do about it?
A: “While this side effect appears to be relatively common, I do not have a lot of patients complaining of the sunken appearance,” Dr. King says. Patients have more complaints about hyperpigmentation of the lids than the loss of periorbital fat, he says.
He says that when starting patients on treatment, discuss the possible side effects of medications—including cosmetic side effects. “In my experience, most patients prefer medications with less systemic side effects. But some are very concerned with cosmetic issues,” Dr. King says. “Obviously, unilateral dosing highlights the differences and will elicit more patient concern.”
So, when treating only one eye, take this into consideration to choose the most appropriate drop. Be sure to lay out the potential side effects and options for the patient, and clearly document in the chart that you did so.
“As with hyperpigmentation, some recovery of the inferior fat pads can occur upon discontinuing the medication,” he says.3 “But the superior sulcus hollowing is possibly more permanent.”1 If this becomes problematic, try switching the patient to a different class of medication.
“Also, advise patients to wipe away the residue from the medication a couple minutes after application, as this may help reduce the hyperpigmentation of periocular tissue,” Dr. King says.
1. Shah M, Lee G, Lefebvre DR, et al. A cross-sectional survey of the association between bilateral topical prostaglandin analogue use and ocular adnexal features. PLoS One. 2013 May 1;8(5):e61638.
2. Filippopoulos T, Paula JS, Torun N, et al. Periorbital changes associated with topical bimatoprost. Ophthal Plast Reconstr Surg. 2008 Jul-Aug;24(4):302-7.
3. Aydin S, Isikligil I, Teksen YA, Kir E. Recovery of orbital fat pad prolapsus and deepening of the lid sulcus from topical bimatoprost therapy: 2 case reports and review of the literature. Cutan Ocul Toxicol. 2010 Sep;29(3):212-6.

