 Q: I recently saw a patient who had collagen crosslinking (CXL) for keratoconus and his intraocular pressure seems to have increased. Is it typical for CXL to cause a rise in IOP? What type of device would provide the most accurate measure of IOP in these patients?
Q: I recently saw a patient who had collagen crosslinking (CXL) for keratoconus and his intraocular pressure seems to have increased. Is it typical for CXL to cause a rise in IOP? What type of device would provide the most accurate measure of IOP in these patients?
A: “An increase in measured IOP after CXL treatment is a typical finding in keratoconic patients, which has also been shown in relevant published studies,” says Michael A. Grentzelos, MD, who coauthored a study that reported a significant increase in Goldmann applanation tonometry measurements of IOP in a prospective case series of 55 eyes in 55 patients in Greece.1 “However, it is not clear what the reason for this finding is; we cannot be certain if the increase in measured IOP is an overestimation, as we believe, or an increase in ‘true’ IOP, or both,” he explains.
Used to halt the progression of keratoconus, CXL substantially stiffens the cornea by creating chemical bonds within or between collagen fibrils and proteoglycans.2 And properties of the cornea—including thickness and biomechanical strength—are known to influence measured intraocular pressure.3
“While the thinner corneas found in eyes with keratoconus or prior LASIK lead to underestimation of IOP, several studies have suggested that the change in biomechanical properties of the cornea that are induced by cross-linking may result in slight overestimation of IOP,” says Grace Lytle, OD, MS, director of professional education at Avedro, a medical device company that makes CXL technology, in Waltham, Mass. “However, topical steroids are frequently incorporated into the postoperative regimen for crosslinking, and care should be taken to differentiate an overestimation of IOP from true IOP increase due to steroid response or other etiologies.”
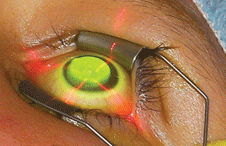
An intraoperative photo of a keratoconic patient undergoing a corneal collagen cross-linking procedure. Photo: Peter Hersh, MD, Hersh Vision Group, Teaneck, NJ.
While there is not yet an established standard of care for measuring IOP following CXL, current literature suggests that methods of tonometry that compensate for biomechanical properties of the cornea (such as the Pascal tonometer, Ziemer Ophthalmic Systems) may provide more accurate measurement than Tonopen (Reichert Inc.) or Goldmann applanation tonometry.1,4
“It seems that a dynamic contour tonometer should probably provide the most accurate measurement of intraocular pressure in these patients postoperatively, but this has not been proven yet,” Dr. Grentzelos says.
1. Kymionis GD, Grentzelos MA, Kounis GA, et al. Intraocular pressure measurements after corneal collagen crosslinking with riboflavin and ultraviolet A in eyes with keratoconus. J Cataract Refract Surg. 2010 Oct;36(10):1724-7.
2. Meek KM, Hayes S. Corneal cross-linking—a review. Ophthalmic Physiol Opt. 2013 Mar;33(2):78-93.
3. Liu J, Roberts CJ. Influence of corneal biomechanical properties on intraocular pressure measurement: quantitative analysis. J Cataract Refract Surg. 2005 Jan;31(1):146-55.
4. Gkika MG, Labiris G, Kozobolis VP. Tonometry in keratoconic eyes before and after riboflavin/UVA corneal collagen crosslinking using three different tonometers. Eur J Ophthalmol. 2012 Mar-Apr;22(2):142-52.

