Q: I have a patient who has severe dry eye and is recalcitrant to virtually all attempted treatments. Has anyone had success with non-conventional treatments ?

A: Most of our dry eye patients respond well to conventional treatment modalities, such as artificial tears, space humidifiers and cyclosporine. And, while therapy may need to be continuous, most patients experience symptomatic relief and are able to function in their daily tasks fairly unencumbered. But, every so often, the patient in our chair will exhibit recalcitrant dryness that is non-responsive to tried and true treatments. For such patients, additional therapies are required. Luckily, we have some options.
“We have become increasingly aware of the role of meibomian gland dysfunction (MGD) in severe dry eye,” says William Townsend, O.D., executive board member of the Ocular Surface Society of Optometry. Dr. Townsend instructs his patients to use warm compresses, increase the intake of omega-3 fatty acids by alterations in diet or supplementation with fish or krill oil capsules.
Dr. Townsend believes that off-label use of medications can be very beneficial to these individuals. “We often prescribe Xibrom (bromfenac, ISTA Pharmaceuticals) as an off-label application. While we have used this on a limited number of patients, many of whom have very severe dryness, our overall impression is that they often benefit from once-a-day dosing of bromfenac,” he says.
Another dry eye remedy that is considered non-conventional is albumin, which is a key protein in autologous serum. But some report more success with autologous serum. “The reason
I like autologous serum is because it’s the patient’s own natural serum and they’re getting more than just the albumin,” says Paul Karpecki, O.D., Cornea Services & Ocular Disease
Research Director at the Koffler Vision Group in Lexington Ky.
Dr. Karpecki explains how it works: A phlebotomist at an eye bank draws a patient’s blood. The serum is then extracted and mixed with artificial tears. This solution is split into doses and flash frozen. “Patients are then instructed to keep these drops in the freezer and thaw them out before use one at a time.” For patients who prefer not to have blood drawn, compounded albumin is a good option.
Androgen drops have been shown to be effective against persistent dry eye in premenopausal females. Another experimental hormone therapy for dry eye that is being studied is 3% testosterone cream that is applied to closed eyelids before bed. “Doctors can have a compounding pharmacy prepare this cream,” says Dr. Karpecki. Leiter’s Pharmacy (
www.leiterrx.com) and other compounding groups can make DHEA drops, a pro-androgen, in a carboxymethy cellulose vehicle. It may work best with evaporative dry eyes because it seems to have a direct effect on androgen receptors located in the meibomian glands or other areas on the ocular surface. This is not an FDA-approved drug and should be used with caution. Long-term effects are unknown, especially as they relate to the agent’s conversion to testosterone and estrogen in patients with a medical history of breast or prostate cancer.
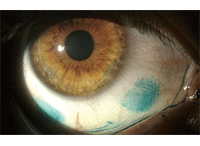
This contact lens wearer has severe dry eye that is evidenced by marked lissamine green staining of the conjuctiva.
Intense pulsed light therapy is another alternative in patients who have rosacea. Higher concentrations of cyclosporine may also work well for some patients.
Because of its anti-inflammatory properties, another option is tetracycline 0.025%, says Dr. Karpecki. Keep in mind, however, that tetracycline is contraindicated in pediatrics and pregnant or nursing women as well as patients on blood thinning medications (e.g., warfarin).
Dr. Karpecki warns that all therapies mentioned are not first-line treatment options. “We don’t know everything about these treatments, as they had not gone through the FDA for ocular indications, which is why they should only be used as a last resort,” he says.

