 |
History
Entoptic phenomena were first described by Johann Purkinje in the early 1800s, to describe the fleeting, black afterimage of retinal vasculature, later coined the ‘Purkinje tree.’1 This phenomena occurs due to the location and pattern of the branching retinal vascular ‘tree’ in front of the photoreceptor layer, casting a shadow that is only induced when the anterior segment of the eye is illuminated.1 It differs from a real image, particularly in that it does not track with eye or retinal movement due to the direct and constant relationship with the photoreceptor layer.2 In fact, it is this observation, which led to the conclusion that there must be a rapid mechanism of image creation and erasure as the foundation of normal visual processing.2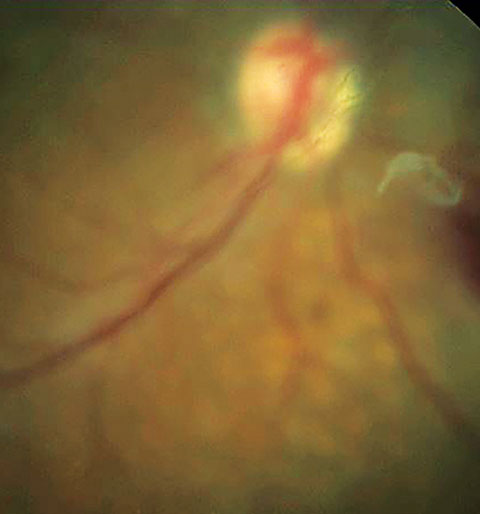 |
| Here, entoptic phenomenon is perceived as vitreous floater secondary to posterior vitreous detachment. |
Screening Applications
In the late 1990s, the application of this afterimage was used clinically to grossly measure potential acuity, as patients’ lack of perception of their vessels correlates highly with poor macular function and markedly reduced acuity.1 It was also helpful in cases where significant media opacities existed, where—if the illumination of a closed eye induced shadows—it correlated with good retinal and macular function.1,2Scanning laser entoptic perimetry. More recent studies recognize this modality as the method to measure entoptic phenomena, as it can offer significant retinal detail as it pertains to foveal capillary detail, the size of the foveal avascular zone (FAZ) and macular blood flow, with greater accuracy than more invasive methods, such as fluorescein angiography.3,4
Scanning laser entoptic perimetry is of particular interest to assess diabetic retinopathy, a leading cause of blindness where early detection is a key factor in visual preservation.3 Studies suggest that this is an effective, noninvasive and portable screening tool to detect retinal dysfunction in diabetic retinopathy, allowing practitioners to identify asymptomatic patients prior to the onset of central vision loss.3,5 Although this would not replace a retinal exam or photo, it has the potential for patients to train and screen themselves to identify early changes in many retinal diseases.5
For example, in a study that used scanning laser entoptic perimetry for the evaluation of age-related macular degeneration (AMD), the training period for patients took no longer than two minutes and, using a computer screen and digital pen, these patients were able to view various stimuli and draw the areas of qualitative difference directly onto their screen. This method was very effective in this case as well, in detecting very early stages of AMD, a time when patients do not typically exhibit any symptoms of the disease.6
Clinically Significant EPs
The most commonly observed pathological phenomenon is the shadow cast by vitreous floaters, appearing as either a black spot, in the case of posterior vitreous detachment with Weiss ring, or colorless ellipses thought to be due to embryonic remnants or proteins in the vitreous. These constituents cast a shadow on the retina and elicit the symptomatic presentation. Moore’s lightning streaks. These are also a commonly encountered photopsia, described as the flash of light that many patients experience in cases of anomalous posterior vitreous detachment, where vitreous liquefaction precedes the weakening of vitreoretinal adhesions, resulting in instances of retinal
traction.7
Blue arc entoptic phenomena. These were first observed by Dr. Purkinje after viewing fire embers in the dark, consist of transient and varying shades of blue arches. Researchers believe they arise in response to the stimulus of the blue-yellow wavelength systems, and follow the distinct anatomy of the nerve fiber layer; potential exists to use this to help practitioners diagnose and monitor very early stages of glaucoma.7 Other theories speculate that leukocytes, moving within one’s own retinal capillaries, mediate the phenomenon.8 Blue arc EP is inversely correlated with the degree of amblyopia, with studies concluding that its loss varies with the severity of the condition.5
Our patients will often report to us with subjective visual disturbances, of either a normal or abnormal cause. Taking a thorough history may reveal underlying ocular pathology. In several cases, these common visual phenomena have the potential to serve as the basis for future implementation of ocular disease screenings and monitoring techniques.
| 1. Mark HH. The entoptic view of the retinal vessels. Acta Ophthalmologica. 2014;92(3):e237-40. 2. Cappola D, Purves D. The extraordinary disappearance of entoptic images. Proc Natl Acad Sci USA. 1996;93(4):8001-4. 3. El-Bradey M, Plummer DJ, Uwe-Bartsch DU, Freeman WR. Scanning laser entoptic perimetry for the detection of visual defects associated with diabetic retinopathy. Br J Ophthalmol. 2006;90(1):17-9. 4. Wang Q, Kocaoglu O, Cense B, et al. Imaging retinal capillaries using ultrahigh-resolution optical coherence tomography and adaptive optics. Invest Opthalmol Vis Sci. 2011;52(9):6292-9. 5. Applegate R, Bradley A, van Heuven W, et al. Entoptic evaluation of diabetic retinopathy. Invest Opthalmol Vis Sci. 1997;38(5):783-91. 6. Freeman WR, El-Bradey M, Plummer DJ. Scanning laser entoptic perimetry for the detection of age-related macular degeneration. Arch Ophthalmol. 2004;122(11):1647-51. 7. Pasquale LR, Brusie S. The blue arc entoptic phenomenon in glaucoma (an American ophthalmological thesis). Trans Am Ophthalmol Soc. 2013;111:46-55. 8. Grunwald J, Sinclair S, Crandall A, Riva C. Blue field entoptic phenomenon in amblyopia. Ophthalmology. 1981 Oct;88(10):1054-7. |

