 |
A 73-year-old woman presented for her glaucoma progress evaluation. She had been diagnosed with primary open-angle glaucoma (OAG) four years earlier and started on latanoprost 0.005% in each eye, which she tolerated well. She was 20/25 OU and her vision was commensurate with her mild cataracts.
Her visual fields showed very mild loss OD and a moderately extensive inferior arcuate defect OS. Recent visual field analysis confirmed no changes in either eye. Central corneal thickness was 562µm OD and 568µm OS. Intraocular pressures (IOPs) were 19mm Hg OU. Her best IOP reduction from latanoprost was 15mm Hg OD and 17mm Hg OS.
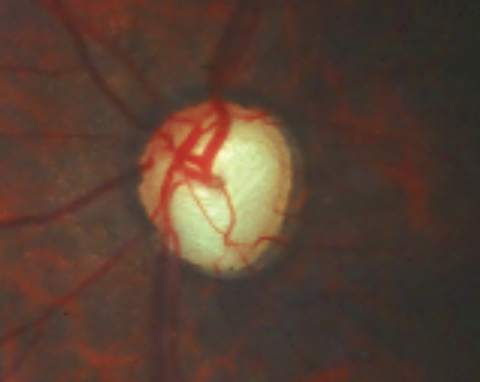 |
| Glaucomatous optic nerves such as this one now have a new potential lifeline. |
To Treat or Not To Treat?
Today’s reading was especially troubling in that her peak IOP was 22mm Hg OD and 23mm Hg OS.
Previously, it was felt the IOP reduction from latanoprost was insufficient, and she had been prescribed a beta-blocker, carbonic anhydrase inhibitor and an alpha adrenergic agonist. She had either local ocular or systemic adverse effects to each, necessitating discontinuation, leaving latanoprost as maximal tolerable medical therapy.
While her IOP rising into the upper teens was disconcerting given her low baseline untreated pressures, it was comforting to see that visual fields, optic discs and retinal nerve fiber layer were all stable. This left a conundrum: either monitor a seemingly unchanging patient with current therapy or go on to more invasive laser or surgical options based simply on suboptimal IOP reduction.
Recently, a new option for patients like ours, Vyzulta (latanoprostene bunod 0.024%, Bausch + Lomb and Nicox), was approved for the reduction of IOP in patients with OAG and ocular hypertension (OHTN).
Mechanism of Action
Vyzulta is a nitric oxide-donating prostaglandin analog designed to exploit both the uveoscleral aqueous outflow pathway (through the prostaglandin action) and the trabecular outflow channels (through the nitric oxide actions).1 Until now, enhancing outflow through the trabecular pathway has been limited to the effects of laser trabeculoplasty and poorly tolerated miotics.
Vyzulta works by metabolizing into two moieties, latanoprost acid and butanediol mononitrate. The latter subsequently releases nitric oxide in human trabecular meshwork cells after application of latanoprostene bunod.1 Nitric oxide has many physiological roles and is involved in inflammation, pain sensation, rheumatoid arthritis, immune system modulation and gastroprotection. It is also an antioxidant.2
Nitric oxide released from latanoprostene bunod elicits trabecular meshwork cell relaxation that, in turn, enhances aqueous outflow through the trabecular meshwork, Schlemm’s canal and distal scleral vessels. It does so by inducing cytoskeletal relaxation via the soluble guanylyl cyclase-cyclic guanosine monophosphate (sGC-cGMP) signaling pathway.3 Targeting the conventional outflow tissues using nitric oxide-donating drugs represents an opportunity to restore trabecular outflow, a medically untapped area in glaucoma management with the added benefit of promoting a healthy trabecular meshwork.1,4
Galaxy Quest
Several pivotal trials show Vyzulta’s efficacy, including the VOYAGER and CONSTELLATION studies, which compared Vyzulta with latanoprost and timolol, respectively.5,6 VOYAGER concludes once-daily dosing of Vyzulta provided IOP reductions greater than those from latanoprost.5 In CONSTELLATION, both Vyzulta and timolol decreased IOP, but Vyzulta produced a greater mean reduction in nighttime IOP and improved diurnal ocular perfusion pressure compared with both baseline and timolol.6
The APOLLO study—which includes OAG and OHTN patients with baseline IOP between 25mm Hg and 36mm Hg—revealed that mean IOP with Vyzulta was significantly lower compared with timolol at all time points, a finding maintained during the open-label phase and confirmed in the crossover group from timolol to Vyzulta.7
The LUNAR study found mean IOP with Vyzulta was significantly lower compared with timolol at all points except at the 8am week-two point. IOP lowering was maintained during the open-label treatment and confirmed in the crossover group.8
The JUPITER study showed IOP decrease of 22% that lasted for a year (in a low baseline IOP group).9
A study involving 24 healthy, normotensive Japanese male volunteers evaluated the effect of Vyzulta instilled once daily.10 Following 14 days of treatment, investigators saw a mean pressure reduction of 27% from baseline over the 24-hour diurnal.10 The authors concluded that studies of Vyzulta in patients diagnosed with normal tension glaucoma are warranted.10 Safety and tolerability has been established with no serious adverse events reported.11 The most common adverse event noted was transient hyperemia, which is largely well tolerated.11
With its dual mechanism of action, once-daily dosing and favorable efficacy and side effect profiles, Vyzulta gives optometrists and our patients cause to be hopeful.
Dr. Sowka is on Bausch + Lomb’s Vyzulta advisory board.
1. Cavet M, DeCory H. The role of nitric oxide in the intraocular pressure lowering efficacy of latanoprostene bunod: review of nonclinical studies. J Ocul Pharmacol Ther. 2017 Aug 7. [Epub ahead of print]. |

