Cataract surgery is a once in a lifetime opportunity to provide our patients with greatly improved vision. As the comanaging OD, any information we can gather prior to the surgical referral will help determine the procedure and outcome. For instance, if a patient has corneal astigmatism and a toric IOL would be appropriate, send the corneal topographies along with the referral notes, so the surgeon can look for consistency in the readings. 

This month, let’s review how pre-op testing can aid surgical planning.
Biometry
Precise biometry is essential in cataract surgery. Simply put, outcomes depend on it. Measurement of axial length by ultrasound has been the gold standard for many years. The introduction of optical biometry has increased accuracy and added the ability to measure anterior chamber depth, lens thickness, pachymetry, pupillometry, keratometry and white-to-white distance.
Popular optical biometers include the Lenstar LS900 (Haag-Streit) and the IOLMaster 500 (Zeiss). Both measure corneal curvature; the IOLMaster makes six measurements at 3mm of the central cornea and the Lenstar performs 16 central corneal readings—eight at 1.7mm and eight at 2.3 mm. All the standard IOL prediction formulas (Holladay I and II, SRK-T, Haigis and Hoffer Q) are built into the software.
If optical biometry cannot be performed, use applanation biometry. Compared to traditional biometry, A-scan biometry by immersion has better reproducibility, which leads to an overall increase in accuracy.
Corneal Measurements
Accurate corneal measurements are critical in IOL calculations and surgical planning, and they also determine which patients would benefit from limbal relaxing incisions or toric IOLs. Several technologies can provide this important data, and many practices capture corneal measurements on a number of devices to ensure consistency and accuracy of the measurements. Options include:
|
|
|
|
|
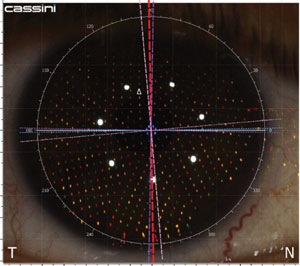
Measuring the relative distance between points allows precise mapping of corneal curvature, improving toric IOL planning.
|
• Keratometry. A mainstay of optometry, this reflection-based test measures four points over a central zone of 2.88mm to 4mm, two at the steep axis and the other two 90 degrees away.
• Placido disk topography reflects a series of concentric rings, or mires, off the cornea. Placido disk systems have certain advantages over the keratometer in that they are able to measure more points over the corneal surface and over an infinite corneal power range.
• Scanning slit topography such as the Orbscan (Bausch + Lomb) is a projection-based method that uses a series of slit-beam images to generate data regarding anterior surface curvature, posterior surface curvature and pachymetry.
• Scheimpflug-based systems. The Pentacam (Oculus) is a combination device consisting of a slit illumination system and a Scheimpflug camera that rotates around the eye. Rotating around the central corneal axis, the slit-camera device generates a series of radially oriented images of the anterior eye chamber. Results can be used to generate data on elevation, curvature, pachymetry and depth of the anterior eye chamber.
• Color LED Topography. The Cassini (i-optics) technology uses ray-tracing principles to measure the relative position of each point, using the three different colors as ‘triangulation’ points to determine elevation, depression and curvature.
If we are unable to take accurate pre-op measurements—e.g., in patients who could not easily access the diagnostic technology due to physical limitation—many surgeons rely on average corneal readings and approximations of axial length.
Additional Diagnostic Tests
• Endothelial cell count.
Assessing endothelial cell counts and density is useful in spotting patients at higher risk of corneal decompensation.
• Pachymetry determines corneal thickness and helps identify patients at risk of corneal decompensation; it also aids in glaucoma management.
• B-scan ultrasound is indicated for mature cataracts and to detect any posterior segment pathology prior to surgery.
1. Hill W. IOL Power Calculation Formulas. 2015. www.doctor-hill.com/iol-main/formulas.htm. Accessed Feb. 14, 2015.2. haag-streit-usa.com/mylenstar.aspx. Accessed Feb. 14, 2015.
3. www.meditec.zeiss.com/C1256CAC0038CEFF/ContainerTitel/IOLMaster500/$File/index.html. Accessed Feb. 14, 2015.

