 |
Optometrists have yet to reach a consensus on the meaning of optic disc hemorrhage (ODH) and management of patients when it develops. We don’t know what causes ODH. Some even consider the development of an ODH to be progression of disease.
During training, we were taught that if any patient who is being treated for glaucoma develops an ODH, whatever treatment they were receiving was not good enough. We’ve come a long way from then, but much of the mystery remains unsolved.
Is It ODH at All?
Before embarking on a glaucoma diagnostic evaluation or amplification of therapy in an already-diagnosed patient, ensure that what you are looking at is truly a glaucoma-related disc hemorrhage and not something else. Features of a true ODH include small size, contiguous with the neuroretinal rim, residing within the retinal nerve fiber layer (RNFL) and typically occurring at the superior, superior-temporal, inferior or inferior-temporal margin of the disc. Numerous other conditions, such as posterior vitreous detachment, optic neuropathy, diabetes, anemia, hypertension and retinal vascular disease, can cause optic disc hemorrhaging and parapapillary retina. This may lead to a glaucoma mimicking and misdiagnosis, but these other conditions typically don’t have the same features of a true glaucomatous ODH.1,2
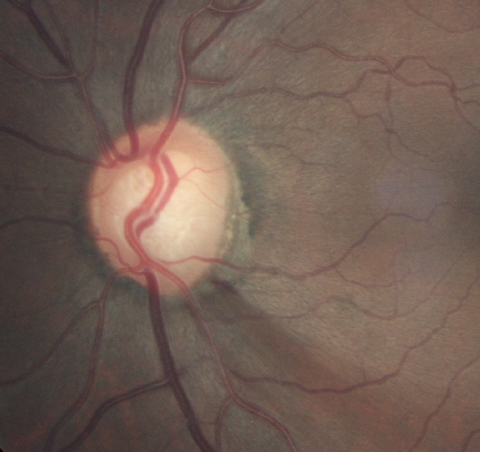 |
| This patient displays an inferior-temporal optic disc hemorrhage and RNFL loss. |
What Causes ODH?
Researchers suspect one of two likely drivers of this condition—mechanical vascular disruption and ischemic vascular dysregulation.3 The mechanical theory posits that shifting of tissue causes rupture of small blood vessels around the level of the lamina cribrosa or margin of the optic disc, ultimately resulting in ODH.3 Research using enhanced-depth imaging optical coherence tomography shows associations between laminar defects and ODH, supporting this theory.4 Additionally, this helps explain recurrent ODH developing in essentially the same disc location. The ischemic vascular theory suggests that systemic vascular diseases, platelet dysfunction, primary vascular dysregulation, vasospasm and faulty autoregulation of the blood flow to the anterior optic nerve result in ODH.
Patients with normal tension glaucoma experiencing exaggerated dips in blood pressure at night are at increased risk of ODH, lending credence to an ischemic etiology.5 Certainly, there is merit to this theory, but it does fail to explain the stereotypical location of most ODH, in addition to recurrent ODH in the same location as previous hemorrhages, and existence of strictly unilateral hemorrhages.3
What Comes First?
It remains unclear if ODH is a precursor to glaucomatous damage or merely an epiphenomenon of the disease process. Some evidence suggests that glaucomatous structural and functional abnormalities exist prior to ODH.6 Conversely, other research shows that ODH precedes RNFL thinning seen on OCT.7 Numerous reports identify ODH as an independent risk factor for glaucoma progression. However, major glaucoma studies do not consider the development of ODH itself to be the marker of progression.2
A 2001 study identified ODH as a risk factor for normal tension glaucoma progression.8 Curiously, the authors also found that in eyes with baseline ODH, lowering intraocular pressure (IOP) did not positively affect the visual outcome of the disease.9 Researchers in the Early Manifest Glaucoma Trial found that ODH was a risk factor for worsening disease.10
The study also found that not every patient with glaucoma will develop ODH and that lowering IOP did not prevent ODH from recurring.11 The Ocular Hypertension Treatment Study (OHTS) shows that ODH is a risk factor for the conversion to glaucoma from ocular hypertension.12 The study also found optic disc photographs were the most sensitive method of detecting ODH.12 In a 13-year follow-up of ODH in ocular hypertension, the OHTS group noted that its development increased the risk of primary open angle glaucoma (POAG) 2.6-fold.2 Though ODH increased the risk of converting to glaucoma, 78% of those with ODH have not converted to glaucoma in the 49 months following the event.2
It seems the preponderance of research indicates that a greater rate of visual field and RNFL loss exists after the development of ODH.13-15 Unfortunately, the ephemeral nature of ODH likely leads to an underestimate of its prevalence in glaucoma. Despite popular opinion, recurrent ODH does not seem to portend a greater rate or severity of progression than does a single hemorrhage.16,17 However, this appears to only be true in cases of recurrent ODH occurring in the same area of the optic disc. Eyes with ODH recurring at different locations from the initial ODH sites seem to have more pronounced visual field progression.18
Case in PointA 61-year-old male being treated for POAG for five years presented for his regularly scheduled progress evaluation. His entering, untreated peak IOPs were 30mm Hg OD and 20mm Hg OS. His central corneal thickness was average at 536µm OD and 531µm OS. He showed no evidence of angle closure or secondary glaucoma, but he had moderately damaged optic discs and RNFL in each eye. He was initially started on a prostaglandin analog and, through subsequent follow-up care, medications were added to further lower IOP. Currently, he uses latanoprost and dorzolamide/timolol FC in each eye with a consistent IOP of 10mm Hg to 12mm Hg OU. His most recent dilated exam and disc photography showed a developing ODH inferior-temporal in the left eye. Our review of older photographs found he had two previous ODHs in the same location in the last five years. On every visit, we look at the optic discs (dilated or undilated) on every glaucoma patient, mostly to screen for ODH. Typically, when we see an ODH develop in a treated glaucoma patient and IOP could be easily reduced further without invasive options (such as adding an additional medication to a treated IOP of 19mm Hg), we consider doing so. However, if further IOP reduction cannot be easily and safely done (such as a patient on maximal medical therapy or with a very low IOP already where surgery would be the next option), we typically monitor closely and intervene further only when we see definitive disc, RNFL or visual field deterioration. For this patient, since his treated IOP was already in the 10mm Hg to 12mm Hg range, and further reduction could not be easily achieved medically, we elected to monitor him. To date, five years after beginning therapy and having three ODHs over time in his left eye, we saw no change to his visual field, optic disc or RNFL. |
What’s a Doc to Do?
ODH is, like glaucoma itself, a complicated phenomenon that cannot be easily explained by IOP, mechanical or vascular factors alone.3 Glaucoma patients experiencing ODH clearly have an increased risk of progression. It has been suggested that glaucoma treatment intensification may have a beneficial effect in reducing the rate of thinning of the RNFL.14 Most definitely, glaucoma patients manifesting ODH should be observed more closely with frequent disc photographs, OCT and visual fields. Then, practitioners must decide if the current level of IOP is adequate or if therapy should be amplified.
ODH cannot be prevented from recurring simply by lowering IOP, nor should that be the goal. Recognize that ODH is a strong risk factor for glaucoma progression, and that lowering IOP is for the overall visual health of the patient. We cannot stop ODH from occurring by lowering IOP, nor are we doing poorly in our treatment plan should one develop in a patient.
1. Razeghinejad MR, Nowroozzadeh MH. Optic disc hemorrhage in health and disease. Surv Ophthalmol. 2017 Apr 8. pii: S0039-6257(16)30279-X. [Epub ahead of print]. |

