
What do you do when a young patient screams in the office? Ever had to chase a patient whos running away and brandishing your retinoscope? These are but a few of the tricky situations wed like to avoid when working with any of our patients, especially those with special needs.
Patients with special needs can create problems with the staff, the schedule and other clients. Many optometrists avoid such populations because they can be frustrating and intimidating.
Its normal to feel anxiety, but how can we manage this unique, special and needy population productively and to everyones satisfaction? Know that when we do provide care for these children, it really can be life changing for them, their parentsand even the doctor.
As a parent of an 18-year-old daughter, Jessica, who has Down syndrome, I have the professional and personal experience of examining and living with children with special needs. In this fourth and final installment of Reviews Role Playing series, Ill offer some tools to useand actions to avoidas we serve this special population.
Don"t talk so much. Use gestures when you communicate with children who have special needs. They"re more familiar with and responsive to body language.

All Kids Are Special
But, what are special needs"? I believe that special needs are those perceived as being unique or different from the routine. These children are special in that they dont do what we want or expect. Their needs are to be accepted and understood, and to grow like everyone else.
Accept the Situation, Accept the Patient The first lesson I learned came from my wife when we first learned that our new daughter, Jessica, had Down syndrome. Without hesitation, my wife accepted the situation and took action, while I was paralyzed.
Why optometry? As optometrists, we know that vision entails more than just visual acuity and ocular health. We understand the value of binocular skills and their impact on daily life. In the specialty of behavioral or developmental optometry, this understanding is expanded to include how patients vision influences their behavior and/or development. How patients utilize their vision to probe and understand their world affects how they perceive themselves, others, and the world around them, which in turn influences their behavior. In this sense, behavior may be anything from whether the patient wears their glasses to how their vision may impact a psychosis.
This notion of acceptance is critical. Before we can take action, we must first accept the situation. It is important for us to accept patients as isnot to be judgmental, sympathetic or ignorant; they are who they are, just as we are who we are. This allows us to be objective in our work, minimizing emotional distractions.
Behavior Masks Blur
Clinically, as an optometrist, my exam objective is both routine and behavioral. How do ocular health, refractive status, visual acuity and binocular status relate to function, behavior and the chief complaint?
My premise is that patients behaviors are not arbitrary, and my goal is to justify those behaviors based on my findings. Additionally, I may probe deeper in developmental areas to better explain patients behavior through observations of general movement, visual thinking, and other areas.
For instance, unsuppressed diplopia and unstable accommodation present some of the most misunderstood and clinically difficult situations. How do you know if a nonverbal child has diplopia or intermittent blur? Generally, we would assume chronic strabismics suppress. However, I have found that with the physically and mentally challenged, this cannot be assumed. As a result many have chronic unresolved diplopia or blur. Their visual problem may explain a number of their behaviors.
What we label as laziness, stubbornness or poor attention may not stem from bad personality traits, but from a vision problem. Knowing this can have a profound impact on the patients self esteem and social relationship, and in how the caregiver relates to the patient. Once the vision problem is identified, there can be more empathy and understanding for the patient, which is a big relief. Optometrists in particular can offer such insight.
Performance may be enhanced if the diplopia and blur could be better managed. Ive seen several cases of children with cerebral palsy in which physical therapists were working on head posture only to discover severe non-concomitant strabismus or swimming eyes. When the patient raised her head, her eyes were all over the place, and she immediately would drop her head to her lap. It was likely a nauseating experience, as her vision was more of a liability than an asset. She managed the situation simply by taking her eyes offline and dropping her head to her lap to avoid the visual chaos.
The key tool in this regard is the retinoscope. Dynamic retinoscopy allows us to observe the intricate focusing of the eye in real time and space. The mastery of this technique is unique to optometry and separates us from other professions.
The Special Needs Exam: Dos and Donts Dont: Do: Dont respond to verbal jousts. Ignore obnoxious statements. Dont command and instruct. Draw the patient to the task. Dont say you can do it. Say I bet you cant do it and Dont insist on a phoropter or autorefractor. Try a trial frame and retinoscope. Dont allow parental intervention. Restrain the parent. Dont have all the answers. Say I dont know. Dont pause. Keep the patient busy. Dont talk too much. Be quiet and employ gesture. Dont be rigid in routine and place. Be flexible.
offer an easy task.
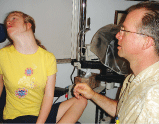
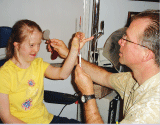

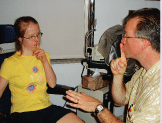

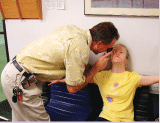
The Special Needs Exam
So, how can we relate to these patients such that we can help them? First, we must engage them at some level. If we cannot share our worlds, the exam will inevitably fail.
Grab attention. I start by approaching the children, not the parents, in the waiting room. I put the patients front and center because they are ones I need to engage. To do so, I stoop down to their eye level and address them formally: Where is Mr. Joey Smith? Ill comment how pretty or handsome the girl or boy is, which always gets a smile from both the child and parent. I ask their age and then pose an unexpected question such as, How does it feel to be so old? This kind of comment raises a smile and lightens the atmosphere. I now say I have some pictures to show them and proceed into the pre-testing area.
I glance or wink at the parent, but I dont talk to the parent. The parent is an observer; I instruct the parent not to speak as I tell the child that he or she and I are the boss. In this way, the child leads the parent into the exam room, which avoids the parent dragging the child in. If the parent jumps in and directs, I gesture the parent to stop and Ill re-establish the child-examiner connection.
Avoid the phoropter. In the exam room, I avoid the phoropter, preferring a trial frame and a retinoscope. Obviously, the subjective refraction is often unproductive. Even skiascopy lenses can be difficult because the patient will look and grab at these. So, I usually start with objective and observational tests, such as the Hirschberg test to check for strabismus. Now, while I have the childs fixation, I quickly do tracking, cover testing and convergence. I also attempt to do a stereo test, such as the stereo fly or glasses-free eye cube.
I follow these with dynamic retinoscopy. I dont worry about fogging or distance fixation at first. I want to see if there is a symmetric, bright and full reflex using a spot retinoscope. Im more concerned with qualitative aspects of the reflex as opposed to a quantitative refractive number. I scope them from across the room, avoiding the need for working lenses. I prescribe from my retinoscopea vital optometric skill for working with this population.
Next, I take the visual acuity with the HOTV chart with isolated letters or the face dot test. LEA cards have better standardization to assess the crowding phenomena in amblyopia, but with the symbols bunched together, they can get lost. With an isolated HOTV letter, at least I know exactly what symbol the patient actually looked at for a more accurate relative comparison when I trial frame and check the corrected acuity.
Draw them to the task. I like to employ simple form boards where I play dumb and let them take over. Nothing inspires kids to try an activity like witnessing failure by someone else, especially an adult. The child will invariably giggle and say, Let me try. Now you have their attention and can proceed to other tests and activities.
Use gesture communication. Children with special needs are more familiar and responsive to body language. Pointing, guiding, thumbs up, thumbs down, finger to the lips for quiet, and many other gestures offer universal and clear expressions generally understood by the child. For example, Ill snap my fingers to get eye contact and then gesture to the child to sit in the chair, be quiet, or point to a task.
Keep moving fast. Dont allow yourself to get stuck or allow them to frustrate you. Stay in control and move to the next test.
Avoid pauses or downtime. Pauses in the exam are an opportunity to make trouble and lose attention. Keep them busy and engaged.
Any one of these topics could involve much more discussion and research. However, this article is meant to provoke thought and introspection on approaching all our patients, not just those with identified special needs. You cannot succeed with every case, but hopefully these ideas will provide and inspire better patient communication and care.
The profound irony is how working with people with special needs helps me. Personally, as I have learned to accept those with special needs, I can also better accept myself and others. We all have faults and shortcomings, and, as such, we all have special needs. As optometrists, we can truly help these patients.
Dr. Lessmann is in private practice in You Control the Exam Here are some tips and tricks for a smoother, more productive examination.
Keep cool. Self-control is critical. The optometrist must maintain a calm demeanor even when the patient and/or parent is upset.
Be flexible in routine, approach and location. Ive started many exams in the waiting room and, once I have the patient engaged, I can then draw him or her into the exam room.
Dont be offended. Understand that the patient may be insecure and may lash out as a defensive act. Its nothing personal. Let it slide and stay on task. Your job is to assess the patients visual status, not to enforce social etiquette.
Be quiet. We talk too much. Even the parents/caregivers and the office should be as quiet and still as possible. Noise is distracting and irritating. Quietness facilitates attention. Be mindful that children are not small adultstheir language and symbolic expression is immature and imitative. Even if they articulate well, you cannot assume they ascribe the same meanings as we do.
Avoid or ignore verbal sensationalism and entrapment. The child may be trying to provoke you. If you respond to it, you give it credence and encourage its propagation. Unproductive or out-of-context speech is a verbal bottomless hole. Though it may be tempting to correct bad talking, it is unproductive in an optometric exam. Some kids get a real charge when they get adults all worked up with only a few utterances. Its a power trip for them. If you ignore it, you devalue it, and discourage its repetition. Control the parents by instructing them not to talk or correct the child, even if the child is obnoxious or uncooperative. You must demonstrate that you, the doctor, are in charge of this encounter. Otherwise, you have no standing in the childs eyes unless the parent authorizes it. And this can bring other unrelated issues to the exam, such as disputes over what the child wasnt allowed to have for breakfast, etc. You must separate your encounter from those other parent-child issues. You just want to do a visual exam. So ignore obnoxious behavior. Stay focused. Keep moving, and do the exam.
Control the parents by instructing them not to talk or correct the child, even if the child is obnoxious or uncooperative. You must demonstrate that you, the doctor, are in charge of this encounter. Otherwise, you have no standing in the childs eyes unless the parent authorizes it. And this can bring other unrelated issues to the exam, such as disputes over what the child wasnt allowed to have for breakfast, etc. You must separate your encounter from those other parent-child issues. You just want to do a visual exam. So ignore obnoxious behavior. Stay focused. Keep moving, and do the exam.
Avoid pre-praise encouragement such as, You can do it. We all want to be encouraging, yet such encouragement often is intimidating because the child doesnt know if he can do it and may not wish to disappoint. Children often prefer not to try rather than fail. Paradoxically, its more inspiring to predict failure by saying, I bet you cant do this. When the child tries it, even if he doesnt succeed, act surprised. And, if he fails, nothing is lost.

