The biggest success story in ophthalmic surgery has to be cataract extraction and IOL implantation. The procedure has evolved from the ancient (and rather barbaric) couching technique to a high-tech marvel that benefits millions today. Once considered major surgery, cataract extraction has become routine—banal, even.

|

|
Still, the procedure is real surgery, with all its attendant risks. Despite advancements in surgical technology, refinements of the procedure and the expanded skill-set of our surgeons, the most devastating and feared of all complications has actually increased in the last 20 years.
Clear and Present Danger
The late 1990s saw a rise in endophthalmitis rates from 0.087% to 0.265% that corresponded with the popularization of sutureless clear corneal incisions.1 This surgical technique is thought to give exogenous microorganisms easier access to the anterior chamber than scleral tunnel incisions.1 Clear corneal incisions typically allow for quicker healing and more aesthetically pleasing postoperative eyes. The problem, however, is that even with good wound architecture, certain angles of pressure can open the wound with relative ease (as seen in the accompanying video). In cases of poor wound architecture or poor collagen synthesis, wound leakage is a much greater concern.
 |
|
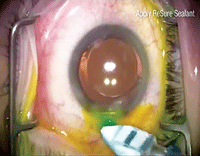
| Go here to see a video of the ReSure gel used for wound closure. |
Wound leak with clear corneal incisions is usually not visible to the surgeon perioperatively because of a wound hydration technique that creates a temporary seal. The onset of clinically identifiable endophthalmitis is typically several days to a week after surgery—putting this devastating complication front and center for comanaging ODs, since most patients are seen only at one-day and one-week follow-ups.
Endophthalmitis—characterized by acute pain, photophobia, decreased vision, increased anterior chamber reaction, hypopyon and conjunctival injection—is immediately sight threatening and thus a time-sensitive emergency. Consultation with the surgeon should be made at the earliest suspicion of occurrence.
In 2005, Taban found a higher rate of endophthalmitis with use of clear corneal incisions (0.19%) vs. traditional scleral tunnel incisions (0.06% to 0.07%).2 However, no prospective clinical trials have evaluated the risk associated with clear corneal incisions.2 Although very rare, the serious nature and small but measurable increased frequency of this complication should keep every comanaging OD vigilant.
Surgeons can decrease the risk of communication between the intraocular space and surface microbes by using a temporary wound sealant after the surgery. In the video, ReSure Sealant (Ocular Therapeutix) is prepared and applied in approximately 20 seconds. It forms a gel in situ, protecting incisions in the immediate post-op period, when wounds are most vulnerable. The hydrogel material contains a blue visualization aid to assist with placement over the incision; it dissipates in a few hours. The hydrogel gradually sloughs off in the tears during reepithelialization, so there is no need for removal of the device.
In our experience this has been well tolerated by patients, with most feeling no different than others who did not experience the gel application. To date, we have yet to see any significant complications with the device. Although our patient volume is entirely too small to get a statistically significant sample size of efficacy, further surgical advancements like this should stem the increase of endophthalmitis cases, while affording our patients the quick, painless recovery they have become accustomed to.
The ReSure gel was just approved in January of this year, reminding us that even an ancient, near-perfect procedure like cataract surgery remains amenable to innovation.
1. Maalouf F, Abdulaal M, Hamam RN. Chronic postoperative endophthalmitis: a review of clinical characteristics, microbiology, treatment strategies, and outcomes. Int. J. Inflam. 2012:313248.
2. Taban M, Behrens A, Newcomb RL et al. Acute endophthalmitis following cataract surgery: a systematic review of the literature. Arch. Ophthalmol. 2005;123(5):613-620.

