 |
A 66-year-old Indian female was examined as an inpatient after she experienced an episode of diplopia following a headache. She reported that the headache, which was present for one month, started around both temples and the occipital region and eventually localized to only the left temple. She was also experiencing double vision for the past two days, which prompted her to go to the emergency room. The patient was found to have a left sixth nerve palsy (CN VI). A CT scan was performed, which was normal. The patient was admitted, and neurology recommended MRI and MRA, which were also normal. At this point, our expertise was consulted.
Exam and Diagnosis
The patient was examined at her bedside. She appeared to be in significant discomfort due to her head pain. She denied jaw claudication or scalp tenderness, though she did report increased fatigue and generalized weakness over the past few weeks. Her visual acuities were 20/30 OD and 20/30 OS. No afferent pupillary defect was noted. Confrontation testing was normal. There was a complete left CN VI nerve palsy. External and anterior segment exams were grossly normal with the exception of bilateral inflamed pingueculae which, according to the patient, had been noted for years. Dilated fundus exam was unremarkable. Her medical history was positive for hypertension, for which she was prescribed carvedilol; however, she reported the hypertension has been under very good control.
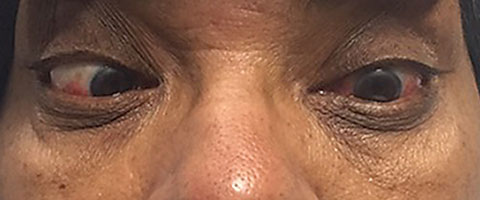 |
| This patient presented with a complete left sixth nerve palsy. |
We confirmed the diagnosis of a left CN VI nerve palsy. Given her normal neuroimaging along with her headache, fatigue and weakness we ordered an ESR and CRP, which were elevated at 80mm/hr and 8.2mg/L, respectively. We started her on 60mg of oral prednisone daily and ordered a temporal artery ultrasound. Twenty-four hours later, the patient was re-examined. Her nerve palsy was unchanged, but she reported almost complete resolution of her headache. Her temporal artery ultrasound revealed a “halo sign” within the left temporal artery, which is indicative of giant cell arteritis (GCA).
The patient was discharged from the hospital and maintained on 60mg prednisone daily. She was referred to rheumatology to manage her GCA and prednisone tapering. One week later, the patient was examined in our office, and we noted a dramatic improvement in the nerve palsy. Repeat ESR and CRP were ordered and reduced at 45mm/hr and 0.9mg/L, respectively. As of our last visit, her nerve palsy had completely resolved and she remains symptom-free on a low dose of prednisone.
GCA is a granulomatous vasculitis affecting medium- and large-sized arteries in older individuals.1 While the temporal artery is often involved, GCA can affect the aorta, cranial arteries and arteries elsewhere throughout the body.1 From an ocular standpoint, GCA can cause sudden and usually severe vision loss from arteritic ischemic optic neuropathy or central retinal artery occlusion.2 Additionally, GCA can lead to cranial nerve III, IV and VI palsies, where the third and sixth nerves are most commonly affected.3
Most CN VI palsies in older individuals are vasculopathic in nature; however, a number of different etiologies exist, including compressive lesions, acute intracranial ischemia, papilledema, herpes zoster virus and GCA.4 When diagnosing a CN VI palsy, evaluate for other accompanying symptoms that may suggest a specific etiology. Although our patient had a history of hypertension, her headache, fatigue and weakness were suspicious for GCA, which prompted us to order the ESR and CRP laboratory tests.
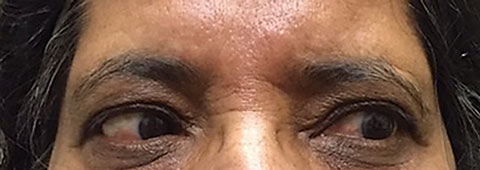 |
| One week after commencing oral anti-inflammatory therapy, this patient showed dramatic improvement of the sixth nerve palsy. It is now completely resolved as of this patient’s last examination. |
Confirmation: Rite of (Diagnostic) Passage
Although the patient’s symptoms, findings and laboratory studies were very suggestive of GCA, it is still recommended to obtain a temporal artery biopsy if you suspect GCA. These patients will require long-term steroid management, which has the potential to cause of number of side effects, so absolute confirmation is essential. While temporal artery biopsy is the gold standard in diagnosis of GCA, it is an invasive surgical procedure. Temporal artery ultrasound can be an efficient and noninvasive alternative with comparable sensitivity and specificity of 85% and 90% respectively.1 In GCA-positive patients, the sonogram shows a halo within the temporal artery due to edema of the arterial wall—referred to as a positive “halo sign.”5 A positive Doppler along with elevated serologic studies as well as clinical symptoms of GCA, as seen in this case, makes the diagnosis highly probable; however, a negative result does not rule out the condition.1
Treatment Outcome: What to Expect
Once steroid treatment is initiated, the nerve palsy and other constitutional symptoms will generally show rapid improvement, as was the case with our patient.6 Although GCA is chronically managed by rheumatologists or vascular specialists, patients will often present initially to us, the optometrists. It is always important to be aware of the various ocular manifestations of GCA in order to lead to a prompt diagnosis.
|
1. Ness T, Bley TA, Schmidt WA, Lamprecht P. The diagnosis and treatment of giant cell arteritis. Deutsches Ärzteblatt Inter. 2013 May;110(21):376-85. 2. Hayreh SS, Podhajsky PA, Zimmerman B. Ocular manifestations of giant cell arteritis. Am J Ophthalmol. 1998 Apr;125(4):509-20. 3. Tamhankar MA, Biousse V, Ying GS, et al. Isolated third, fourth, and sixth cranial nerve palsies from presumed microvascular versus other causes. Ophthalmology. 2013 Nov;120(11):2264-9. 4. Azarmina M, Azarmina H. The six syndromes of the sixth cranial nerve. J Ophthalmic Vis Res. 2013 Apr;8(2):160-71. 5. Black R, Roach D, Rischmueller M, et al. The use of temporal artery ultrasound in the diagnosis of giant cell arteritis in routine practice. Int J Rheum Dis. 2013 Jun;16(3):352-7. 6. Thurtell M, Longmuir R. Third nerve palsy as the initial manifestation of giant cell arteritis. J Neuroophthalmol. 2014 Sep;34(3):243-5. |

