Visual field testing is an important diagnostic consideration in the evaluation of patients with many different types of pathologies. Most commonly, it is used for conditions affecting the optic nerve and other forms of neurological disease; but it’s also helpful for retinal conditions and instances when visual field function needs to be measured.
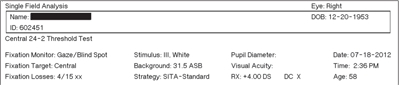
1. The top of the VF printout page contains key information about patient demographics and the type of test that was performed. Always review this portion for accuracy. On the Humphrey Field Analyzer (shown here), the best threshold test is the SITA-Standard. The standard test is better for early detection, while the SITA-Fast test tends to show variable results and is less sensitive.1 The fixation losses are also noted here.
Automated, computerized and threshold static perimetry became available about 30 years ago. While some of the basic principles of interpretation remain, advances in software and hardware have shortened test-taking time and improved accuracy and reliability. Given the subjective nature of the test, it’s essential to differentiate true, disease-related defects and abnormalities from artifact and noise.
Evaluating visual field results from any perimeter can be confusing and daunting at times, especially when attempting to cohesively link all the data together. Good interpretation skills start with a methodical assessment of several key plots, graphs and indices. By following a standardized process on all visual field printouts, clinicians can ensure they are accurately diagnosing ocular disease and/or detecting progression.
For individuals, such as glaucoma patients, who have had a series of visual fields, new analyses are available that greatly help our ability to detect a change in VF defects. In addition, we can measure the rate of disease change as well, giving us powerful insight to our management.
Start at the Top

2. Confirming the validity
of the VF is the second step. Fixation losses, false positives and
false negatives are recorded—with false positives often being the most
critical. An error rate of 5% to 10% significantly affects the
appearance, making the gray scale and other plots appear better than
they really are.1 Do not follow old published guidelines of up to a 33% acceptance rate.1
While the printouts from different perimeters do not look identical, much of the displayed content and information is the same. Regardless of the instrument used, start at the top by locating information about the test parameters (figure 1) and reliability indices.
• Test parameters. Make sure the patient’s birthdate is accurate, because the test results are compared to a normative database. Identify that the proper trial lens was calculated and utilized. Although a standard test program and pattern (e.g., 24-2, Threshold) is often selected for the majority of patients, be sure to confirm that the correct test was selected.
• Reliability indices. Examining the reliability indices is the next key step in visual field interpretation (figure 2). High fixation losses (more than 15% to 20%) are a strong indication that the test results are likely inaccurate. One way to reduce fixation losses is to make sure your technician properly aligns the patient and monitors their attention during the test.
False positives, another key index, help to identify a “trigger happy” patient who is pushing the response button even when no light stimuli are presented. The field may often look normal or “cleaner” (with fewer defects depicted) on patients with values of 5% to 10% or higher.
False negatives are identified when the patient does not respond to a light stimulus that should have been detected, based upon earlier responses. Values of 10% to 15% or more are indicative of a patient who is not paying good attention during the course of the test; the results may look worse than they really are.
After reviewing these key data points, the next part of the page can be evaluated.
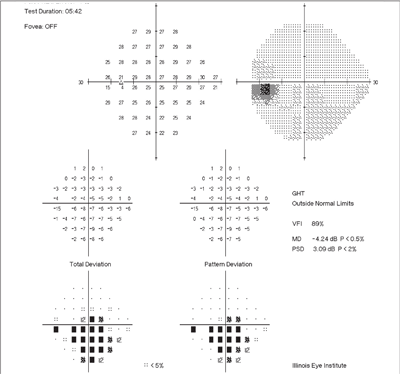
3. In this classic example, the patient has moderate to advanced stage glaucoma. The large inferior defect is clearly depicted and appears similar on both the total and pattern deviation plots. Of note, the gray scale does not show the defect, which is due to an interpolation error in the scaling. Remember, do not rely solely on the gray scale when evaluating visual fields.
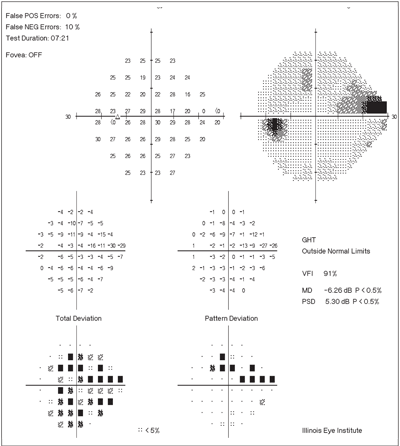
4. This patient has a mild cataract and glaucoma. The generalized depression from the cataract is evident on the TD plot (lower left). The localized defect—a superior nasal step with an arcuate component—caused by the glaucoma is seen on the PD plot. Additional key indicators—the global indices—are on right side of the page. The glaucoma hemifield test (GHT) is a sensitive indicator of differences between the superior and inferior hemifields. The VFI is an overall marker of field loss similar to the MD. Patients with values below 70% may begin to notice functional defects.
Don’t Get Lost in the Middle
The middle part of any visual field printout page can be confusing, with its multiple graphs and plots. There are plots that display the “raw data” in decibels (dB) from the patient’s test. While the dB values can be helpful when there is conflicting information on the printout, they often don’t need to be examined in detail.
• Gray scale. The gray scale of the VF printout is an easy plot to use for quick identification of potential scotomas and depressions, as well as getting a general assessment about the location and size of any defect. One common mistake in VF interpretation is that the clinician looks only at the gray scale (figure 3). Doing this can lead to inaccurate identification of VF loss. Rather, the gray scale should be viewed as a starting point, as two other plots—total deviation (TD) and the pattern deviation (PD)—must be assessed to get the full and accurate clinical picture.
• Total deviation. The TD plot shows all the portions of the patient’s visual field that are different from a “normal” patient’s field of the same age. It is a key graph that can be best assessed by using the probability plots with the shaded boxes at each test location, and not the numerical dB plot.
Solid, fully black squares indicate test points that are statistically more likely to be abnormal compared to the other, lighter shades of gray. When examining the TD plot, look at the size, shape and location of any abnormal points/boxes. Often, a generalized depression (perhaps from a cataract) is noted on this plot, with darkly shaded squares uniformly filling up the grid (figure 4). However, when trying to identify a visual field defect related to glaucoma or lesions along the visual pathway, localized defects (not generalized) are the key finding. Localized defects will appear on the TD plot, but may be hidden by a generalized depression caused by a corneal or lenticular opacity. To separate the localized defect (likely the true disease-related defect) from any defect caused by a media opacity, the PD plot must be examined.
• Pattern deviation. As with the TD plot, the PD plot is best analyzed by using the shaded boxes on the probability plot. The PD plot is designed to highlight localized defects by “removing” generalized visual field loss (likely due to a cataract). True defects on the PD should be characterized by their shape and location (i.e., nasal steps, central and arcuate scotomas). Clusters of adjacent points can be grouped together so that their particular shape can be associated with the correlating disease or lesion.
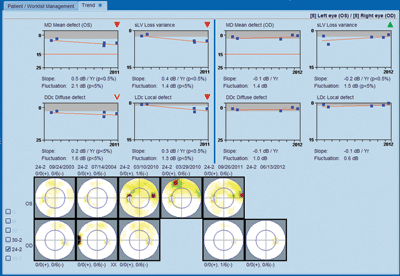
5. This is a progression analysis printout (EyeSuite, Haag-Streit) for a patient with advancing glaucoma in the left eye. EyeSuite uses the mean defect (same as mean deviation) value, among others, to plot the rate of change. In this example with visual field tests from 2003 to 2011, there is a negative slope to the MD. Red triangles generated by the software alert the clinician.
The Final Step
The key indicators that remain are often found on the right side of the printed page. Thus, the middle part of the printout should be read from left to right, proceeding from total to PD plots and then to the global indices. The global indices give a numerical quantification in decibels of the visual field loss that appears on the page.
The mean deviation or mean defect (MD) gives an overall value of the total amount of visual field loss, with normal values typically within 0dB to -2dB. The MD value becomes more negative as the overall field worsens—a common example is when a cataract progresses.
Using MD for tracking changes to localized field loss (as in glaucoma) is limited. For patients with a localized visual field defect, the pattern standard deviation (PSD) best quantifies the amount of loss as well any progression of glaucoma in the early stages. Note that the PSD is not helpful in tracking advanced glaucomatous defects. Despite its limitations, the MD value can be helpful in tracking moderate stage glaucomatous visual field loss (-6dB to 12dB), because at this point the amount of localized loss is significant enough to be tracked.
On the Humphrey Field Analyzer, the visual field index (VFI)—a value similar to the MD—was added to the printout several years ago. The VFI is a staging index for the total amount of field loss. It is reported to be less sensitive to cataracts.1 Values range from 100% (normal) to 0% (perimetrically blind). The percentage value can be tracked over a series of tests and used as one indicator for progression.
New Data Analysis for Chronic Disease
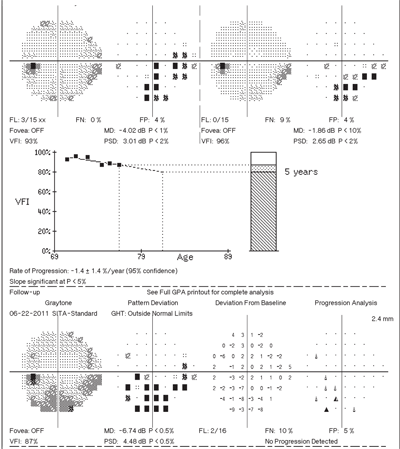
6. This is a progression analysis printout (Guided Progression Analysis, or GPA, Humphrey Field Analyzer) for a patient with advancing glaucoma in the left eye. The two baseline fields are on the top while the most recent test is on the bottom. In the middle is a trend line analysis, which is a regression line of the VFI values for the series of tests. The slope of this line is plotted as a rate of change indicator. While many variables must be considered, values of -1.5% or more should be considered high, and more aggressive therapy may be indicated.1
Accurate progression analysis of VF changes is essential to monitor patients with optic nerve disease, particularly glaucoma. In the past, the trend or change analysis provided on the printout was very limited. Clinicians resorted to looking back over multiple VF pages scattered within the patient’s chart. They could also try to track the MD or PSD to see if individual values got worse or stayed the same. Practically speaking, this was a tedious and time-consuming task. Instead, some doctors simply looked only at the gray scale to see if the defect got larger or darker—but doing so could lead to major errors in VF interpretation.
New perimeters incorporate a much more accurate tracking system for decibel values. Using the most recent software packages, they are able to display trend lines that can quantify the rate of change to the visual field defect (figure 5). These trend lines are a statistical regression line analysis of the MD value or a similar value that reflects the overall field sensitivity. New perimeters can produce graphs with a regression line based upon a series of visual fields over a time period.
A line with a negative slope indicates worsening of the VF defect. The slope of this line can be calculated by the perimeter and provide the rate of loss. Identifying the rate of change (loss) in a glaucoma patient is a new piece of information that allows differentiation of “slow” progressors that have a shallow, sloped trend line as compared to “rapid” progressors with a very step slope trend line.
Some progression analysis plots can also provide a five-year projection of VF loss, assuming no change in treatment or underlying disease. An example of this is seen in the Humphrey Field Analyzer GPA printout that uses the VFI (figure 6).
These progression plots have had the largest impact on patient management for chronic disease, significantly improving any clinician’s ability to identify change. With a little experience, they are easily read and understood. Unfortunately, their use is not widespread, either from lack of awareness or from doctors and clinics using outdated software. Practitioners should evaluate their current perimeter and investigate options for upgrading hardware and or software so that they can use the newest tools.
Dr. Chaglasian is an associate professor at Illinois College of Optometry and chief of staff of the Illinois Eye Institute, in Chicago.
1. Heijl A, Patella VM, Bengtsson B. The Field Analyzer Primer: Effective Perimetry. 4th ed. Dublin, CA: Carl Zeiss Meditec; 2012.

