
|
As a practice that emphasizes children, specialty contact lenses and research (including myopia control research), we often are referred patients seeking an alternative method of vision correction to reduce myopia progression. These patients are among the more than 41% of people in the United States suffering from myopia.1 Although there are currently no interventions that cease myopic progression, it has been suggested that a number of treatment options can decrease its progression.
If we can slow this progression in children, not only could we potentially reduce the cost of U.S. vision care, but also possibly save them from the devastating vision loss due to myopic retinopathy, retinal detachment and glaucoma that is associated with myopia.2-4
Like many practitioners, we have found it challenging at times to address parent and patient questions regarding the methods and treatment options to stop or slow the progression. However, with several studies ongoing and many on the verge of publication, we might soon have more answers.
In the last decade, we have seen an increasing interest in research to slow myopia progression—especially in children, given that we see the greatest amount of myopia progression before adulthood. Evidence has shown a reduction in progression using a number of treatments, including anti-muscarinic therapy and orthokeratology.
While some of these treatment modalities have been approved in other countries, there are no FDA-approved treatment methods specifically targeting myopia control in the United States. As such, you will need to explain to patients that these interventions are off-label should you decide to use them in practice.
Spectacles
While these various spectacle lens options offer mild help for some patients, we have not seen the significance to be large enough in our clinic to actively recommend any type of lens for patients on a regular basis.
However, if a child is progressing in myopia and is unwilling or unable to use any of the other methods, we will consider progressive addition lenses (PALs). Additionally, we are keeping our eyes peeled on the studies looking at novel spectacle lens options for patients.
Undercorrected Single Vision Lenses
Parents often get concerned when their children’s spectacle prescriptions increase, fearing that their child will end up highly myopic. So, many times, they ask us to prescribe lenses that are not as strong in order to “keep their child’s prescription from getting worse.” The bottom line is there’s no evidence to back it up—in fact, it’s just the opposite.
A 2006 study looked at myopic children between ages six and 15 years old over a period of 18 months.5 Twenty-three of the participants were fully corrected, while 25 were undercorrected by +0.50. Although statistically insignificant, there was a slight progression of myopia (0.17D) in the children who were undercorrected.5
A 2002 study showed similar results of increased myopia progression (0.23D) over a two-year period.6 Although the increase was not significant, both studies suggest that undercorrecting myopes has a negative effect on the progression of myopia.5-6 Ergo, undercorrected single vision lenses should not be used for slowing the progression of myopia.
At our practice, we bring patients with a history of increasing myopia corrected by spectacle lenses back for refraction in six months to ensure their myopia is not progressing further. If we note that their myopia has progressed, we will make a change to their spectacles rather than waiting another six months (one year total), as we do not want them to be undercorrected for a significant period of time.
The data shows undercorrected children progress faster in their myopia—therefore, we make sure these children have a new update prescription as soon as their eyes change in an effort to stabilize their vision as best as possible.5-6
Traditional Bifocal Glasses
Since Dr. Robert Wick first reported on the use of bifocals to correct myopia in 1947, practitioners have been using them with varied success.7 One study noted that myopic children who were appropriately corrected showed an accommodative response to near objects that was weaker than emmetropic patients.8
This inspired the hypothesis that patients with progressing myopia who have a decreased accommodative response may have a slight blur on the retina that stimulates increased myopia development. Thus, bifocal glasses may offer a benefit, as they compensate for the reduced accommodative response, especially in children who are esophoric as they show an even greater accommodative lag.
In 2000, researchers randomized 82 myopic children with esophoria to bifocals or single vision lenses. They found that bifocals reduced the progression of myopia by 0.25D over 30 months compared to single vision lenses.9 The mean change in vitreous chamber depth was 0.36 +/- 0.34mm in the bifocal group and 0.48 +/- 0.28mm in the single vision group. Overall, there was a 20% reduction in myopia progression with bifocal lenses vs. the single vision lens counterpart.9 Older studies have suggested that bifocals could provide reduction in myopia progression of 44% or more.10
Progressive Addition Lenses
Given the improvements that progressive addition lenses (PALs) offer to adult patients with presbyopia, it makes sense to consider using PALs for children with decreased accommodative issues and as a consideration for decreasing myopia’s progression.
PALs offer many advantages to patients, but for young children and adolescents, the appearance of the lenses cannot be overstated. Patients enjoy the smooth transition of vision from their distance to near vision without the distinct junction line. One of the inherent drawbacks to PALs is that there can be an adaptation period where the patient experiences peripheral distortion, and some patients are unable to adapt to PALs.
The Correction of Myopia Evaluation Trial (COMET) looked at the effect of PALs compared to single vision lenses on myopic progression.11 Investigators enrolled 469 subjects, age six to 11, with myopic prescriptions between -1.25 and -4.50 spherical equivalent. One arm of the study had single vision distance correction while the other had PAL lenses with a +2.00 add.
The researchers looked at the progression of myopia through cycloplegic refraction over the course of three years, and found a difference between PAL and single vision lenses of 0.20 D.11 Although their findings were statistically significant, the authors concluded that the use of PALs as a clinically significant treatment option is not warranted on a routine basis. Considering the significant cost of PALs compared to single vision lenses and how minimal the reduction is, PALs do not merit the frequent use that we currently see in the optometry field.
One theory related to myopia progression suggests a correlation to hyperopic defocus in the peripheral retina. One recent study looked at a control group of single vision-wearing children and compared them to patients wearing lenses that were intended to reduce peripheral hyperopic defocus.12 In this 12-month study, there was no statistically significant difference between the novel designs and the control group. However, when evaluating the differences between the control group and children who were younger (six to 12 years) with a parental history of myopia, there was a difference of 0.29D.12
Contact Lenses
Now that optometrists are fitting younger children with contact lenses, they are a much more viable option for treating myopia progression. While many children feel insecure about wearing glasses, contact lenses have been found to improve their self image and self worth, allowing them to both see and feel better.13
However, there are some drawbacks—namely, the possibility of infection and increased chair time. Luckily, the array of contact lenses in today’s market gives us plenty of options to find the right fit for each patient.
Gas Permeable Contact Lenses
Gas permeable (GP) contact lenses have been used in practice for years in attempts to slow myopia progression. The possible mechanism behind GPs slowing myopia progression is in the improved retinal image compared to other forms of correction, the flattening of the cornea with GP wear and/or an
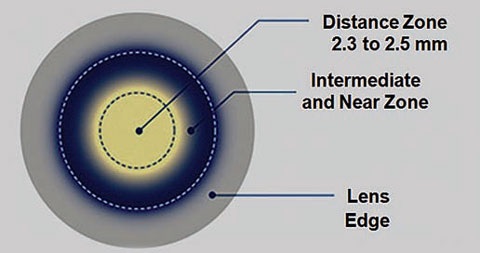 |
| Center distance multifocal contact lenses are a form of peri-focus lens design for myopia control. Customized design and visual axis registration may be required to optimize refractive therapy. |
overcorrection for myopic patients when fitting contact lenses.14 Many studies have looked at the relationship between GPs and myopia progression; one of the more recent studies concluded that rigid GPs didn’t slow the rate of myopia progression, even among children who used them regularly.14
In this study, the children assigned to GP contact lenses (105) remained more myopic by 0.20D than those in the spectacle group did (192).14 The study authors concluded GP contact lenses likely did not hold any promise for slowing the rate of myopia progression in children.
While GP lenses are effective for vision correction and offer a fantastic option for children just starting lens wear, we do not recommend discussing them as a treatment option for myopia progression. We typically reserve these for more complicated patients who have some sort of astigmatism (regular or irregular), purely because of their adaptation time.
Soft Spherical Contact Lenses
Soft contact lenses are used readily in the United States and elsewhere. As they are a popular option for vision correction, patients often discuss them during a myopia progression assessment. The Adolescent and Child Health Initiative to Encourage Vision Empowerment (ACHIEVE) study found that soft contact lenses do not cause a clinically relevant increase in myopia.15
The rate of change per year was 0.06D greater in soft contact lens wearers than spectacle wearers, which was not a statistically significant difference—even after three years.15
We don’t feel, in our practice, that such a minute increase warrants eliminating soft contact lenses as a potential option for vision correction in children with myopia.
Usually, we choose a single-use disposable lens for these patients in an effort to emphasize compliance and reduce maintenance. However, we do not turn to soft contact lenses as a modality for myopia reduction.
Multifocal Soft Contact Lenses
Multifocal and bifocal soft contact lenses have reemerged in the spotlight with regards to myopia progression.
In one study, myopia progression and eye elongation were reduced significantly with the use of bifocal contact lenses.16 Forty children, age 11 to 14, wore a dual-focus lens in one randomly assigned eye and a single vision distance lens in the fellow eye for 10 months. The lenses were then swapped between eyes and worn for another 10 months.
Researchers found that for 70% of the children, myopia progression was reduced by 30% or more in the eye wearing the bifocal lens compared to the single vision lens.16 The data suggest that with bifocal lenses, the sustained myopic defocus can slow myopia progression without compromising visual function—even when presented to the retina simultaneously with a clear image.16
|
| Image of a 20-year-old female patient who was successfully fitted with overnight ortho-k lenses when she nearly 12 years old. Photo: Joseph Ruskiewicz, O.D., M.P.H.
|
However, we still need a better understanding of the design type (near center v. distance center) that needs to be used and the amount of add power to provide the most appropriate retinal image and blur to achieve the best results. One identical twin study showed that a distance center lens achieved greater success in the eyes wearing the multifocal lens.17 At our practice, we use multifocal lenses as an off-label treatment for patients progressing in their myopia. As the research is still emerging, however, we typically do not use multifocal lenses as a first-line treatment.
Instead, we see this as an option for children who have higher amounts of refractive error and would be more difficult to fit with orthokeratology lenses. Additionally, if a patient has a large amount of cylinder, we will order a lens that is multifocal and toric. We use lenses with distance center and higher adds—typically in the realm of +3.00 to +4.00.
Although we do not have published evidence to back up our treatment methods yet, through our relationship with the clinical and research team in Pacific University’s contact lens department we believe that the higher add powers are more effective than lower add powers.
One major drawback is that this eliminates the use of many of the standard multifocal lenses that are in stock. Instead, the lenses must be custom made or ordered directly from the manufacturer or distributor.
|
| A recent review of myopia treatments in children found that anti-muscarinic eye drops had the largest positive effects for slowing myopia progression. Photo: NEI/NIH
|
Anti-Muscarinic Therapy
A recent review that included 23 clinical investigations of myopia treatments in children found that anti-muscarinic medications (eye drops) had the largest positive effects for slowing myopia progression.18 At one year, children receiving pirenzepine gel, cyclopentolate eye drops or atropine eye drops showed significantly less myopic progression compared with children receiving placebo.18
In Singapore, researchers used topical atropine on 400 myopic children ages six to 12 years. The treatment was found to be well tolerated and effective in slowing the progression of low and moderate myopia and ocular axial elongation in Asian children. The mean reduction of myopia in the atropine-treated eyes was 0.03 +/- 0.50D, while there was progression of myopia of -0.76 +/- 0.44D in the placebo-treated eyes.19
Although this intervention appears to be somewhat effective, it is not a first-line treatment in our office due to the potential side effects that are encountered by anti-muscarinic medications.18
Orthokeratology
Orthokeratology has long been used to treat myopia in adults and children, with great success for daily vision without the aid of glasses or daytime contact lenses. Throughout the years, practitioners have begun to notice that their younger patients have had a reduction in their myopia progression as a result of using orthokeratology lenses. In recent years, several studies have come out with evidence that appears to mirror this anecdotal experience.20-22
The Longitudinal Orthokeratology Research in Children (LORIC) study followed 35 children over a two-year period. Researchers looked at children wearing ortho-k lenses and compared them to a historical control group of children wearing single vision lenses.20 Rather than comparing the refractive outcomes of the children, the LORIC study evaluated axial length changes.
Following the two-year study, the ortho-k group increased in their myopia by 0.29mm vs. 0.54mm in the control group.20 A similar study looked at children wearing ortho-k lenses vs. a control group of children wearing soft lenses. 21 These researchers also followed participants for two years and found a similar reduction in the progression of axial length elongation.21
|
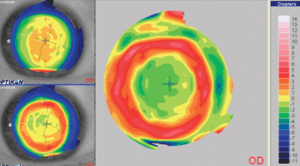
| Pre- and post-treatment corneal maps, as well as a difference map for a child being corrected with orthokeratology lenses. Not only is the central cornea reduced in power, the mid-periphery is actually increased in power. Photo: Jason Jedlicka, O.D
|
Currently, we are awaiting the completion of the five-year Stabilization of Myopia by Accelerated Reshaping Technique (SMART) trial, which will end next year.22 It is the largest clinical investigation yet to look at whether overnight vision correction with orthokeratology lenses can stop myopia progression in children.
Researchers have been following 200 children, ages eight to 14, who were separated into groups at the start of the study—one wearing ortho-k lenses and other wearing conventional soft contact lenses. Interim results showed that participants wearing overnight ortho-k lenses experienced a minimal change in myopia after three years of wear, while the average prescription level had worsened in the soft lens wearers.25
Ortho-k is the number one myopia progression treatment method for patients referred to our office. We discuss its off-label status with parents; however, we believe that the current literature supports the clinical use of the lenses as an excellent option for our patients.
We talk with them about the studies, explaining their limitations and smaller sample size, as well as the anecdotal success that practitioners have had with these lenses for decades. We also review the limited options on the market and explain to parents why we believe that their child is best suited for ortho-k lenses.
With so many potential treatment options, there is a lot to look forward to for the future. At this time, the literature and research point us in the direction of using ortho-k and bifocal soft contact lenses for the greatest decrease in the progression of myopia.
David Kading, O.D., owns Specialty Eyecare Group in Seattle, a group practice with multiple locations. He specializes in anterior segment disease and custom contact lens fitting. Amber Mayberry, a 4th year student at University of Saint Louis Missouri College of Optometry, is an optometric intern at Specialty Eyecare Group.
1. Vitale S, Sperduto RD, Ferris FL 3rd. Increased prevalence of myopia in the United States between 1971-1972 and 1999-2004. Arch Ophthalmol. 2009 Dec;127(12):1632-9.
2. Celorio JM, Pruett RC. Prevalence of lattice degeneration and its relation to axial length in severe myopia. Am J Ophthalmol. 1991 Jan 15;111(1):20-3.
3. Sørensen KE, Baggesen K. Retinal detachment following intracapsular cataract extraction. Acta Ophthalmol (Copenh). 1990 Oct; 68(5):549-53.
4. Saw SM, Katz J, Schein OD, et al. Epidemiology of myopia. Epidemiol Rev. 1996;18(2):175-87.
5. Adler D, Millodot M. The possible effect of undercorrection on myopic progression in children. Clin Exp Optom. 2006 Sep;89(5):315-21.
6. Chung K, Mohindin N, O’Leary DJ. Undercorrection of myopia enhances rather than inhibits myopia progression. Vision Res 2002 Oct;42(22):2555-9.
7. Wick RE. The use of bifocals in myopia; a case report. Am J Optom Arch Am Acad Optom. 1947 Aug;24(8):368-71.
8. Gwiazda J, Thorn F, Bauer J, Held R. Myopic children show insufficient accommodative response to blur. Invest Ophthalmol Vis Sci. 1993 Mar;34(3):690-4.
9. Fulk GW, Cyert LA, Parker DE. A randomized trial of the effect of single-vision vs. bifocal lenses on myopia progression in children with esophoria. Optom Vis Sci. 2000 Aug;77(8):395-401.
10. Goss DA, Uyesugi EF. Effectiveness of bifocal control of childhood myopia progression as a function of near point phoria and binocular crosscylinder. J Optom Vis Dev. 1995 June;26(2):12-7.
11. Gwiazda J, Hyman L, Hussein M, et al. A randomized clinical trial of progressive addition lenses versus single vision lenses on the progression of myopia in children. Invest Ophthalmol Vis Sci. 2003 Apr;44(4):1492-500.
12. Sankaridurg P, Donovan L, Varnas S, et al. Spectacle lenses designed to reduce progression of myopia: 12-month results. Optom Vis Sci. 2010 Sep; 87(9): 631-41.
13. Walline JJ, Jones LA, Sinnott L, et al. Randomized trial of the effect of contact lens wear on self-perception in children. Optom Vis Sci. 2009 Mar;86(3):222-32.
14. Katz J, Schein OD, Levy B, et al. A randomized trial of rigid gas permeable contact lenses to reduce progression of children’s myopia. Am J Ophthalmol. 2003 Jul;136(1):82-90.
15. Walline JJ, Jones LA, Sinnott L, et al. A randomized trial of the effect of soft contact lenses on myopia progression in children. Invest Ophthalmol Vis Sci. 2008 Nov;49(11):4702-6.
16. Anstice NS, Phillips JR. Effect of dual-focus soft contact lens wear on axial myopia progression in children. Ophthalmology. 2011 Jun;118(6):1152-61.
17. Aller TA, Wildsoet C. Bifocal soft contact lenses as a possible myopia control treatment: a case report involving identical twins. Clin Exp Optom. 2008 Jul;91(4):394-9.
18. Walline JJ, Lindsley K, Vedula SS, et al. Interventions to slow progression of myopia in children. Cochrane Database Syst Rev. 2011 Dec 7;(12):CD004916.
19. Chua WH, Balakrishnan V, Chan YH, et al. Atropine for the treatment of childhood myopia. Ophthamology. 2006 Dec;113(12):2285-91.
20. Cho P, Cheung SW, Edwards M. The longitudinal orthokeratology research in children (LORIC) in Hong Kong: a pilot study on refractive changes and myopic control. Curr Eye Res. 2005 Jan;30(1):71-80.
21. Walline JJ, Jones LA, Sinnott LT. Corneal reshaping and myopia progression. Br J Ophthalmol. 2009 Sep;93:1181-5.
22. Eiden B, Davis R. Stabilization of myopia by accelerated reshaping technique. Presented at Global Specialty Lens Symposium, January 2011; Las Vegas.

