
Clinicians and scientists have long noted a strong correlation between cigarette smoke and myriad health concerns, including cancer, respiratory disease and cardiovascular disease. Tobacco use is projected to kill a billion people during the 21st century.1,2
Cigarette smoke contains toxic chemicals such as nicotine, cyanide, benzene, formaldehyde, methanol, acetylene and ammonia, not to mention tar, carbon monoxide and nitrogen oxide.1 Nicotine in particular can have many different effects on the body, including:3
- Decreases appetite; fear of weight gain makes some people unwilling to stop smoking
- Boosts mood, giving people a sense of well-being
- Increases intestinal activity
- Creates more saliva and phlegm
- Increases heart rate by about 10 to 20 beats per minute
- Increases blood pressure by 5mm Hg to 10mm Hg
- Stimulates memory and alertness; people who use tobacco often depend on it to help them accomplish certain tasks and perform well
Beyond Cigarettes
Cigarettes are not the only delivery method for tobacco—there are many non-cigarette forms of tobacco and nicotine, and their use varies regionally and globally. Smoked forms of tobacco such as cigars, traditional pipes and water pipes are highly popular and are often perceived as significantly less hazardous than cigarettes. Novel nicotine delivery systems not directly reliant on tobacco, such as electronic cigarettes, are becoming increasingly popular, and their emergence presents challenges and opportunities for public health.
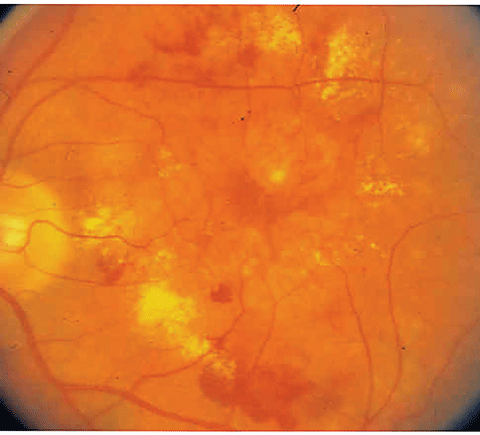 |
| Wet AMD in a life-long smoker. Smoking reduces cellular antioxidants in various ocular tissues, especially the retina. Click image to enlarge. |
Research suggests that some tobacco and nicotine products may pose less of a health hazard than cigarette smoking, potentially playing a role in reducing morbidity and mortality due to smoking.4 However, evidence also suggests the public broadly misperceives the relative risks of smoking, tobacco use and nicotine, erroneously thinking smoked tobacco products other than cigarettes, such as cigars and pipes, are harmless.5
Cigars
According to the Centers for Disease Control and Prevention, cigar consumption more than doubled in the United States from 2000 to 2011, from slightly less than 6.2 billion in 2000 to more than 13.7 billion in 2011.6 Unlike nearly all cigarette smokers, most cigar smokers do not inhale. However, even if a cigar smoker doesn’t intentionally inhale, potentially harmful amounts of nicotine can be absorbed through the lining of the mouth.11 For some, switching from cigarettes to cigars can be particularly harmful because they might inhale cigar smoke the way they inhaled cigarette smoke.11
Although cigar smokers have lower rates of lung cancer, coronary heart disease and lung disease than cigarette smokers, they do have higher rates of these diseases than those who do not smoke cigars.6,7
Cigar smoke contains many of the same toxic constituents as cigarette smoke, and research shows cigar smoke has higher levels of tobacco-specific nitrosamines (TSNAs) than cigarette smoke, due to cigar tobacco’s curing and fermentation process.7 Many of these TSNAs, such as N-nitrosonornicotine and nicotine-derived nitrosamine ketone, are known carcinogens.7 Investigators have also found that cigar smoke has higher levels of carbon monoxide and nitrogen oxide than cigarette smoke.7 The International Agency of Research on Cancer found that cigar smoking, pipe smoking or both is causally connected to cancers of the pancreas, stomach, urinary tract and bladder, lung and upper digestive tract, including the oral cavity, oropharynx, hypopharynx, larynx and esophagus.8,9
More specifically, a systematic review of published studies on current cigar smoking and all-cause and cause-specific mortality risks found that primary cigar smoking (i .e.,current, exclusive cigar smoking with no history of previous cigarette or pipe smoking) was associated with all cause-mortality; oral, esophageal, pancreatic, laryngeal and lung cancers; coronary heart disease and aortic aneurysm.10
The researchers also noticed strong dose trends by cigars per day and inhalation level for primary cigar smoking for oral, esophageal, laryngeal and lung cancers. Among primary cigar smokers reporting no inhalation, relative mortality risk was still elevated for oral, esophageal and laryngeal cancers.10
Table 1. |
Although mortality risks from cigar smoking vary by level of exposure (cigars per day) and inhalation level, evidence suggests cigar smoking carries many of the same health risks as cigarette smoking.10 Future studies will hopefully collect detailed information on cigar type, exposure level and biomarkers of exposure and potential harm.10
Ocular Considerations
Repeated exposure to tobacco smoke accelerates the body’s aging process, including that of ocular tissues (Table 1).12 The chemicals in cigarette smoke reduce the body’s ability to protect itself by concurrently increasing the levels of oxidants and decreasing the levels of antioxidants.1 Smoking causes blood vessels throughout the body to narrow and stiffen, known as arteriolar sclerosis. It also reduces the amount of oxygen in the blood, thus reducing the amount of oxygen reaching the retina. Research suggests that cigarette smoke-related tar triggers the formation of drusen.11
Inhaling these toxic chemicals, even briefly, significantly increases the risk for cataract, age-related macular degeneration (AMD) and ocular ramifications of cardiovascular disease—and the more a person smokes, the higher the risks. Added to that, tobacco smoke, including second-hand smoke, is an irritant that worsens dry eye disease.1,2
For patients diagnosed with AMD and diabetic retinopathy, smoking increases their risk of serious vision loss.12,13 Patients with Graves’ disease who smoke have a fourfold increased risk of developing ocular complications compared with non-smokers.13
Fortunately, after people quit smoking, their risk for these ocular diseases becomes almost as low as for people who never smoked.1,2,3
In our next column, we will discuss pipes, hookahs, e-cigs and smoking cessation strategies.
|
1. Centers for Disease Control and Prevention. 2010 Surgeon General’s Report—How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease. Atlanta, GA:2010. 2. Benowitz NL, Brunetta PG. Smoking hazards and cessation. In: Broaddus VC, Mason RJ, Ernst JD, et al., eds. Murray and Nadel’s Textbook of Respiratory Medicine. 6th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 46. 3. Rakel RE, Houston T. Nicotine Addiction. In: Rakel RE, Rakel DP, eds. Textbook of Family Medicine. 9th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 49. 4. Le Houezec J, McNeill A, Britton J. Tobacco, nicotine and harm reduction. Drug Alcohol Rev. 2011 Mar;30(2):119–23. 5. O’Connor RJ, McNeill A, Borland R, et al. Smokers’ beliefs about the relative safety of other tobacco products: findings from the ITC collaboration. Nicotine Tob Res. 2007 Oct;9(10):1033–42. 6. Centers for Disease Control and Prevention (CDC). Consumption of cigarettes and combustible tobacco—United States, 2000–2011. MMWR Morb Mortal Wkly Rep 2012;61:565–9. 7. Hoffmann D, Hoffmann I. Chemistry and Toxicology. National Cancer Institute, Smoking and Tobacco Control, Monograph 9: Cigars Health Effects and Trends. 1998:55-104. http://cancercontrol.cancer.gov/brp/tcrb/monographs/. 8. IARC Working Group on the Evaluation of Carcinogenic Risks to Humans. Tobacco smoke and involuntary smoking. IARC Monogr Eval Carcinog Risks Hum. 2004;83:1–1438. 9. Sasco AJ, Secretan MB, Straif K. Tobacco smoking and cancer: a brief review of recent epidemiological evidence. Lung Cancer. 2004;45 Suppl 2:S3–9. 10. Chang CM, Corey CG, Rostron BL, Apelberg BJ. Systematic review of cigar smoking and all cause and smoking related mortality. BMC Public Health. 2015;15:390. 11. Hurt RD, Murphy JG, Dunn WF. Did we finally slay the evil dragon of cigarette smoking in the late 20th century?: unfortunately, the answer is no - the dragon is still alive and well in the 21st century and living in the third world. Shame on us! Chest. 2014;146(6):1438-43. 12. Khan JC, Thurlby DA, Shahid H, et al. Smoking and age-related macular degeneration: The number of pack years of cigarette smoking is a major determinant of risk for both geographic atrophy and choroidal neovascularization. Br J Ophthalmol. 2006;90:75-80. 13. Solberg Y, Rosner M, Belkin M. The association between cigarette smoking and ocular diseases. Survey of ophthalmology. 1998;42(6):535-47. |

