 History
History
A 48-year-old black female presented for a comprehensive eye examination. She explained that after having a stroke five years ago, she has had trouble seeing objects in her far left periphery. She also complained of persistent ocular dryness, despite the use of artificial tears.
Her ocular history was significant for dry eye O.U. Her systemic history was remarkable for hypertension, diabetes, cardiac pathology and a prior cerebrovascular accident (CVA). She reported that these conditions were well controlled with the use of metformin, glyburide, hydrochlorothiazide and Tarka (trandolapril/verapamil hydrochloride, Abbott Laboratories). She also reported an allergy to erythromycin.
Diagnostic Data
Her best-corrected visual acuity measured 20/20 O.U. at distance and near. External examination uncovered full extraocular muscle motilities and normal pupillary responses. Confrontational testing showed visual field loss located in the nasal periphery O.D. and temporal periphery O.S. The defects were located below the horizontal midline in each eye.
Evaluation of the anterior segment revealed a scant tear film and scattered areas of superficial punctate keratitis O.U. Intraocular pressure measured 16mm Hg O.U.
On dilated fundus evaluation, the patient exhibited a cup-to-disc ratio of 0.60 x 0.60 O.U. with deep excavation. We saw no signs of optic nerve pallor or edema O.U. All other aspects of her posterior segment were normal. The pertinent results from the automated visual field testing are illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
Discussion
Additional testing included separate measurements of afferent visual function, such as color vision testing, red cap desaturation, brightness sense, confrontational visual field evaluation using colored targets, and optokinetic nystagmus evaluation. Neuroimaging on MRI—both with and without contrast—was ordered. We also scheduled scanning laser ophthalmoscopy, gonioscopy and pachymetry testing.
The diagnosis in this case is left inferior homonymous hemianopsia secondary to prior CVA. A recent brain MRI ordered by the patient’s primary care provider showed encephalomalacia involving the posterior right frontal and parietal lobes that was consistent with previous infarction. There was no evidence of acute infarct or hemorrhage at the time of imaging. We also noted evidence of punctate signal abnormalities in the left parietal region that were consistent with chronic small vessel disease.
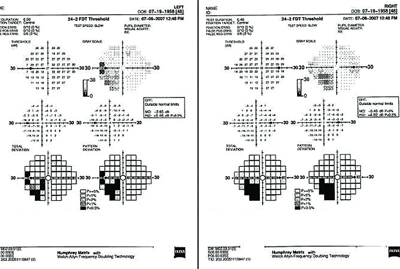
Here are the visual field results of our 48-year-old patient who complained of
difficulty seeing in her far left periphery. What do you notice?
Inferior homonymous hemianopic defects often suggest involvement of the optic radiations in the superior parietal lobe. These defects usually are more congruous than those produced by lesions of the temporal lobe. If the lesion is large enough, a complete homonymous hemianopsia with macular splitting may result.1 Other features of parietal lobe involvement include conjugate eye movements to the side located away from the lesion on forced lid closure—often referred to as Cogan’s sign or an abnormal optokinetic response. “Word blindness” and visual agnosia may result when the left angular gyrus, found in the posterior portion of the parietal lobe, is affected.1
Involvement of the post-central convolution can cause sensory seizures that produce a sensation of tingling or numbness. A lesion located in the dominant parietal lobe can lead to the development of Gerstmann’s syndrome, which is defined by finger agnosia, right-left disorientation, agraphia, acalculia and associated homonymous hemianopia.1 Lesions of the non- dominant lobe may cause disturbances in spatial orientation as well as homonymous hemianopsia.1
Recent research has shown that homonymous quadrantanopia is the most common type of incomplete homonymous hemianopsia.2 The most common etiology of any homonymous hemianopsia is CVA (specifically ischemic CVA, which accounts for nearly 70% of all hemianopsias).2,3 Research also has shown that, while visual field characteristics are helpful in lesion location, specific visual field defects do not always indicate specific brain locations.2-4 In fact, one study indicated that 76% of lesions that caused inferior quadrantanopsias were found in the occipital lobe, while just 22% were isolated to the parietal lobe.4 In our patient’s case, neuroimaging results verified her visual field loss.
In a large study, other documented causes of hemianopic defects included trauma (13.6%), tumor (11.3%), brain surgery (2.4%), demyelination (1.4%), rare causes (1.4%) and unknown etiologies (0.2%).2 The researchers determined that the lesions were most commonly located in the occipital lobes (45%) and the optic radiations (32.2%).2
Aphasia is among the common consequences of left hemispheric lesions and is the most common neuropsychological consequence of stroke (33% in all stroke patients proceed through the acute phase).5 Unilateral neglect is a disorder that mostly affects patients with lesions of the right hemisphere.5 In general, left-sided neglect is the most widespread neuropsychological deficit following damage to the right cerebral hemisphere.5 Reports on the incidence of visual neglect vary, ranging from 13% to 85% of cases.5
Additionally, many patients exhibit denial of the motor, visual or cognitive deficits.5 This syndrome, which includes denial of hemiparesis or hemianopsia, is a common disorder that has been verified in 17% to 28% of all patents with acute brain stoke.5
We educated our patient on the extent and etiology of her visual field loss. Communication with her primary care provider was paramount in establishing the etiology of field defect. Subsequently, we plan to evaluate our patient for the presence of glaucoma. However, we controlled her dry eye effectively with daily artificial tear supplementation.
Thanks to Jason Price, O.D., of Louisburg, N.C., for contributing this case.
1. Miller NR, Walsh FB, Hoyt WF. Walsh and Hoyt’s Clinical Neuro-Ophthalmology. 4th ed. Baltimore: Williams and Wilkins; 1982:136-7.
2. Zhang X, Kedar S, Lynn MJ, et al. Homonymous hemianopias: clinical-anatomic correlations in 904 cases. Neurology. 2006;66(6):906-10.
3. Zhang X, Kedar S, Lynn MJ, et al. Homonymous hemianopia in stroke. J Neuroophthalmol. 2006;26(3):180-3.
4. Jacobson DM. The localizing value of a quadrantanopia. Arch Neurol. 1997;54(4):401-4.
5. Sinanović O.Neuropsychology of acute stroke. Psychiatr Danub. 2010 Jun;22(2):278-81.

