
Although presbyopia can be corrected in many ways, none are perfect. Every practitioner does everything he or she can to prevent patients dissatisfaction with their vision correction. For example, progressive addition lenses (PALs) have been a boon to our patients and our practices. Initially, practitioners faced challenges in dispensing them, but continuous technological improvements and progressive experience with PALs have made them standard treatment options for presbyopia.
Likewise, presbyopia-correcting intraocular lenses (IOLs) are going through a similar process; the technology and our experience with it is improving, as it has with PALs for the past 20 or so years. Multifocal and accommodating IOLs have been in FDA trials since the 1980s. The first FDA-approved multifocal IOL, the Array (Advanced Medical Optics), was approved in 1997.
Now, there are four FDA-approved IOL options to decrease patients need for reading glasses, and more are on the way.1 The IOLs currently available in the U.S. to decrease a patients dependence on glasses after cataract surgery are the Array multifocal IOL, the AcrySof ReSTOR multifocal IOL (Alcon), the Crystalens accommodating IOL (Bausch & Lomb), and the ReZoom multifocal IOL (AMO). And, the Tecnis multifocal IOL (AMO) will likely be approved in early 2009.
All recent IOL improvements are based on a better understanding of wavefront science. Wavefront has helped us to better understand and treat patients visual problems. Wavefront analysis has become useful in diagnosing vision complaints, even in cases when the eye looks normal. This was first recognized in the late 1990s. Patients presented with induced spherical aberration after laser vision correction. Their eyes looked normal, but they complained of increased glare and halos. Wavefront analysis helped the clinician and the patient understand the problem. Now, wavefront analysis prior to laser vision correction is a standard procedure.
Today, wavefront analysis is helping us to better understand presbyopia and how to treat it. This article is another step on the road to understanding wavefront technology. It will provide a wavefront-based explanation of these new IOLs, so you will understand when to recommend them and how to care for your patients who opt for them.
Current Understanding
Presbyopia is often more complex than one may initially think. For example, the graph created by Franciscus Cornelius Donders, M.D., which is often studied by optometry students, illustrates a steady decline of near vision over time.2 The common misconception is that this graph demonstrates a steady, uniform decline in focusing power over the pupilwhich is not what happens. Wavefront analysis demonstrates the non-uniform response by the normal healthy crystalline lens to accommodative stimuli at all ages (figure 1). As the natural crystalline lens ages, its response diminishes and becomes even more non-uniform with time.3,4,5 As the lens becomes more rigid, higher-order aberrations (HOAs) occur. These are noted with accommodation.3
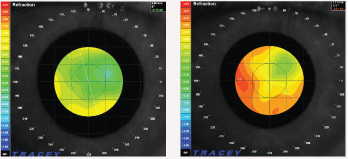
1. Left, a normal wavefront image for a healthy 13-year-old eye, 20/15 O.U., looking at a distance target. Cooler colors represent hyperopia, and warmer colors represent myopia or accommodation. Right, the same eye at the same exam, looking at a near target with 5.00D of vergence stimulus. Note the non-uniform response to a near image with normal accommodation. The red area shows a maximum accommodative response of about 4.00D, and the green area has essentially no response; yet, the patient has normal subjective and objective near vision.
Accommodation is a very complicated process that we tend to over-simplify. While we have been successfully treating presbyopia with plus-power lenses for hundreds of years, remember that our understanding of the problem is evolving. When PALs were first introduced, there was much skepticism. When artificial lenses after cataract surgery were introduced, there was much skepticism. But, both tools became standard as we better understood the problem.
The treatment of presbyopia with IOLs is on a similar trajectory. Two broad categories of IOLs are FDA-approved to treat presbyopia: accommodating IOLs and multifocal IOLs. Within the latter category, there are refractive and diffractive IOLs. The terms refractive and diffractive refer to the mechanism used to create the near image. Each group has its unique pluses and minuses.
Accommodating IOLs attempt to simulate the natural process of accommodation by changing power during accommodationit changes power in response to muscular contraction, just like the natural crystalline lens. Currently, the Crystalens is the only FDA-approved accommodating IOL.
The advantages of accommodating IOLs are these: They can more closely simulate a persons original vision, and they have the least amount of unwanted visual sensations, such as glare or halos, out of the presbyopia-correcting IOLs.
The problem: While the lens works very well in most patients, current technology does not allow for consistent, strong near vision in every patientthe accommodation seen with such IOLs can be likened to that of a patient in their early 40s. In most cases, resultant vision is satisfactory, but there is effort involved, and sometimes, the near vision fatigues and the patient needs help from low-power reading glasses.
On rare occasion, eyes implanted with accommodating IOLs wont demonstrate much (if any) accommodation. In these situations, the advantage of an accommodating IOL is its ability to convert to a monovision type correction with laser vision correction. This is a great secondary option if the accommodating lens does not respond as desired.
On the other hand, the distance image produced by an accommodating IOL is often better than that produced by a multifocal IOL, and any insufficient near vision can be improved with reading glasses or laser vision correction (figure 2).
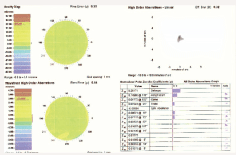
2. A composite wavefront image of an eye with an accommodating IOL. There are very few aberrations; most of them are defocus or sphere and cylinder. Laser vision correction will eliminate the majority of aberrations from this eye.
There are many more accommodating IOLs in the pipeline. Most likely, the next to be FDA approved is the Synchrony (Visiogen), a dual-optic accommodating IOL, in which one optic moves relative to the other.
Multifocal IOLs, on the other hand, attempt to replace accommodation with multiple, fixed images, similar to the principle behind bifocal contact lenses or spectacles. Multifocal IOLs produce strong distance and near vision, but the multiple images can cause significant side effects with distance vision in a notable minority of patients.
The ReZoom and the Array are FDA-approved zonal refractive IOLs. The AcrySof ReSTOR and the AcrySof ReSTOR Aspheric are currently the only FDA-approved diffractive multifocal IOLs; the Tecnis will join this group upon FDA approval.
Refractive multifocal IOLs, such as the ReZoom, create the most simultaneous images. They allow an object to be viewed at all distances, so they are very versatile, but they also create the most unwanted visual sensations due to all of these images. So, these lenses offer the most consistent focus from far to intermediate to near, but with the associated cost of more aberrations (figure 3).
Aspheric, diffractive IOLs, such as the ReSTOR Aspheric and the impending Tecnis, compensate for spherical aberration in most patients, which improves visual quality for most patients (figure 4). Diffractive lenses create two distinct imagesone for distance and one for near. These lenses usually provide very strong distance and near vision. However, they tend to provide the worst intermediate vision.
Aspheric IOL technology was developed to correct spherical aberration induced by standard monofocal IOLs. It was developed after wavefront technology demonstrated excess positive spherical aberration in eyes implanted with standard monofocal IOLs, much like wavefront technology demonstrated excess positive spherical aberration in eyes after myopic laser vision correction in the late 1990s. Aspheric technology can be a very powerful tool to improve the optical image quality of any type of IOL.
Making Waves
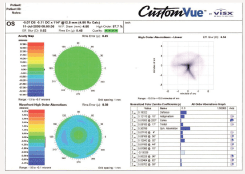
3. A composite wavefront image of an eye with a refractive multifocal IOL that does not correct for spherical aberration. The major wavefront error in this eye is spherical aberration, and minor elevations are noted with other aberrations. Only minimal sphere and cylinder are noted, so laser vision correction enhancement will not improve much. The cumulative visual effect of all aberrations is seen at the top right.
Wavefront technology and imagery provides an excellent platform on which to evaluate patients and their IOL options.
We have discussed the history of laser vision correction thanks to wavefront technology, resulting in what we now call custom wavefront laser vision correction. Wavefront technology has also been used to understand the iatrogenically induced excess positive spherical aberration in pseudophakic patients implanted with standard monofocal IOLs after cataract surgery. The solution to this problem was the introduction of negative aspheric IOLs to neutralize the average amount of naturally occurring positive spherical aberration of cornea. Now, many of the IOLs implanted in the
Imagine the patient who comes to you with bitter complaints of poor vision, but with an eye that looks normal upon examination. In our practice, we have seen an interesting pattern develop while caring for these patients. They are referred to our retinal specialist for evaluation. The patient receives a full retinal evaluation, including 90D lens, Amsler grid, photos and OCT, and perhaps even an angiogram.
Occasionally, after all of these tests, nothing has been found to explain the patients vision. At this point, the retinal specialist orders a wavefront analysis, and significant HOAs, consistent with the patients complaints, are noted on the test. These are nearly always lenticular and resolved with cataract surgery. These patients have defined themselves as very sensitive to HOAs, and for this reason, they are happiest when an aspheric monofocal IOL is implanted into their eye.
Patients Needs vs. Wants
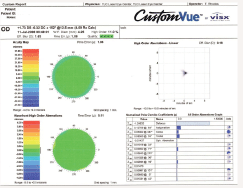
4. A composite wavefront image of a diffractive IOL that corrects spherical aberration. There is essentially no spherical aberration noted in this eye and very few other aberrations, but the eye is still hyperopic. It will benefit from a laser vision correction enhancement.
So, how do you know what lens to recommend for each patient? If there was one perfect lens, the decision would be easy for both doctor and patienthowever, all of the current IOL options are a compromise. Spend time talking with the patient, learn about his or her specific visual needs and desires, and note his or her tolerance for adverse symptoms. After this discussion, a good decision can be made regarding the lens that will most likely enable patients to function well in their everyday lives with the least amount of adverse symptoms.
Often, the best choice for a given patient is an aspheric, monofocal IOL, with the aim of a
The issue, as far as patient satisfaction goes, is the need for reading glasses. Some people simply dont want to wear them. So, if the patient wants to consider other options, there is monovision with monofocal IOLs, as well as multifocal and accommodating IOLs.
A good strategy for choosing IOLs is based on patients tolerance for adverse symptoms vs. their willingness to wear reading glasses as needed. An accommodating IOL is similar to a monofocal IOL in symptom profile with relatively few adverse subjective symptoms, but it is also more likely to require low-power reading glasses than a multifocal IOL. If the patient wants the least risk of adverse visual symptoms and is motivated to be less dependent on reading glasses, but is willing to use them as needed, an accommodating IOL is a good choice.
Or, if the patient is willing to run a slightly higher risk of adverse symptoms, but really does not want to wear reading glasses, a good option is to use an accommodating IOL in one eye and a diffractive IOL in the fellow eye. This mix and match concept works well. If a patient wants to have the best possible reading vision and is willing to tolerate adverse visual symptoms, the best option may be a bilateral, diffractive IOL implantation. This combination will usually provide the strongest near vision. If the patient wants to have the most flexible vision for all distances and is also willing to tolerate adverse visual symptoms, the best option may be to mix and match with a refractive IOL in one eye and a diffractive multifocal in the fellow eye. All of these options can make sense in a given patient. When mixing and matching IOLs, there does not appear to be a clear benefit to placing a certain one in the dominant or non-dominant eye. The pair of eyes will usually function quite well together regardless of which lens is placed in which eye.
Our knowledge of wavefront science and specialty IOLs is constantly improving. There is no doubt that they will improve in the future, much like progressive addition lenses have over the last several decades. It is important to be able to educate patients on the options. Both you and your patients will benefit from the process of learning about wavefront and the newer IOLs based on them.
Dr. Kevin Waltz is a founding partner of Eye Surgeons of Indiana in
Dr. Brenda Wahl is the Vice President of Research at Eye Surgeons of Indiana in
1. Chang DF, Dell SJ, Hill WE, et al., eds. Mastering Refractive IOLs: The Art and the Science.
2. Borish
3. Rosales P, Wendt M, Marcos S, Glasser A. Changes in crystalline lens radii of curvature and lens tilt and decentration during dynamic accommodation in rhesus monkeys. J Vis 2008 Jan 28;8(1):18.1-12.
4. Vilupuru AS, Roorda A, Glasser A. Spatially variant changes in lens power during ocular accommodation in a rhesus monkey eye. J Vis 2004 Apr 22;4(4):299-309.
5. Baumeister M, Wendl M, Glasser A. Edinger-Westphal stimulated accommodative dynamics in anesthetized, middle-aged rhesus monkeys. Exp Eye Res 2008 Jan;86(1)25-33.
6. Waltz KL. CrystalensWhat is the Mechanism of Action? In: Chang DF, Dell SJ, Hill WE, et al (eds). Mastering Refractive IOLs: The Art and the Science.
7. Waltz KL. The crystalens changes its radius of curvature. Cataract Refract Surg Today 2005 June. Available at: www.crstoday.com/PDF%20Articles/0605/CRST0605_F9_
Waltz.html (Accessed Sept 5, 2008).
8. Ganem S, Waltz KL. Presbyopia Treatment Options. Presented at the European Society of Cataract and Refractive Surgery. September, 2004;

