As health care providers, optometrists must be ethical, moral, responsible and knowledgeable decision-makers. But what happens when youre faced with a case that isnt cut-and-dried? What if you must pick between two equally important responsibilities, or choose the best of several unfortunate outcomes?
Real doctors submitted each of the actual cases below. Consider the case of the brain-injured patient with a compromised field of vision. Do you respect the doctor-patient relationship and allow her drive if she chooses, or do you break this confidence and report her to the Division of Motor Vehicles? Compare your responses with those of five optometric clinicians as they weigh in on this case and others.
Do You Refer a Lousy Kid?
A 10-year-old male with itchy, red lashes is brought in by his mother. His symptoms had increased over several days. Vision is 20/20 in both eyes with no significant refractive error. Ocular health exam is unremarkable except for nits, tubules around the lash roots, and a single louse. I removed the nits and louse with forceps, instructed the mother on hygiene around the house and told her to purchase Rid or Nix shampoo. (I dont recommend Kwell [lindane], which has demonstrated serious side effects, especially in children.) The mother was vigilant, and all symptoms were gone in several days.
Meanwhile, I consulted with two M.D.s about this case. One doctor said that all eyelid lice are pubic lice and that I have a responsibility to report this to Human Services in the case of any minor. The other doctor said this infestation was probably a random occurrence and not worth worrying about.
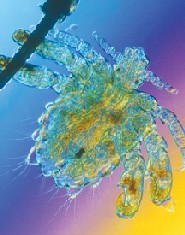
What do you do if you see a pubic louse (such as the crab louse pictured here) in the eyelashes of a 10-year-old boy? Do you report it, or hope its nothing to worry about?
Is it our responsibility and liability to report lice in lashes in children, or is it coincidental and best left unreported?
Dr. Hudson: First, action in a case such as this should not be taken based on the hearsay advice of an M.D. In this case, the optometrist should ask the local Department of Human Services if there is public policy regarding pubic lice. If there is, follow that policy.
In the absence of such policy, you have to act on the very real possibility that the youth has been compromised. Start with a heart-to-heart talk with the mother about what your responsibilities are and explain that you need to report the findings to Human Services.
Dr. Goodman: We have a responsibility to report suspicions of child abuse to the appropriate authorities, and it is suspicious that pubic lice could be on a 10-year-old childs eyelashes. However, the vectors of transmission for lice include common items with which an infected person comes in contact, including towels, washcloths, sheets, clothes, etc. Therefore, I would not feel compelled to do more than treat him and educate the mother as this doctor did above.
Dr. Murphy: Pubic lice are crab-like in appearance and are fairly easily distinguishable from the two other types of licehead lice and body licewhich are seldom found on lashes. Pubic lice are found on lashes, especially in children. Pubic lice can be contracted by means other than sexual contact, but it is not common.
If the louse in this case is indeed a pubic louse, the optometrist cannot simply ignore the implications. He should inform the mother that this particular type of louse can attack other areas of the body and that he is going to refer the child to a pediatrician for a more thorough examination. The pediatrician is more expert in dealing with these cases and it would be more appropriate for him to consider referring the case to Human Services. Referral to Human Services can cause significant turmoil to a family and should not be done unless a very strong possibility of abuse exists. That appears doubtful in this case but a more thorough exam may indeed lead to such a conclusion. Therefore make the referral to the pediatrician.
Should I Map This Chap?
A 21-year-old male soft contact lens patient, who has worn -3.00D spheres without complications, presents for his one-year follow-up. The exam finds a plano over-refraction, 20/20 corrected visual acuity O.U., clear corneas and unchanged K readings.
I am an associate at a practice that has finally acquired a corneal topographer, and we hope to expand our orthokeratology and extended-wear population. With the addition of the topographer, our new protocol is to perform corneal topography on all new contact lens fits and to repeat the procedure annually at an additional charge to the patient of $25, incorporated in the annual exam fee.
On one hand, Im obligated to comply with the practices protocol, and I understand the clinical value of this policy overall. Yet Im not sure that follow-up topography (and the additional fee) is warranted for this patient. What to do?
Dr. Murphy: The optometrists primary obligation is to the patient. The optometrist has a fiduciary responsibility to the patient and should not perform testing needlessly to generate revenue for the practice. This case does not demonstrate a need for topography because it very likely would not contribute any worthwhile information.
The Clinical Panel
Steven I. Goodman, O.D., is in private practice in Medford, N.Y. He specializes in primary care and low vision.
Marc Hudson, O.D., is in private practice in Lexington, Va.
John Murphy, O.D., (no relation to the author) is chief optometrist at Kaiser Permanente Riverside Medical Center in Riverside, Calif. He notes that the views he presents are his own and not necessarily that of the organization.
Michael C. Radoiu, O.D., is in a multidisciplinary practice in rural Staunton, Va.
Bobby Wood Jr., O.D., is in group practice in rural Uvalde, Texas. He specializes in glaucoma and diabetic retinal care.
The optometrist should consult with the members of the practice and structure protocols for ordering topography when a more clearly defined need is indicated. Cases such as this needlessly increase the cost of health care and undermine the doctor-patient relationship.
Dr. Wood: This patient has not had a history of contact lens intolerance, anterior segment disease or myopic creep, so annual corneal topography would not be considered medically necessary. But since the practice has bundled the corneal topography fee into the annual exam and this service will be provided to all patients, the practitioner is obligated to provide the patient with the services for which he will be charged.
If the associate feels strongly about the need to not charge this patient for corneal topography, he should petition the partners in the practice to provide an additional level of contact lens exam. This additional level would carry a lower fee and would not include corneal topography for patients in whom it is not warranted. The associate optometrist has a duty to perform the necessary testing required for each patient. He must also, to the best of his ability, determine the appropriate fee for the services rendered according to the fee schedule set forth by the clinic.
Dr. Radoiu: To ignore topography would be to possibly miss occult corneal problems such as irregular astigmatism, corneal dystrophies, etc. And, to miss something when you have the instrument at hand would be negligent.
So, I advocate performing corneal topography regularly but judiciouslynot on every patient every time, and not to pay off the instrument. Only use for baseline contact lens fits and when you suspect corneal disease. Also, have a set office policy in which corneal topography is included in the contact lens fitting fee and not parsed out.
Dr. Hudson: Newer technology often reveals things of which you were previously unaware. It is your responsibility to apply these technologies to the best of your abilities. Do you skip tonometry because the patient is at low risk for glaucoma? Do you skip the slit lamp exam because he has no complaints? Obviously not. You never know what you will find.
Binocular indirect ophthalmoscopy once was a new procedure. Did you stop doing it when you didnt find pathology in most of your patients? No, you continued to do it because you were striving to do the best job possible, and it has become the standard of care.
In this situation, the associate needs to voice his or her reservations regarding the use of topography in the practice. This associate obviously does not support the policy. He or she needs to express this opinion to the principals in the practice and get their input as to why they think the policy is justifiable. This situation will only fester. Open, honest exchange between all doctors is necessary so that patient care can be provided seamlessly among all the doctors.
Can I Stall This Motorist?
A 34-year-old woman came in after hearing me present on brain injury and vision therapy at a conference of the state brain injury association. An operation for brain aneurysm left her with an absolute left homonymous hemianopia and total paralysis of the left side of her body. The brain operation saved her life, but she lost function in most of the right side of her brain. Her drivers license was suspended following the brain injury.
During my examination, she mentioned that she was working with a driving instructor and was scheduled to take her drivers test in a few weeks. I was concerned that her blind field was the left field and that there was no way that she met the driving regulations for visual field in my state or in any state. I considered both her safety and the safety of other drivers that would cross her path.

For this driver, do you honor your duty to the public, or to patient confidentiality?
However, some state laws prohibit doctors from reporting a driver who is mentally competent but whose driving ability is impaired without the patients permission.
Which takes precedence: My civic duty to protect motorists (including the patient herself) or doctor-patient confidentiality?
Dr. Wood: With the advent of HIPAA and the longstanding doctor-patient confidentiality policy adopted by most states, this doctor cannot and should not make a report to any government or local organization concerning the patients fitness to operate a motor vehicle until authorized to do so by the patient.
Fortunately, most states require that drivers pass a vision test before receiving their license. Since this patient will most likely fail the vision test, the patient will be required to have the doctor fill out a vision statement and give his recommendation or restrictions for driving. At that time, the doctor can report this patients visual field defect and impaired ability to drive to the appropriate agency.
As both a preventative measure and a medicolegal alternative, the doctor could send a letter via certified mail to this patient before the patient takes the drivers test. This letter should outline the patients visual impairment, the driving regulations for their state, whether this driver meets the regulations and the possible consequences of death or injury that could occur due to these impairments. This informs the patient of the real risks involved with operating a motor vehicle with impaired vision. It also shows that the doctor counseled the patient to the best of his or her ability to prevent the patient from potentially causing harm to herself or others.
Dr. Goodman: A potential public health threat should not be dismissed lightly. Your first obligation, though, is to your patient. This includes educating your patient about the field defect so that she understands how dangerous it is for herself and any passenger with her.
In [my state of] New York, if acuity is 20/40 or better, there is no field requirement unless the field is less than 20 degrees. With a left homonymous hemianopia, she still has the other half of her field and she meets the requirements for driving. So, the civic duty must take a back seat.
Dr. Radoiu: Youll have to comply with your state laws at the least. But a lot of times, Ill try to go beyond the state law for the patients sake and everybody elses. The bottom line here is that the motorists privilege is trumped by public safety. So public safety supersedes the motorists desire to drive. Flag this patient to the DMV.
Follow or Fudge the Rules?
A 55-year-old woman presents for an annual exam. She requires a slight change in prescription and desires a new pair of designer frames. Her insurance plan, however, does not cover the cost of the frames that she wants. Her plan requires the full price of the frame to be covered and does not allow the patient to pay any overage.
I explain that we have a nice selection of less expensive frames that are covered by her insurance plan. She takes me aside and asks if she can have the designer frames and she will pay the difference. Itll be just our little secret, she says.

Is it okay to bend the strict rules of a vision plan to satisfy this patient?
I often find myself in a difficult situation. Im required to follow the rules of insurance plans, but I also want to satisfy my patients needs any way I can. Whats the right thing to do?
Dr. Radoiu: I wouldnt even entertain this patients proposal. Theres both a pragmatic side to this and a moral one. Both lead to the same conclusion. On the moral side, I never do any under-the-table deals. Its fundamentally unethical. On the pragmatic side, youre inviting the insurance company to either drop you from their panel or worseto inspect or audit you.
Dr. Murphy: By accepting the insurance plan, the optometrist has a contractual obligation to the plan and should follow the terms of the contract. The doctor, however, could satisfy the patient by giving her a discount on a second pair of glasses that are more to her liking.
Dr. Wood: The doctor must follow the rules of the insurance plan and not have a secret policy for certain patients. The patient may then expect other rules and policies to be bent or broken. Furthermore, the patient may expect the same courtesies for her family and co-workers, thus making this not a little secret at all.
The real ethical dilemma here is not whether to allow the designer frame upgrade. It is whether the practice should accept an insurance plan that limits the O.D.s ability to provide high-quality services and materials to their patients. In this situation, the insurance plan is not meeting the patients or the doctors needs. This plan limits the patients choice of eyewear, and it limits the doctors ability to meet the patients needs and receive higher compensation through the sale of designer eyewear. So, this insurance plan fails both the practitioner and patient and should likely be dropped by the practice.

